
HYDROCEPHALUS

Hydrocephalus
• A syndrome, or sign, resulting from
disturbances in the dynamics of
cerebrospinal fluid (CSF), which may
be caused by several diseases.
Incidence
• Occurs in 3-4 of every 1000 births.
• Cause may be congenital or acquired.
• Congenital- may be due to
maldevelopment or intrauterine infection
• Acquired- may be due to infection,
neoplasm or hemorrhage.

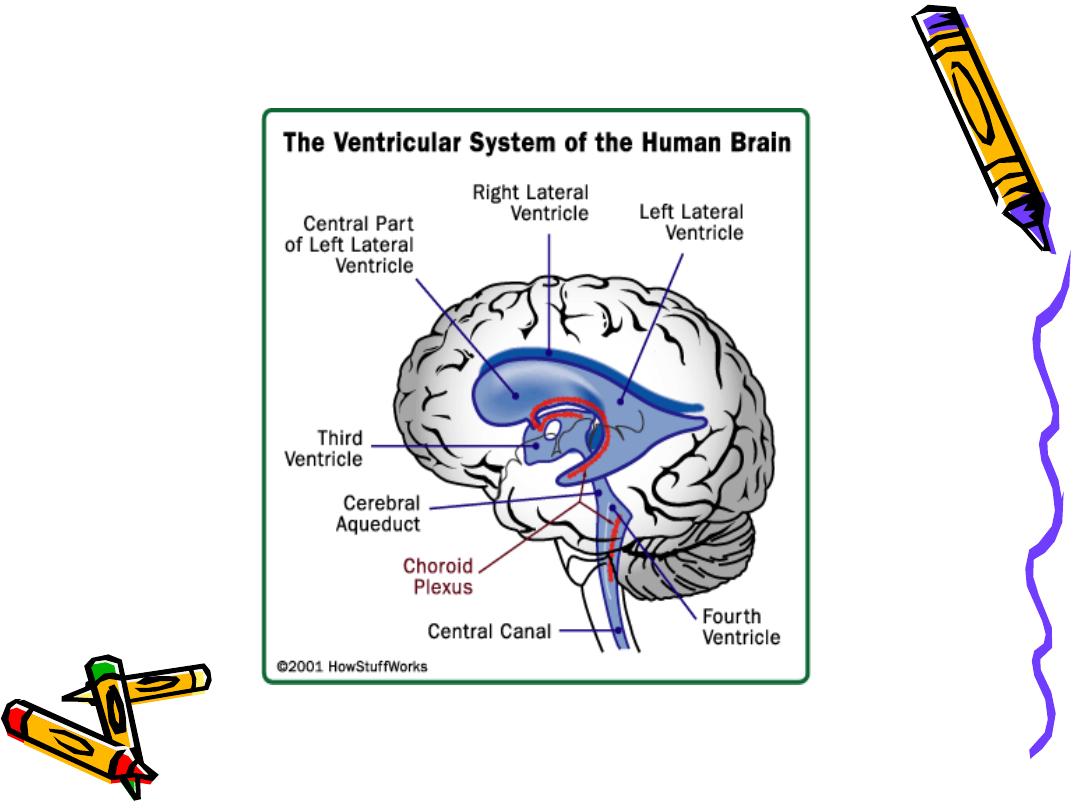
Pathophysiology
• CSF is formed by two mechanisms:
– Secretion by the choroid plexus,
– Lymphatic-like drainage by the extracellular
fluid in brain.
CSF circulates thru ventricular system and is
absorbed within subarachnoid spaces by
unknown mechanism.

Mechanisms of Fluid
Imbalance
• Hydrocephalus results from:
• 1. Impaired absorption of CSF within the
subarachnoid space (communicating
hydrocephalus), or
• 2. Obstruction to the flow of CSF through
the ventricular system (non-communicating
hydrocephalus)

