
EAR
Dr. Rana Mumtaz
Special Senses: EAR
Sources:
Stevens & Lowe's Human Histology Fourth Edition
Wheater’s functional histology: a text and colour atlas.
OXFORD HANDBOOK OF CLINICAL SPECIALTIES-NINTH EDITION
Learning objectives:
1. Understand the bony and membranous labyrinths.
2. In the vestibule be able to recognize and describe the function of the sensory end organs.
3. Be able to recognize and describe the function of the components of the cochlea including the
organ of Corti.
4. Be able to distinguish the auditory parts of the inner ear from those of the vestibular system.
What are their roles in hearing and balance?
5. What are sensory hair cells?
6. What is presently the only known "cure" for deafness besides hearing aids?
Introduction
The ear has the dual sensory function of maintenance of equilibrium and hearing. Structurally,
the Vestibulocochlear system may be divided into three parts, the external ear, the middle ear
(or tympanic cavity), and the internal ear (or labyrinth).
The specific sensory receptors for both movement and sound are situated within a
membranous structure located in the internal ear, while the external and middle ear are
concerned with reception, transmission and amplification of incoming sound waves.
The external ear:
Comprises the pinna and external auditory canal. Is responsible for reception of sound waves
which are funneled onto the eardrum. The pinna is composed of elastic cartilage covered by
hair-bearing skin.
External Auditory Meatus:
It is a sinous tube that leads from the auricle to the tympanic membrane, conducting
sound waves along its pathway.
EAR
Dr. Rana Mumtaz
The outer third of the meatus is formed of elastic cartilage, and the inner two-thirds is
bone (formed by the tympanic plate of the temporal bone).
Is lined by thin skin which is closely bound to the underlying cartilage or bone by a dense
collagenous dermis. The skin of the outer third has fine hairs which provide protection
from foreign bodies.
The dermis contains numerous coiled tubular ceruminous glands which secrete wax
(cerumen). These glands open directly onto the skin surface or into the sebaceous
glands associated with hair follicles.
The accumulation of the secretions of the ceruminous glands together with sebaceous
secretions, and desquamated cells produce a yellowish-brown waxy material called
cerumen which protects the skin of the external auditory meatus from moisture and
infection.
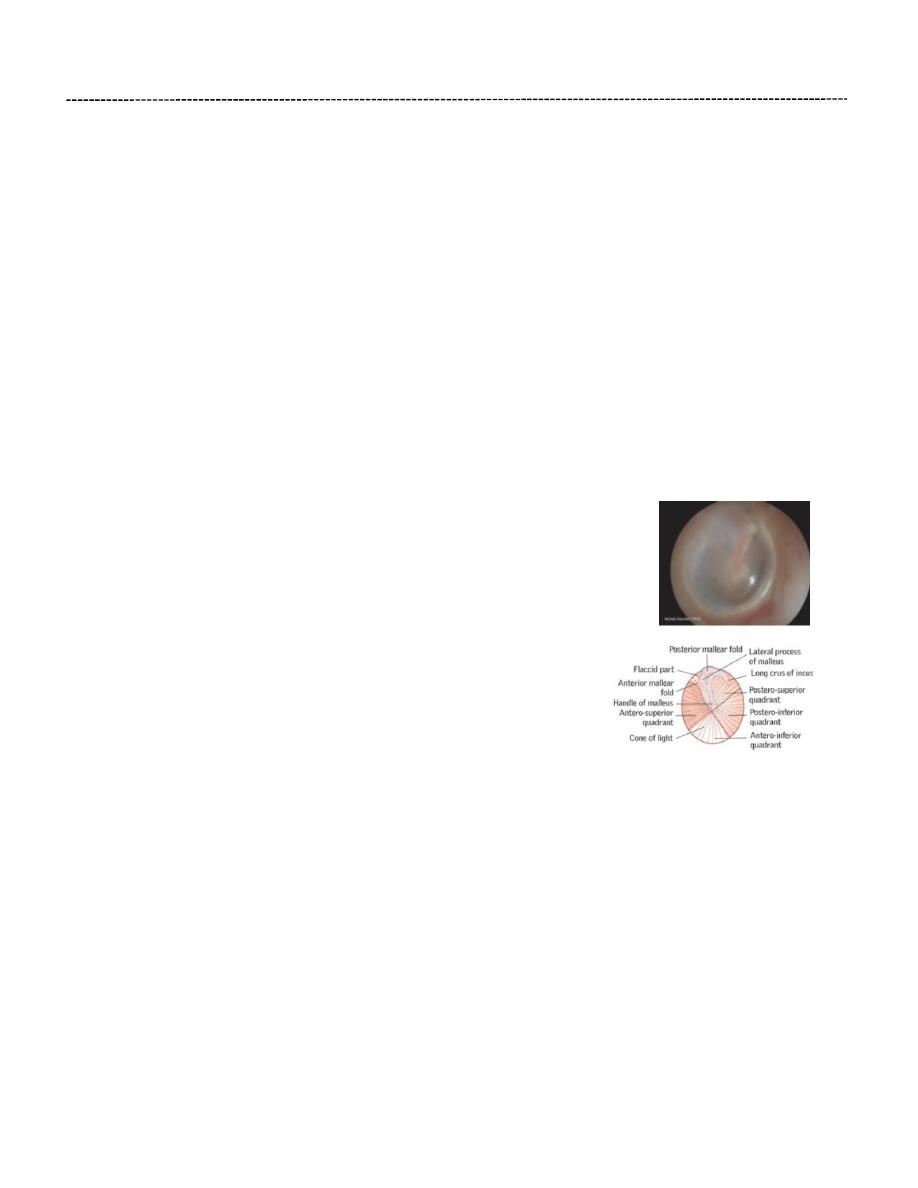
Tympanic Membrane (Eardrum):
Is pearly grey, thin fibrous membrane separating the external auditory
canal from the cavity of the middle ear.
