Dermatophyte Infection
(Dermatophytoses)By
Dr.Alaa Al-sahlany
Nov. 4, 2018
Introduction
Dermatophytoses are fungal infections caused by three genera of fungi that have the ability to invade and multiply within keratinized tissue (hair, skin and nails):include(1) Trichophyton
(2) Epidermophyton
(3) Microsporum
Epidemiology
Trichophyton rubrum is the most common dermatophyte worldwideOccur most frequently in postpubertal hosts except tinea capitis which occurs mainly in prepubertal children
Men tend to more frequently have tinea cruris and tinea pedis than women
Pathogenesis
First stepClinical features
Mode of transmission
Type
Non-inflammatory to mild inflammation, chronic
Human to human
Anthropophilic
i.e. T. rubrum
Moderate inflammation
Soil to human or soil to animal
Geophilic
i.e. M. gypseum
Severe inflammation, acute
Animal to human
Zoophilic
i.e. M. canis, T.verrucosum
Host factors
Dermatophyte factors
Protease inhibitor: limit the extent of invasion by inhibiting keratinase
Keratinase : break down keratin and help the fungi invade skin
Sebum has an inhibitory effect on dermatophyte
Mannans in cell wall: has immuno-suppressive effect and inhibit the epidermal proliferation that prevent sloughing off of fungi
Diseases that affect barrier function i.e. icthyosis , Hailey-Hailey disease and Darier disease predispose the skin to infection
Second step
Third stepOnce dermatophytes have invaded the skin with help of dermatophyte factors mentioned in the box, three factors limit the infection to stratum corneum:
(1)Preference of dermatophyte for Cooler temperature at skin surface,(2) serum factors such as ferritin and β-globulin that inhibit dermatophyte growth and(3) immune system
Causative pathogen
Type of dermatophyte infection• Any dermatophyte but T.rubrum is the most common
Tinea corporis, tinea pedis, tinea cruris, tinea manuum, tinea faciei and tinea unguium
T.Tonsurans is the most common in USAT.Verrucosum is the most comon in Iraq
Note: favus is caused by T. schoenleinii.
Tinea capitis
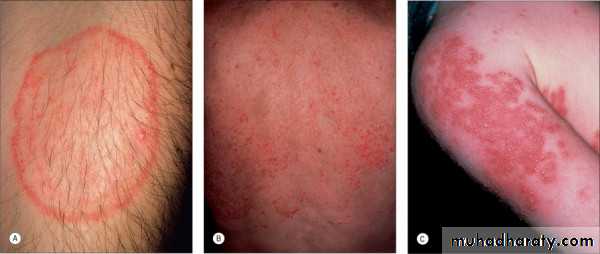
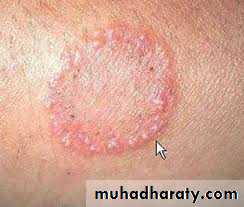
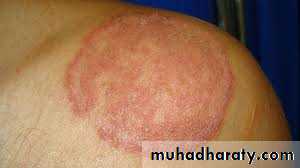
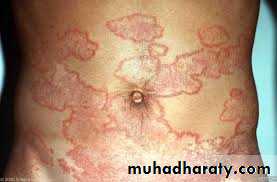
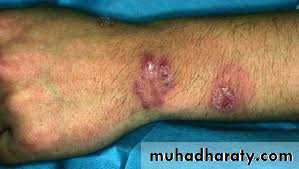
Tinea corporis
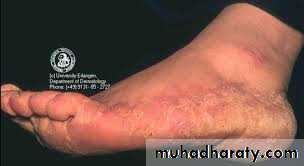
Infection of the skin of the trunk and extremities, excluding the hair, nails, palms, soles and groinAny dermatophyte can cause it BUT T. rubrum is the most common pathogen
Infection spreads centrifugally from the point of skin invasion, with central clearing of the fungus , typically resulting in annular lesionsVariants:
Tinea incognito: tinea lesion modified by topical steroids, may lack a raised scaly border and clear center.Majocchi’s granuloma: is characterized by follicular papulopustules or nodules, commonly seen in women who have tinea pedis or onychomycosis and shave their legs. Topical steroids and immunosuppression are predisposing factors.
