*
Assest.prof.Dr.Hameed N. Mousa
Cosultant pathology.

MALE REPRODUCTIVE SYSTEM
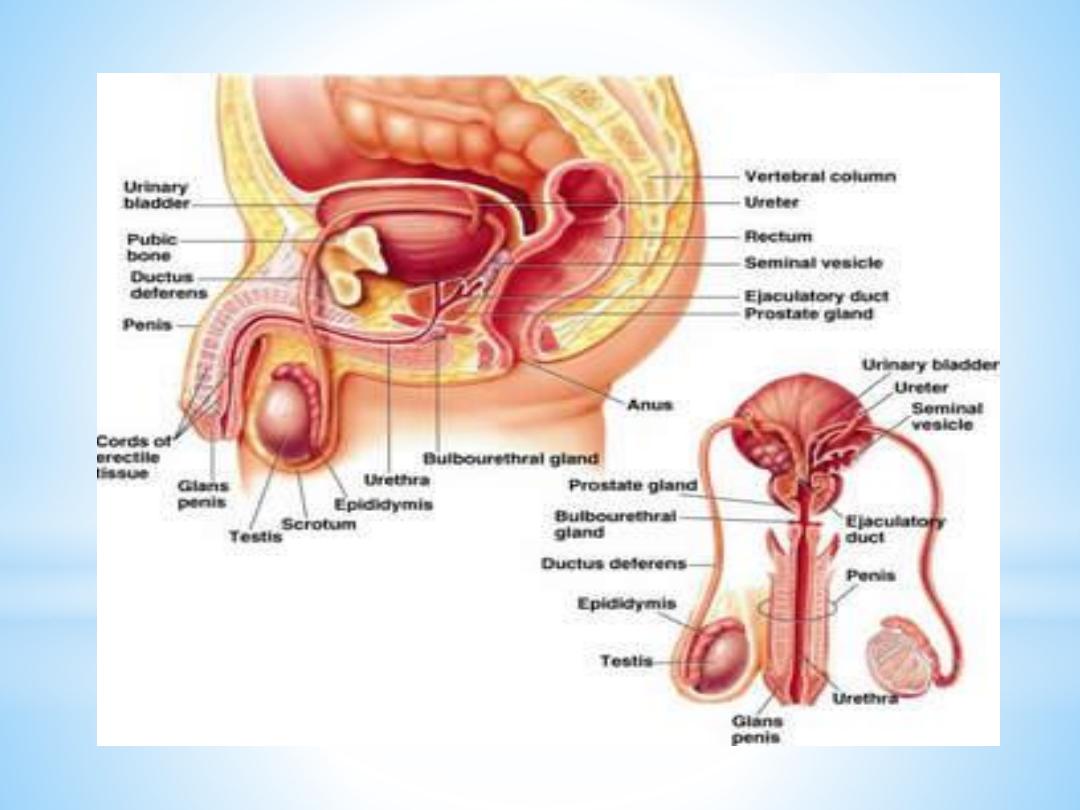
The internal male genitalia consist of the testes with the
adjoining epididymis, the vas deferens and the accessory
sex glands, namely the seminal vesicles, the prostrate and
the bulbourethral glands (the latter sometimes are
included in the external genitalia).