Mechanisms of fluid
imbalance
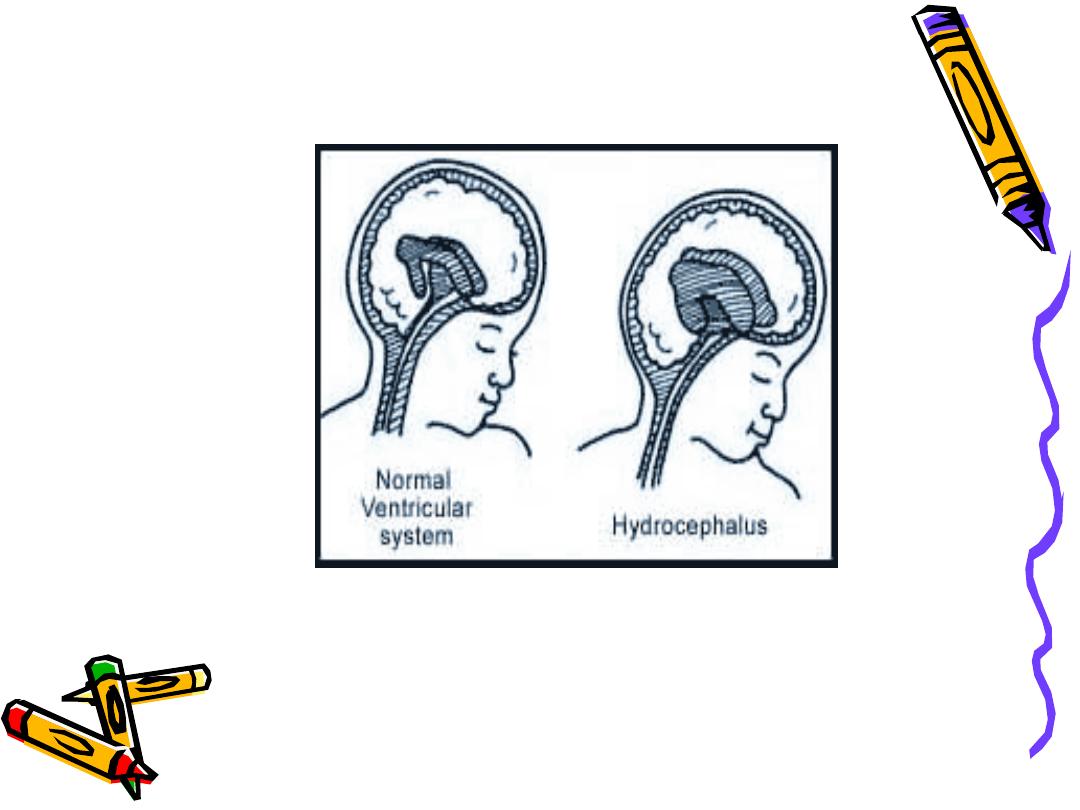
• Both lead to increase accumulation of CSF in
the ventricles!
• Ventricles become dilated and compress the
brain.
• When this happens before cranial sutures are
closed, skull enlarges.
• In children <10-12, previously closed sutures
may open.

Hydrocephalus
• Most cases of non-communicating
(obstructive) hydrocephalus are a result of
developmental malformations.
• Other causes: neoplasms, intrauterine
infections, trauma.
• Developmental defects account for most
causes of hydrocephalus from birth to 2
years of age.

