L1
Anatomy of Female Genital Tract
D. Wsn
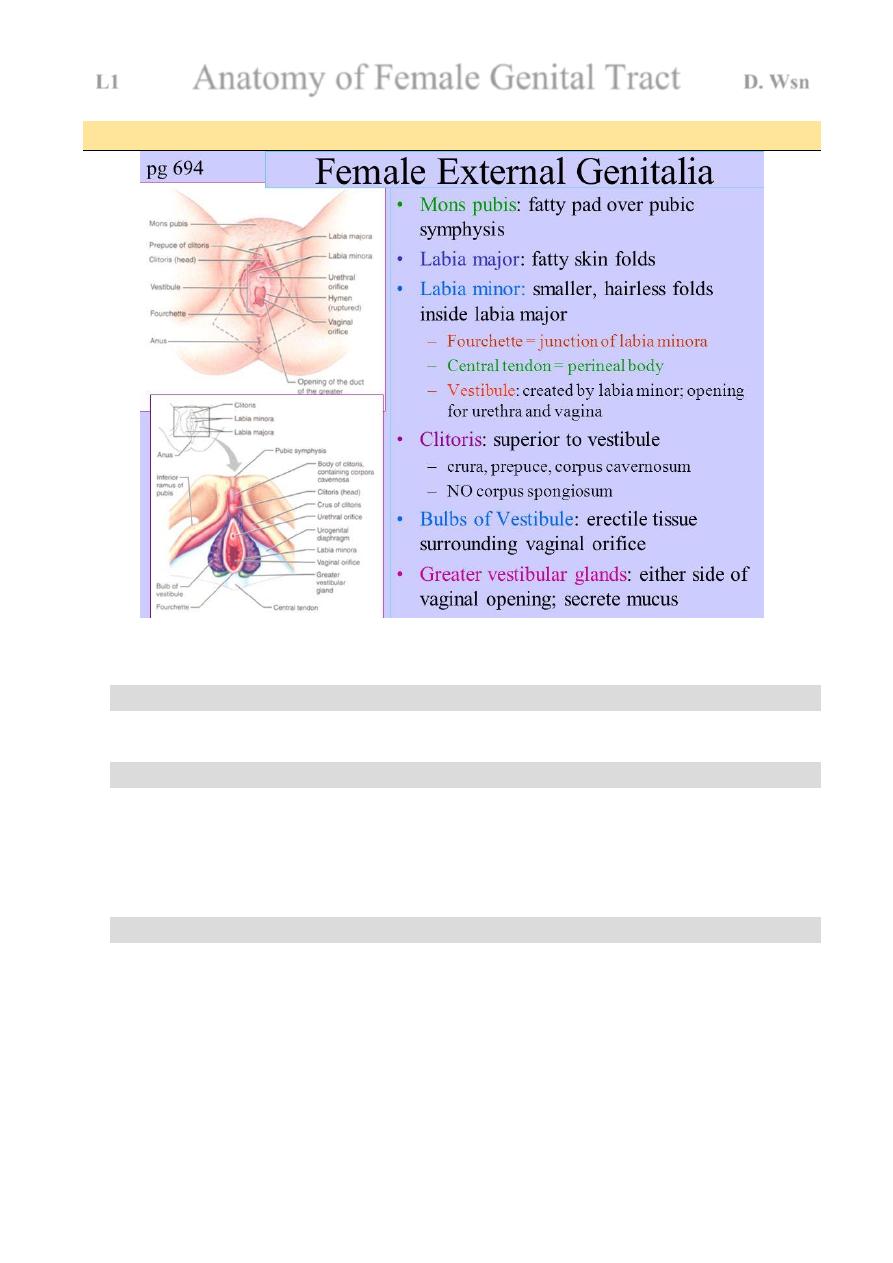
The external genitalia
Is commonly called the vulva
Includes the
1. Mons pubis
Fibro fatty pad covered by hair bearing skin, which covers the body of pubis bone
2. labia majora
Are two folds of skin with underlying adipose tissue either side of the vagina opening.