Testes
The testes have, like the ovaries, two functions:
1- they
produce the male gametes or spermatozoa,
2-they produce male sexual hormone, testosterone, which stimulates the accessory male sexual organs and causes the development of the masculine extragenitalsex characteristics.
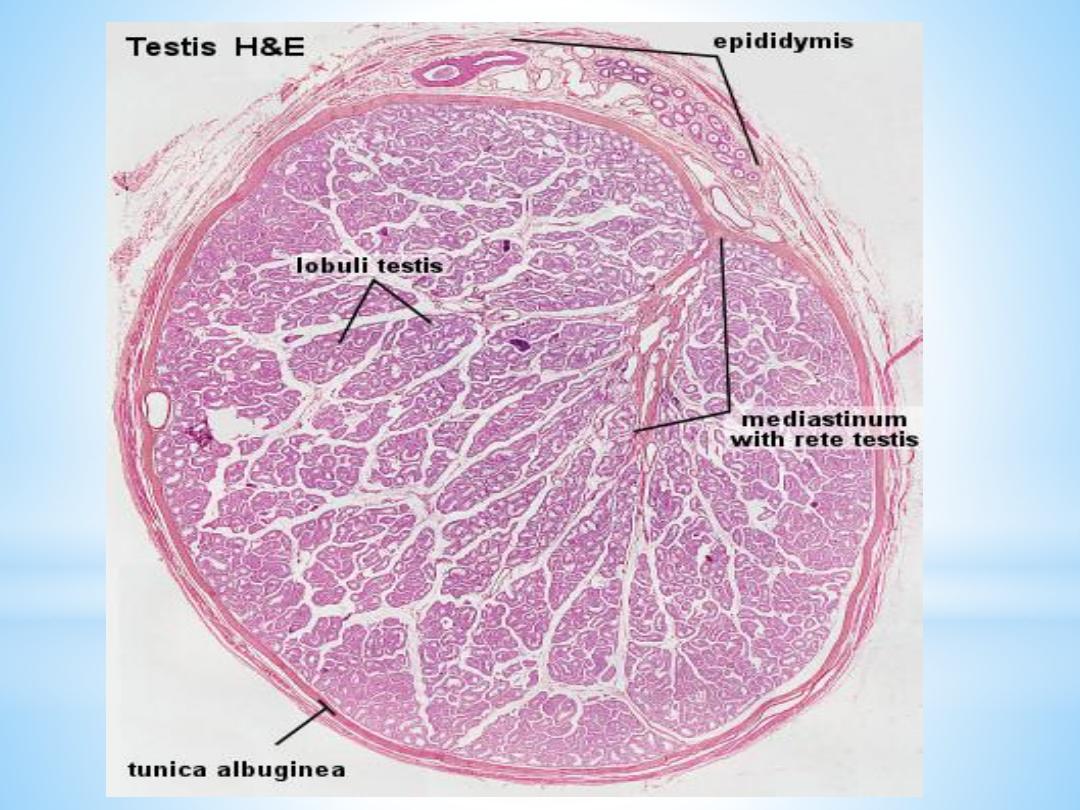
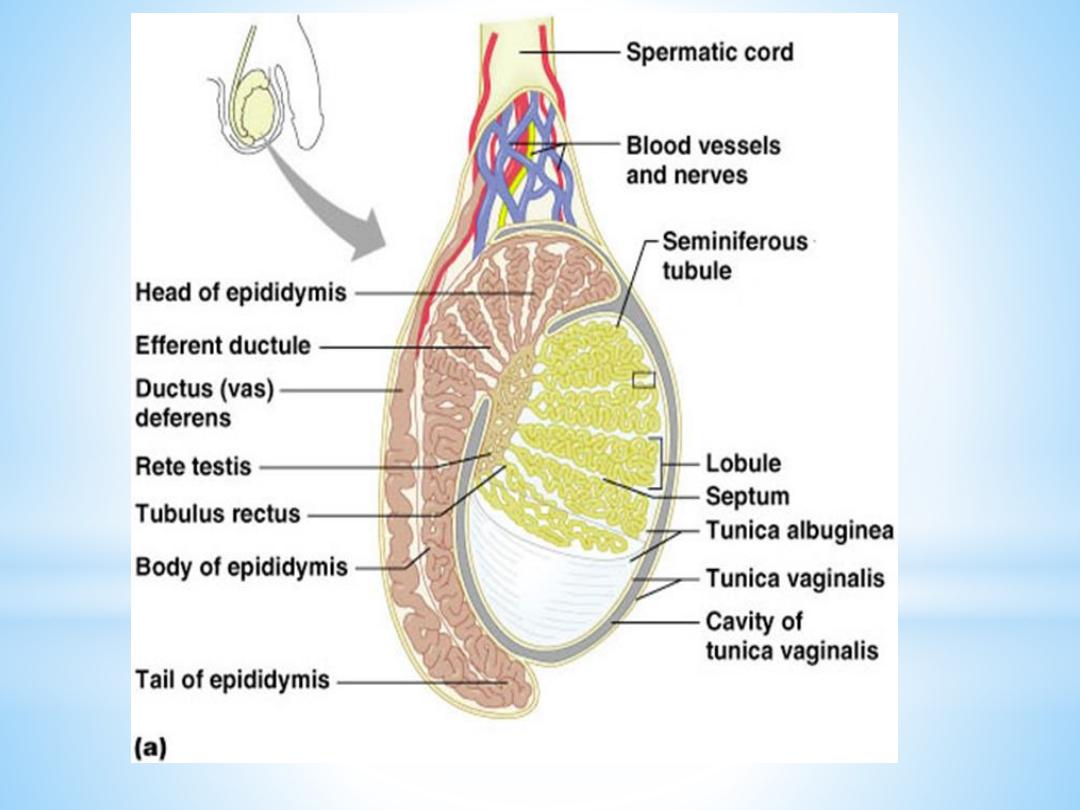
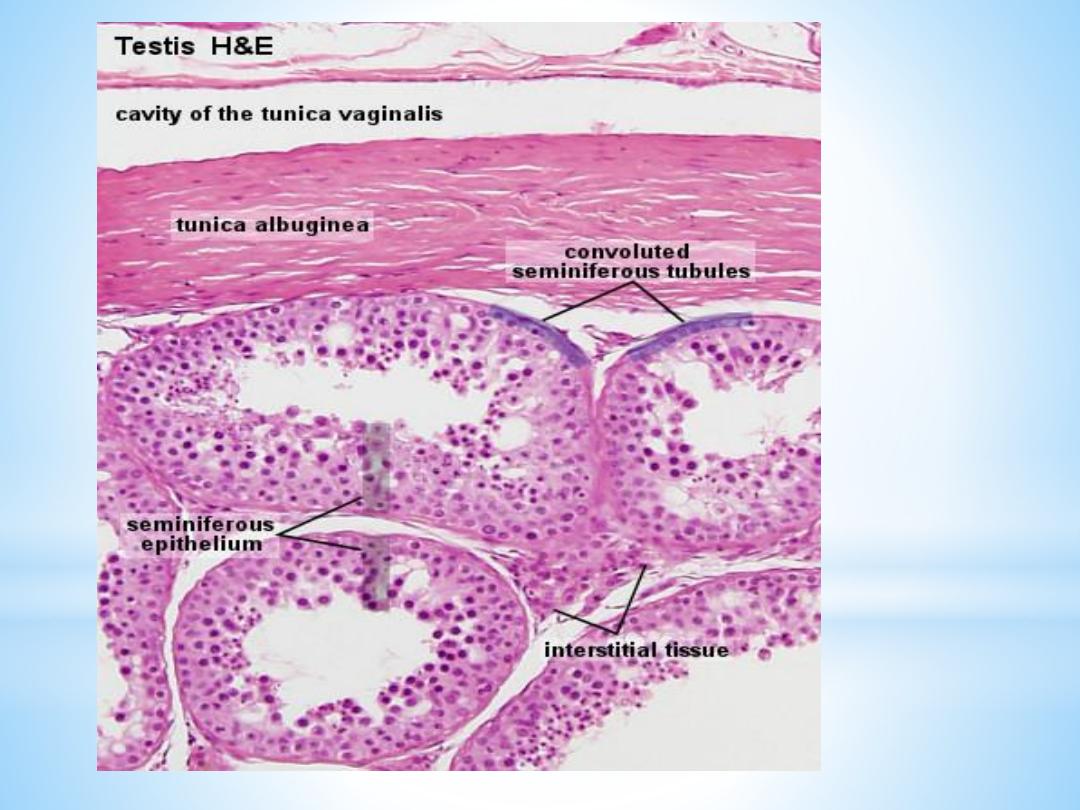
The testis is surrounded by a thick capsule, the
tunica albuginea
, from which a conical mass of connective tissue, the
mediastinum testis
, projects into the testis. The tunica albugineais covered externally by
a serosa.
.

