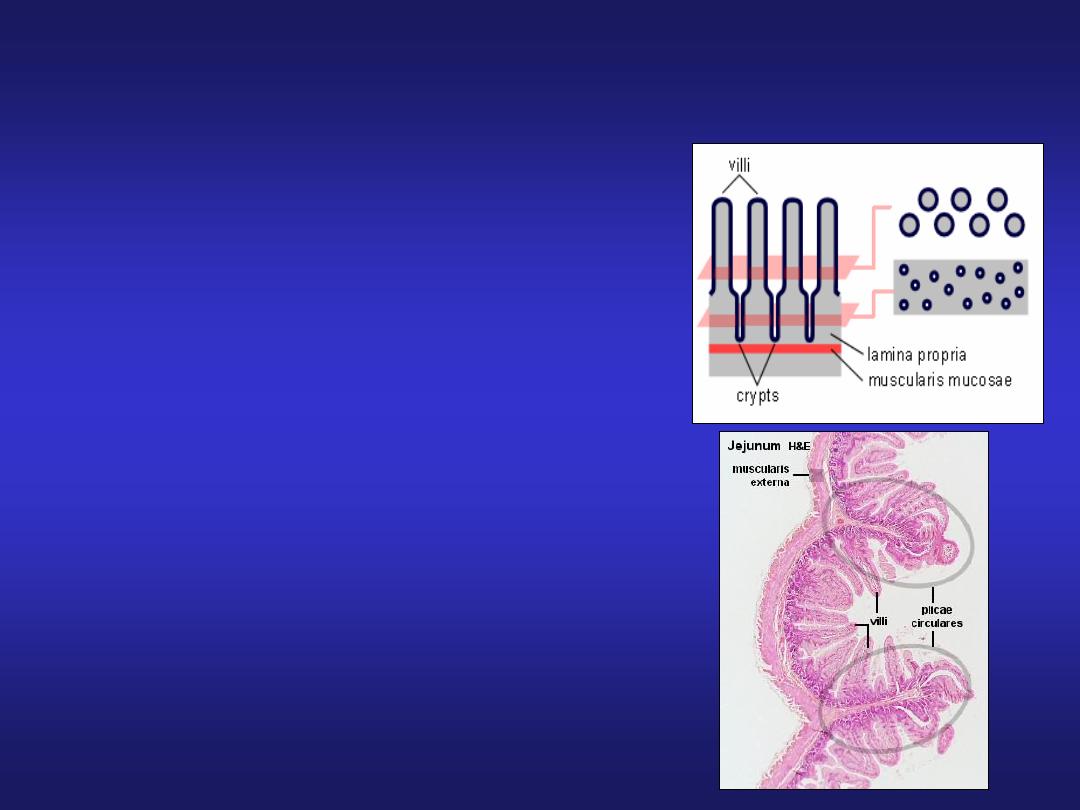
Small Intestine
It is divided into duodenum, jejunum
and ileum.
• Mucosa: characteristic features-
Plicae circularis (valves of Kerkring)
Villi & Microvilli
Goblet cells (few)
Crypts of Lieberkuhn (intestinal glands)
Glands are lined by columnar cells,
goblet cells, Paneth cells &
enteroendocrine cells

The Small Intestine
• Plays key role in digestion and absorption
of nutrients
• 90% of nutrient absorption occurs in the
small intestine
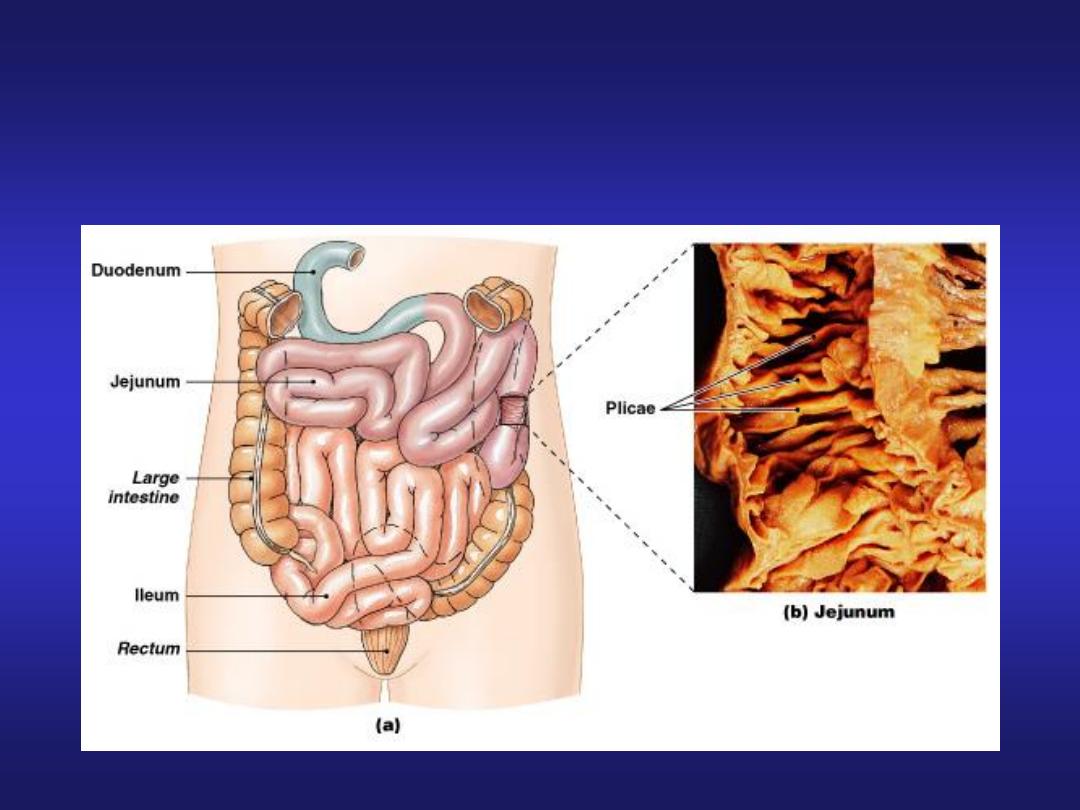
Segments of the Intestine
Figure 24–16

Segments of the S.I.
• S.I. Runs from pyloric sphincter to the ileocecal
valve; 3 segments:
• The Duodenum is the 25 cm (10 in.) long segment of
small intestine closest to stomach
– “Mixing bowl” that receives chyme from stomach,
digestive secretions from pancreas and liver
• The Jejunum is the 2.5 meter (8.2 ft) long middle
segment and is the location of most chemical
digestion and nutrient absorption
• The Ileum is he final 3.5 meter (11.48 ft) long
segment, joins large intestine at ileocecal valve

Intestinal Folds and Projections
• Structural modifications of the small intestine wall
increase surface area
• Plicae = Largest; deep transverse (circular) folds in
intestinal lining; permanent features (they do not
disappear when small intestine fills)
• Intestinal Villi: a series of fingerlike projections of
mucosa
• Villi are covered with simple columnar epithelium
which themselves are have many plasma membrane
projections called microvilli
• All serve to increase surface area for absorption
(altogether by 600x)

Intestinal Histology
• Absorptive columnar cells
• Goblet cells between columnar epithelial cells
eject mucins onto intestinal surfaces
• Enteroendocrine cells in intestinal glands produce
intestinal hormones:
– gastrin
– cholecystokinin
– Secretin
• Peyer’s patches are found in the submucosa

Lacteals
• Each villus lamina propria has ample capillary
supply (to absorb nutrients) and nerves
• In addition, each villus has a central lymph
capillary called a lacteal. These are larger than the
blood capillaries and thus can absorb larger
particles into the body, such as lipid droplets.