They contain sebaceous and sweat glands and few specialized apocrine glands
In the deepest part of each labium are the core of fatty tissue continuous with that of
inguinal canal and the round ligament terminate her
3. labia minora
Are two thin folds of skin that lie between the labia majora
These vary in size and may protrude beyond the labia majora where they are visible but
also my concealed by labia majora
Anteriorly the divide into two to form prepuce and frenulum of clitoris (clitoris hood)
Posteriorly they divide to form fold of skin called fourchette
They contain sebaceous glands but have no adipose tissue
They are not well developed before puberty and atrophy after menopause
4. Clitoris
Is an erectile structure measuring approximately 0.3 -3.5 cm in length
Body of clitoris made up of paired of corpora cavernosa (which is columns of erectile
tissue and vascular tissue)
These become crura at the bottom of the clitoris
5. Vestibule
Is the cleft between the two labia minora
It contains opening of the urethra, Bartholin glands and vagina
6. Bartholin glands
Bilateral about the size of pea
They opening via 2 cm duct into the vestibule below hymen
Contribute to lubrication during intercourse
7. Hymen
Is a thin covering of mucus membrane across the entrance of the vagina is usually
perforated which allow menstruation?
Remaining part of the hymen after rupture are called carunculate myrtiforms
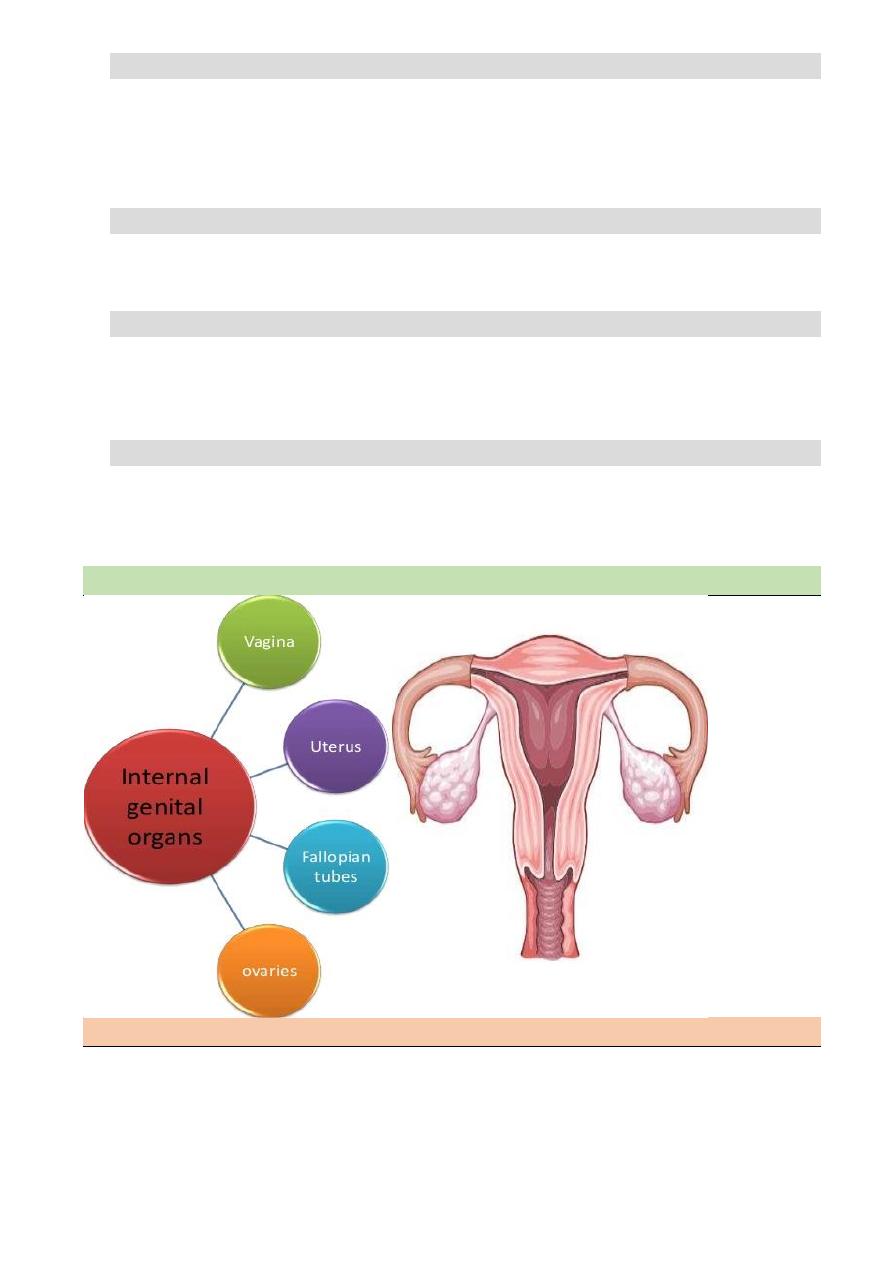
The internal reproductive organs
The vagina
Is fibromuscular canal lined with stratified squamous epithelial that leads from the
uterus to the vulva