The anterior upper quadrant of the tympanic membrane (pars flaccida)
is flaccid and more transparent, since the connective tissue layer is much
thinner there. This region is known as Shrapnell’s membrane. The
remaining part of the membrane is tense (pars tensa) being firmly
attached to the surrounding bone by a fibrocartilagenous ring. The
handle of the malleus is attached to the centre of the membrane.
Structurally, the tympanic membrane is made up of three layers:
An external cuticular layer: consists of thin hairless skin,
the epidermis being only about 10 cells thick and the basal layer being flat and devoid of
the usual epidermal ridges.
An intermediate fibrous layer consists of an outer layer of fibres radiating from the
centre of the membrane towards the circumference and an inner layer of fibres
disposed circumferentially at the periphery.
An inner mucous layer represents a continuation of the modified respiratory-type
mucous membrane lining the middle ear cavity, but in this situation it is merely a single
layer of cuboidal cells devoid of cilia and goblet cells. The underlying lamina propria is
thin with a blood supply separate from that of the dermis of the cuticular layer. A similar
modified respiratory-type mucosa invests the ossicles, small muscles and nerves
exposed to the middle ear cavity.
EAR
Dr. Rana Mumtaz
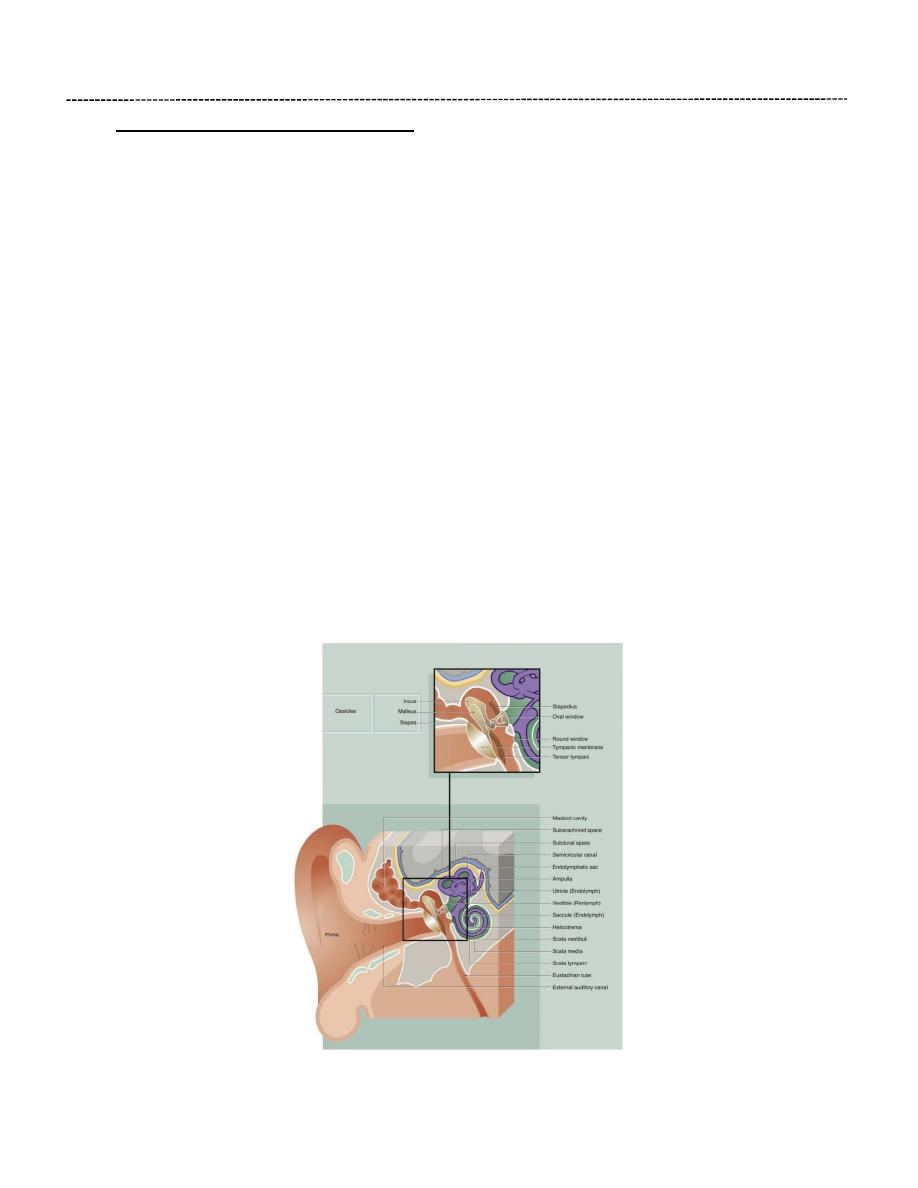
The Middle Ear (Tympanic Cavity):
Is an air-containing cavity in the petrous part of the temporal bone and is separated
from the external auditory canal by the tympanic membrane.