• Muscle contractions move villi back and forth to
facilitate absorption and to squeeze the lacteals to
assist lymph movement
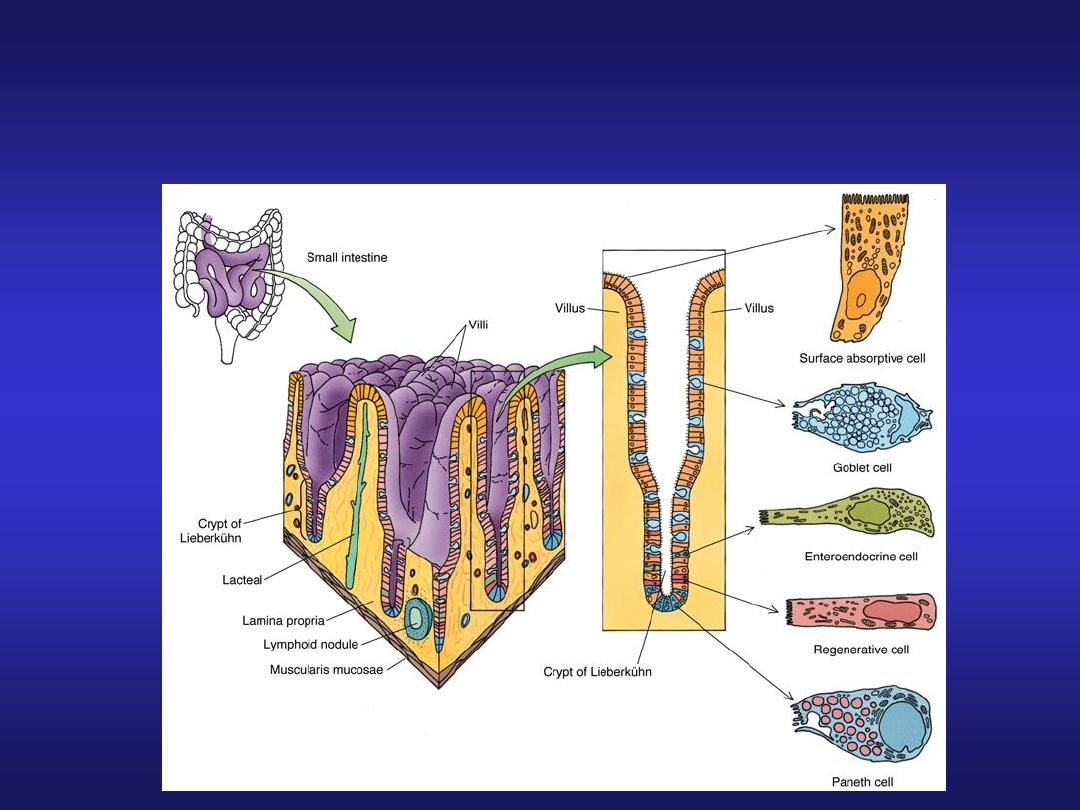
Small Intestine
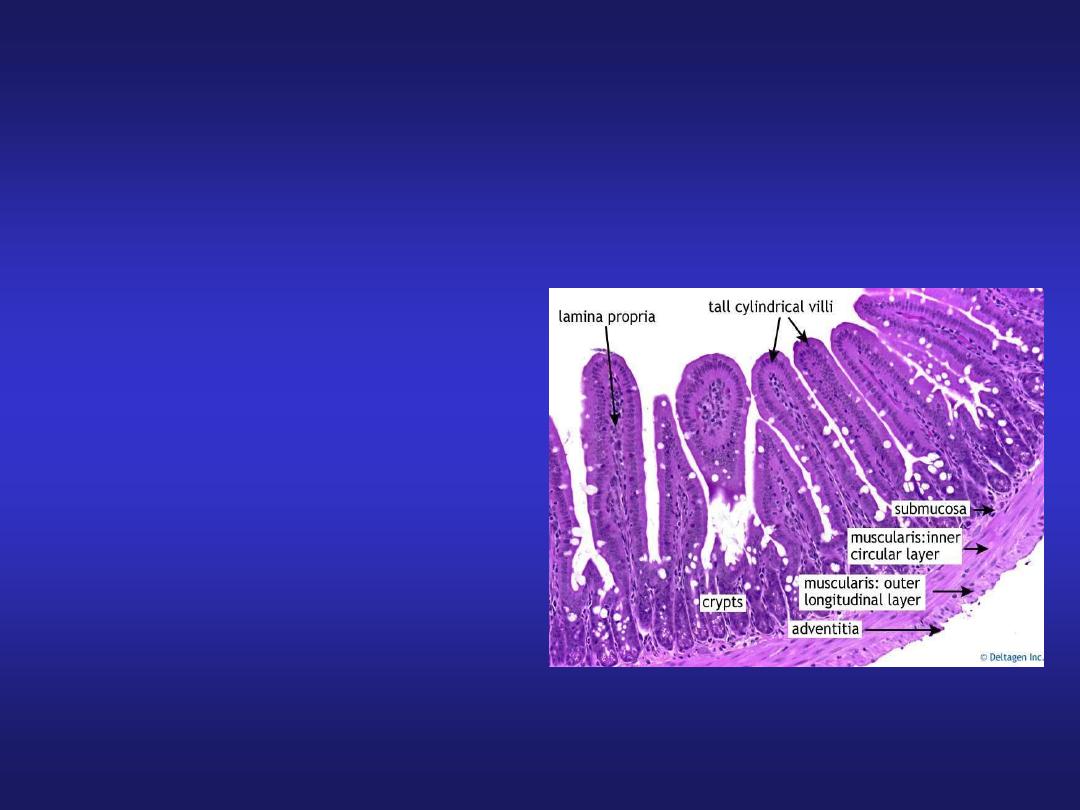
Small Intestine
• Submucosa: contains
blood vessels, lymphatics
and Meissner’s plexus.
• Muscularis externa:
Outer longitudinal and
inner circular layers of
smooth muscle.