Its longer in the posterior wall 9 cm than in the anterior wall 7 cm
The vaginal wall usually in apposition except at the vault where they are separated by
the cervix
The vault of the vagina is divided into four fornices posterior, anterior and two lateral
The vaginal wall lined with transverse folds
Has no gland and is kept moist by the secretions from uterine and cervical gland and
from transudation from its epithelial lining
The epithelium is thick and rich in glycogen but absent before puberty and after
menopause due to lack of estrogen
The upper posterior wall forms the anterior peritoneal reflection of the pouch of Douglas
Middle third separated from rectum by pelvic fascia and the lower third abuts the
perineal body
Anteriorly the vagina is direct contact with bladder base
Laterally the vagina is related to the cardinal ligament
Below levator muscle and ischiorectal fossa
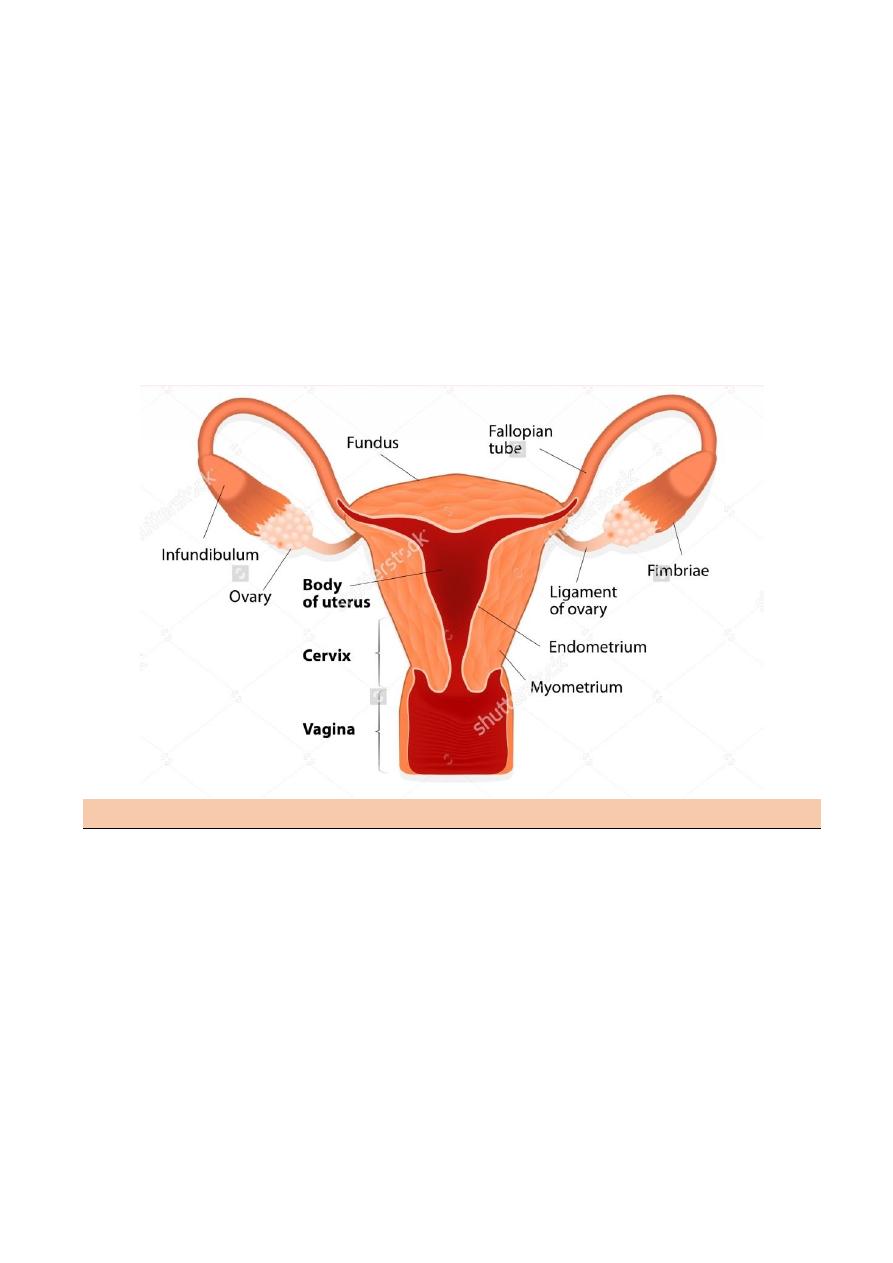
The uterus
Shape like inverted pear tapering inferiorly to the cervix and is situated entirely within
the pelvis
Hallow thick muscular structure
7.5 cm long 5cm wide 3 cm thick 70 gm weight
Upper part called body, the area of insertion of each fallopian tube is called cornu ,
fundus is the part of the body above the cornu , isthmus is small lower constricted area
Direction
o anteversion the longitudinal axis of the uterus at right angle to the vagina
o Ant flexion the uterus flexed foreword on itself at the isthmus
o Retroversion the uterus tilted backward 20 % of female
Three layer outer serous layer (peritoneal) middle muscular layer (myometrium) and the
inner mucous layer (endometrium)
