
1
Course: Clinical Analysis
Lecturer: Dr. Weam Saad
Lecture: Cells of Inflammation
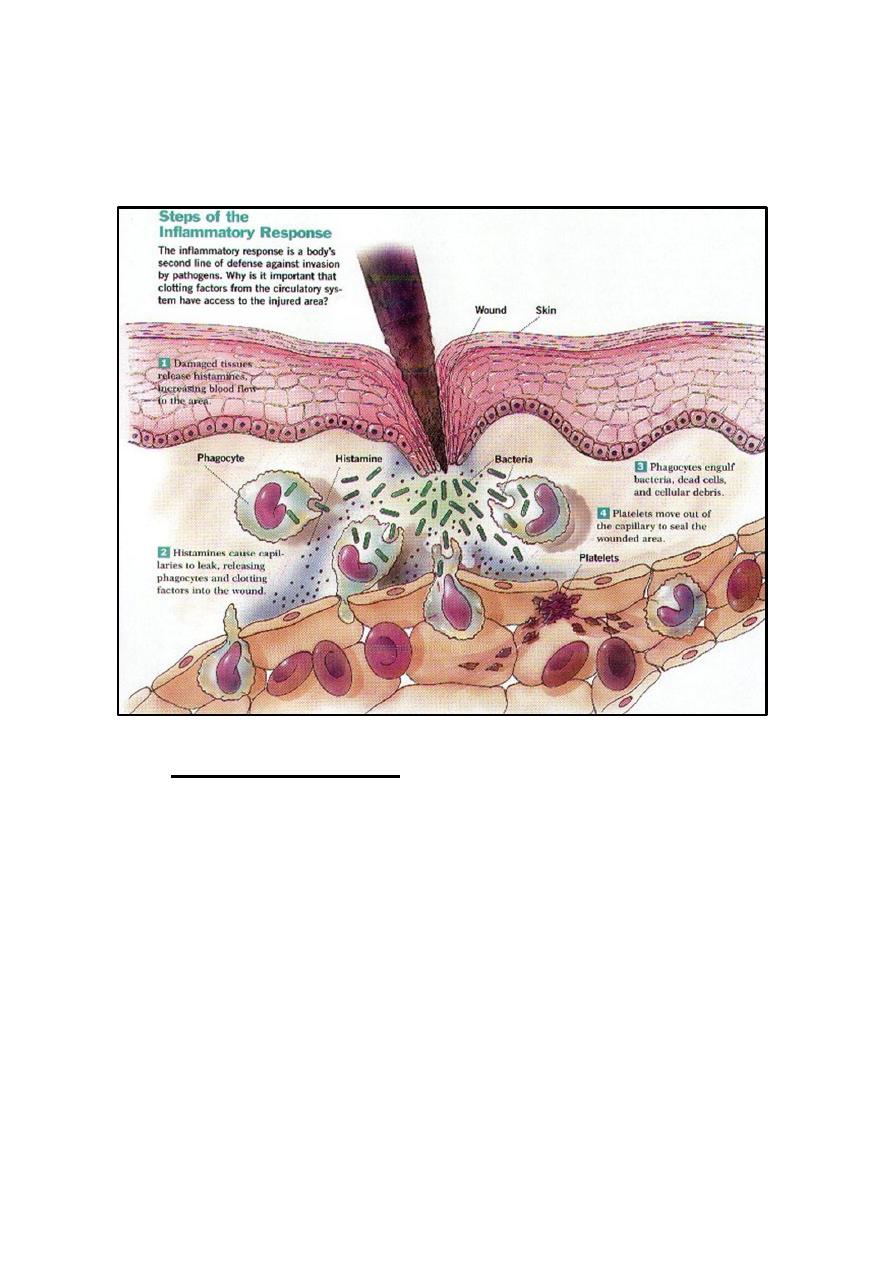
Inflammation
It is the response of living tissues to injury or infection by the help of
the immune system in the site of infection or damage. It is a reaction and
an ordered process mediated by the inflammatory mediators produced by
injured tissues and immune cells. This process consists of four major
events:
1. Increased blood supply to the region.
2. Increased capillary permeability in the affected area (vasodilation).
3. Increase the degree of temperature (fever).
4. Migration of W.B.Cs from the blood vessels into the tissues.
Neutrophils are the first cells reach inflammatory sites followed by
macrophages and lymphocytes in order to generate an immune response.
Inflammatory mediators include; complement system proteins, fibrin,
clotting plasmin, kinin system, prostaglandin, serotonin, histamine, etc. the
function of these mediators is very important to initiate the immune
response.
Importance of inflammation
1. Limitation of the infection and make it localized.
2. Control the infection by stop spreading of infectious
organisms to the surrounding healthy tissues by forming the
fibrin clot around.
3. Activation of the immune system to generate the proper
immune response against the pathogen.
Cells of Inflammation
1. Blood cells
Granulocytes (Neutrophils, Basophils, eusinophils and
Platelets).
Non-Granulocytes (Monocytes, Lymphocytes).

