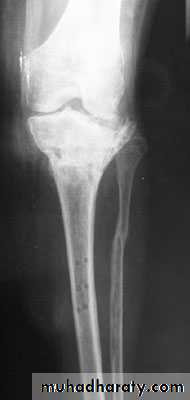
Complications of fractures
There are pathologies other than the loss of bone continuity which either co exist or originate due to the fracture.early diagnosis and aggressive treatment is necessary to minimize disabilities.
Immediate complicationsEarly complications :
Late complications :Delayed union
Mal union
Non union
Avascular necrosis
Shortening
Joint stiffness
Sudeck’s astrophy
Osteomyelitis
Ischemic contracture
Myositis ossificans
Degenerative arthritis ( osteoarthritis )
Hypovolaemic shock :
Commonest cause of death in fractures of major bones Like pelvis or femurExteral or internal bleeding and veceral injuries are the main causes of shock.
Fracture femural shaft = 1 – 1.5 L of blood
Fracture pelvic ring = 1.5 – 2 L of blood
Treat the cause , start IV fluid and blood , stabilize the fracture.
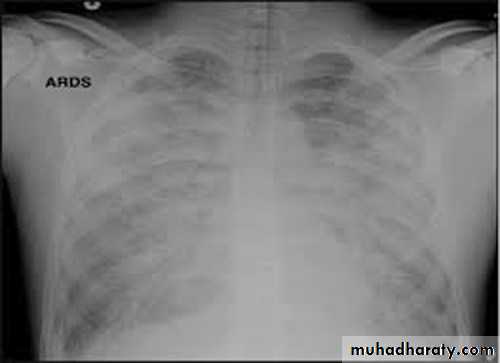
ARDS ( acute respiratory distress syndrome )
The cause is not definite. Hypothesized to be by release of Inflammatory cells and proteinaceous fluid that accumulate in the alveolar spaces leading to a decrease in diffusing capacity and hypoxemia. Usually within the first 24 hours after injury.Clinical features :
-Tachypnea , hypoxia
-X- ray- diffused pulmonary infiltrates
Treatment is by 100% O2 and assisted ventilation
• If not detected early and treated , death may occurs by multiorgan failure or cardiorespiratory failure.
Fat embolism
It is a life threatening complication of fracture where fat globules occlude the small blood vessels. Usually occur 48 – 72 hrs from the injury.Pathogenesis : 3 theories
• release fat globule from the fractures bone marrow to blood stream.
• fat can also be released from the adipose tissue.
• Fat is converted to free fatty acid , which induces toxic vasculitis followed by thrombosis which obstruct the microvasculature.
Clinical features of fat embolism :
Patechial rash of anterior neck, anterior axillary fold or conjunctivaDrowsiness Restlessness Disorientation Coma
Tachypnoea Tachycardia , hypoxia
Dx : Urine: fat globules CXR: pulmonary infiltration\Snow storm appearance ( not always )
Treatment of fat embolism: (supportive treatment)
ventelation supportheparin
corticosteroeds
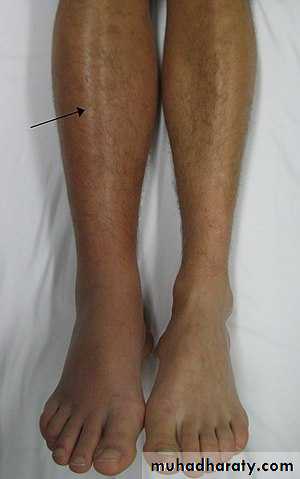
Thrombo-embolism :
Include leg veins thrombosis (DVT ) and pulmonary emboism
a common complication especially in pelvic and spinal injuries. Usually 3 – 5 days from the injury .