The myometrium forms the bulk and is made of interlacing smooth muscle fibers
intermingling with areolar tissue blood vessel and lymphatics
The endometrium is covered with single ciliated columnar epithelial varies thickness
1-5 according to the cycle
The cervix
2.5 cm length
Lateral to cervix connective tissue called parametrium
Upperpart mostly consist of involuntary muscle whereas lower part is mainly fibrous
connective tissue
The membrane of cervical canal (endocevix) has ant and post columns from which folds
radiate out ,the arbour vitae .it has numerous deep glandular follicle that secrete clear
alkaline mucus the main component of physiological vaginal discharge
Ciliated columnar epithelial in upper 2/3 and change to stratified epithelial around the
region of external os and the junction of these two types of epithelial is called
squamocolumner junction or transformation zone
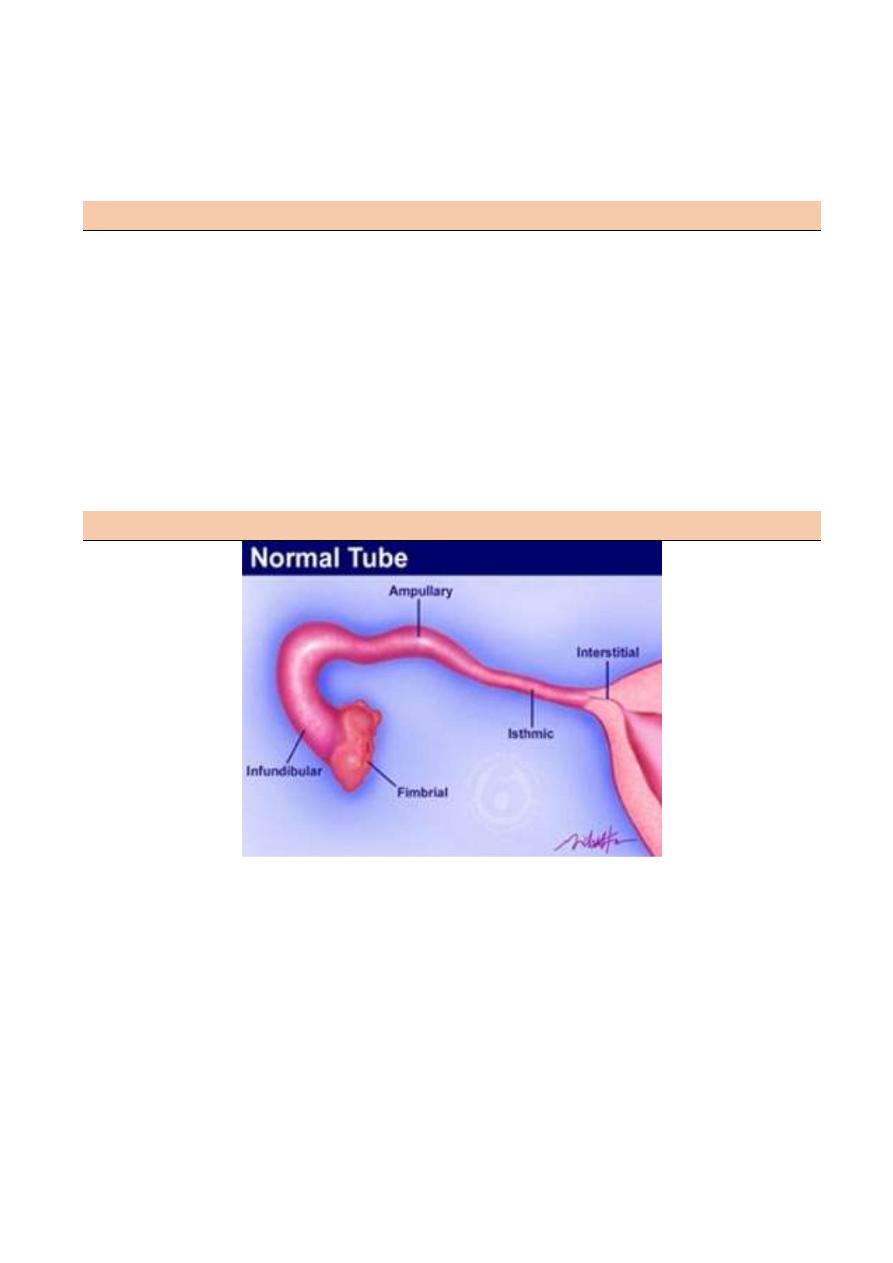
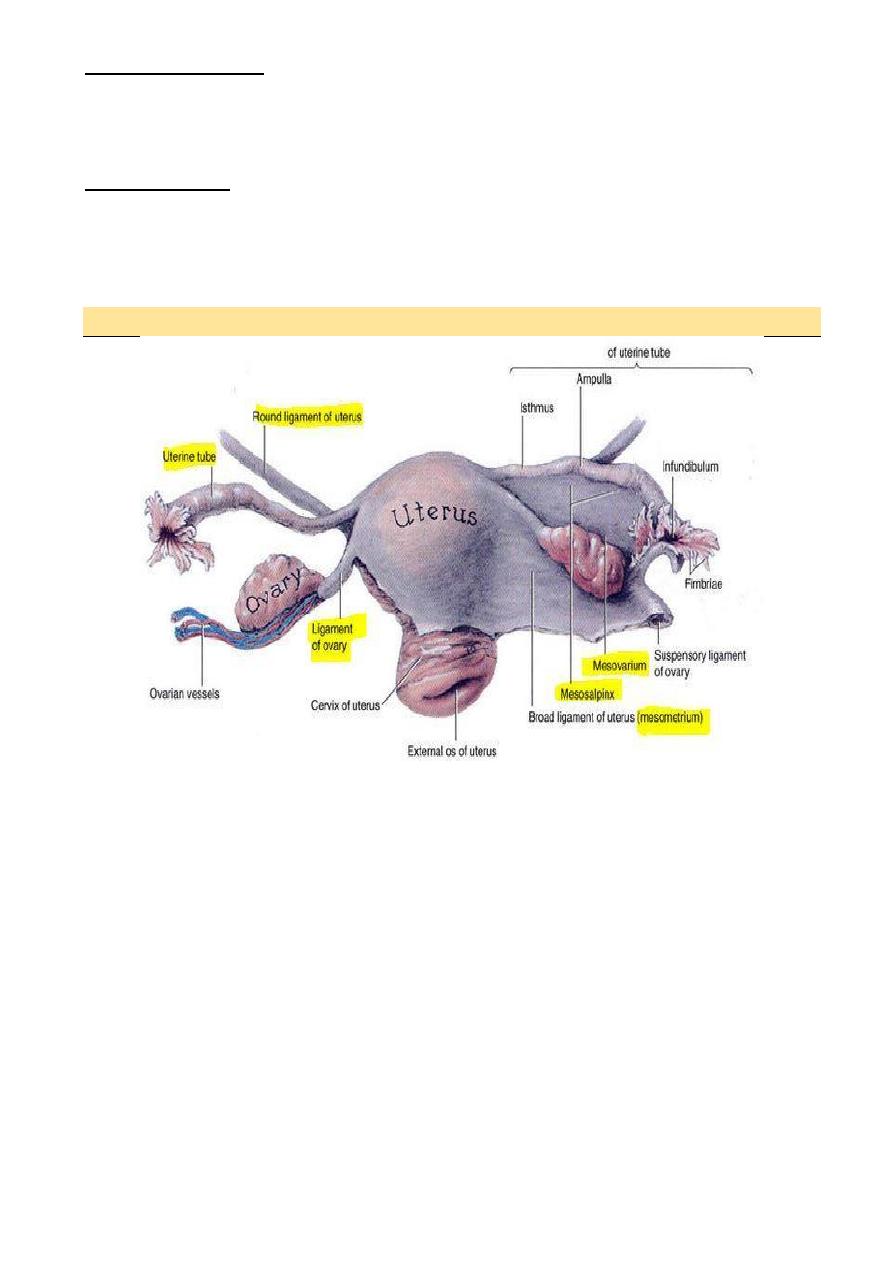
The fallopian tubes
Each tube is about 10 cm long run in upper margin of broad ligaments connect between
the uterus one side and the peritoneal cavity on the other side
Describe in four parts
The interstitial portion
The isthmus
The ampulla
The infundibulum or fimbrial portion
The muscular fibers of the wall of the tube are arranged in the inner circular and an outer
longitudinal layer
There is no submucosa and there are no gland
The epithelial of the tube contain ciliated cell
The ovary
The size and appearance of the ovaries depend on
the the age and the state of the menstrual cycle
Almond shaped and measure approximately 3 cm
