INTRODUCTION
• Burning Mouth Syndrome (BMS), or idiopathic stomatodynia, is a chronic debilitating oral condition characterized by a burning sensation of the oral mucosa in an apparently normal person. Its etiology and pathogenesis remain unclear. However, psychophysi-cal and neurophysiological studies highlight peripheral and central neuropathic sensory alterations rather than psychogenic factors.• 1
• طب فم نظري / خامس اسنان كركوك
• د.لانا
• 15/1/2019
• 281
DEFINITION
spontaneous pain and burning sensation in an intact oral mucosa with no objective clinical sign and no identifiable dental or medical cause.The pathology has been evolving for at least 4 to 6 months
• 2
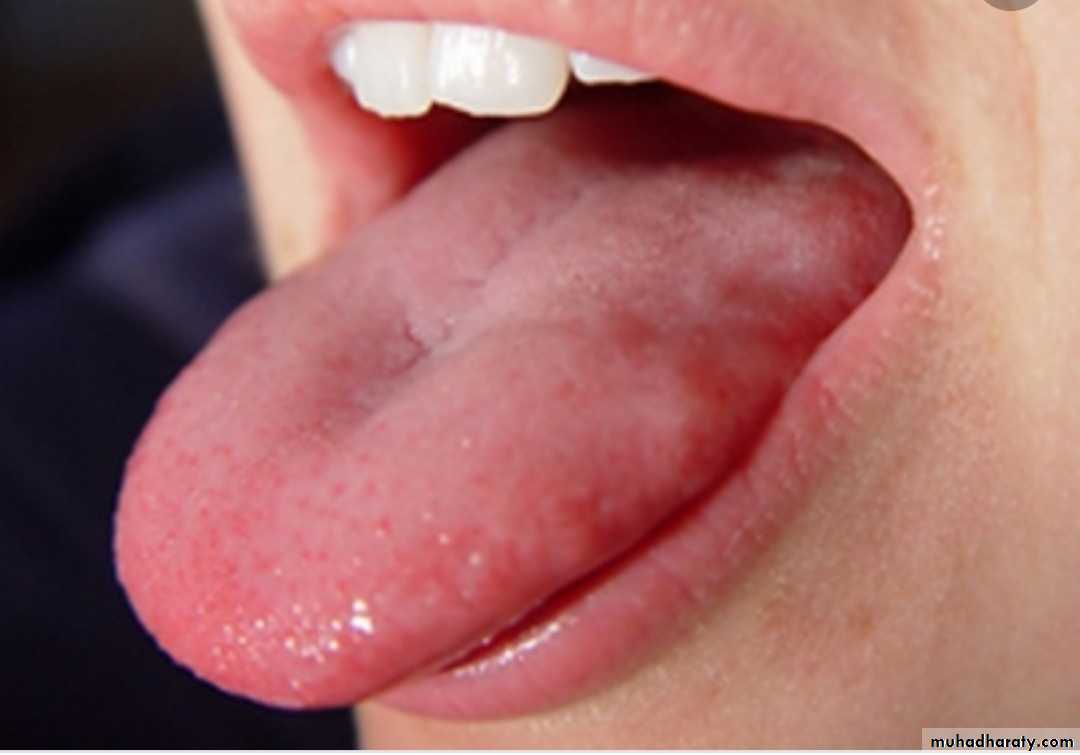
Symptoms/clinical feasure• Pain Mostly occur at anterior part of tongue followed by labial mucosa
• And occasianally palate.
• The burning pain is often accompained witg tingling or numbness and sensation of dryness of mouth , reduced taste intensity and bitter and metallic taste.
• Moderate to severe intensity is usually bilateral symmetrical and is present every day for most of the day.
• 3
CLASSIFICATION
Based on etiology as:
Primary, where etiology is unknown
Secondary, where the etiology is known
• 4
Based on symptoms as• Type 1 BMS: Patients have no symptoms upon waking but symptoms progress throughout the day reaching its peak intensity by evening. Night-time symptoms are variable. It is linked to systemic disorders like nutritional deficiency and diabete.
• Type 2 BMS: Patients have continuous symptoms through-out the day and are symptomatic at night resulting in sleep less nights.This type is associated with chronic anxiety due to altered sleep pattern and is related to use of antidepressant drugs which cause xerostomia.
Type 3 BMS: Patients have intermittent symptoms through out the day with symptom free periods. Usually seen due to anxiety or allergic reactions especially to food allergens.
• 5
local factors
…-• 1-xerostomia ( low salivary flow)
• 2-candidal infection
• 3-Stomatitis under prosthesis
• 4-Chronic trauma
• 5-Oral mucosal conditions (erythema/erosion of whatever cause, atrophic tongue, geographic tongue, lichen planus, pemphigoid, pemphigus)
• 6-Gastritits, Gastroesopha-geal reflux diseases.
• 7-Allergic stomatitis (al-lergic or immunological factors)
• 8-Parafunctional habits (cheek sucking, tongue thrusting, bruxism, suction
• 6
Systemic factors
• 1-Decreased levels of vitamins B1, B2, B12, folate, iron, zinc
• 2-Diabetic patient.
• 3-Thyroid hypofunction.
• 4-Menopause.
• 5-Sjogren’s syndrome.
• 6-Systemic lupus erythematosus.
• 7-Various peripheral or central neuropathies such as parkinson’s disease.
• 8-Drugs therapies :ACE Inhibitors , Angiotensin receptor blockers ,Antidepressant and hypoglycemic drug.