From the mediastinum, delicate fibrous septa radiate towards
the tunica albuginea and divide the parenchyma of the testis
into about
300 lobuli testis
, which communicate peripherally.
Each lobule contains ;
1-4 convoluted seminiferous tubules
(about 150-300 µm in
diameter, 30-80 cm long).
Interstitial tissue between the convoluted tubules is continuous
with a layer of loose vascular connective tissue, the
tunica
vasculosa testis
, which is found beneath the tunica albuginea.
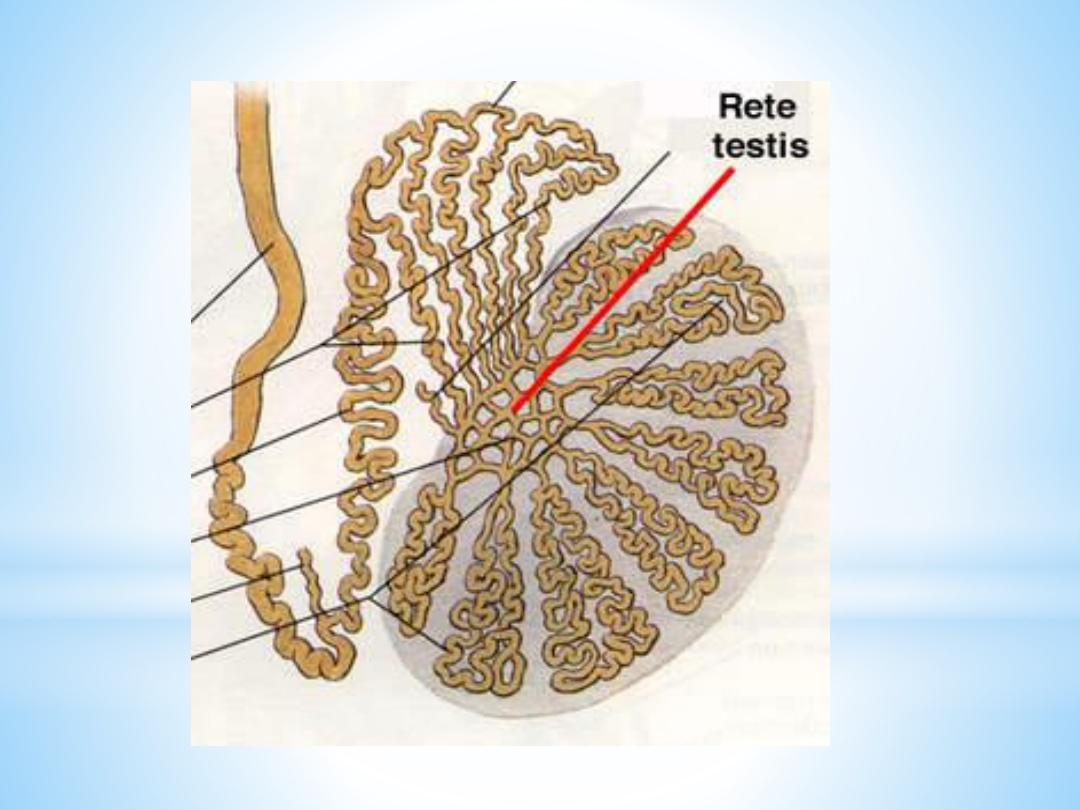
Each seminiferous tubule continues near the mediastinum into
a straight tubule, a
tubulus rectus
. The straight tubules
continue into the
rete testis
, a labyrinthine system of cavities
in the mediastinum
.