long 1.5 cm width and 1 cm thick
Each ovary is attached to the cornua of the uterus
by ovarian ligment and at the hilum to the broad
ligment by mesovarium which contains its supply
of blood vessels and nerves
The ovary is the only intraperitoneal structures not
covered by peritoneum
Has central vascular medulla and outer thicker
cortex
The vestigial structures
Remains of the mesonephric duct and tubules are always present in young children
Variable structures in adult the epoophoron ,paroophoron in the broad ligament
The duct of Gartner is the caudal part of mesonephric duct running alongside the uterus
to internal os
The pelvic muscles ligaments and fascia
The pelvic diaphragm
Is formed by the levetor ani muscles which are broad flat muscles the fiber of which
pass down wards and inwards, one on either side constitute the pelvic diaphragm
The muscle is described in two parts
The pubococcygeus which arises from the pubis bone and the anterior part of the
tendinous arch of pelvic fascia (white line )
The iliococcygeus which arises from the posterior part of the tendinous arch and ischial
spine
Urogenital diaphragm
Is triangular ligament made up of two layers of pelvic fascia which fill the gap between the
descending pubic rami and lies beneath the levator ani muscles. the deep transvers perineal
muscles lie between the two layers and diaphragm is pierced by the urethra and the vagina
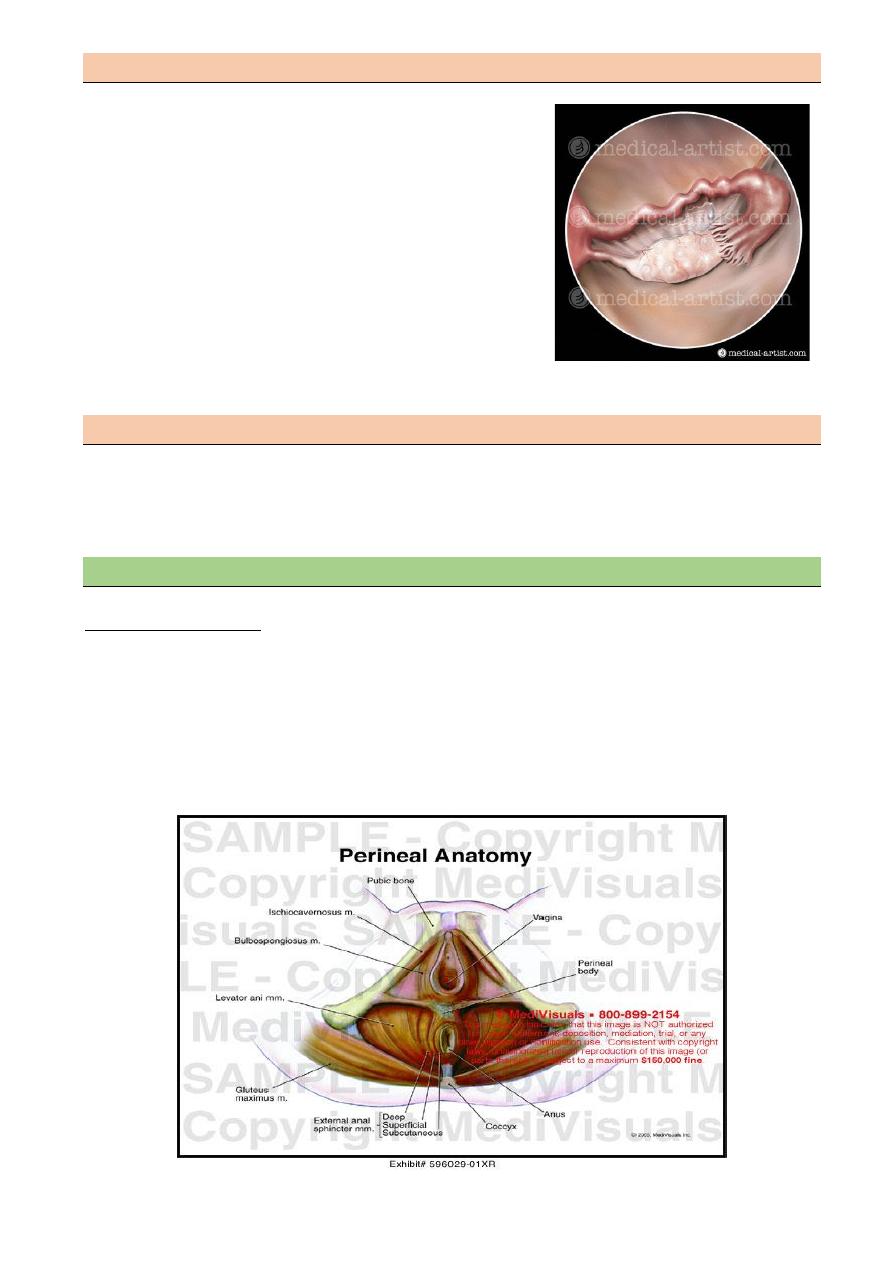
The perineal body
This is mass of muscular tissue that lies between the anal canal and the lower third of the vagina
Its apex is at the lower end of the rectovaginal septum at the point where the rectum and