It contains the auditory ossicles, 3 small compact bones, articulated by synovial joints
and covered externally by the same low cuboidal epithelium that lines the inner ear.
These ossicles transmit the vibrations of the tympanic membrane (eardrum) to the
perilymph of the internal ear through the oval window.
Two small skeletal muscles, the tensor tympani and stapedius, pass to the midpoint of
the tympanic membrane and stapes bone, respectively, and damp down excessive
vibrations which might otherwise damage the delicate auditory apparatus.
The tympanic cavity communicates in front (anteriorly) with the nasopharynx through
the auditory (Eustachian) tube which is lined by ciliated epithelium similar to that of the
respiratory tract. Its function is to equilibrate pressure between the middle ear cavity
and the atmosphere. Normally, the auditory tube is collapsed, but it is opened by
movement of muscles in the nasopharynx, such as occurs with swallowing or yawning.
From behind (posteriorly), the middle ear cavity communicates directly with air-filled
spaces in the mastoid bone (mastoid sinuses), which are lined by low cuboidal or
flattened squamous epithelium.

EAR
Dr. Rana Mumtaz
The Inner Ear:
Is situated in the petrous part of the temporal bone, medial to the middle ear and it consists of:
1. A series of bony cavities in the temporal bone of the skull called the bony labyrinth.
2. An interconnected fluid-filled sacs that are contained within the bony labyrinth called the
membranous labyrinth.
The bony labyrinth is divided into three main areas:
• The vestibule. The central part of the osseous labyrinth; it gives rise to three semicircular
canals posteriorly and to the cochlea anteriorly. The vestibule contains two components
of the membranous labyrinth, the utricle and the saccule, which are connected by a
short Y-shaped duct from which arises the endolymphatic duct.
Laterally, the vestibule is separated from the middle ear cavity by a thin bony plate
containing two fenestrations or windows. The oval window is occluded by the base of
the stapes bone and its surrounding annular ligament whereby vibrations are
transmitted to the perilymph from the tympanic membrane via the ossicle chain. The
round window is closed by a membrane similar to the tympanic membrane (and is thus
sometimes described as the secondary tympanic membrane). This membrane permits
vibrations, which have passed the sensory receptors for sound, to be dissipated.
• The semicircular canals. Three semicircular canals arise from the posterior aspect of the
vestibule, two being disposed in vertical planes at right angles to one another and the
other in a near-horizontal plane. Within each semicircular canal is a semicircular duct
filled with endolymph and continuous at both ends with the utricle; near one end of
each semicircular membranous duct is a dilated area called the ampulla . In each
ampulla, there is a ridge called the crista ampullaris containing sensory receptors with
axons converging on the vestibular nerve. Together with the receptors of the maculae of
the utricle and saccule, these receptors help maintain balance and equilibrium.
• The cochlea. The cochlea occupies a conical spiral-shaped space in the temporal bone,
extending from the anterior aspect of the vestibule. The membranous component of the
cochlea arises from the saccule and spirals upwards, with its blind end attached at the
apex of the osseous space.