Common Defects
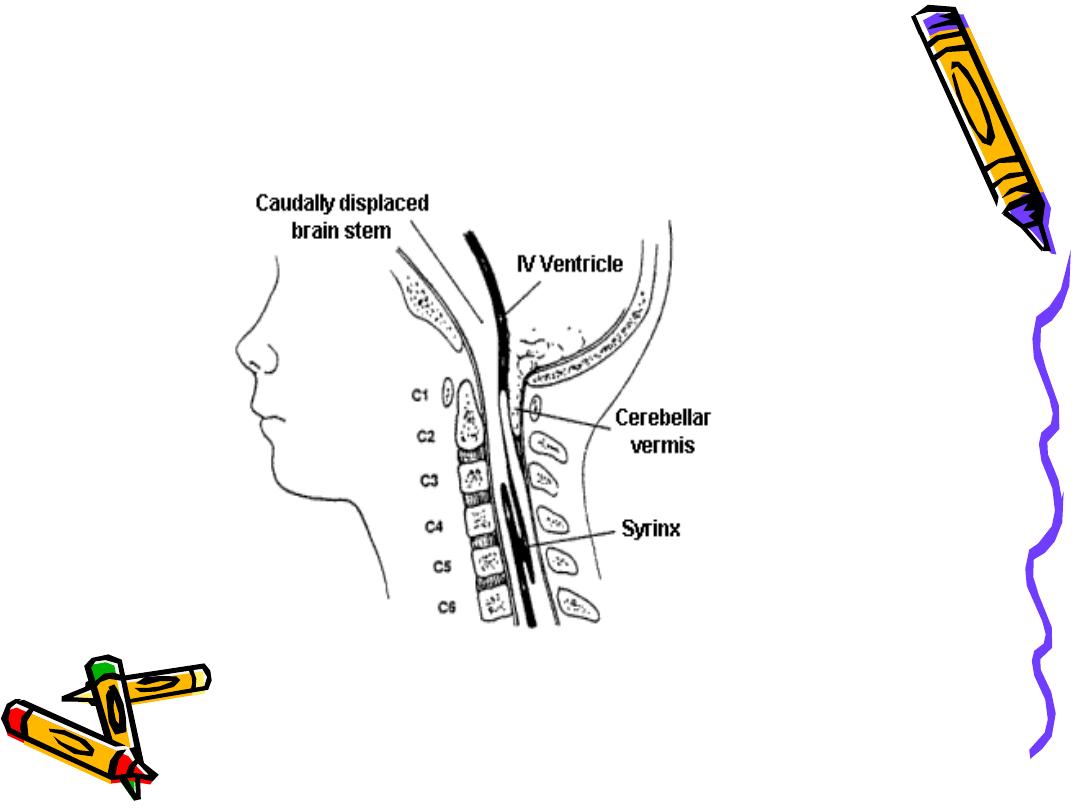
• Arnold-Chiari Malformation (ACM)
– Type 2 malformation of brain seen most
exclusively with myelomeningocele, is
characterized by herniation of a small
cerebellum, medulla, pons, and fourth
ventricle into the cervical spinal canal
through an enlarged foramen magnum.

Clinical manifestations
• Clinical picture depends on acuity of
onset and presence of preexisting
structural lesions.

Infancy
• Head grows at alarming rate with
hydrocephalus.
– First signs- bulging of fontanels without head
enlargement.
– Tense, bulging, non-pulsatile anterior fontanel
– Dilated scalp veins, esp. when crying
– Thin skull bones with separated sutures
(cracked pot sounds on percussion)
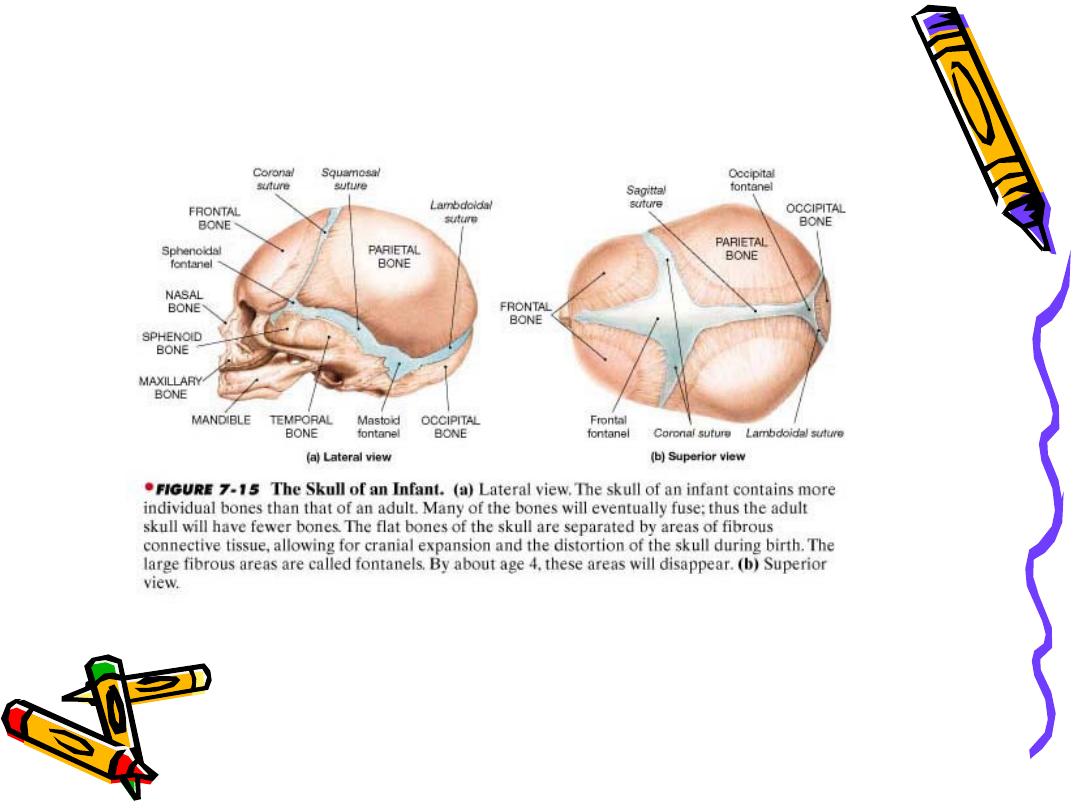