• Serosa/Adventitia
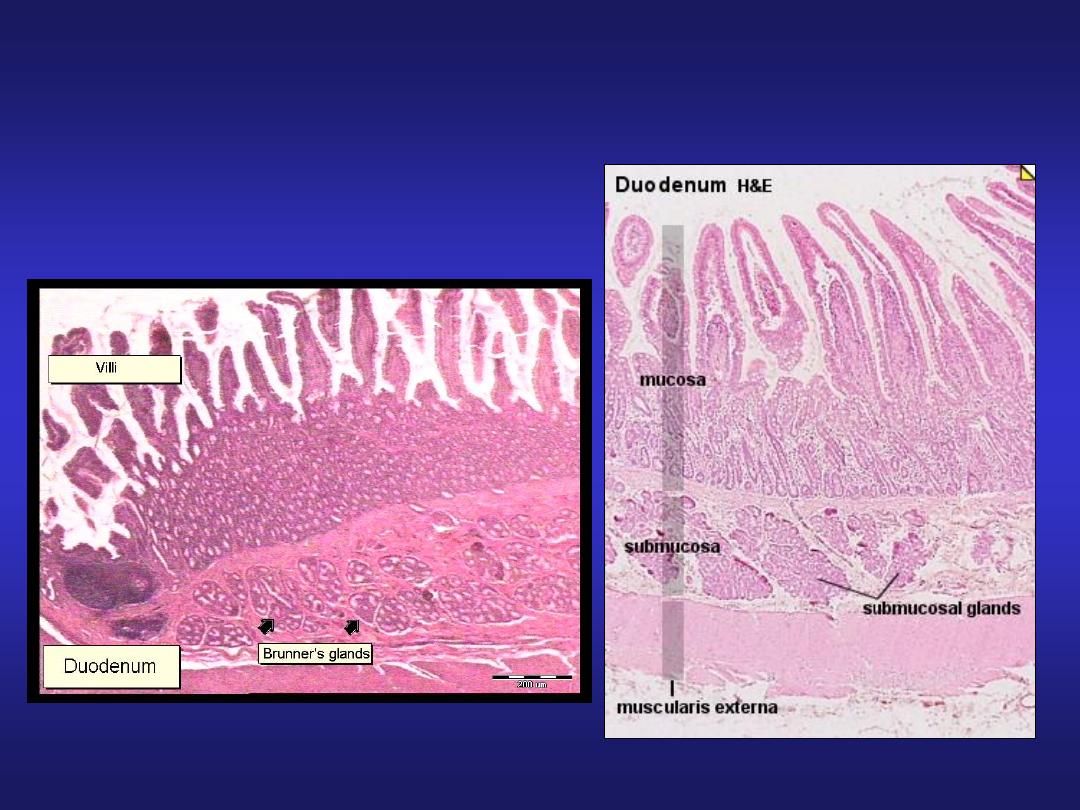
Duodenum
Presence of Brunner’s glands
in submucosa
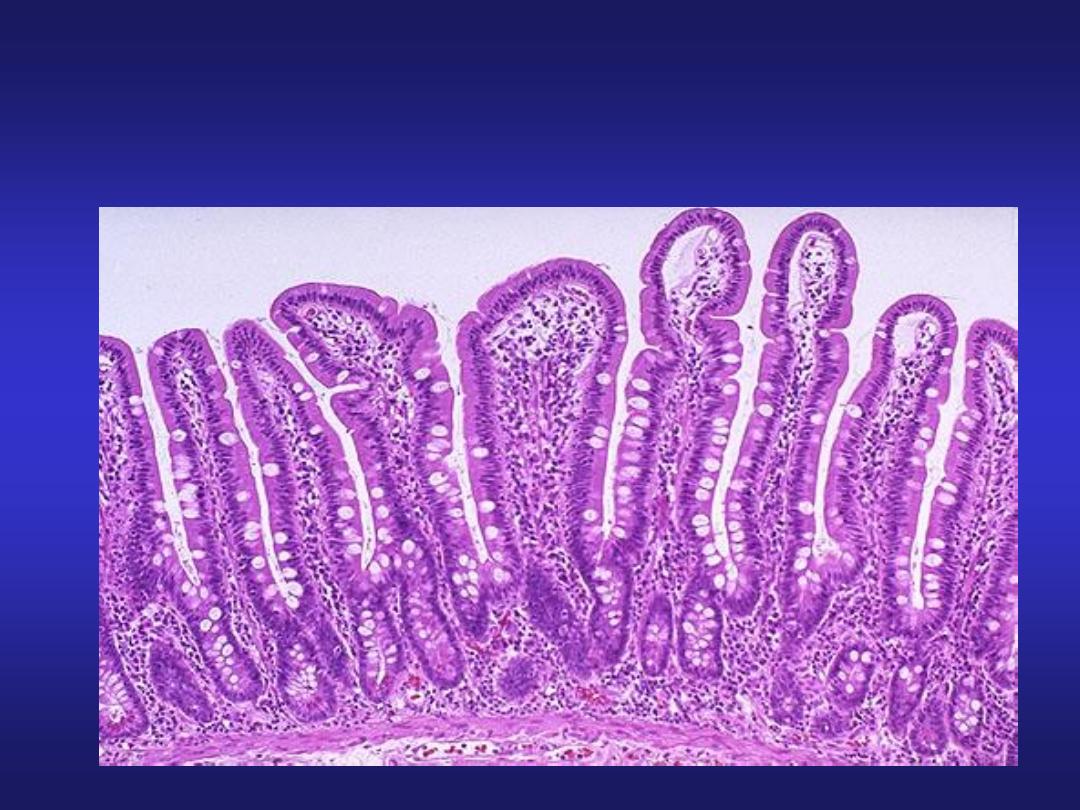
High power view of
the Duodenal Mucosa
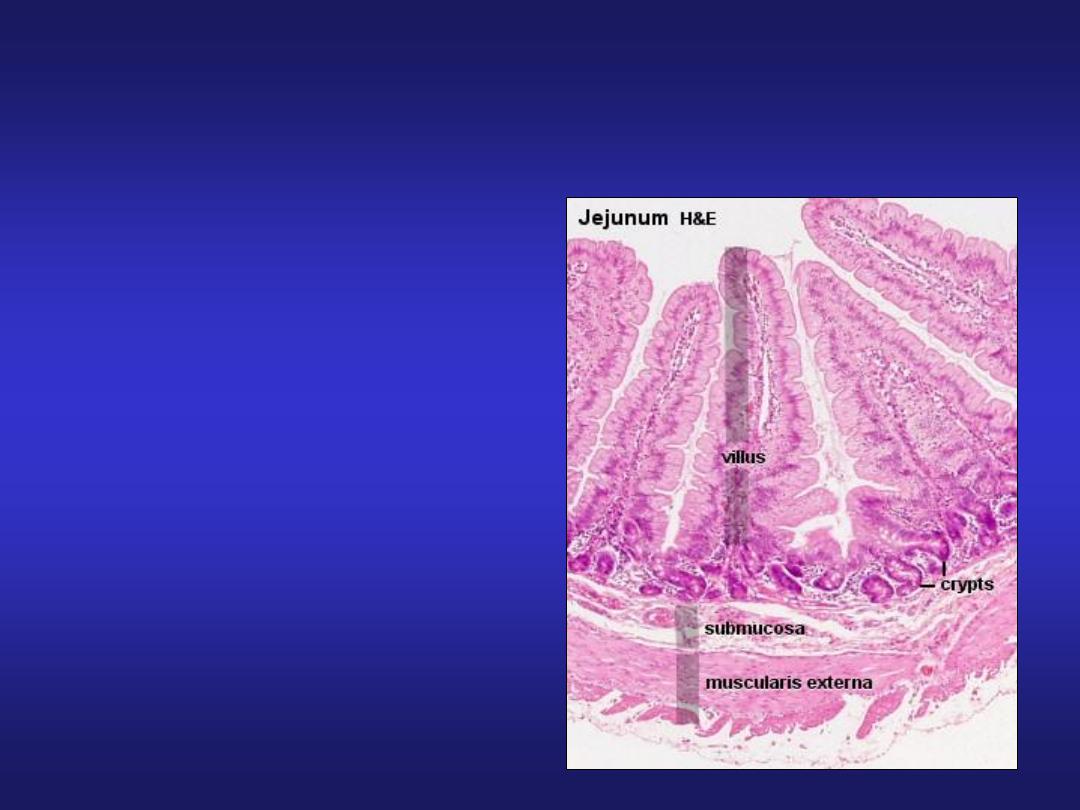
Jejunum
• Villi are tongue shaped.