• 7
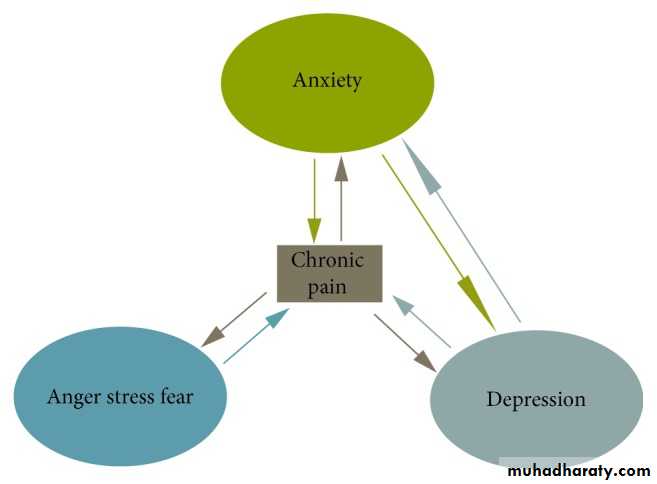
SYCHOLOGICAL FACTORS
1-Anxiety.2-Depression.
3-Stress psychological post traumatic.
• 8
• 9
Local examination
• 1-Measurement of salivary flow rate.• 2-Oral cultures: For bacterial, viral and fungal infections.
• 3-Inspection of mucous: erythema, erosion, ul-cerations, trauma, contact reactions with removable prostheses.
• 4-Biopsy of tongue or oral mucosa.
• 5-Search for parafunctional habits.
• 10
General examination
Blood tests:Complete blood cell count
• Glucose level, glycosylated hemoglobin (A1C)
• Nutritional factors (dosage vitamins B, zinc and folate)
• Thyroid function
• Immune function
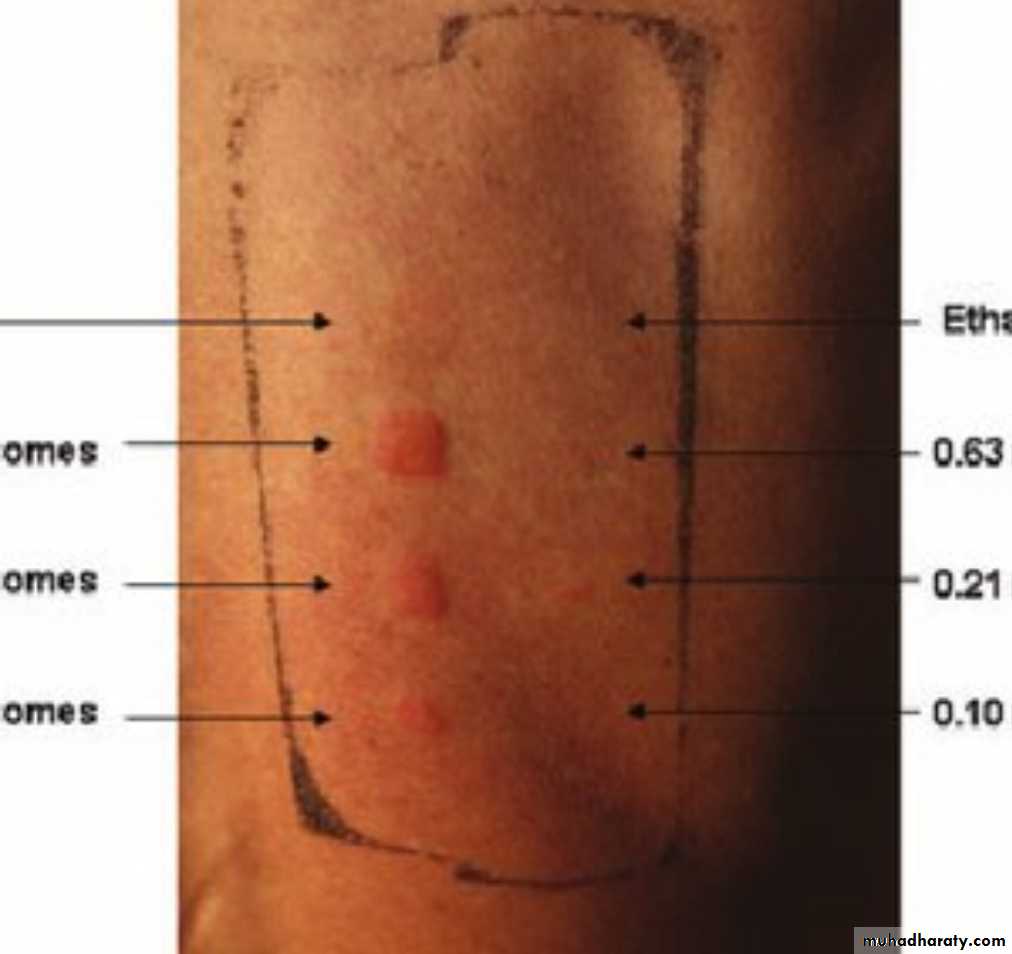
• Patch tests: To check allergy to certain foods
• 11
Treatment and managment
Topical (local) and systemic therapies1-Capsaicin is an alkaloid responsible for the burning sensation produced by chilli peppers. It is capable of desensitizing TRPV1 calcium channel nociceptors and c-fibers.
• 2-Oral lidocaine has also been used topically to relieve the burning sensation.
• 3-Clonazepam takes low doses
• 4-female hormone replacement
• 5-mouth rinses
• 6-Medicines that help with nerve-related pain such as amitriptyline (Elavil) nortriptyline (Aventyl, Pamelor)
• 7-Vitamin supplement
• 13
You can do a few things that may help your symptoms as well
Avoid acidic foods like tomatoes and orangeAviod spicy food
Aviod mouthwashed with alcohol
Aviod tobacco
Drink a lot of water
Chew sugerless gum (You will make more saliva)
Reduce stress by exercises
• 14