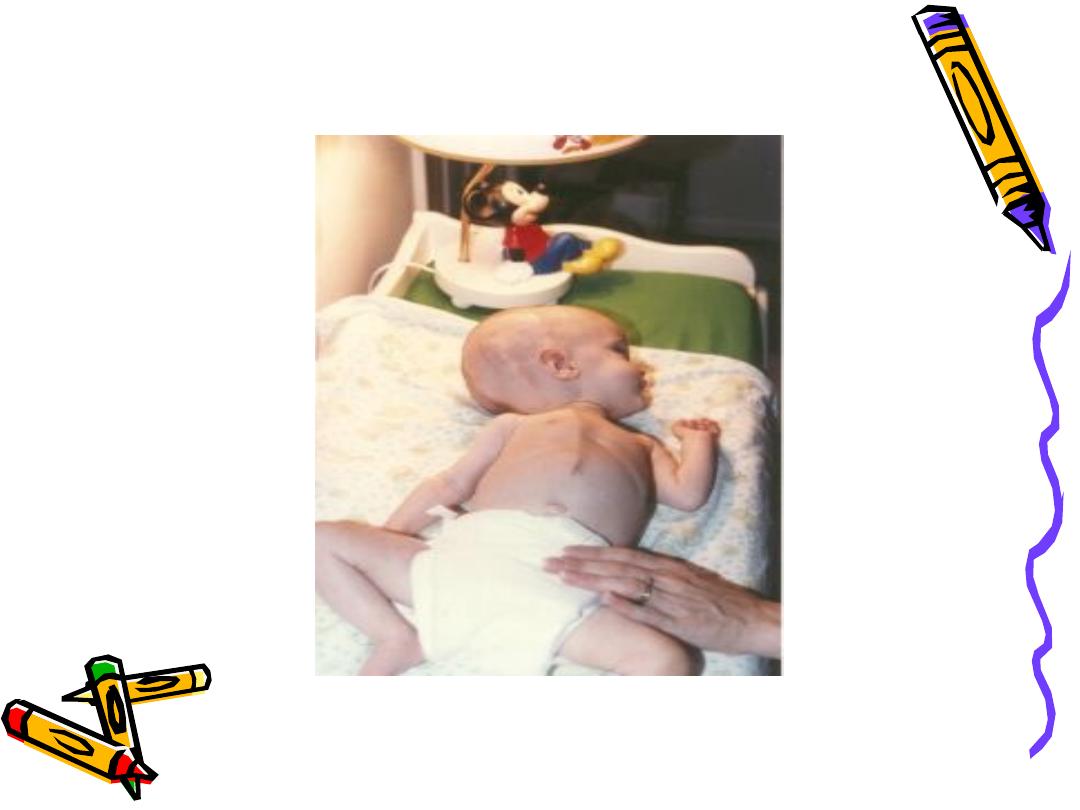

Infancy
• Protruding forehead or bossing.
• Depressed eyes or setting-sun eyes (eyes rotating or
downward with sclera visible above pupil)
• Pupils sluggish with unequal response to light
• Irritability, lethargy, feeds poorly, changes in LOC,
arching of back (opisthotonos), lower extremity
spasticity.
• May cry when picked up or rocked; quiets when allowed
to lay still.