• Absence of Brunner’s
glands.
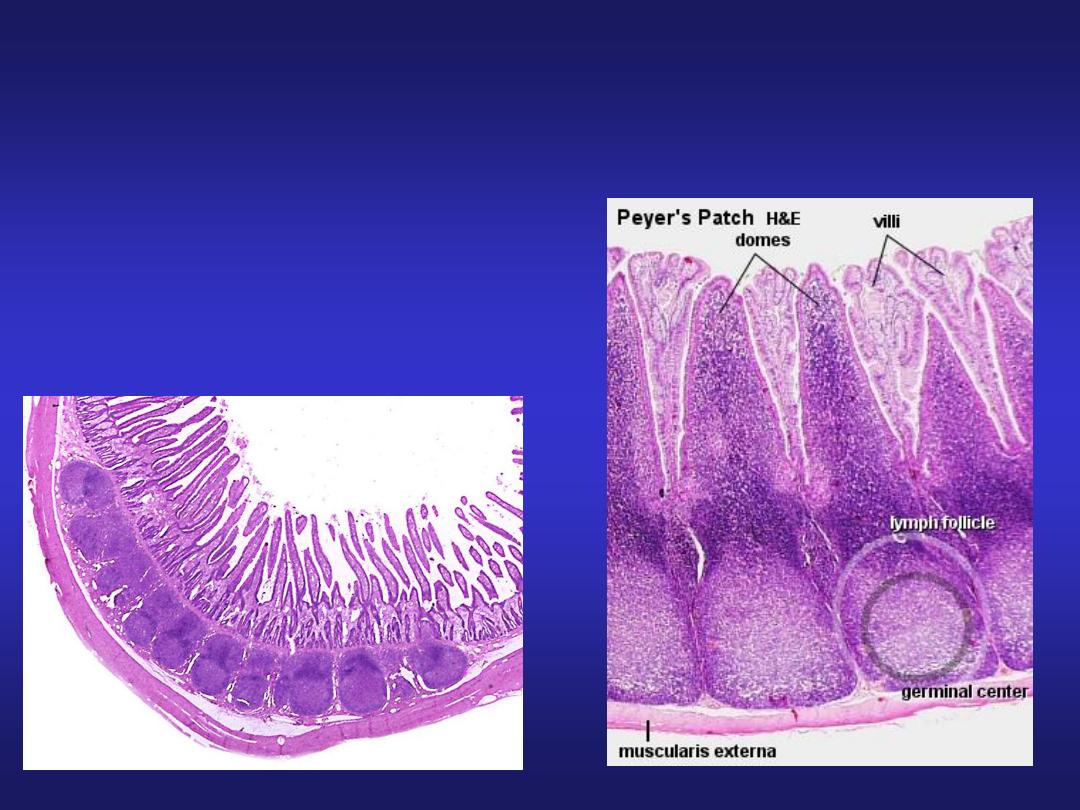
Ileum
• Presence of lymphoid
aggregations in lamina propria
known as Peyer’s patches.
• Villi are short & finger like.

The Large Intestine
• Also called large bowel
• Horseshoe-shaped, about 1.5 meters long and 7.5 cm
wide
• Extends from end of ileum to anus
• Lies inferior to stomach and liver
• Frames the small intestine
• Functions
– Reabsorption of water [the last 15-20%]
– Compaction of intestinal contents into feces
– Absorption of important vitamins produced by bacteria
– Storage of fecal material prior to defecation

Parts of the Large Intestine
• Cecum:
– the pouchlike first portion
– Has wormlike appendix projecting from it
• Colon:
– the largest portion
• Rectum:
– the last 15 cm of digestive tract
• Anal canal

The Colon
• Has a larger diameter (this is why it is
called large) and thinner wall than small
intestine
• The wall of the colon forms a series of
pocketlike pouches (haustra) giving it a
sgmented appearance
• Haustra permit expansion and elongation of
colon

Colon Muscles
• 3 longitudinal bands of smooth muscle
(taeniae coli) run along outer surfaces of
colon deep to the serosa (similar to outer
layer of muscularis externa)
• Muscle tone in taeniae coli creates the
haustra

Large Intestine
• It consists of: appendix, colon, rectum and anal canal.
• Mucosa: Absence of Plicae circulares and villi
Presence of Microvilli
Presence of Crypts of Lieberkuhn
Presence of Goblet cells in large number
• Submucosa
• Muscularis externa:
Inner circular layer - thin compared to small intestine.
Outer longitudinal layer- forms Taenia coli.