Pathogenesis : Virchow's triad
• Venous blood stasis
• damage to the blood vessel wall
• hypercoagulability
Diagnosis :
Clinical features leg pain , redness , sweling and pain , or feature of pulmonary embolism.D-dimers
doppler ultrasound
venography ( the gold standard )
Treatment of thrombo embolism :
Prophylaxis : mechanical and chemical ( medications)therapeutic anticoagulants and thrombolytics
Early surgical stabilization to start early movement of the limb and patient.
Tetanus
Is a potentially fatal disease that is preventable by appropriate immunization
caused by clostredium tetani , which is anaerobic, gram-positive spore forming bacilli found in fecal matter of animals and humans.
Risk factors : Deep wounds without exposure to air, Wounds containing ischemic tissues, No immunization, Improper sterilization
Clinical features :
Prodromal symptoms like headache and restlessness. Trismus or lock jawDysphagia and Neck rigidityRigidity of back muscles (Risus sardonicus)May end with convulsion
Sustained spasm of laryngeal and respiratory muscles may cause asphyxia and death.
Prevention :
Immunizationremoval of soil, foreign body and necrotic tissue.
Tetanus antitoxin (ATS)
Management :
Tracheostomy if breathing difficult ( may need ET tube ventilation ).Managed by heavy sedation to avoid spasms and convulsions.
During this period adequate nutrition, care of bladder and bowel
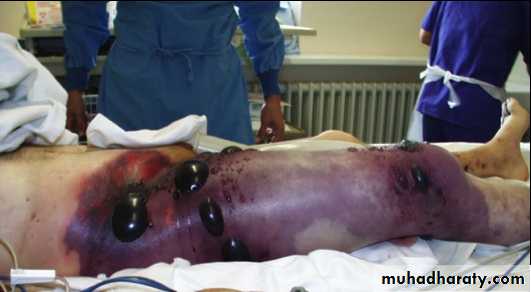
Gas gangrene :
terrifying condition is produced by Clostridium prefrengens , an anaerobic organisms that can survive and multiply in a dirty wound with dead muscle that has been closed without adequate debridement.
Toxins produced by the organisms destroy the cell wall and rapidly lead to tissue necrosis .
Clinical features
appear within 24 hours of the injury with intense pain and swelling around the wound and a brownish discharge may be seen. little or no pyrexia but the pulse rate is increased and a characteristic smell becomes evident.Rapidly the patient becomes toxemic and may end with coma and death.
Prevention
- Deep, penetrating wounds in muscular tissue are dangerous , they should be explored,all dead tissue should be completely excised
the wound should be left open.
Treatment
The key to life-saving treatment is early diagnosis.General measures, such as fluid replacement and intra- venous antibiotics, are started immediately.
Hyperbaric oxygen has been used
the mainstay of treatment is prompt decompression of the wound and removal of all dead tissue.
In advanced cases, amputation may be essential.
Crush syndrome:
Definition : renal failure following extensive crushing injury of muscles.