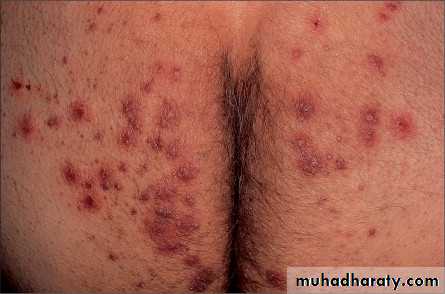
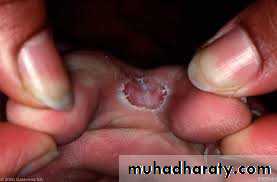
Tinea cruris(Jock itch)
Infection of the inguinal regionAny dermatophyte can cause it BUT T. rubrum is the most common pathogen
This disease is more often seen in men than in women, since the scrotum provides a warm and moist environment that encourages fungal growth
The inflicted are more likely to have tinea pedis and onychomycosis as a source of dermatophytes
Other predisposing factors include obesity and hyperhidrosis
Presented as a sharply demarcated with a raised, erythematous, scaly active border that may contain pustules or vesicles and a central clearanceThe scrotum itself is generally spared, unlike candidiasis of groin
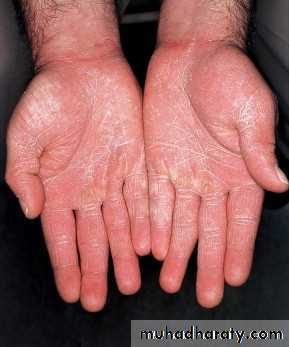
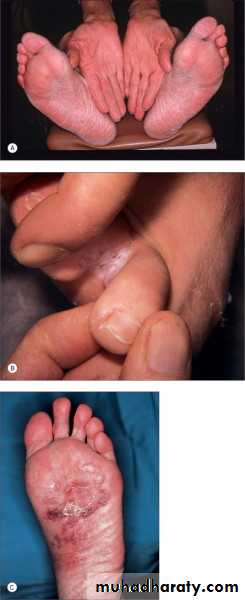
Tinea manuumInfection of the palm and interdigital spaces
It is different from that of back of hands due to lack of sebaceous glands on the palms
.Usually non-inflammatory and often unilateral there is diffuse hyperkeratosis of the palms and digits with accentuation of scales on creases that fails to respond to emollients
An important clinical clue is tinea unguium
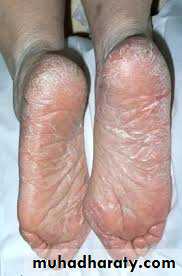
Is often present in patients with tinea pedis(two feet and one hand syndrome)Tinea pedis(Athlete’s foot)
Infection of the soles and interdigital web spaces of the feetMore common in adults
Lack of sebaceous glands and moist environmentdue to occlusive shoes are predisposing factors
Tinea pedis is uncommon in populations that do not wear shoes although the barefoot people can acquire the fungus in public facilities i.e. gym
The feet are the most common location for dermatophyte infections
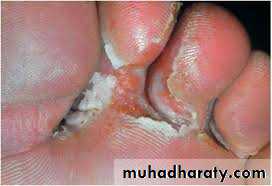
Types:(1)Moccasin: diffuse hyperkeratosis, scaling and erythema
(2)Interdigital :Most common type; erythema, maceration, fissures and ,ulceration between toesMoccasin
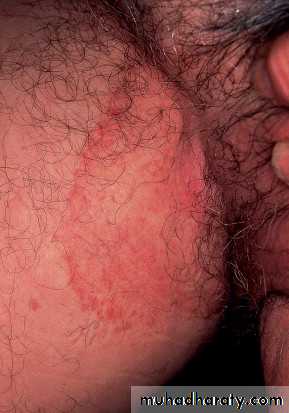
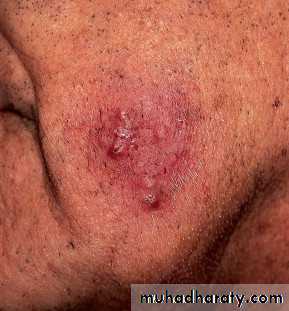
Tinea barbae
Involves the bearded areas of the face and neck in men
Two types:
(1) The inflammatory type: develops slowly and produces nodules and kerion-like swellings: acquired from animal, caused by T. verrucosum.(2)Non-inflammtory type: less inflammatory, characterized by pustular folliculitis , caused by T. rubrum. Aquired from contaminated razors in barber- shops. Now less common owing to use of disposable instruments and disinfectant
In both types: the hairs are either easily plucked or lost.