• Adventitia: Appendices epiploicae (peritoneum forms
pouch like processes filled with fat)
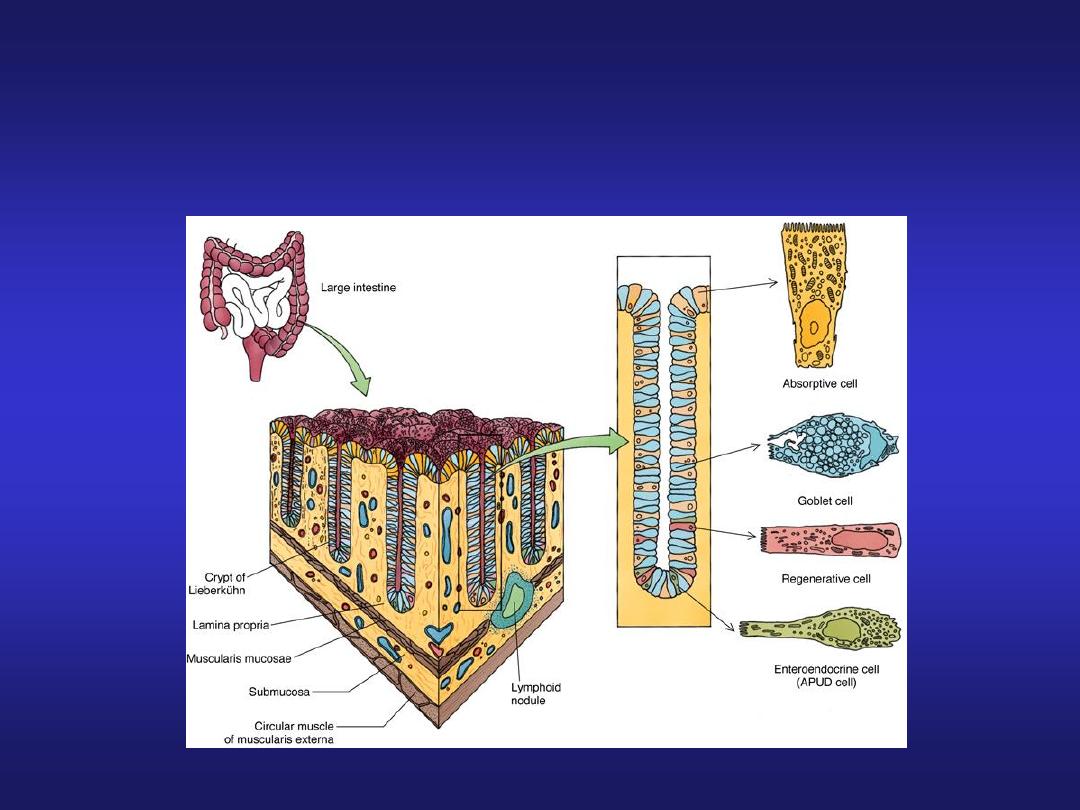
Large Intestine
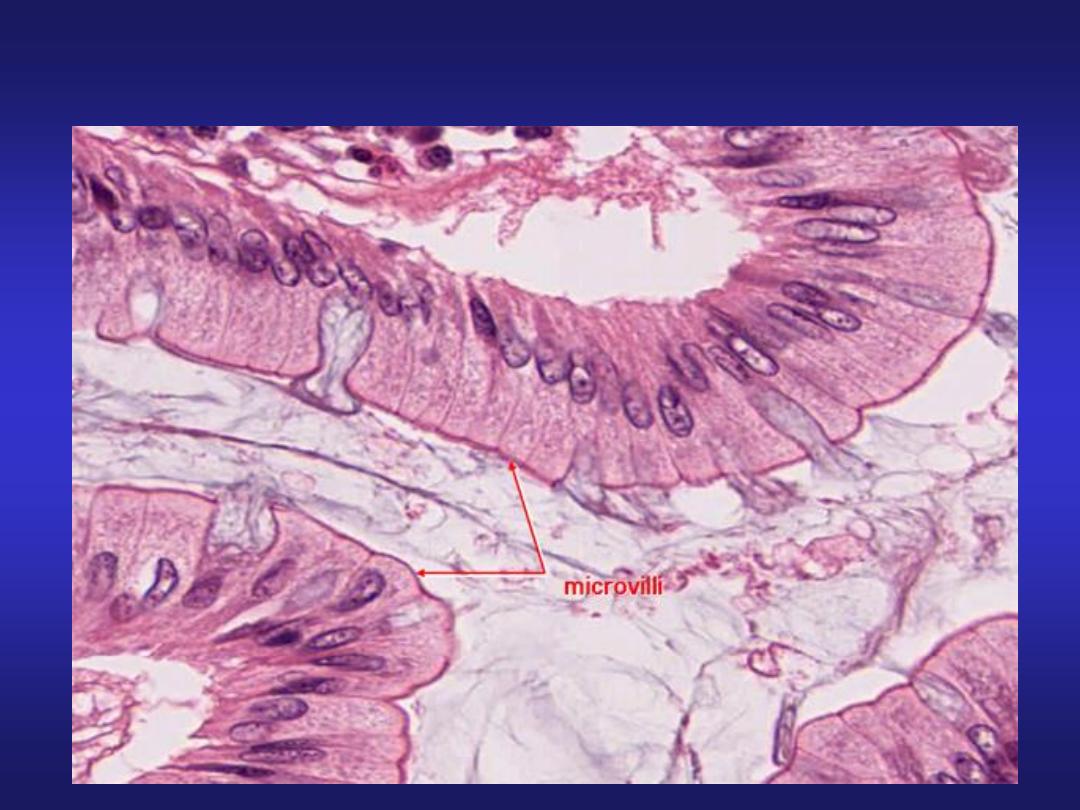
Magnified view of a villus
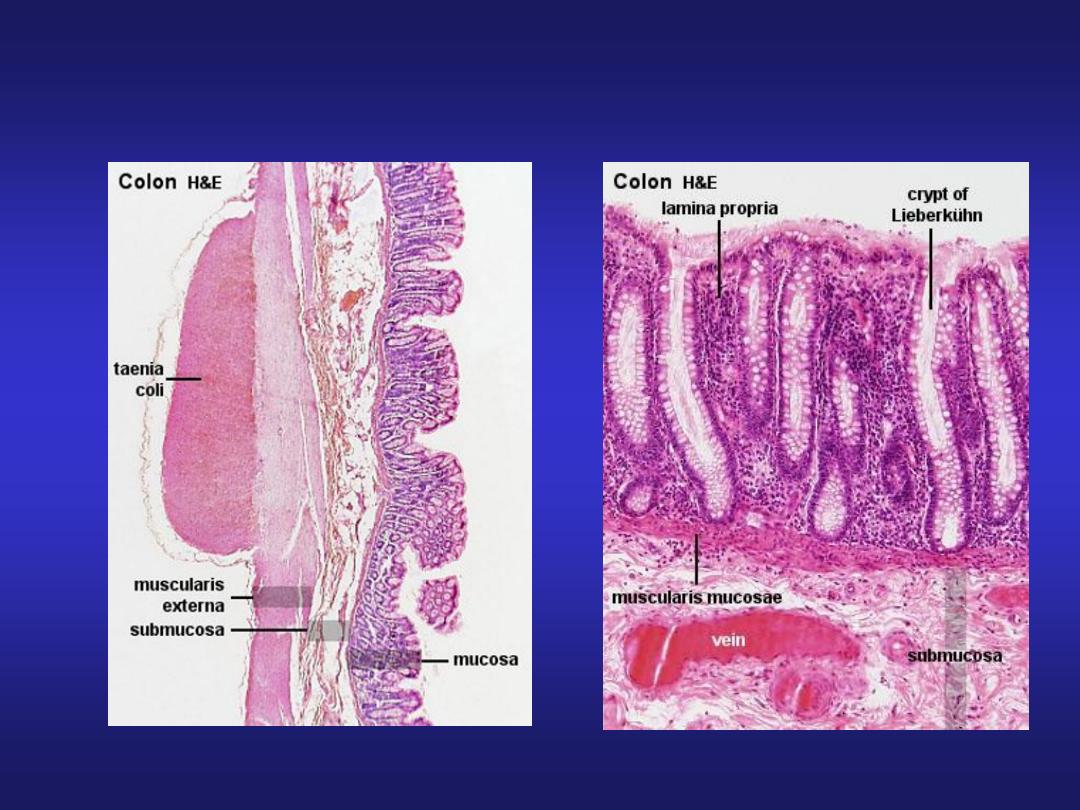
Large Intestine
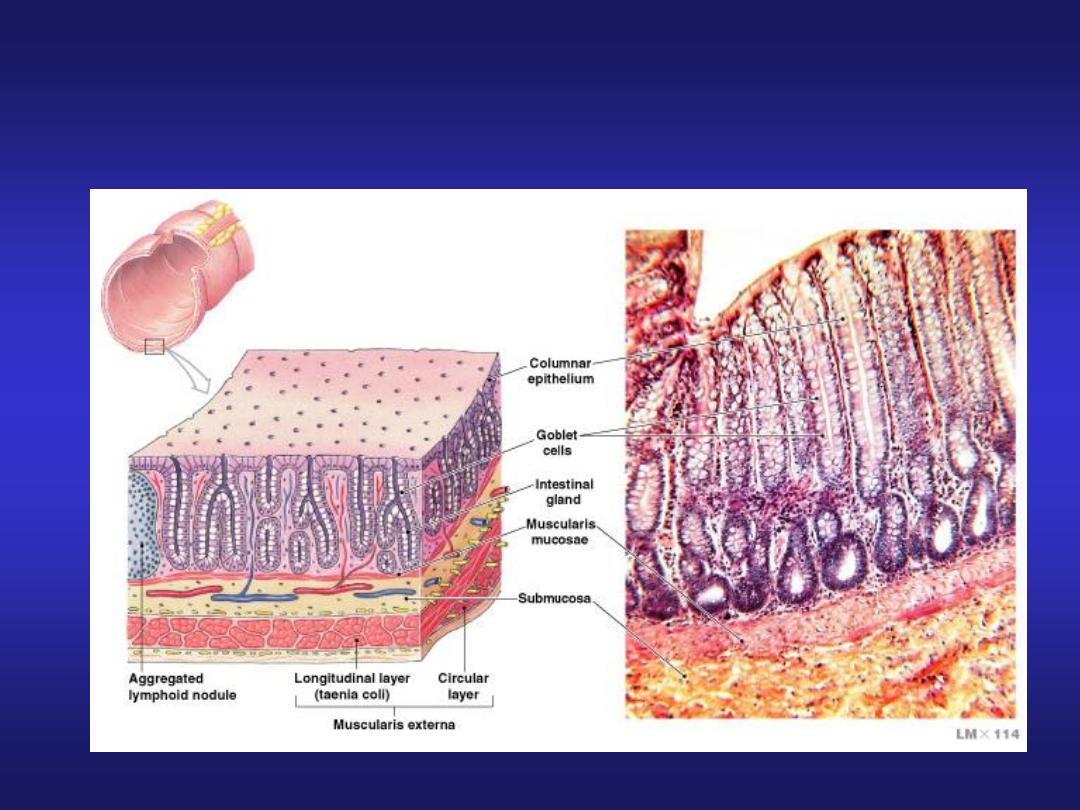
Mucosa and Glands of the Colon