Infancy
• Swallowing difficulties, stridor, apnea,
aspiration, respiratory difficulties and arm
weakness may indicate brain stem
compression.
• If hydrocephalus progresses, difficulty
sucking and feeding, and a high-pitched shrill
cry results. (lower brain stem dysfunction)

Infancy
• Emesis, somnolence, seizures, and
cardiopulmonary distress ensues and
hydrocephalus progresses.
• Severely affected infants may not
survive neonatal period.
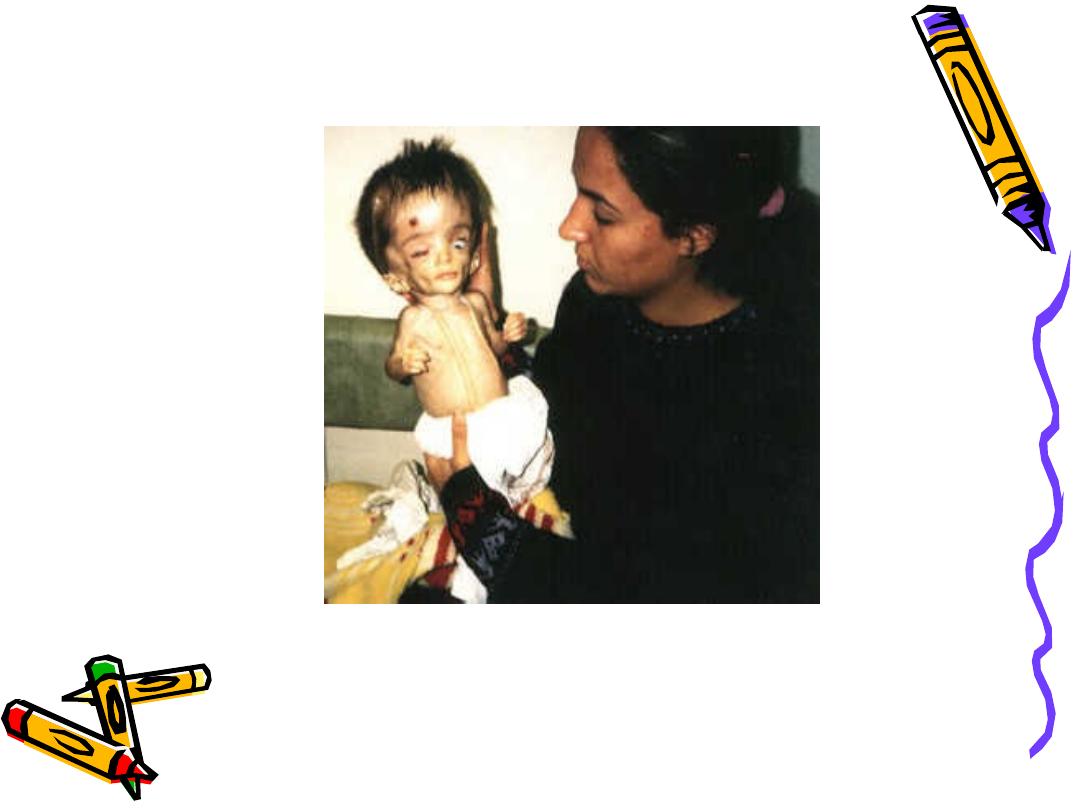

Childhood
• Signs and symptoms caused by
increased ICP.
• Manifestations caused by posterior
neoplasms and aqueduct stenosis,
manifestations associated with space-
occupying lesions.

