DENTAL IMPLANTS’ MATERIALS
Dr. Inas AzizImplants
Definition – A prosthetic device or alloplastic material that is surgically inserted into soft or hard tissues, to be used for functional or cosmetic purposes.Classification of Dental Implants:
Dental implants are classified depending on the placement within the tissues:• Epithelial / mucosal implants
• Epiosteal / Subperiosteal implants
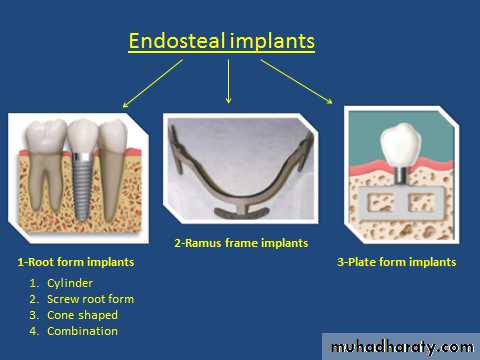
• Endosteal / endosseous implants:
• Plate-form implant
• Ramus-frame implant
• Root-form implant
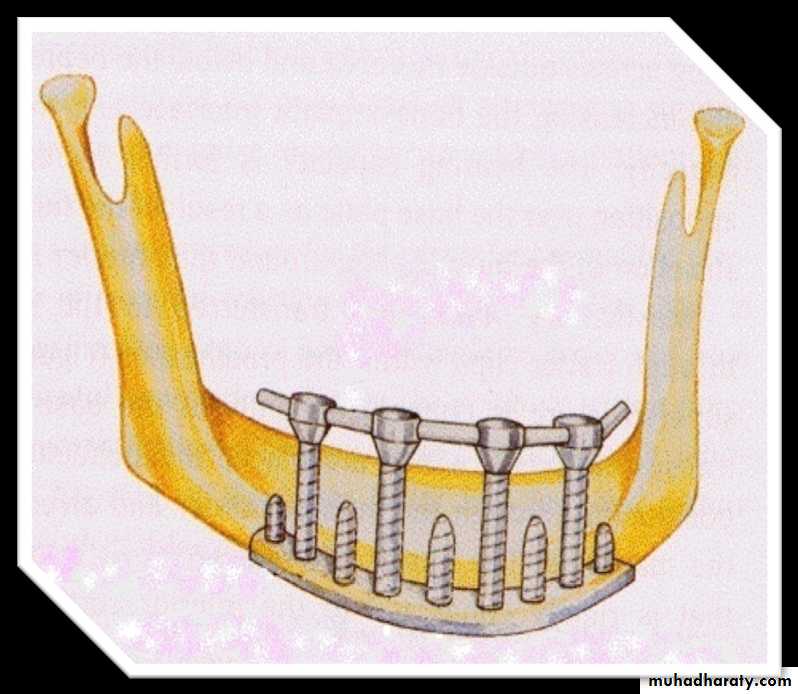
D. Transosteal / transosseous implants
Epithelial / mucosal implants which is inserted into the oral mucosa.
Epiosteal / Subperiosteal implants: which rests upon the bony ridge but does not penetrate it.Endosteal / endosseous implant: Most commonly used which is placed into the alveolar bone/basal bone of maxilla or mandible.
Transosteal / transosseous implants: Penetrates both cortical plates and passes through full thickness of alveolar bone.
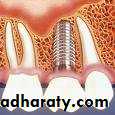
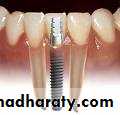
Root form implants
The most popular implants in the world today.come in a variety of shapes, sizes, and materials
can be placed wherever a tooth or several teeth are missing when enough bone is available to accommodate them.
if the bone volume is not sufficient to place Root form Implants, Bone grafting procedures within reasonable limits should be initiated, in order to benefit from these implants.
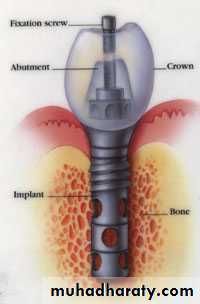
Implant components
Fixture – implant component that engages the bone.( threaded ,grooved ,perforated ,plasma sprayed , or coated.)Transmucosal abutment – provides connection between implant fixture and prosthesis.
Prosthesis .
Requirements of clinical success of dental implants
Individual ,unattached implant is immobile when tested clinically.Radiograph does not demonstrate any evidence of periapical radioluscency.
Vertical bone should be less than 0.2 mm following implant’s first year of service.
Implant performance must be absent of signs and symptoms such as pain, infections, neuropathies, parasthesia or violation of mandibular canal.
Success rate of 85% or more at end of 5 years
Classification of Implant materials
Dental implant materialsmetals
ceramics
CP Titanium and
Ti-6Al-4V alloys
Cobalt alloys
Inert ceramics
Bioactive ceramics
alumina
Carbon
Zirconia
Bioactive glasses and ceramics
Calcium phosphates
polymer
Stainless steel
Non metallic
Metallic implants
Based on the ability of implant to stimulate bone formation around the implant, metallic implants are bio inert materials.
Metallic implants undergo several surface modification to become suitable for implantation.
These modifications include passivation, anodization, ion implantation and texturing.
Titanium is the most commonly used implant material.
Titanium & Titanium Alloys
• Ti-6Al-4V most commonly used. Modulus of elasticity of (Ti-6Al-4V) is closer to that of bone than any other implant material. This ensures a more uniform distribution of stress along the bone-implant interface.• Newer titanium alloys developed include (Ti-13Nb-13Zr) and (Ti-15Mo-2.8Nb) which exhibit greater corrosion resistance.