EAR
Dr. Rana Mumtaz
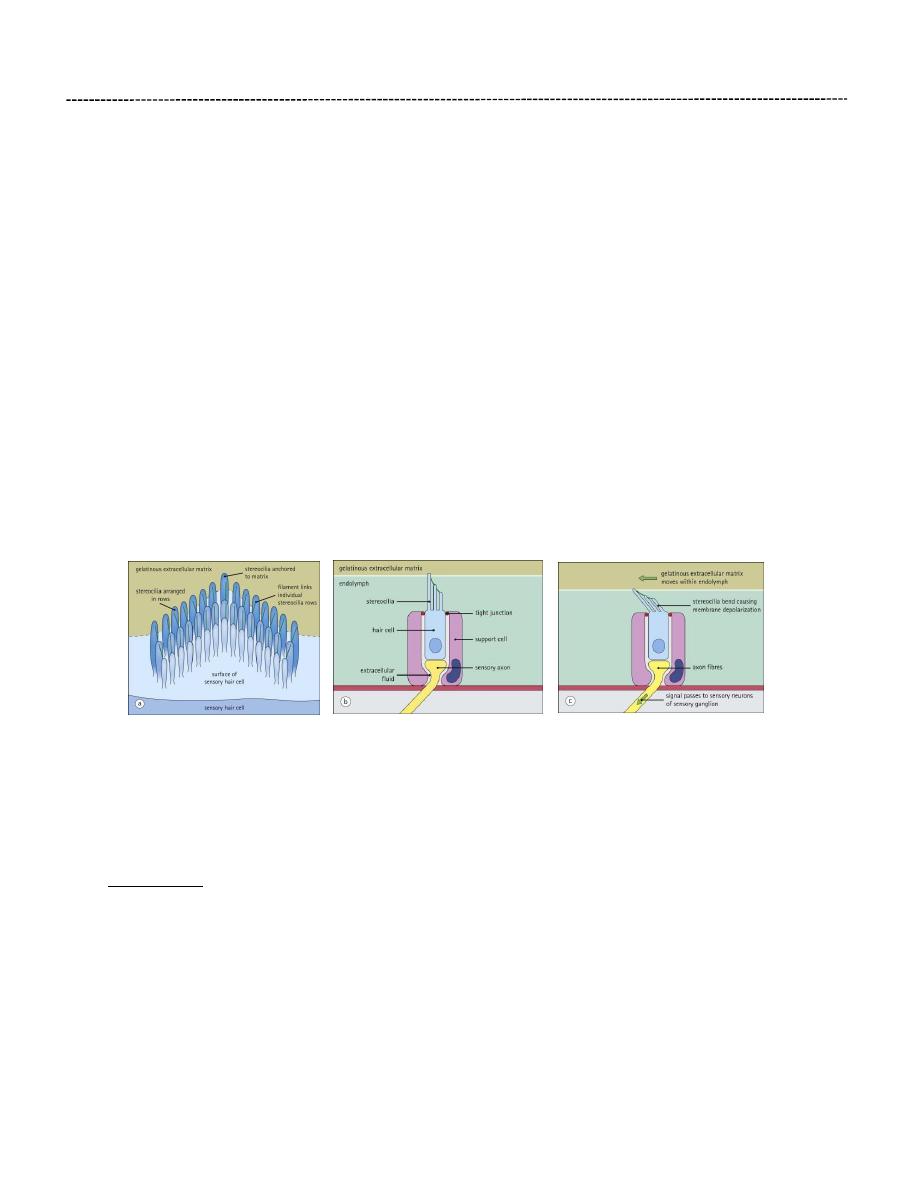
Hair Cells:
Within the inner ear, movement of endolymph is detected by specialized epithelial cells (hair
cells). Hair cells are arranged in different patterns in the cochlea and vestibular apparatus to
detect acceleration (movement), gravity (position) or sound (hearing).
The apical surface of each hair cell bears a highly organized system of microvilli (stereocilia),
which are arranged as three parallel rows in a V- or W-shaped pattern. The height of the
microvilli progressively decreases from the back to the front of the hair cell. Fine filaments link
individual microvilli from each row, with the tips of the shorter microvilli behind. Each hair cell
is rigidly fixed in place by support cells, however, the tips of the tallest row of microvilli are
embedded in a gelatinous extracellular matrix, which is free to move within the fluid cavities of
the inner ear or vestibular system. Deflection of the microvilli causes electrical depolarization of
the hair cell membrane, which is transmitted to the central nervous system by the connecting
axons of sensory nerve cells.
Support cells surround the hair cells and are anchored to them at their apex by occluding
junctions. These junctions maintain ionic gradients between the endolymph and the
extracellular fluid around the cells, the gradients being reversed on depolarization.
Patches of hair cells are located in three sites:
• Within the vestibular apparatus in the ampullae of the semicircular canals to detect acceleration
• Within the macula of the utricle and saccule to perceive the direction of gravity and static position
• Within the organ of Corti of the cochlea to detect sound vibration.