Pathogenesis:
Crushing of muscles causes entry of myoglobin into circulation. Myoglobin precipitates in renal tubules causing acute tubular necrosis, metabolic acidosis & hyperkalemia
Clinical features(appear within 2-3 days of injury) , Oliguria (Scanty urine) , Restlessness , Cardiac arrhythmia ,Shock
Treatment :
As acute renal failure : fluid with diureticsAl kalinazaion of urin by sodium bicarbonates
Infection
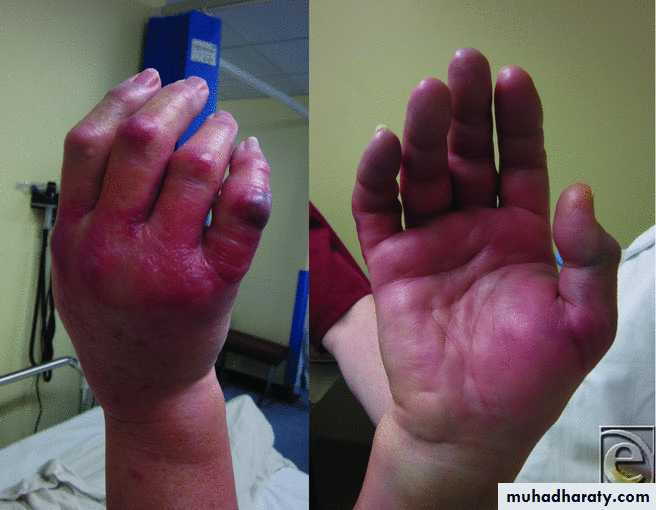
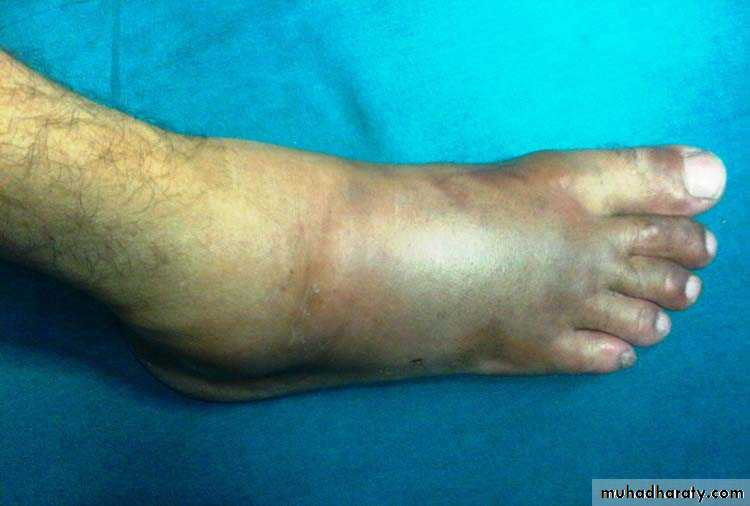
Open fractures may become infected; closed fractures hardly ever do unless they are opened by operation.Compartment syndrome
A devastating complication of fracture or other kind of injuries .Definition : An increased pressure within enclosed osseo-fascial space that reduces capillary perfusion below level necessary for tissue viability ( especially the nerve and muscle tissues )
Causes:
Trauma ( fracture or crushing injuries )
Bleeding disorders
Burns
Tight wraps and casts
Leakage of iv fluid infusion .
Diagnosis :
Tense compartment
Severe pain out of proportion to the injury
Pain to the passive stretch of muscle (the earliest sign)
5 Ps : pain , parasthesia , pallor , pulselessness ,paralysis , poikilothermia ( late signs )
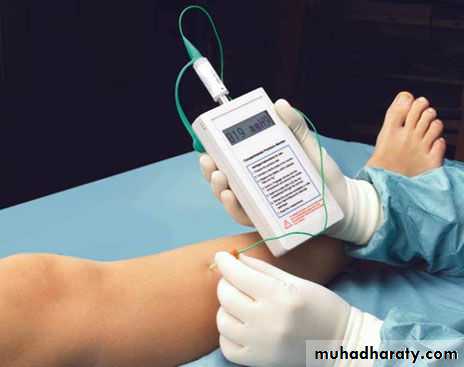
Compartment pressures :
> 30 mmHg or within 20 mmHg from the diastolic BP indicate abnormal compartment pressure and necessitate faciotomy.