Childhood
• Headache on awakening with improvement
following emesis or sitting up.
• Papilledema (swelling of optic disc),
strabismus, and extrapyramidal tract signs
such as ataxia
• Irritability, lethargy, apathy, confusion, and
often incoherent
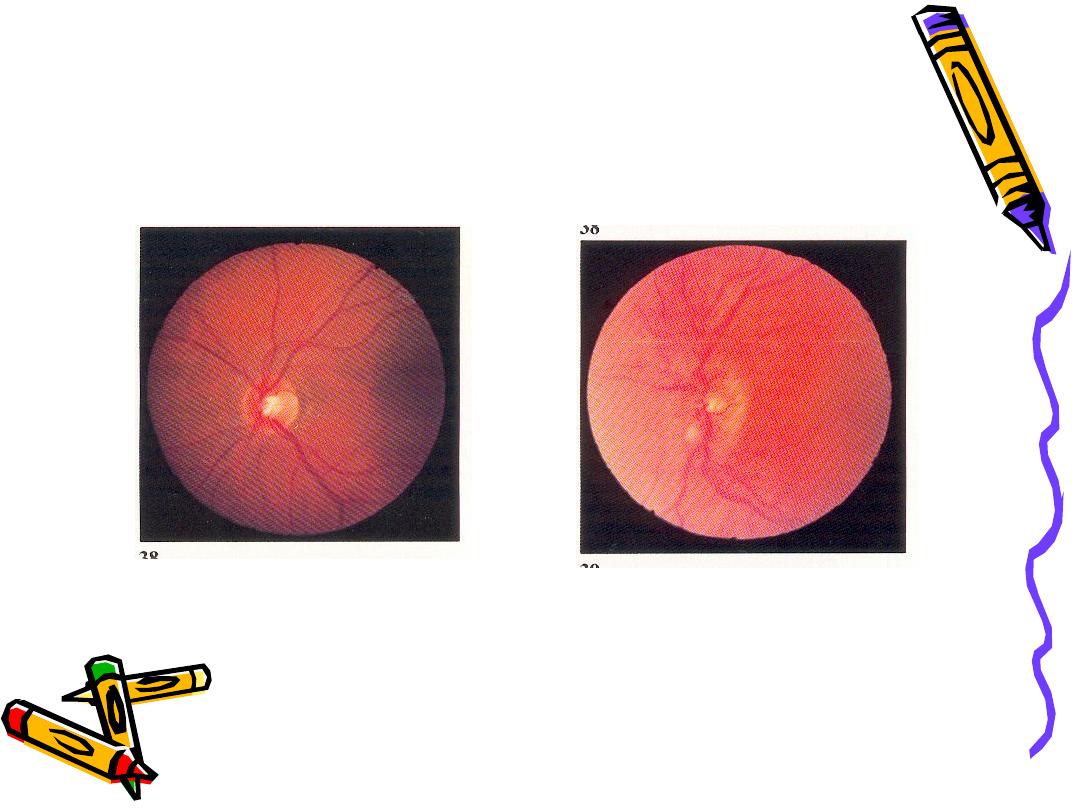

Childhood
• Dandy-Walker syndrome- congenital defect-
late onset.
– Obstruction of foramen of Lushka and
Magendie
– Bulging occiput, nystagmus, ataxia, cranial nerve
palsies
– Female predominance (3:1)
– Absence or occlusion of ventricles

Diagnostic Evaluation
• Antenatal- fetal ultrasound as early as 14
weeks
• Infancy- based on head circumference crosses
one or more grid lines on the infant growth
chart within a 4 week period and there are
progressive neuro signs.
• CT and MRI to localize site of obstruction;
reveal large ventricles

Therapeutic management
• Goals:
• Relieve hydrocephaly
• Treat complications
• Manage problem resulting from effects
of disorder on psychomotor development
• USUALLY SURGICAL!

Surgical Treatment
• Therapy of choice!
• Direct removal of source of obstruction
(neoplasm, cyst, or hematoma)
• Most require shunt procedure to drain CSF
from ventricles to extracranial area; usually
peritoneum(VP shunt), or right atrium (VA
shunt) for absorption.
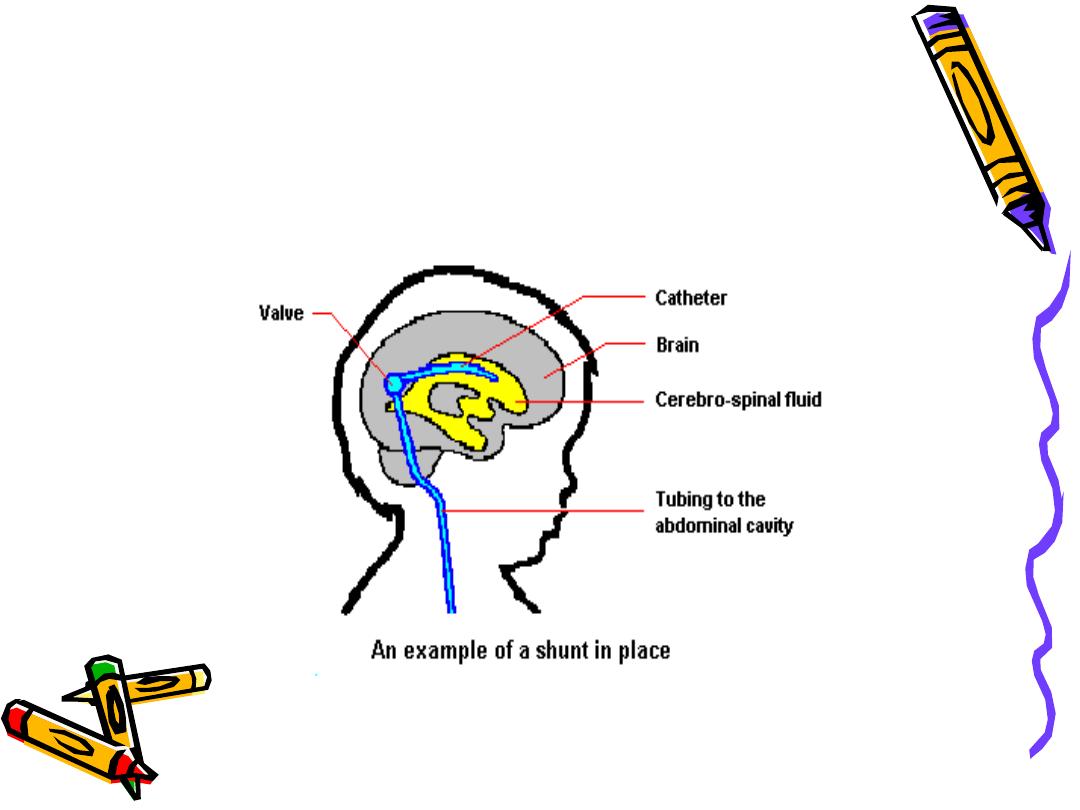