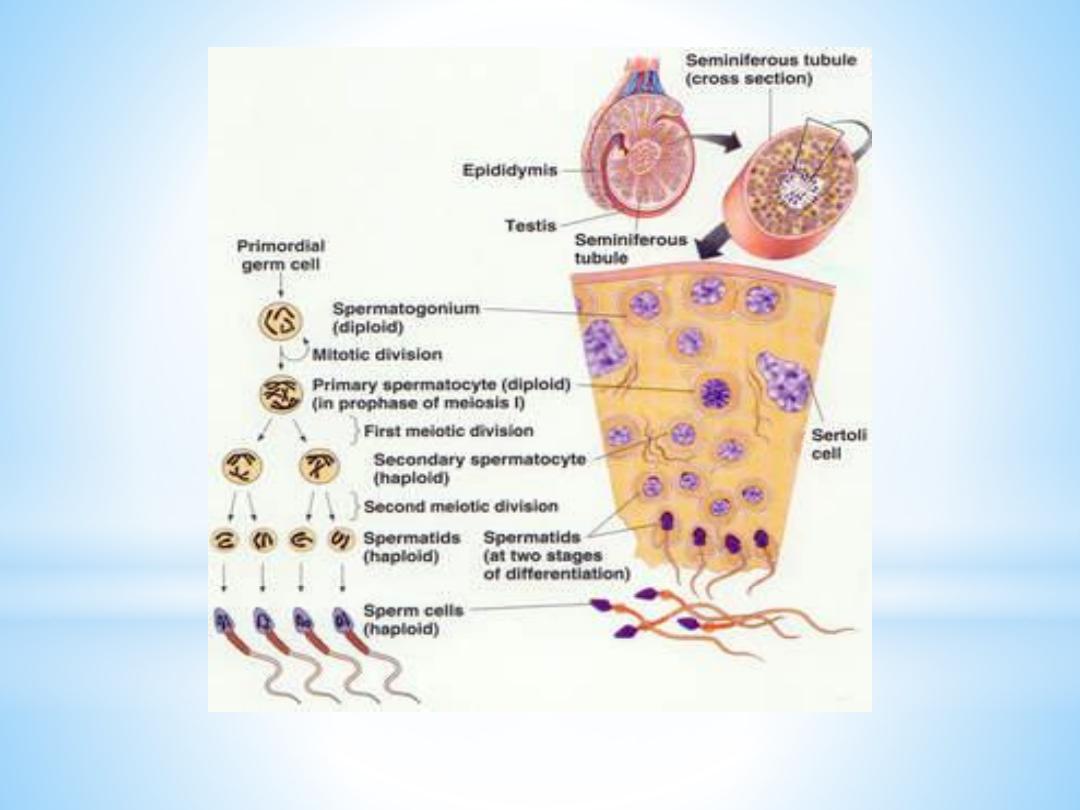
The Convoluted Seminiferous Tubules
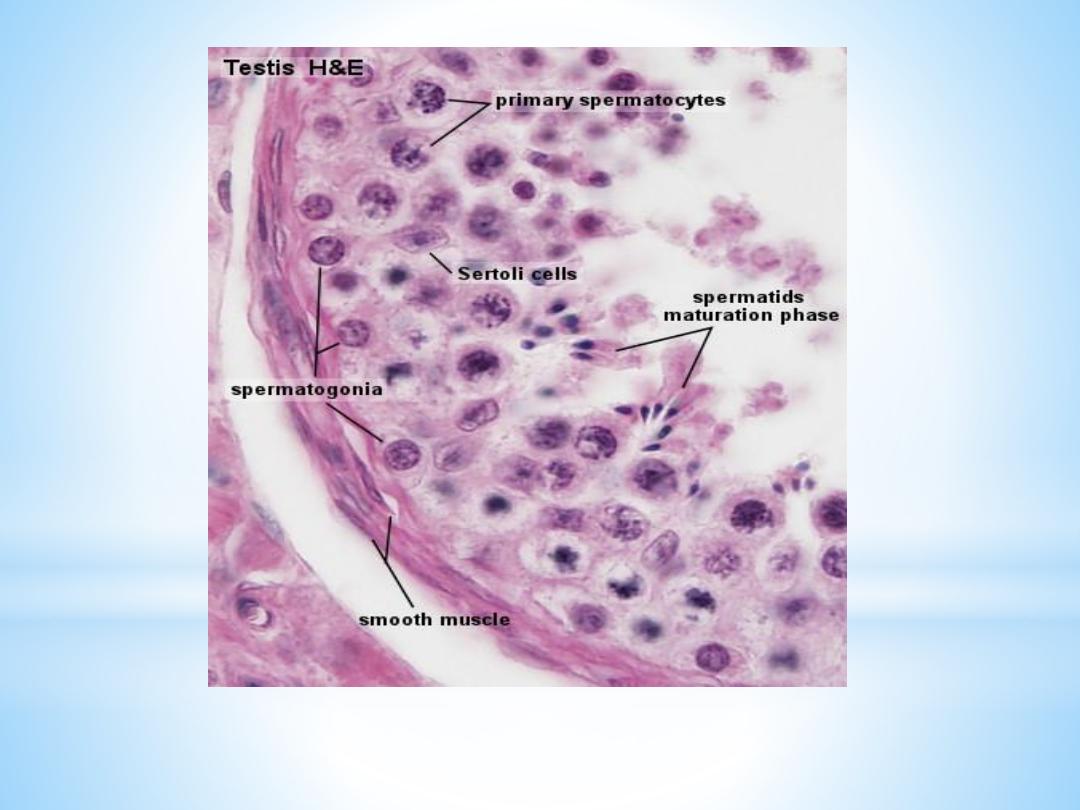
These tubules are enclosed by a thick basal lamina and surrounded by 3-4 layers of
smooth muscle cells (or myoid cells). The insides of the tubules are lined with
seminiferous epithelium, which consists of two general types of cells:
spermatogenic cells and Sertoli cells.
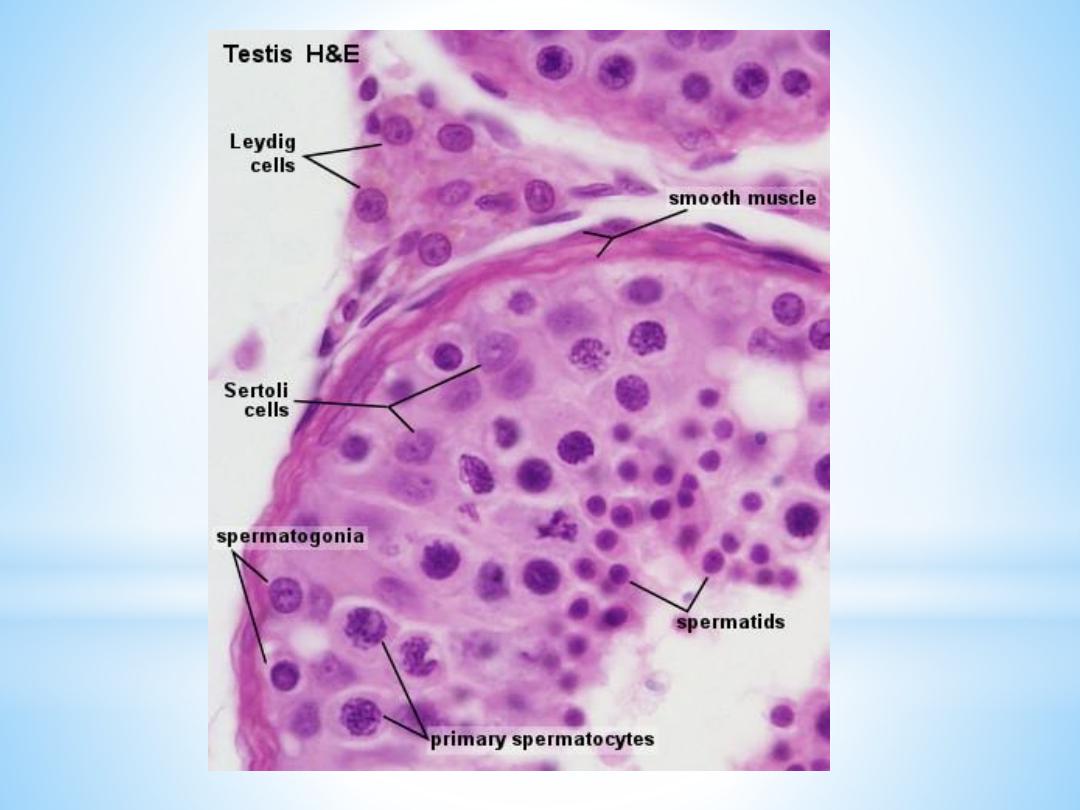
Spermatogenic cells:
Spermatogonia
are the first cells of spermatogenesis. They originate in the 4th week of foetal
development in the endodermal walls of the yolk sac and migrate to the
primordium of the testis, where they differentiate into spermatogonia.
Spermatogonia remain dormant until puberty. They are always in contact with the
basal lamina of the tubule.
Two types of spermatogonia can be distinguished in the human seminiferous
epithelium:
Type A spermatogonia
have a rounded nucleus with very fine chromatin grains and
one or two nucleoli. They are stem cells which divide to form new generations of
both type A and type B spermatogonia.
Type B spermatogonia
have rounded nuclei with chromatin granules of variable
size, which often attach to the nuclear membrane, and one nucleolus. Although
type B spermatogonia may divide repeatedly, they do not function as stem cells and
their final mitosis always results in the formation of primary spermatocytes.