posterior vagineal walls come into contact. the base is covered with the skin and extend from
the fourchette to the anus
Ligament
Broad ligament its peritoneal reflection from lateral borders of the uterus so despite the
name its not ligament and does not support the uterus
The ovarian ligament from the medial pole of the ovary to the uterus just below the
point of the entry of the fallopian tube
The round ligament is the continuation of the same structure and run forwards under the
anterior leaf of peritoneum to enter the inguinal canal ending in the subcutaneous tissue
of the labium major
The cardinal ligaments (transverse cervical ligaments) provide the essential support of
the uterus and vaginal vault .these are two strong fan shaped fibromuscular bands which
pass from the cervix and vagineal vault to the side wall of the pelvis on either side
The uterosacral ligament run from the cervix and vaginal vault to the sacrum
The bladder is supported laterally by the condensations of the vesical pelvic fascia one
each side and by the sheath of pubocervical fascia which lie beneath it anteriorly
The blood supply
The ovary --- ovarian arteries from abdominal aorta
Right vein to inferior vena cava, left vein to left renal vein
The uterus --- main supply from uterine artery, which is branch of internal iliac artery
Uterine branch of ovarian artery on each side
Other parts of the pelvic organs are supplied by branches of internal iliac artery, which includes
vaginal artery, vesical artery, rectal artery, pudendal artery