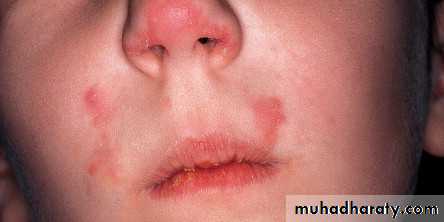
Tinea facieiInfection of face
The same as tinea corporis
Typical annular rings are usually lacking and the lesions are exquisitely photosensitive. Therefore, misdiagnosedTinea capitis
A common dermatophyte infection of the scalp in children, whereas adult infection occurs infrequentlyT. tonsurans is currently the most common cause of tinea capitis in the US while T.verrucosum in Iraq
The “carrier state” of tinea capitis is contagious through contaminated brush, hat, towel and barber tools
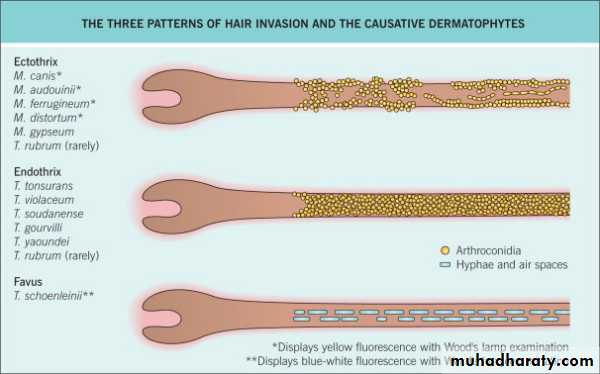
Types of dermatophytes that invade hair:
(1)Endothrix: exist inside the hair shaft, caused by Trichophyton, non- fluorescent. Exception is T. schoenleinii (fluorescent)(2)Ectothrix: exist outside the hair shaft, caused by Microsporum(fluorescent) or Trichophyton (non-fluorescent)
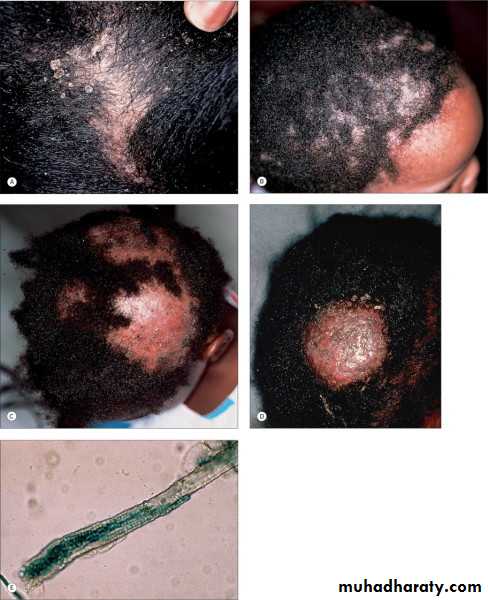
Clinical types:
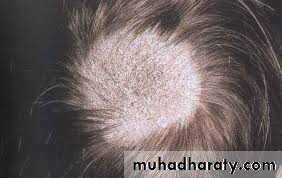
Non-inflammatory:Gray patch:M. auduinii, present as a dry scaly patch of alopecia
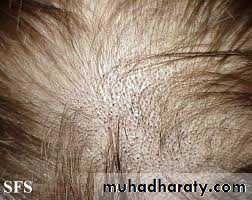
Black dots:T. tonsurans, caused by hair breakage near the surface
Inflammatory:
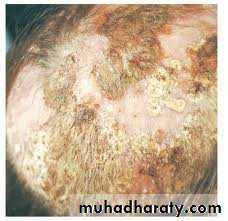
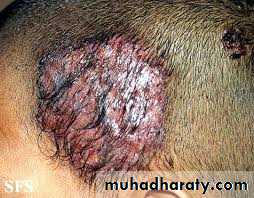
Kerion: M.canis, present as a boggy, purulent plaques with abscess formation and associated alopecia, patient may become systemically ill with extensive lymphadenopathyFavus: T. schoenleinii, the most severe type of dermatophyte hair infection, present as a concave, sulfur-yellow crusts pierced by hairs (“scutula”)
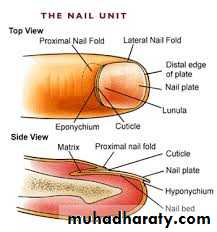
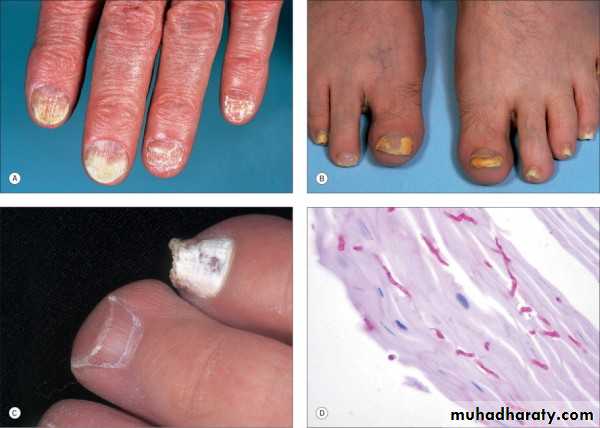
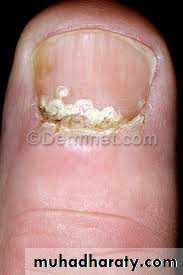
Tinea unguium (onychomycosis)
Infection of the nail unitThree types : based upon the point of fungal entry into the nail unit
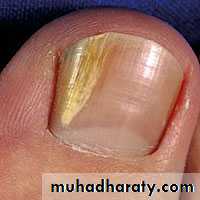
Distal/lateral subungual: (most common)
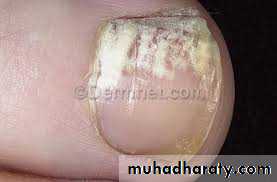
Superficial white:Proximal subungual: ( seen frequently in immunocompromised hosts).