2
2. Tissue cells
Mast cells (specific Basophils).
All fixed macrophages.
Giant cells (group of macrophages united as one giant cell).
Plasma cells.
Types of inflammations
1. Acute inflammation
The most common type of inflammations characterized by swelling,
pain, redness and heat at the site of inflammation due to Odema,
increase blood supply and toxic effects of inflammatory products on
nerves in the site of inflammation the most important sign of acute
inflammation is exudate formation.
Exudate defined as the odema inflammatory liquid forms during
acute inflammations contain high levels of protein, many inflammatory
cells, low glucose, pus and sometimes fibrin clot.
The importance of exudates is:
A. Killing causative pathogen.
B. Dilution of toxins in the site of inflammation.
C. Media for immune response (Abs reaction with Ag).
D. Localization of infection and stop spreading.
Pus: it is the solid components of inflammatory exudates contain living
and dead neutrophils and the debris of dead cells of necrotic tissues.
Steps of Acute inflammation
1. After infection, increase permeability of blood vessels in the infected
site.
2. Formation of exudate which contain proteins (e.g. Albumin,
Globulins, plasmin).
3. Aggregation of RBCs due to conjestion.
4. Migration of PMNs (polymorph nucleus cells) to the site of
inflammation), followed by monocytes by the effect of chemotaxis.

3
5. Revisable vasicular changes.
6. Repair damage: [reabsorbtion of liquids, regeneration of damaged
cells of infected tissues by repair blood vessels and fibroblast cells.
This process is called regernation and that is the end of
inflammation.
NOTE: when the damaged tissue repaired by fibrinous tissue and new
blood vessels from nearby tissues (neighboring tissue), this process is
called granulation tissue formation or scar tissue. This repaired tissue
under microscope look like dotted.
Factors affect the repair are:
1) Neutrition (vit D and C).
2) Medications and drugs e.g. antibiotics increase repair while
cortisone drugs decrease due to prevent new blood vessels
formation.
Microscopic view of acute inflammated tissues:
1) Serous exudates.
2) Large number of PMNs.
3) Large number of monocytes.
4) Fibrin.
Types of acute inflammations:
Acute inflammations can be classified according to the type of exudates
formed as following:
1) Serous inflammation (the exudate is serum e.g.: Tuberculosis).
2) Mucoid or catarrhal inflammation (the exudate is mucous e.g. flue or
influenza).
3) Fibrinous inflammation (the exudate is fibrin. e.g.: Diphtheria,
caused by Corynebacteria diptheriae).
4) Purulent or suppulative inflammation (the exudate is pus and called
abscess.
4
5) Combined Inflammation when there are more than one type of
inflammation like muco-purulent or sero-fibrinous usually occur during
mixed infections.
2.
Chronic inflammation
Occurs when the pathogenic infection last for long time without
treatment or with low immune response or when the pathogen is
intracellular parasite lives inside cells and escape immune system defense
mechanisms and has no Immunogenic antigens, also when the acute
inflammation left without treatment will become chronic inflammation.
Signs of chronic inflammation:
1) Long standing inflammation.
2) Low exudate.
3) Histological changes in tissue (most important sign) e.g.:
Hyperplasia, hypertrophy.

5
Metaplasia and suppress the physiological function, hence giving
immunosuperssor drugs with the therapy in order to avoid these
histological changes for example chronic inflammation in middle ear
(chronic otitis media) lead to hearing loss due to ear drum damage.
3.
Granulomatous inflammation.
Long standing inflammation transformed from chronic inflammation,
occurs due to internal fungal infections and some intracellular bacterial
infections e.g.: Tuberculosis, laprosy, brucellosis, syphilis, when the
pathogenic microorganism hide and escape from host immune system
mechanisms inside cells.
Granuloma: it is the site of this type of inflammation and composed of
nodule containing a giant cell (merge of macrophage cell) in the center
surrounded by epithelial cells and some lymphocytes with fibrin deposited
around these cells.
Lesion: Any abnormality in any tissue caused by any process that damages
tissues or metabolic defects scientists usually depend on lesion formation
during researches for understanding and comparing the effects of harmful
organisms or when testing a new drug or treatment for example on
laboratory animals.