Major nerve supply of the pelvis comes from the pudendal nerves, which arise from the second
third and fourth sacral nerves
The embryology
The primitive gonad is formed between 5-7
weeks of gestation ,when undifferentiated germ
cell migrate from the yolk sac to the genital
ridges
In the absence of male determinants, the
primitive gonad becomes an ovary
Granulosa cells derived from the proliferating
coelomic epithelium surround the germ cells
and form primordial follicles
Theca cells develop from the proliferating
coelomic epithelium and are separated from the
granulosa cells by basal lamina
The maximum number of primordial follicles is
reached at 20 weeks gestation when at this time
there are six million primordial follicles present
The number of these reduce by atresia and by
birth one to two million are present .atresia
continues throughout childhood and by
menstruation 300 000 – 400 000 are present
The uterus and vagina
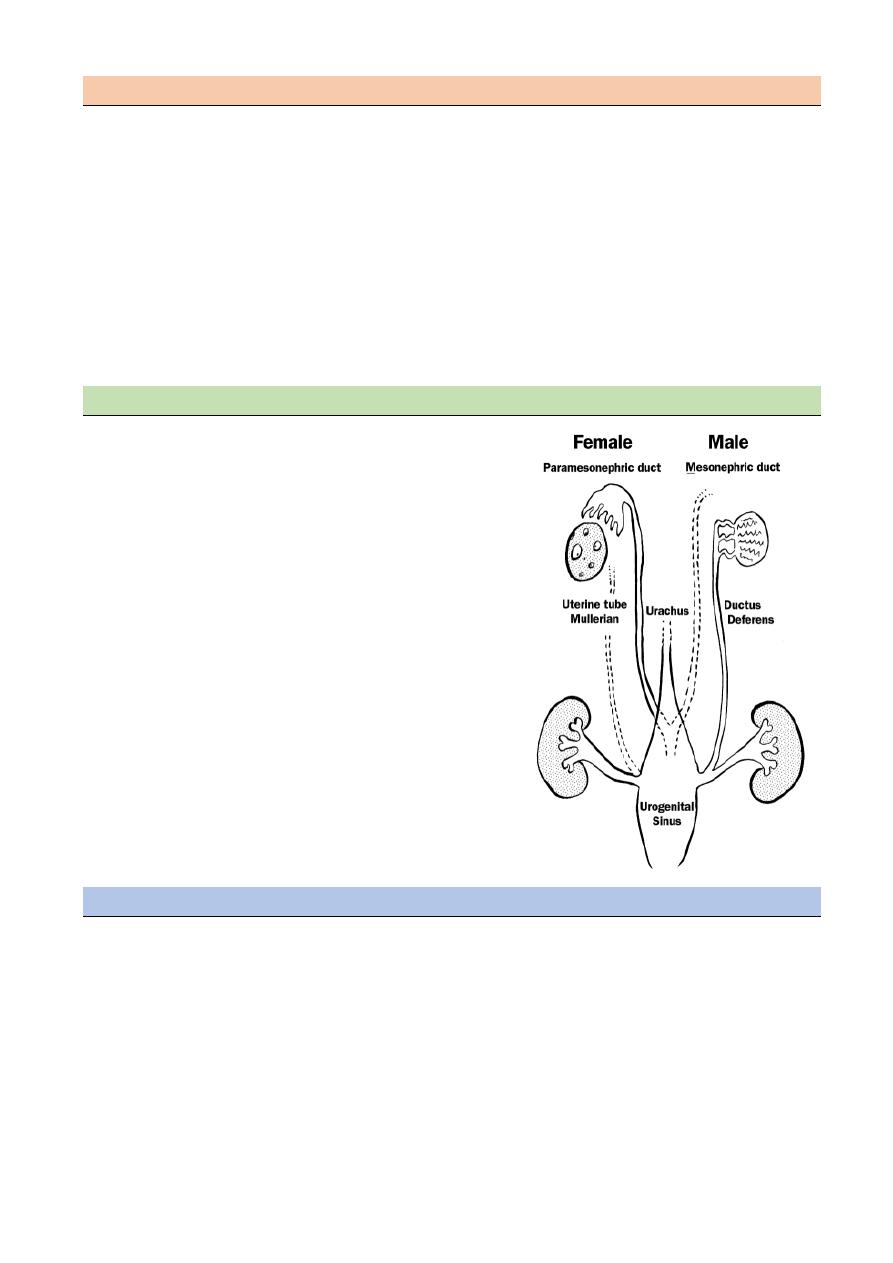
The genital system develops in close association with the urinary system
5th week of embryonic life the nephrogenic duct develops from the mesoderm and forms the
urogenital ridge and mesonephric duct
The mesonephric duct (wolffian duct ) develops under the influence of testosterone into
vas deferens, epididymis and seminal vesicle
The female reproductive tract develop from paired ducts which are adjacent to the
mesonephric duct and so are called the paramesonephric ducts or Mullerian ducts .these
extend caudally to project into posterior wall of the urogenital sinus as the mullerian
tubercle

These fuse in the midline distally to form the uterus ,cervix and proximal two thirds of