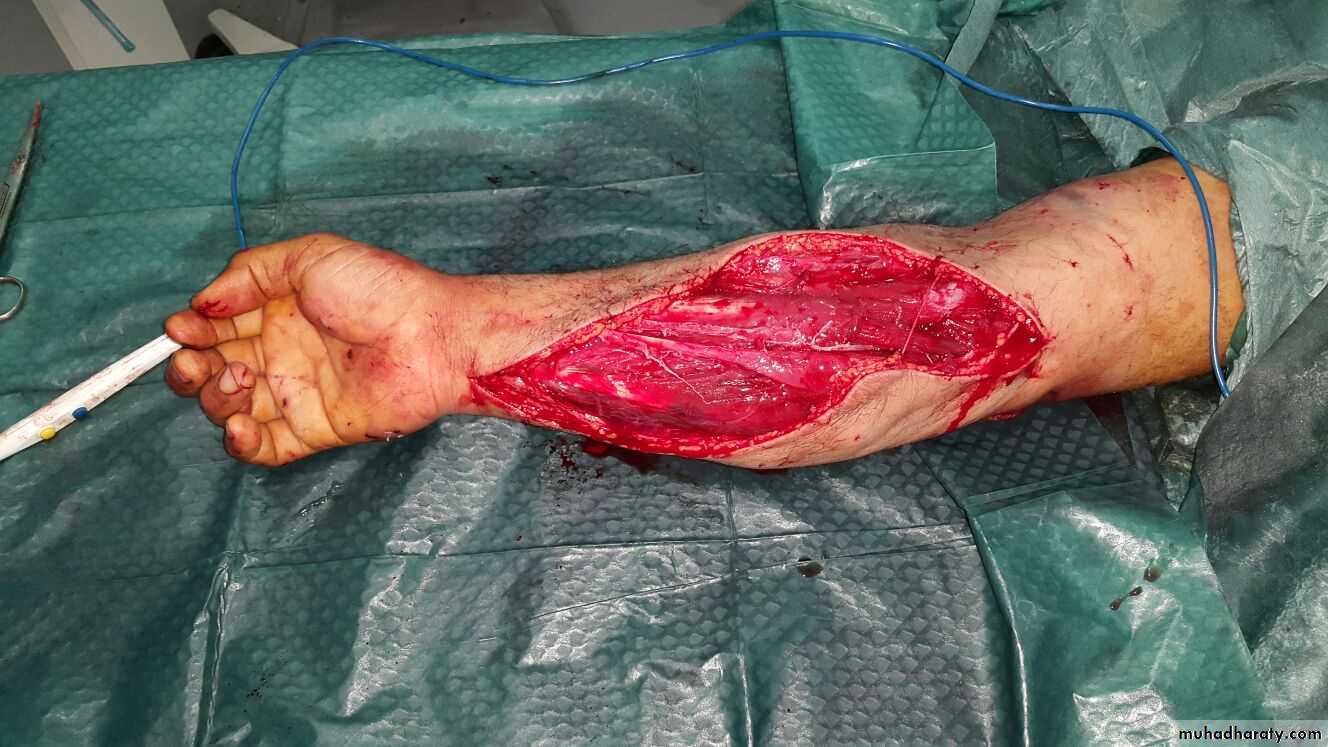
Treatment :
Leg should be put and the level of the heartRemove cast and Split all dressings down to skin
Fasciotomy if continued clinical findings and/or elevated compartment pressure
Late complications
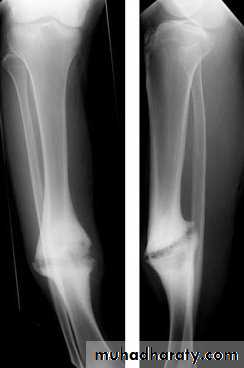
Delayed union and non union :When the fracture takes more time than expected to unite then it is delayed union
When the fracture fail to unite . For diagnosis of non union , 6 months of follow up should pass without clinical and\or radiological signs of union.
Causes :
Biological : - inadequate blood supply- severe soft tissue damage
- excessive periosteal stripping
- infection
Biomechanical : - inadeqaute reduction
- unstable fixation
- infection
Patient related : - medical conditions like DM
- non compliant patient
diagnosis
Delayed union : fracture tenderness persist , fracture line in the xray with very little or no callus
Non union : pain diminished , movement in the fracture site (pseudarthrosis or pseudojoint ) , xray show atrophic or hypertrophic bone ends
Treatment :
Delayed union : look for and treat the cause .Non union : treated mainly by surgical fixation with bone graft ( in Atrophic non union or without bone graft in cased of hypertrophic
Non union.