Figure 24–24
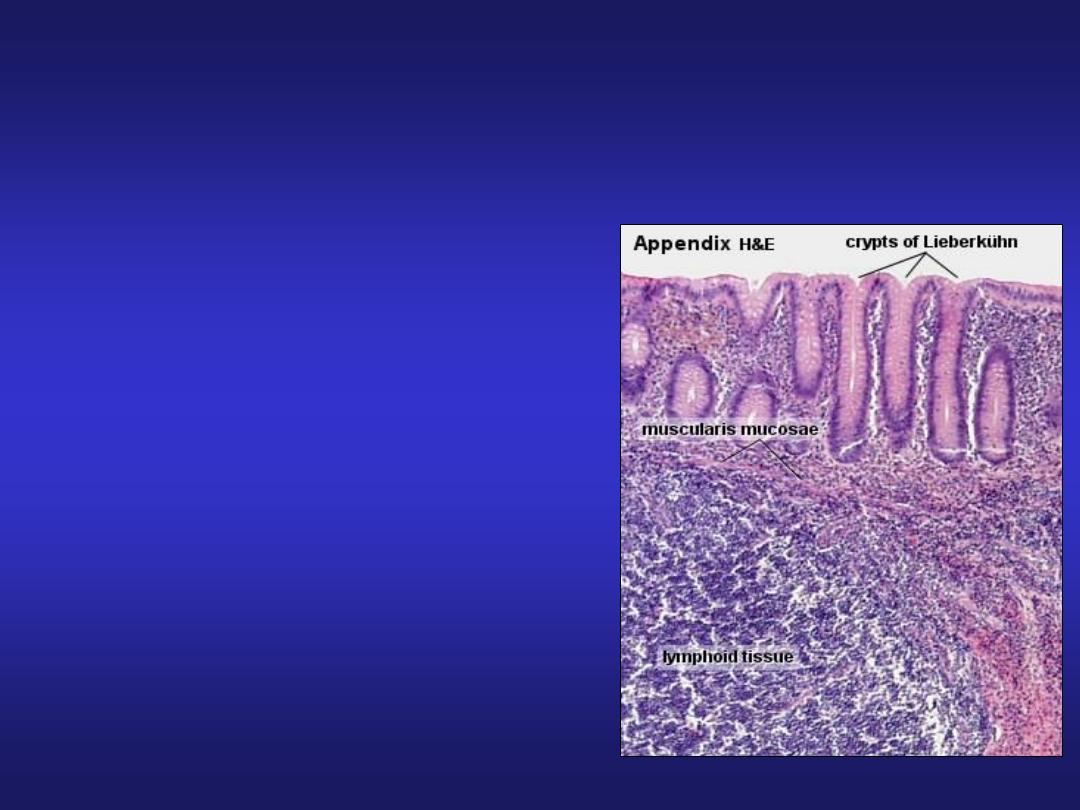
Vermiform Appendix
• A small blind-ending
diverticulum.
• Large accumulations of
lymphoid tissue in lamina
propria which may extend into
submucosa.
• Intestinal villi are usually
absent.
• Crypts are poorly formed.
• Muscularis externa is thin.
• Absence of taenia coli.