the
Vagina
The unfused caudal segments form the fallopian tubes
The distal vagina is form the sinovaginal bulb in the upper portion of urogenital sinus
The external genitalia
5
th
to 7
th
weeks of life the cloacal folds which are a pair of swellings adjacent to the
cloacal membrane fuse anteriorly to become the genital tubercle.this will become the
clitoris
The perineum develops and divides the cloaca membrane into an anterior urogenital
membrane and posterior anal membrane
The cloacal folds anteriorly are called the uretheral folds which form the labia minora
Another pair of folds within the cloacal membrane form the labioscrotal fold which
eventually become the labia majora
The urogenital sinus become the vestibule of the vagina
The external genitalia are recognizable female by the end of 12 weeks gestation
Quiz (True & False)
1. The vagina has two wall anterior and posterior one, which are equal in length
2. The vaginal wall is rich in glandular tissue which responsible on acidity of vaginal discharge
3. The serous layer of the uterus is vary in its thickness according to menstrual cycle
4. The widest part of fallopian tube is isthmus part
5. The ovary has central thick avascular medulla and outer loose cortex
6. The perineal body is a mass of muscular tissue lies between the urethra and lower third of
the vagina
7. The broad ligament is the main support of the uterus
8. The ovarian artery is branch of internal iliac artery
9. The fused mesonephric duct form the future uterus and cervix
10. The external genitalia are recognize as female by the 9 weeks gestation
Mubark A. Wilkins