VP shunt
• Used in neonates and young infants
• Greater allowance for excess tubing;
which minimizes number of revisions
needed as child grows


VA shunt
• Reserved for older children who have
attained most of somatic growth, or
children with abdominal pathology.
• Contraindicated in children with
cardiopulmonary disease or with
elevated CSF protein.
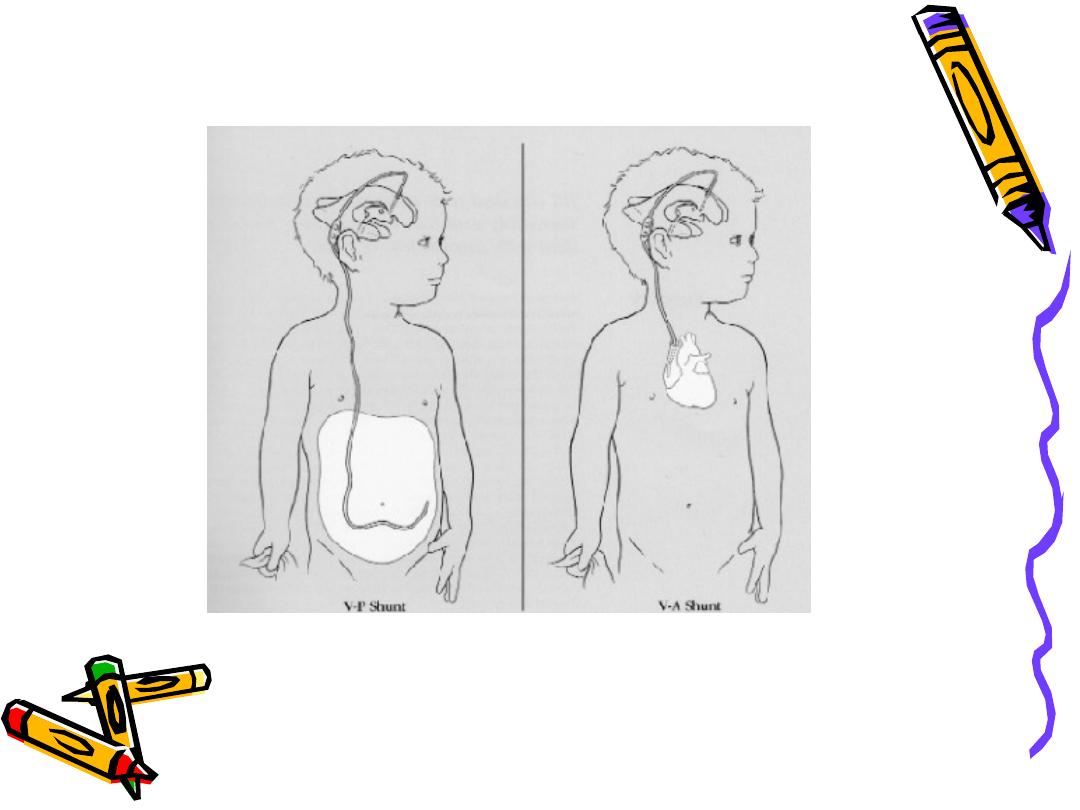
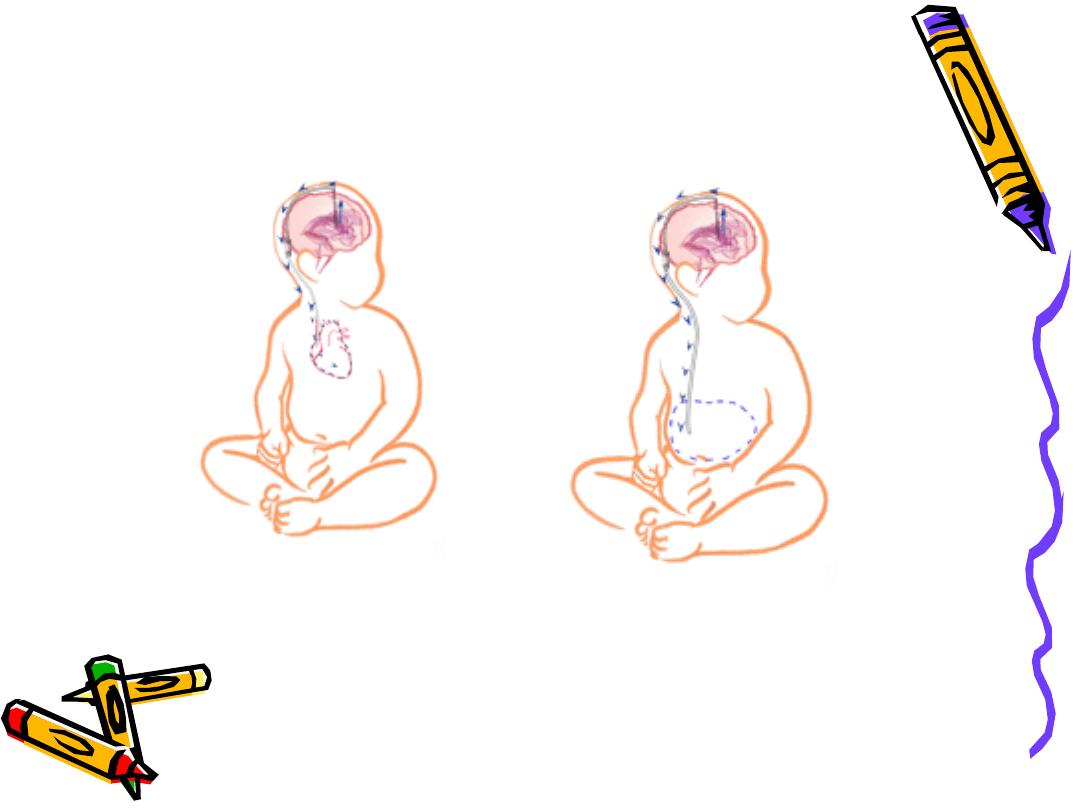

Major Complications
• Shunt infection is most serious
complication!
• Period of greatest risk is 1 to 2
months following placement.
• Staph and strep most common
organisms

Complications
• Mechanical difficulties
kinking, plugging, migration of tubing.
• Malfunction is most often by mechanical
obstruction!
• Look for signs of increased ICP; fever,
inflammation and abdominal pain.

Post-op care
• In addition to routine post-op care:
– 1. Place on unoperated side to prevent pressure
on shunt valve
– 2. Keep HOB flat; rapid decrease in IC fluid
may cause subdural hematoma due to small vein
rupture in cerebral cortex.
– 3. Do not pump shunt without specific
direction from doctor (too many different
pump devices)

Post-op care
• 4. Observe for signs of Increased ICP! May
indicate obstruction of shunt!
– Assess pupil size; as pressure on oculomotor
nerve may cause dilation on same side as
pressure.
– Blood pressure may be variable due to hypoxia
to brainstem
– Abdominal distention- due to CSF peritonitis or
post-op ileus due to catheter placement.

Post-op
• 5. Monitor I and O- may be on fluid
restriction or NPO for 24 hours to prevent
fluid overload.
• 6. Monitor VS- increased temp may indicate
infection.
• 7. Give good skin care to prevent tissue
damage, etc.

Family support
• Fear
• Communication of procedures
• Prepare for discharge.