Primary spermatocytes
which lie in the cell layer luminal to the spermatogonia. They appear larger than
spermatogonia. They immediately enter the prophase of the first meiotic division,
which is extremely prolonged (about 22 days!). A large number of primary
spermatocytes is always visible in cross-sections through seminiferous tubules.
Cell divisions, from the formation of primary spermatocytes and onwards, to the
production of the spermatocytes, are incomplete. The cells remain connected by
bridges of cytoplasm. The completion of the first meiotic division results in the
formation
of secondary
spermatocytes

Secondary spermatocytes
,
which are smaller than primary spermatocytes. They rapidly enter and
complete the second meiotic division and are therefore seldom seen in
histological preparations. Their division results in the formation of spermaids.
Spermatids,
which lie in the luminal part of the seminiferous epithelium. They are small
(about 10 µm in diameter) with an initially very light (often eccentric)
nucleus. The chromatin condenses during the maturation of the spermatids
into spermatozoa, and the nucleus becomes smaller and stains darker.

The terminal phase of spermatogenesis is called spermiogenesis and
consists of the differentiation of the newly formed spermatids into
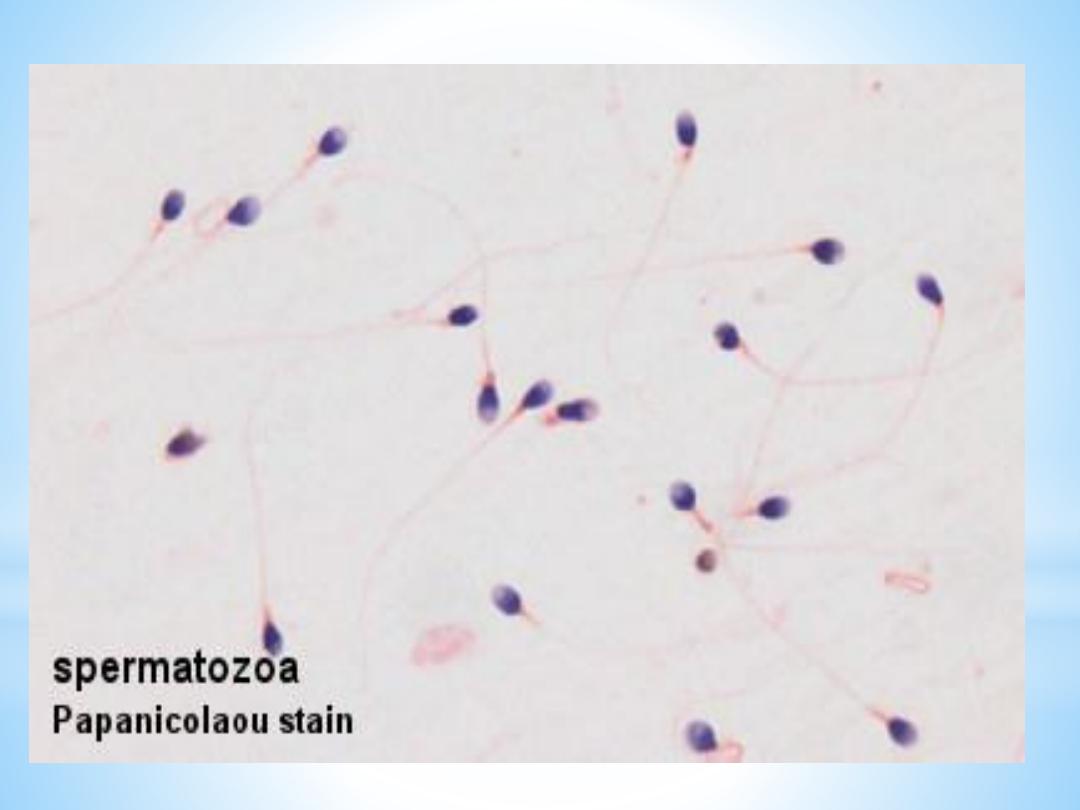
Spermatozoa
The mature human spermatozoon is about 60 µm long and actively motile.
It is divided into head, neck and tail.
The head (flattened, about 5 µm long and 3 µm wide) chiefly consists of
the nucleus (greatly condensed chromatin!). The anterior 2/3 of the
nucleus is covered by the acrosome, which contains enzymes important in
the process of fertilisation. The posterior parts of the nuclear membrane
forms the so-called basal plate.
The neck is short (about 1 µm) and attached to the basal plate. A
transversely oriented centriole is located immediately behind the basal
plate. The neck also contains nine segmented columns of fibrous material,
which continue as the outer dense fibres into the tail.
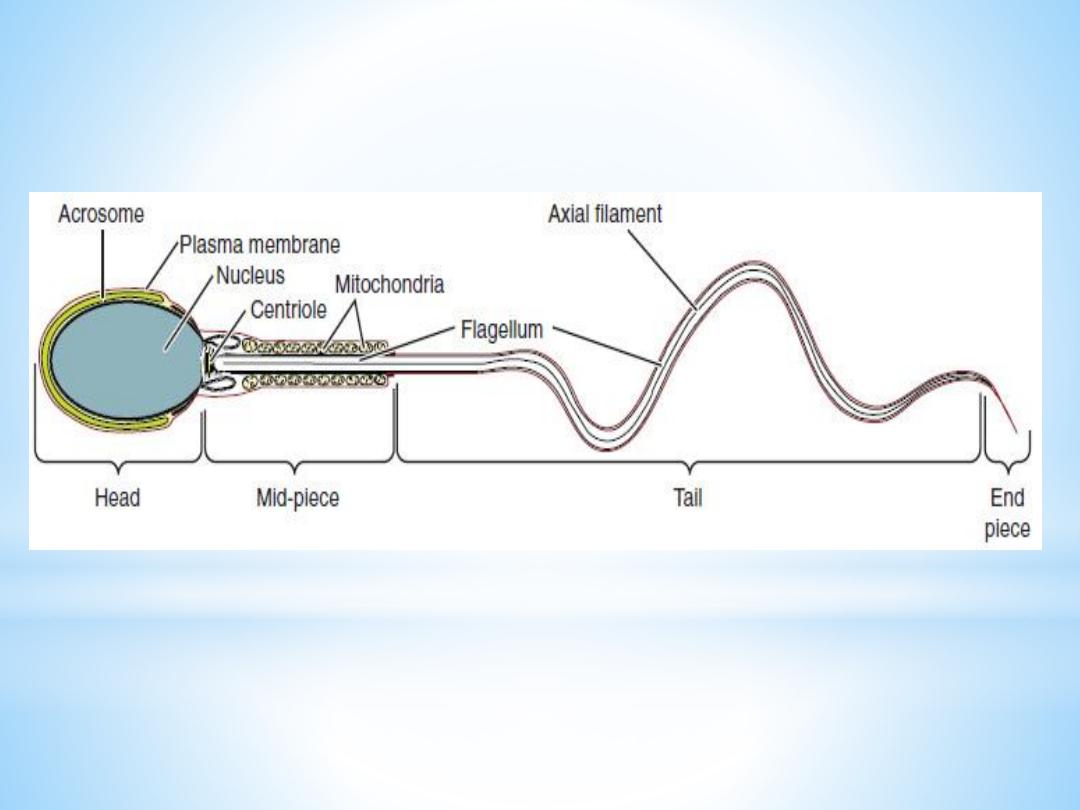

The tail is further divided into a middle piece, a principal piece and
an end piece. The axonema (the generic name for the arrangement
of microtubules in all cilia) begins in the middle piece. It is
surrounded by nine outer dense fibres, which are not found in other
cilia. In the middle piece (about 5 µm long), the axonema and dense
fibres are surrounded by a sheath of mitochondria. The middle piece
is terminated by a dense ring, the annulus. The principal piece is
about 45 µm long. It contains a fibrous sheath, which consists of
dorsal and ventral longitudinal columns interconnected by regularly
spaced circumferential hoops. The fibrous sheath and the dense
fibres do not extend to the tip of the tail. Along the last part (5 µm)
of the tail, called the end piece, the axonema is only surrounded by
a small amount of cytoplasm and the plasma membrane
.

Spermatogenesis.
takes about 48 days from the time cells enter meiosis until morphologically
mature spermatozoa are formed. Depending on the length of reproduction of
spermatogonia (which is not precisely determined) it takes approximately 64
days to complete spermatogenesis.
Spermatogenesis is regulated by follicle stimulating hormone (FSH), which in
males stimulates the spermatogenic epithelium, and luteinizing-hormone (LH),
which in males stimulates testosterone production by Leydig cells in the
interstitia

Sertoli cells
are far less numerous than the spermatogenic cells and are evenly
distributed between them. Their shape is highly irregular - columnar is the
best approximation. Sertoli cells extend from the basement membrane to
the luminal surface of the seminiferous epithelium. Processes of the
Sertoli cells extend in between the spermatogenic cells (cell limits are
therefore not clearly visible in the LM). The nucleus of Sertoli cells is ovoid
or angular, large and lightly stained and often contains a large nucleolus.
The long axis of the nucleus is oriented perpendicular to wall of the
tubule. A fold in the nuclear membrane is characteristic for Sertoli cells
but not always visible in the LM (well ... actually ... it's not that difficult
to find, but not that easy either ....).