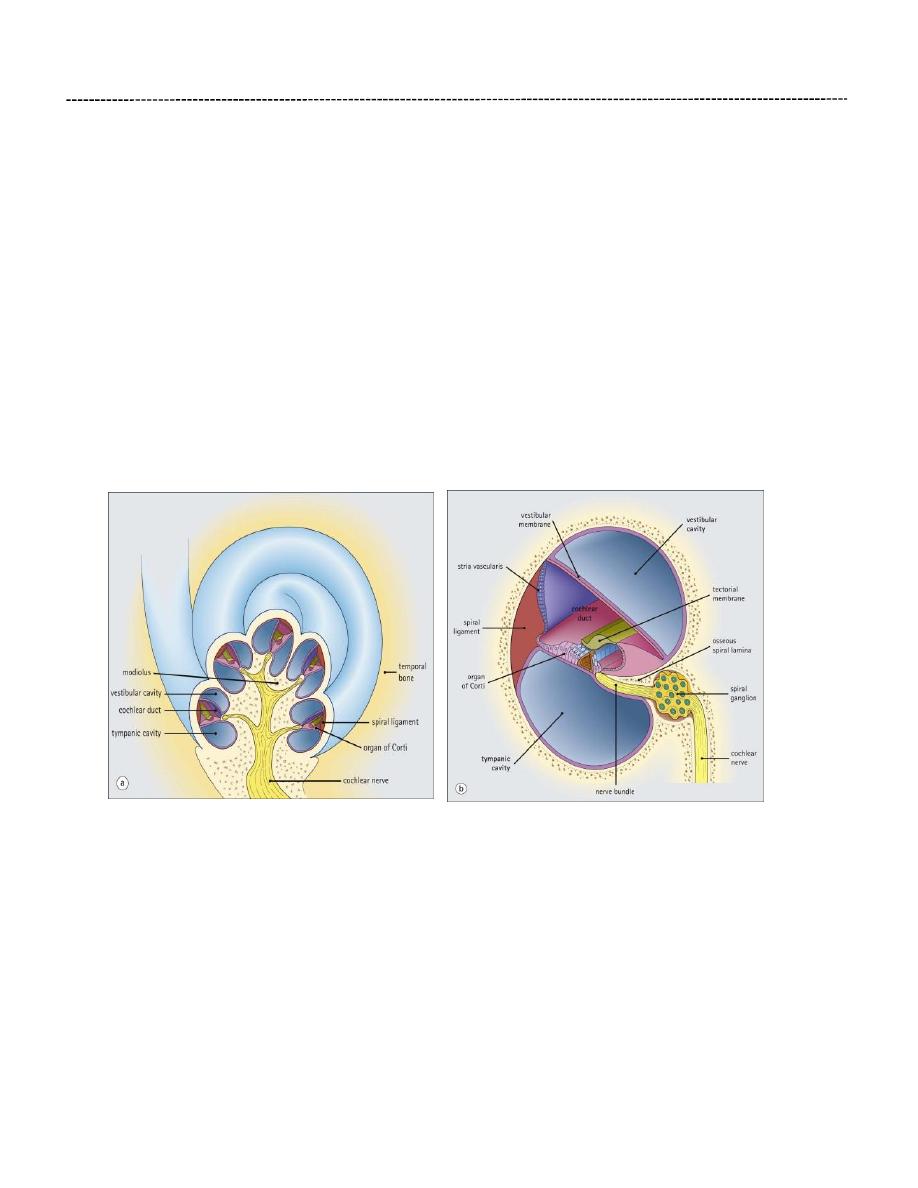
The Cochlea:
Is the part of inner ear concerned with perception of sound. The cochlea (about 35mm in
length) makes two-and-half spiral turns around a bony core known as the modiolus. The
modiolus has spaces containing blood vessels and contain the cell bodies and processes of the
acoustic branch of the eighth cranial nerve (spiral ganglion). Extending laterally from the
modiolus is a thin bony ridge, the osseous spiral lamina, which extends further across the
cochlea in the basal region than it does at the apex.
EAR
Dr. Rana Mumtaz
The Cochlear duct (Scala media):
Is a spirally arranged tube lying within the bony cochlea. It is triangular in cross section and is
connected to the saccule by the ductus reuniens. The cochlear duct is attached to the bony
walls of the cochlea in such a manner as to divide the osseous space into three spiral
compartments. The middle compartment, the scala media, contains endolymph and the upper
(scala vestibule) and lower (scala tympani) compartments contain perilymph.
At the base of the cochlea, the scala vestibule is directly continuous with the perilymph of the
vestibule and via this space, vibrations pass through the perilymph towards the apex of the
cochlea. At the apex, the scala vestibuli becomes continuous with the scala tympani of the
cochlear spiral via a minute hole called the helicotrema. the scala tympani terminates at the
secondary tympanic membrane covering the round window.