Advantages:
1. High degree of biocompatibility 2. High strength
3. High corrosion resistance.
Disadvantages:
1. High cost 2. Difficult and dangerous to cast
•
Cobalt-chromium-Molybdenum Alloys:
Elemental composition and function:
• COBALT (63%): provides continuous phase of the alloy
• CHROMIUM (30%): provides corrosion resistance through the oxide surface(Cr2O3).
• MOLYBDENUM (5%): stabilizer; also provides strength and bulk corrosion resistance.
• Traces of CARBON (serves as a hardener), MANGANESE and NICKEL
Advantages :
• Low cost and ease of fabrication
• When properly fabricated , good biocompatibility
• Disadvantages : Poor ductility
Stainless steel
Elemental composition and function:IRON (80%): provides continuous phase of the alloy
CHROMIUM (18%): for corrosion resistance.
NICKEL (8%): to stabilize the austenitic structure.
CARBON (0.05-0.15%): serve as hardener
Advantages:
• It has high strength and ductility, hence is resistant to fracture.
• High Tensile strength
• Ease of fabrication
Disadvantages :
• It cannot be used in Ni sensitive patients
• Susceptible to pit and crevice corrosion
• Galvanic potential
NONMETALLIC IMPLANTS CERAMIC AND CERAMIC COATED IMPLANT MATERIALS:
Ceramics implants are of two types mainly:
• BIO-INERT: aluminium oxide
• BIO-ACTIVE: hydroxyapatite.
GENERAL PROPERTIES OF CERAMICS:
ADVANTAGES :
• Excellent biocompatibility• High compressive strength up to 500 MPa.
• High modulus of elasticity
• Minimal thermal and electrical conductivity
• Color is similar to bone, enamel and dentine
• Chemical composition is similar to constituents of normal biological tissues.
DISADVANTAGES:
• Low mechanical, tensile and shear strength under fatigue loading.
• Variations in chemical and structural characteristics
• Low attachment strengths for some coatings with substrate interfaces.
Ceramic Implant Materials:
Bioinert materials: any material that once placed in the human body has minimal interaction with its surrounding tissue, examples of these are stainless steel, titanium and alumina. Generally a fibrous capsule might form around bioinert implants.
Bioactive materials: a material, which upon being placed within the human body interacts with the surrounding bone and in some cases, even soft tissue. This occurs through a time – dependent kinetic modification of the surface, triggered by their implantation within the living bone. An ion – exchange reaction between the bioactive implant and surrounding body fluids – results in the formation of a biologically active carbonate apatite (CHAp) layer on the implant that is chemically and crystallographically equivalent to the mineral phase in bone. Eg. synthetic hydroxyapatite [Ca10(PO4)6(OH)2], glass ceramic and bioglass.
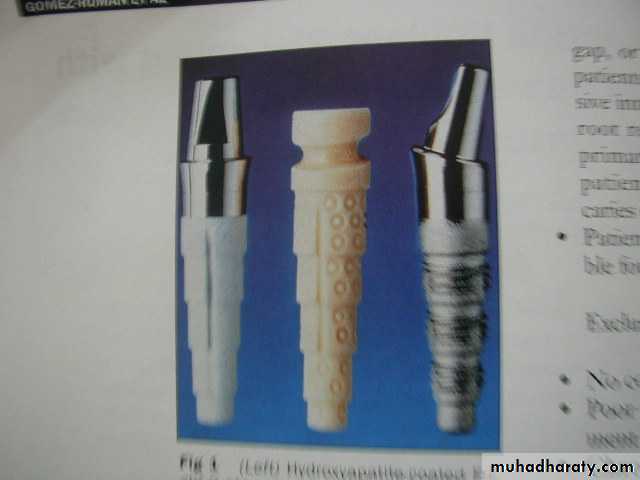
Calcium phosphates (hydroxyapatite HA) : is a bio-active ceramic used as coating materials for metallic implants to promote bone to implant integration.
The more HA coating the more resistant it is to clinical dissolution.
A minimum of 50% crystalline HA is considered an optimal concentration in coating of implants.
• Bioglasses: is bioactive ceramics known to form a carbonated HA layer.
Formation of HA layer is initiated by migration of calcium, phosphate, silica, and sodium ions towards tissue .
Silica gel layer is formed.
Silicon depletion initiates migration of calcium and phosphate ions .
Calcium-phosphorous layer is formed that stimulates osteoblasts to proliferate, stimulating the formation of bone.
very brittle, which makes them unsuitable for use as stress bearing implant materials.
BIO-ACTIVE CERAMIC IMPLANTS :
Polymers
• It is not used nowadays because of low mechanical strength and susceptibility to fracture during function.DISADVANTAGES:
• Low mechanical strength hence susceptible to mechanical fracture
• Physical properties of polymers are greatly influenced by changes in temperature, environment and composition.
• Their sterilization can be accomplished only by gamma irradiation or exposure to ethylene oxide gas.
• Contamination of these polymers because of electrostatic charges that attract dust and other impurities from the environment.
Bone reactions to implants
• It has been accepted that no foreign material placed within a living body is completely compatible. The only substances that conform completely are those manufactured by the body itself (autogenous) and any other substance that is recognized as foreign, initiates some type of reaction (host-tissue response). When a synthetic material is placed within the human body, tissue reacts towards the implant in a variety of ways depending on the material type.Osseointegration : is a "functional ankylosis (bone adherence)", where new bone is laid down directly on the implant surface and the implant exhibits mechanical stability.