Lateral processes of Sertoli cells are interconnected by
tight junctions. Sertoli cells provide mechanical and
nutritive support for the spermatogenic cells. Sertoli cells
also secrete two hormones -
inhibin and activin
- which
provide positive and negative feedback on FSH secretion
from the pituitary
.

Interstitial tissue
Leydig cells (15-20 µm), located in the interstitial tissue between the
convoluted seminiferous tubules, constitute the endocrine component
of the testis. They synthesize and secrete testosterone. Leydig cells
occur in clusters , which are variable in size and richly supplied by
capillaries. The cytoplasm is strongly acidophilic and finely granular.
The nucleus is large, round and often located eccentric in the cell.

Ducts of the Testis
Spermatozoa pass via the tubuli recti (low columnar epithelium) and
the rete testis (flattened or cuboidal epithelium) into numerous
ductuli efferentes, which are lined by a columnar epithelium, which
consists of both absorptive and ciliated cells. The height of the two
cells types which form the epithelium of the ductuli efferentes is
variable which gives the lumen a characteristic wavy outline.

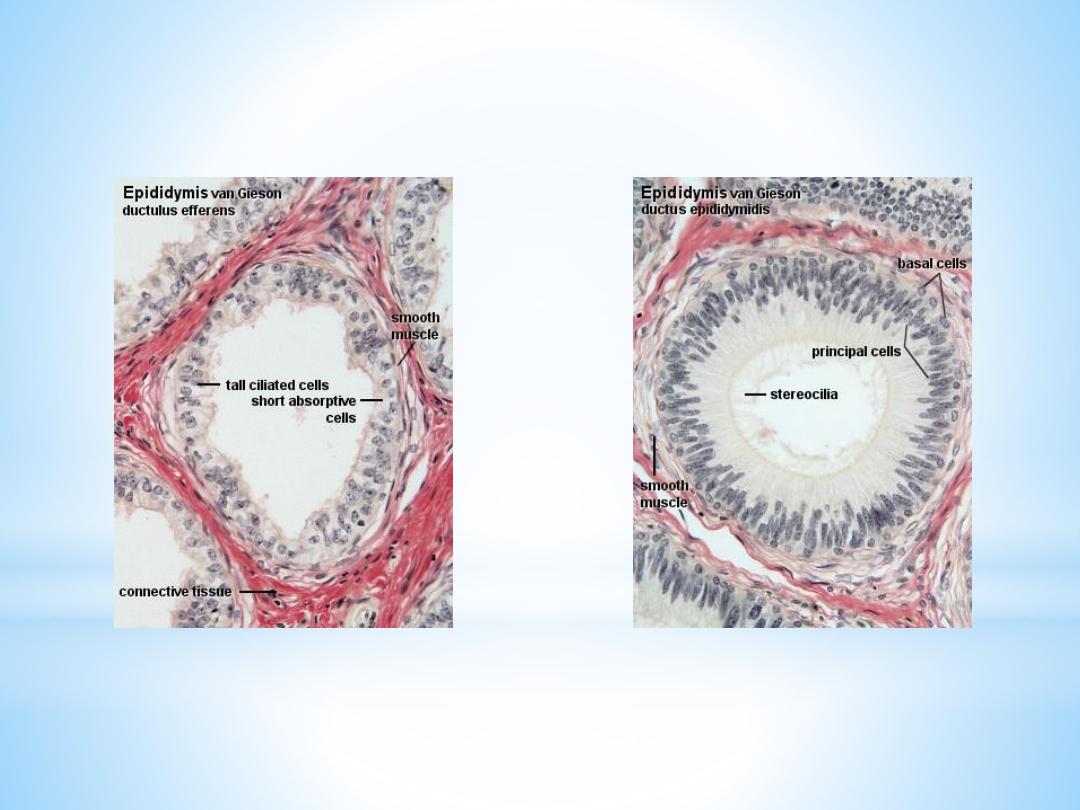
The
ductuli efferentes
leave the testis and open into a common duct, the
ductus epididymidis
(about 6 m long!). It is lined by a very tall pseudostratified
columnar epithelium. Most cells of the epithelium, also called principal cells,
have long stereocilia. Stereocilia are non-motile structures, which in the EM
resemble large microvilli. Towards the basal lamina we see a number of small
nuclei, which belong to the basal cells of the ductus epididymidis. These cells
regenerate the epithelium.
Peristaltic contractions of smooth muscle cells surrounding the ductus
epididymidis move the spermatozoa towards the middle segment of the duct,
which is the
site of final functional maturation of the spermatozoa
- now they are
motile. The terminal segment of the ductus epididymidis is the
site of storage of
the mature spermatozoa
. Smooth muscle fibres of the terminal part of the ductus
epididymidis do not contract spontaneously. They contract during sexual
stimulation concurrently with the contraction of the musculature of the duct into
which it opens, the vas deferens.