The sensory receptors for sound are located in a spiral-shaped structure known as the organ of
Corti.
The sides of the triangular cross section of the cochlear duct are made up of the following
structures: (1) the basilar membrane (forming the floor of the triangular space) (2) the stria
vascularis (forming the lateral wall) and (3) the vestibular membrane (forming the roof the
space). The Cochlear duct ends as a blind sac at the apex of the cochlea.
The basilar membrane consists of a thin sheet of fibrous tissue that is attached medially to the
osseous spiral lamina and laterally to the spiral ligament (which consists of a marked thickening
of the endosteum of the lateral wall of the cochlear canal).The membrane is thinnest at the
base of the cochlea and becomes progressively thicker as it spirals towards the apex. A highly

EAR
Dr. Rana Mumtaz
specialized epithelium lies on the upper surface of the membrane to form the spiral organ of
Corti; the undersurface exposed to the scala tympani, is lined by simple epithelium.
The stria vascularis forms the outer wall of the cochlear duct. It is a specialized area of
epithelium with a rich vascular supply in the lateral wall of the cochlear duct. Many of the cells
here have ultrastructural features indicating an ion transport function, and it is thought that
they secrete endolymph.
The vestibular membrane (Reissner’s membrane) consists of two layers of flattened epithelium
separated by a basement membrane, one cell layer being in continuity with the cells lining the
vestibular cavity and the other in continuity with the cells lining the cochlear duct. The cells are
held together by well-developed occluding junctions to maintain different electrolyte
concentrations between the endolymph and the perilymph.
Organ Of Corti:
The organ of Corti is a highly specialised epithelial structure containing receptor cells which
convert (transduce) mechanical energy in the form of vibrations into electrochemical energy,
resulting in excitation of auditory sensory receptors.
The organ of Corti lies in the scala media, supported on the basilar membrane.
The organ of Corti consists of two types of cells, sensory (hair) cells and support cells of several
different types, including among others the pillar cells and phalangeal cells. The hair cells and
supportive cells are arranged as two groups, an inner group and an outer group, which are
separated by a small opening at the end of the osseous spiral lamina termed tunnel of Corti.
The inner group of cells are smaller and rounder and are arranged as a single row along the
cochlea. The outer group are tall and thin and arranged in three to five parallel rows, depending
on the position in the length of the cochlea.
The sensory cells are known as hair cells because numerous stereocilia project from their free
ends. These stereocilia are embedded in a sheet of gelatinous extracellular matrix (the tectorial
membrane). Axons of the bipolar neurons of the spiral ganglion of the cochlea make synaptic
contact with the hair cells and run to the spiral ganglion.
There are several classes of support cell in the organ of Corti. Inner and outer Pillar cells contain
abundant scaffolding microtubules, and surround and support the triangular cavity (tunnel of
corti). In contrast, phalangeal cells support the hair cells and are attached to them by occluding
junctions at their apices, thus isolating the basal membrane of hair cells from the endolymph
and maintaining electrochemical gradients.

EAR
Dr. Rana Mumtaz
Detection of Sound in the Inner Ear
Sound waves are funnelled into the external auditory meatus and impinge on the
tympanic membrane, which vibrates at the appropriate frequency. These vibrations are
transmitted to the stapes bone via the malleus and incus and, in the process, their
amplitude is enhanced about 10-fold.
The base of the stapes, which lies in the oval window, conducts the vibrations into the
perilymph of the vestibule of the inner ear and pressure waves pass from here into the
scala vestibuli of the cochlea. These pressure waves are probably conducted directly to
the endolymph of the scala media across the delicate vestibular membrane, from which
vibrations are induced in the basilar membrane upon which rests the organ of Corti.
From here, spent vibrations are transmitted into the perilymph of the scala tympani and
dissipated at the secondary tympanic membrane over the round window.
Role of the basilar membrane: the basilar membrane is thinnest at the base of the
cochlea and thickest at the apex. At every point on the spiral, the membrane is ‘tuned’
to respond (vibrate) to a particular frequency of sound waves reaching the ear, with the
highest frequencies (pitch) being sensed towards the base of the cochlea and lower
frequencies being sensed along the spiral towards the apex. For any given sound
frequency, only one specific point of the basilar membrane and organ of Corti is thought
to vibrate and thereby activate the appropriate hair cells to initiate afferent sensory
impulses which then pass to the auditory cortex of the brain. Bending of the stereocilia
of the hair cells results in depolarisation of the cell membrane which, in turn, excites the
sensory nerves which synapse with them.
The sensory input from the cochlea is integrated in the brainstem and auditory cortex,
from which efferent suppressor pathways can modulate receptor activity to enhance
auditory acuity.