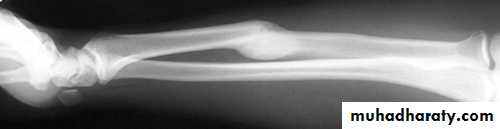
Malunion:
When the fragments join in an unsatisfactory position (unacceptable angulation, rotation or shortening) the
fracture is said to be malunited.
Causes are failure to reduce a fracture adequately, failure to hold reduction while healing proceeds
Treatment of malunited fracture:
In adults, Angulation of more than 10–15 degrees in a long bone or a noticeable rotational deformity may need correction by re- manipulation, or by osteotomy and fixation .In children, angular deformities near the bone ends (and especially if the deformity is in the same plane as that of movement of the nearby joint) will usually remodel with time; rotational deformities will not
Shortening malunion may be treated by bone lengthening procedure.
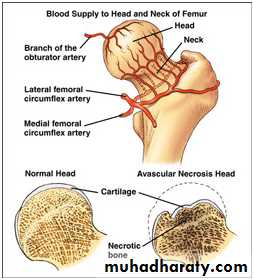
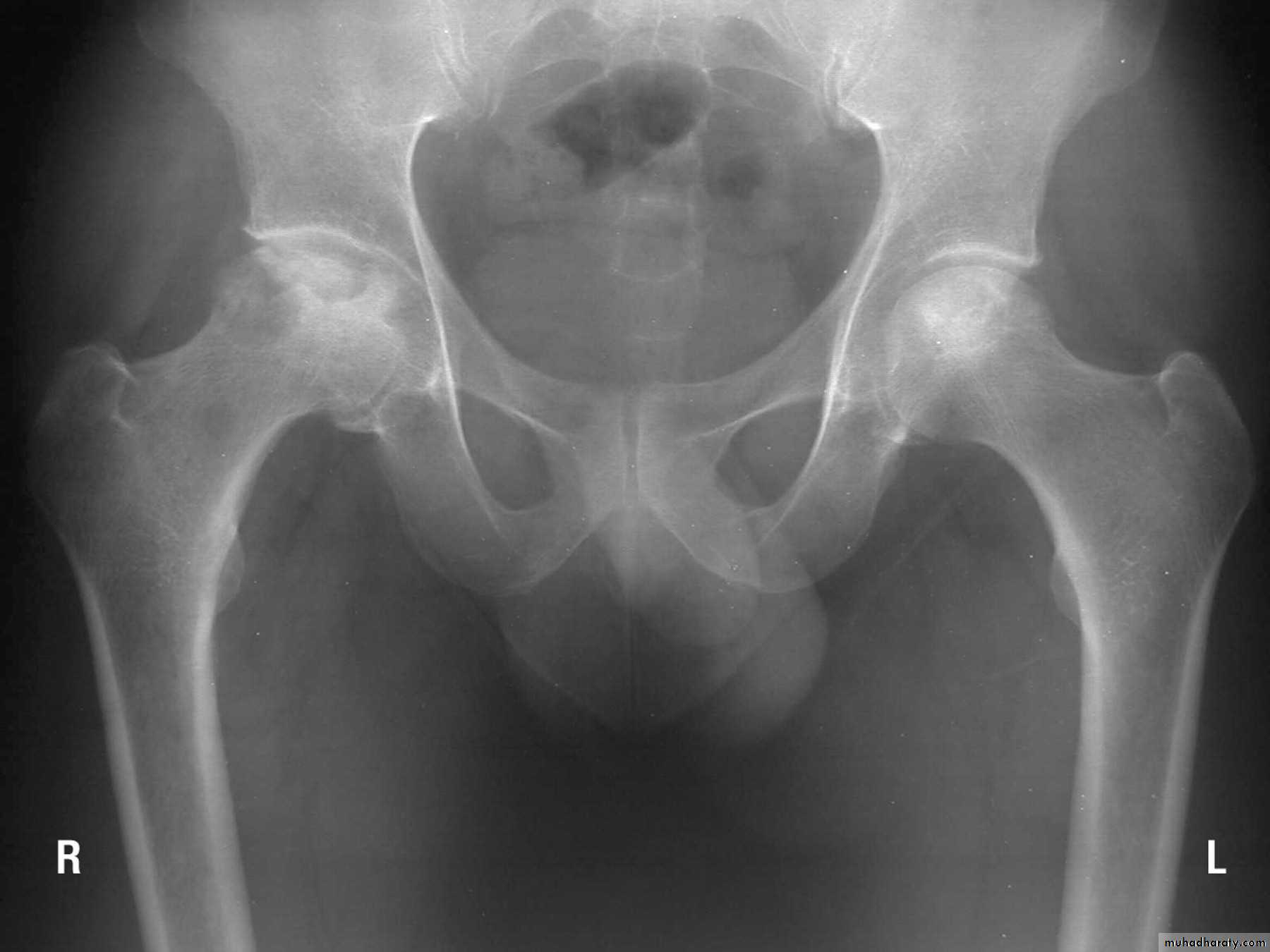
Avascular necrosis :
Certain regions are problematic for their tendency to develop ischemia and bone necrosis after injury.They are:
- the head of the femur (after fracture of the femoral neck or dislocation of the hip);
- the proximal part of the scaphoid (after fracture through its waist);
- the body of the talus (after fracture of its neck).
Accurately speaking, this is an early complication of bone injury, because ischemia occurs during the first few hours following fracture or dislocation.
However, the clinical and radiological effects are not seen until weeks or even months later.
Clinical features of AVN :
Painincreased bone density in the radiography
Treatment :