Characteristics of the Colon
• Lack villi
• Abundance of goblet cells
• Presence of distinctive intestinal glands in crypts
– deeper than glands of small intestine
– dominated by goblet cells
• Mucosa of the large intestine does not produce
enzymes
– Provides lubrication for fecal material
• Large lymphoid nodules are scattered throughout the
lamina propria and submucosa
• The longitudinal layer of the muscularis externa is
reduced to the muscular bands of taeniae coli
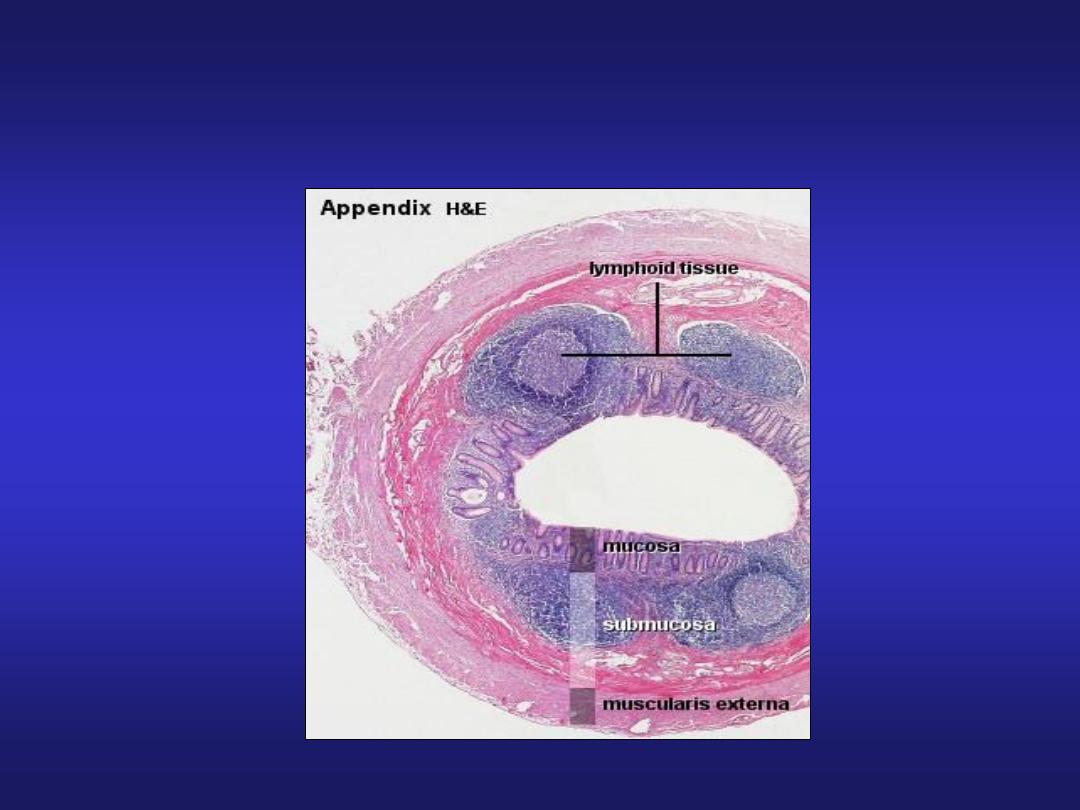
Vermiform Appendix
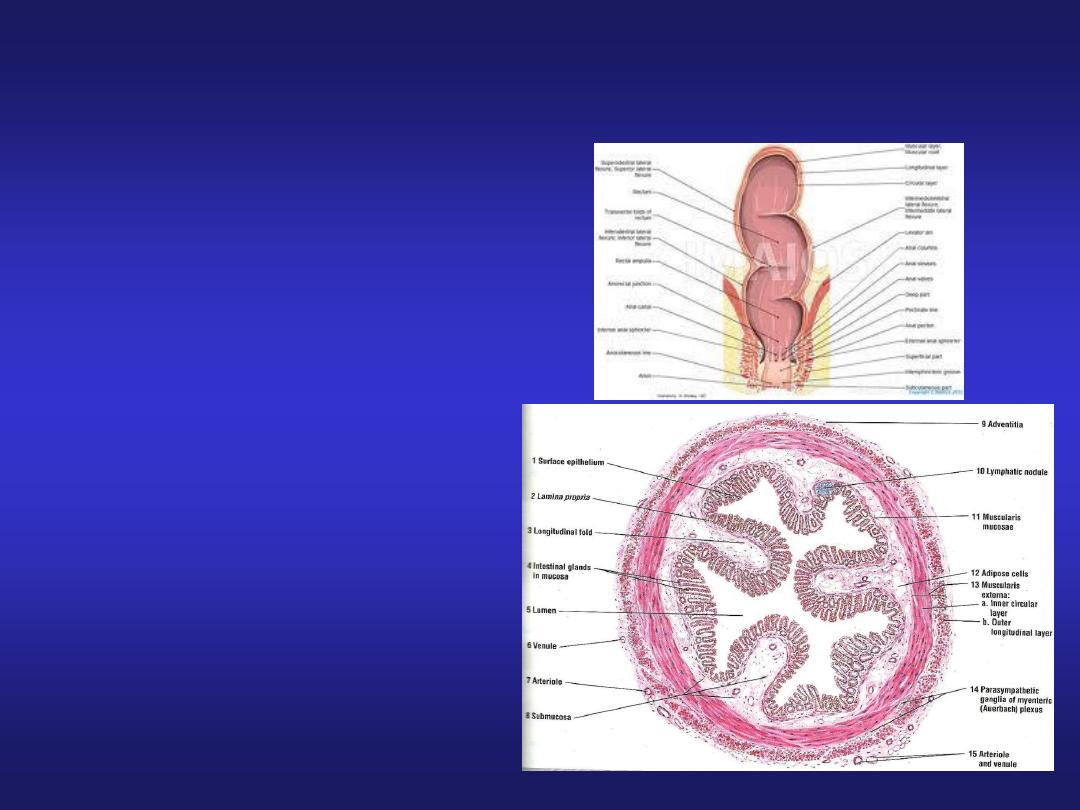
Rectum
• Intestinal glands are
straight, like test tubes.
• A continuous coat of
longitudinal muscle is
present.
• Absence of taenia.
• Absence of appendices
epiploicae.
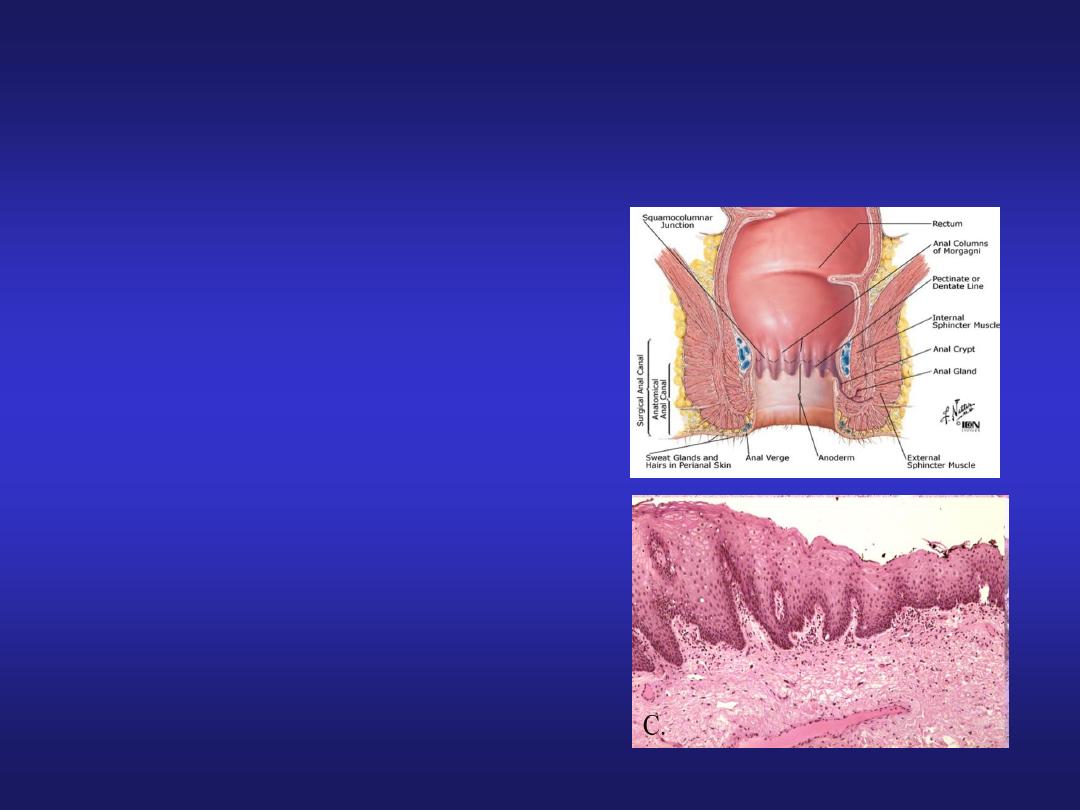
Anal Canal
• Epithelium: upper part-simple
columnar, middle part-stratified
squamous non-keratinized, lower
part-covered by true skin.