EAR
Dr. Rana Mumtaz
Spiral Ganglion:
The spiral ganglion is a spiral-shaped mass of nerve cell bodies lying in a canal at the
extremity of the osseous spiral lamina of the modiolus.
The efferent nerve fibers from the spiral organ of Corti enter the spiral lamina and
converge on the spiral ganglion cells in the modiolus.
The spiral ganglion consists of bipolar neurons whose central processes converge to
form the cochlear division of the eighth cranial nerve.
The vestibular division of the eighth cranial nerve, which receives sensory information
from the maculae of the utricle and saccule and from the ampullae of the semicircular
canals, has a vestibular ganglion situated in the internal auditory meatus.
Vestibule:
Is the central part of the bony labyrinth and lies posterior to the cochlea and anterior to the
semicircular canals. In its lateral wall are the fenestra vestibuli (oval window), which is closed by
the base of the stapes and its annular ligament, and the fenestra cochleae (round window),
which is closed by the secondary tympanic membrane. Lodged within the vestibule are the
saccule and utricle of the membranous labyrinth.
Utricle and Saccule:
The utricle and saccule are two dilated regions of the membranous labyrinth lying within
the vestibule of the inner ear and are joined by the short utriculosaccular duct, which
leads into the slender endolymphatic duct.
Both the utricle and the saccule are filled with endolymph and are suspended in the
perilymph of the vestibule. The walls of each are composed of a fibrous membrane
which is bound down in places to the periosteum of the vestibule and, in other areas, is
attached to the periosteum by fibrous strands, the intervening space being filled with
perilymph .
The utricle and saccule are composed of a thin sheath of connective tissue lined with
simple cuboidal epithelium but in each there is a small region of highly specialized
epithelium called the macula.
These receptors are sensitive to the orientation of the head in relation to gravity or
other acceleration forces.
Maculae in both locations have the same basic histologic structure and consist of a
thickening of the wall and possess two types of receptor cells (type I and type II hair

EAR
Dr. Rana Mumtaz
cells), some supporting cells, and the afferent and efferent nerve endings.
Type I hair cells are polygonal in shape and surrounded by a network of afferent and
efferent nerve endings while Type II hair cells are cylindrical in shape, with basal
synaptic afferent and efferent nerve endings.
Each hair cell possesses on its free surface 40-80 elongated highly specialized microvilli,
or stereocilia, and a single kinocilium which are embedded in a gelatinous membrane
called the otolithic membrane. Within the membrane are numerous crystalline bodies
called otoliths, composed of calcium carbonate crystals.
The supporting cells are tall and columnar, lie on the basal lamina between the hair
cells, Each possesses small microvilli on its free surface and basally located nucleus.
The function of the supporting cells is not known with certainty. The cells may assist in
the nutrition of the hair cells or modify the composition of the endolymph.
Function of the maculae
The function of the maculae relates mainly to the maintenance of balance by providing sensory
information about the static position of the head in space. This is of particular importance when
the eyes are closed or in the dark or under water.
When the head is moved from a position of equilibrium, the otolithic membrane tends to move
with respect to the receptor cells, causing bending of their stereocilia. When the stereocilia are
bent in the direction of the cilium, the receptor cell undergoes excitation and, when the relative
movement is in the opposite direction, excitation is inhibited. The orientation of the hair cells in
different directions in the maculae causes different hair cells to be stimulated with different
positions of the head. The pattern of hair cell stimulation allows the central nervous system to
determine the position of the head very accurately with respect to gravity. The sensory input
from the maculae is integrated with that of other proprioceptors, such as muscle spindles, to
elicit reflex responses directed towards the maintenance of postural equilibrium.
EAR
Dr. Rana Mumtaz
Semicircular Canals:
The three semicircular canals the superior (anterior), posterior, & lateral open into the posterior
part of the vestibule. Lodged within the canals are the semicircular ducts. Each canal has a
swelling at one end called the ampulla (a 1 mm long dilated region of the membranous
labyrinth).