Femoral head AVN – total hip arthroplasty or arthrodesis
Scaphoid or talus – conservative treatment or joint arthrodesis
Joint stiffness :
commonly occurs in the knee, elbow, shoulder and (worst of all) small joints of the hand.due to oedema and fibrosis of the capsule, ligaments and muscles around the joint, or adhesions of the soft tissues to each other or to the underlying bone.
made worse by prolonged immobilization
What is important is to prevent stiffness and to insist on skilled physiotherapy until normal function is restored.
Treatment of joint stiffness :
Extensive physiotherapy
Arthroscopic release of adhesions
Open surgical release of adhesions ( ex. Stiff knee )
Sudeck’s atrophy :
Algodystrophy , reflex sympathetic dystrophy , complex pain regional syndrome ( all refer to same entity )C.F. : continuous ‘ burning ‘ pain. local swelling, redness and warmth, and tenderness.
After few weeks the skin becomes pale and atrophic, movements are increasingly restricted.
X-rays characteristically show patchy rarefaction of the bone.
Treatment :
Elevation and active exercises are essential to prevent and to treat CRPS.- antiinflammatory drugs and adequate analgesia are helpful.
- use of drugs like amitriptyline, carbamazepine , gabapentin and calcium channel blockers may help.
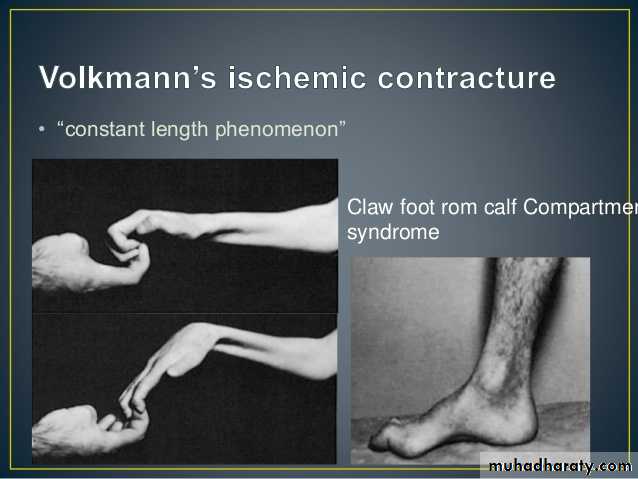
Ischemic contracture :
Following arterial injury or compartment syndrome, the patient may develop ischaemic contractures of the affected muscles (Volkmann’s ischaemic contracture).The sites most commonly affected are the forearm and hand, leg and foot.