Multiple nails on one or both hands or feet are usually affectedAffects men more often than women?
Frequently associated with chronic tinea pedis
Toenail infections are considerably more common than fingernail?
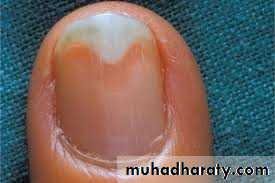
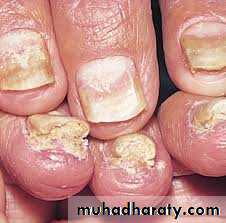
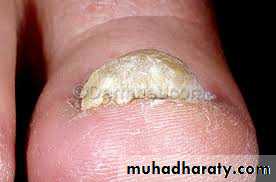
Clinical features:Hyperkeratosis of nail bed
Thickenening and yellowish discoloration of nail plate
Onychlysis (seperation of nail plate from nail bed)Nail dystrophy when the entire nail plate and bed are involved
Diagnosis
Clinical examination(most important)KOH examination of skin scraping(by blade), nail clipping (by nail clipper) or hair plucking(by tweezer)
Wood’s lamp(ultraviolet light of 365 nm wavelength): Infected hairs show bright green or yellow- green fluorescence
Culture:2-4 weeks
Biopsy: we see hyphae in stratum corneumTreatment
Topical antifungals e.g. ketoconazole, clotrimazole are the first line treatmentSystemic antifungal: indications
(A)tinea manuum, (B)mocassin type of tinea pedis, (C)tinea capitis, (D) tinea barbae, (E) tinea unguium, (F) when extensive area is involvedAntifungals
Comment
Spectrum of actionAntifungal agent
In general, the longest course of treatment is for tinea unguium followed by tinea capitis followed by other types of dermatophytosis
Griseofulvin is the first choice for treatment of tinea capitis (4-12 weeks course)
Imidazoles and allylamines are the first choice for treatment of tinea unguium
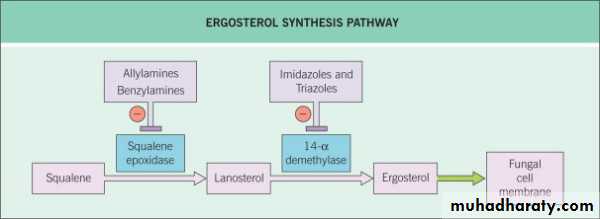
Dermatophytes, Candida and Pityrosporum• Imidazoles e.g. ketoconazole, itraconazole, fluconazole, clotrimazole:
Dermatophytes
• Allylamines e.g. terbinafinCandida only
• Polyenes e.g. amphotericin B and nystatinDermatophytes only
GriseofulvinDermatophytid(id reaction)
Associated with inflammatory tinea capitis and acute tinea pedisRepresent a systemic reaction to fungal antigens
Diagnosis requires:(1) finding of fungus at site remote from the lesions of the dermatophytid, (2)the absence of fungus in the id lesion, and(3) involution of the lesion as the fungal infection is treatedDefinitions
Gyrate:revolves or spin around a fixed point or axisPolycyclic:having two or more rings fused together
Serpiginious: having a wave border (snake-like)
Circinate:circular or round
Annular: ring-like