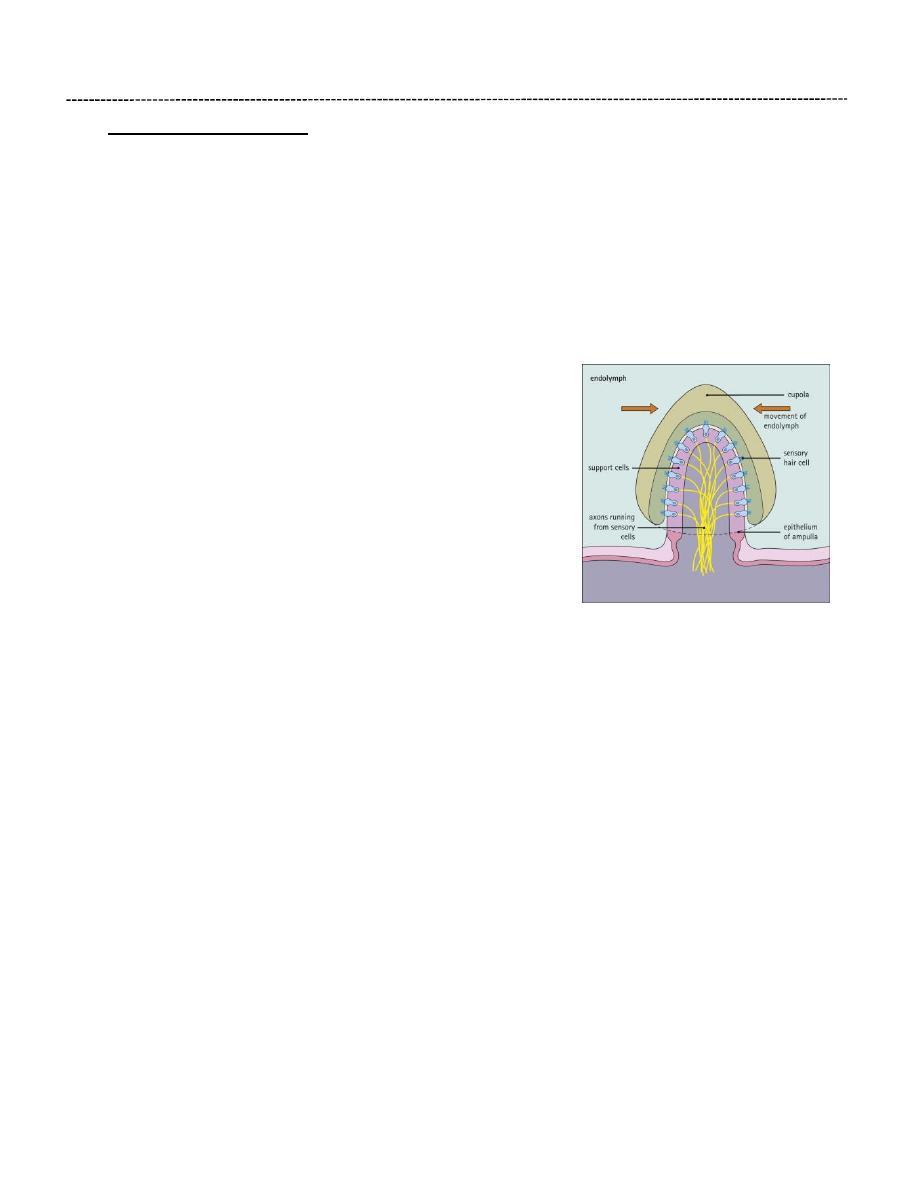
Within the ampullae of the semicircular canals, hair cells are arranged over a finger-like ridge
called the ‘crista ampullaris’. Structurally, the cristae ampullaris bear many similarities to the
maculae of the utricle and saccule. The hair cells are of the same two morphological forms, type
I and type II cells. The hair cells are supported by a single layer
of columnar cells which is continuous with the simple cuboidal
epithelium lining the rest of the membranous labyrinth.
Like those of the maculae, the hair cells of the cristae have
numerous stereocilia and a single kinocilium. The stereocilia
and the kinocilia of the hair cells are embedded in a ridge of
gelatinous glycoprotein which is tall and cone shaped in cross-
section, giving rise to the term cupula. In contrast to the
macula, the cupula does not contain otolithic crystals.
Function of the crista ampullaris
When the head is moved in the plane of a particular semicircular canal, the cupula is deflected
in the opposite direction. The stereocilia of the sensory cells are then deflected towards or
away from the cilia, resulting in excitation or inhibition, respectively. The sensory input from
the cristae ampullaris mainly concerns changes in the direction and rate of movement of the
head. Afferent fibres pass via the vestibular part of the eighth cranial nerve to the brainstem,
cerebellum and cerebral cortex, where sensory information from various other sources is
integrated for the maintenance of balance, position sense and equilibrium.

EAR
Dr. Rana Mumtaz
Discussion points:
The width of the basilar membrane changes such that it is shorter at the base and longer
toward the apex of the cochlea. What is the significance of this change in length?
Is there a difference in the innervation and function of the inner vs. outer hair cells?
The hair cells within the organ of Corti sense sound vibration. Is there any clinical
significance to this other than hearing?
What are the 2 main types of deafness? Where is the lesion in each one?
How do you think cochlear implant is performed?
The vestibular system is important estimate body position. Signals from other parts of
the body also contribute. What are these parts?
Websites:
https://blausen.com/en/topic/ear/
Watch all videos they are very useful.