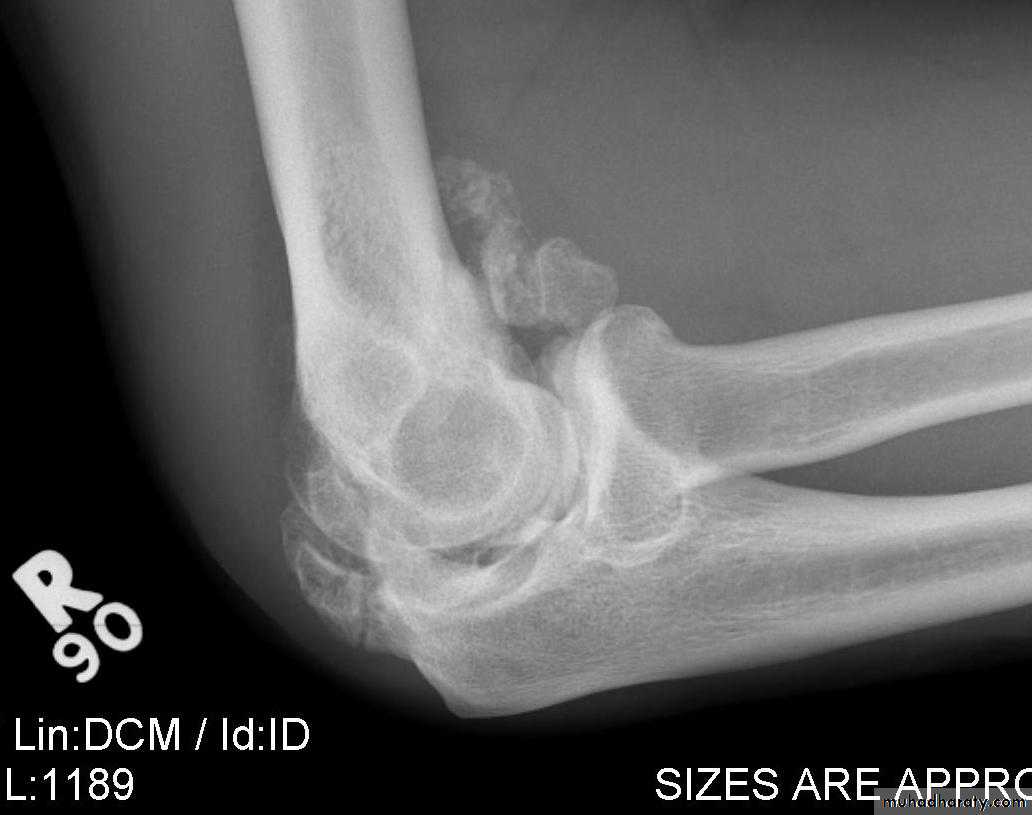
Myositis ossificans :
Heterotopic ossification in the musclesCommon sites : elbow or a blow to the brachialis, deltoid or quadriceps. especially in unconscious or paraplegic patients
x-ray may show fluffy calcification in the soft tissues.
The joint should be rested in the position of function until pain subsides; gentle active movements are then begun.
Months later, when the condition has stabilized, it may be helpful to excise the bony mass.
Indomethacin or radiotherapy should be given to help prevent a recurrence.
Degenerative arthritis (osteoarthritis ) :
A fracture involving a joint may severely damage the articular cartilage and give rise to post-traumatic osteoarthritis.Even if the cartilage heals, irregularity of the joint surface may cause localized stress and so predispose to secondary osteoarthritis years later..