• Mucosa has characteristic
longitudinal folds-Anal columns.
• Small mucosal folds between the
anal columns -Pectinate line.
• Crypts disappear below this line.
• Muscularis externa-circular muscle
forms involuntary internal anal
sphincter.
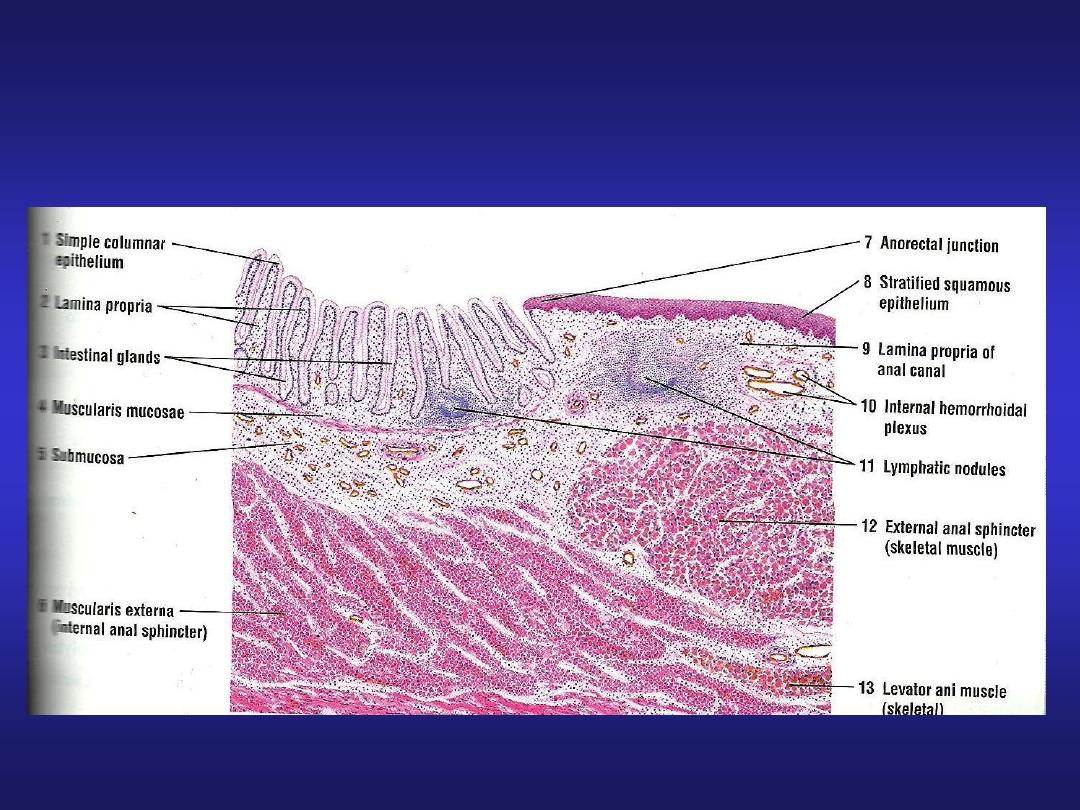
Ano-rectal Junction
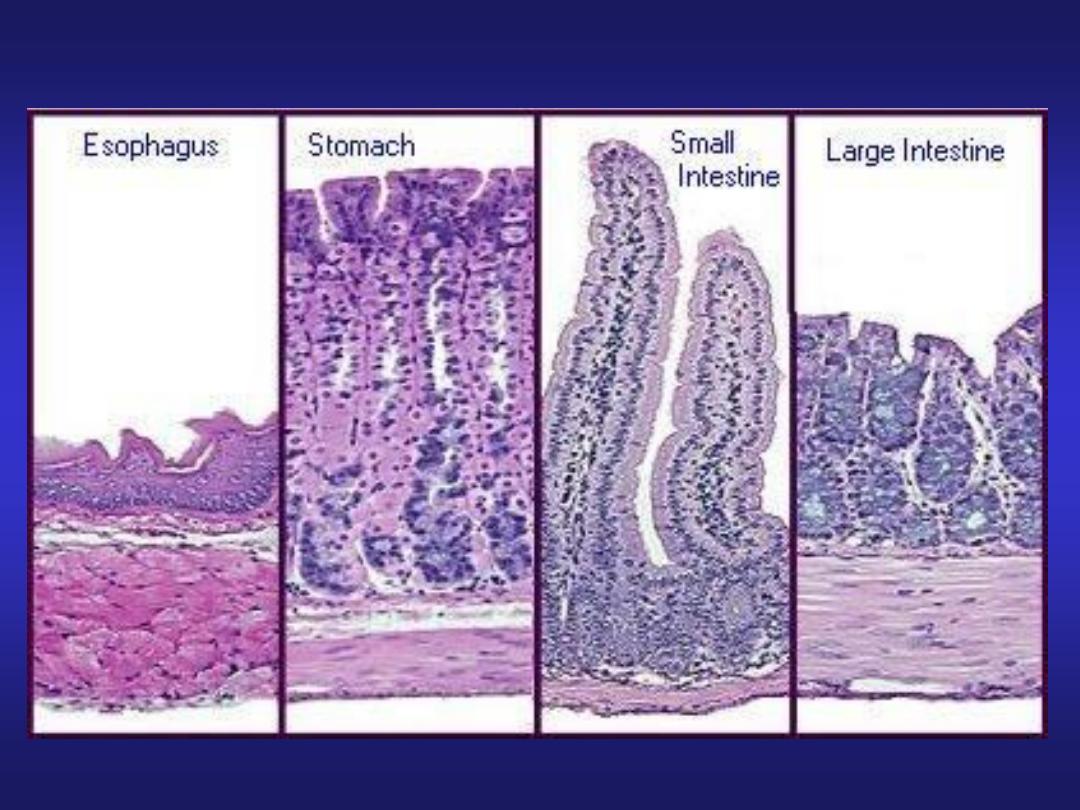

MCQ
Q3. Plica circularis is a feature of:
a. Oesophagus
b. Stomach
c. Small intestine
d. Large intestine

MCQ
Q4. Taenia coli is present in:
a. Oesophagus
b. Stomach
c. Small intestine
d. Large intestine

MCQ
Q5. Abundant lymphoid tissue in lamina propria
is a feature of:
a. Oesophagus
b. Stomach
c. Duodenum
d. Appendix