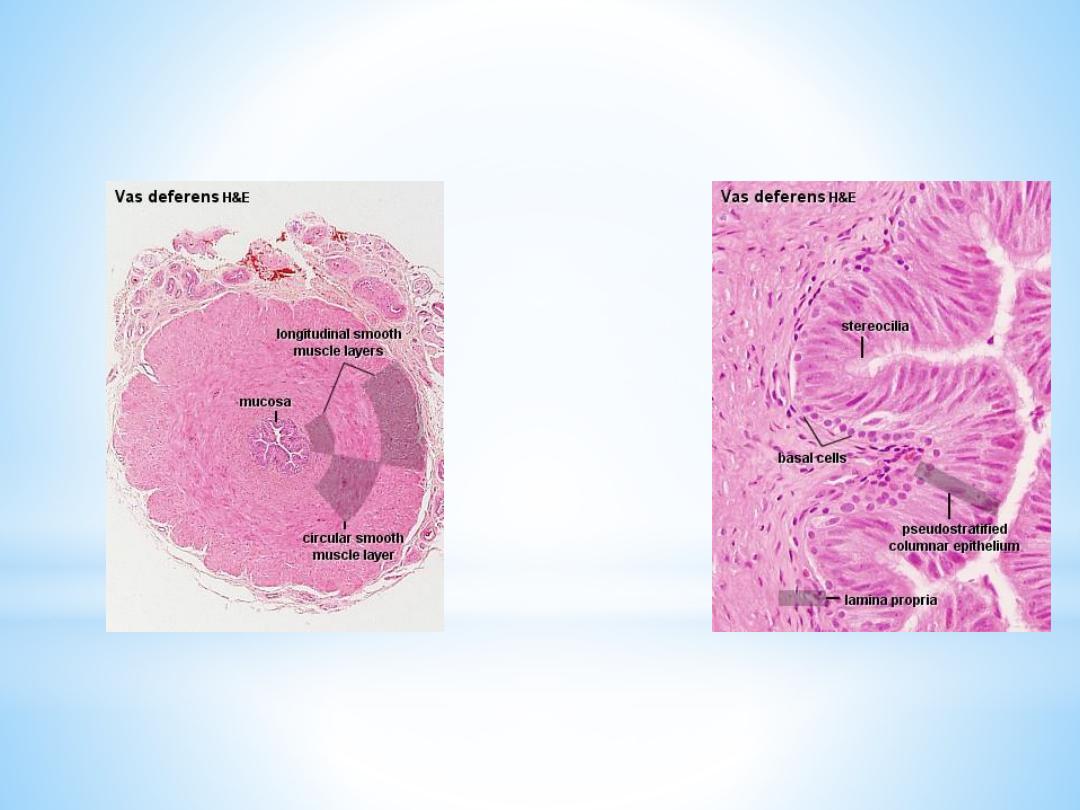
The Vas deferens (or ductus deferens
)
The mucosa of the vas deferens forms low longitudinal folds. It is lined
by a pseudostratified columnar epithelium. Similar to the epididymis,
cells have long stereocilia. The lamina propria is unusually rich in
elastic fibres. The muscularis is well developed (up to 1.5 mm thick)
and consists of a thick circular layer of smooth muscle between thinner
inner and outer longitudinal layers. The muscularis is the structure
which makes the vas deferens palpable in the spermatic cord. The vas
deferens is surrounded by an adventitia, which is slightly denser than
usual
.

Male Accessory Reproductive Glands
The accessory (or secondary) male sex glands consist of the seminal vesicles, the
prostrate and the bulbourethral glands.
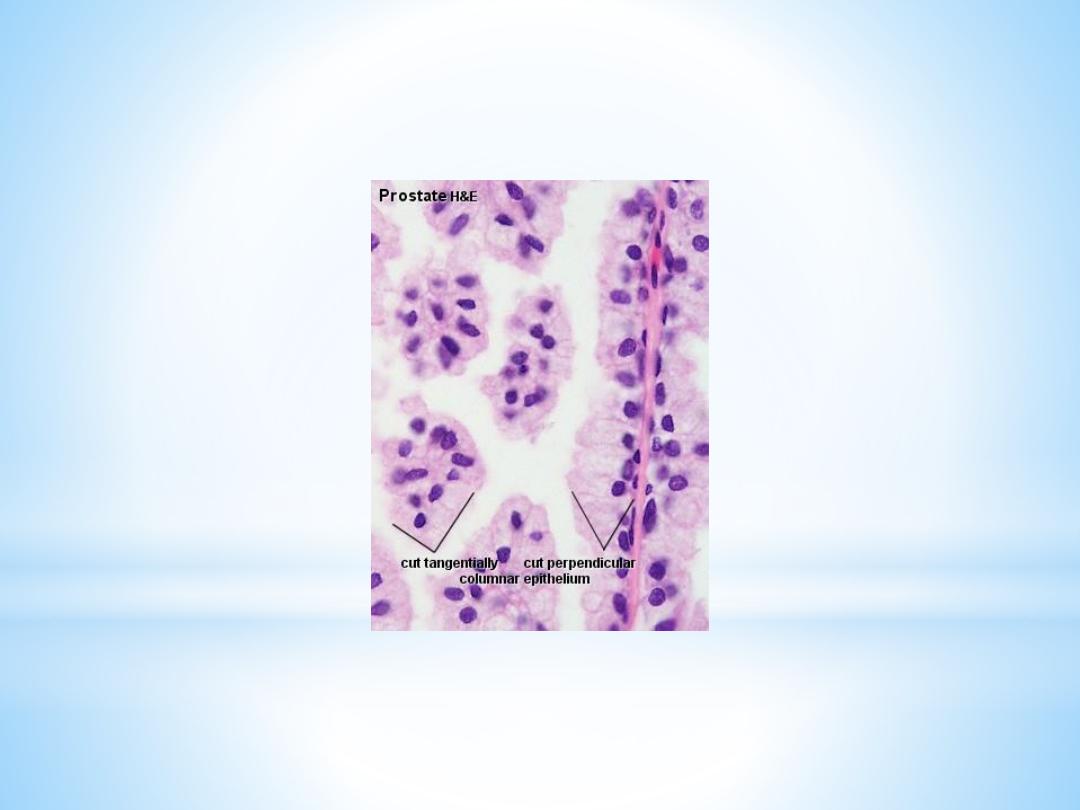
Prostate
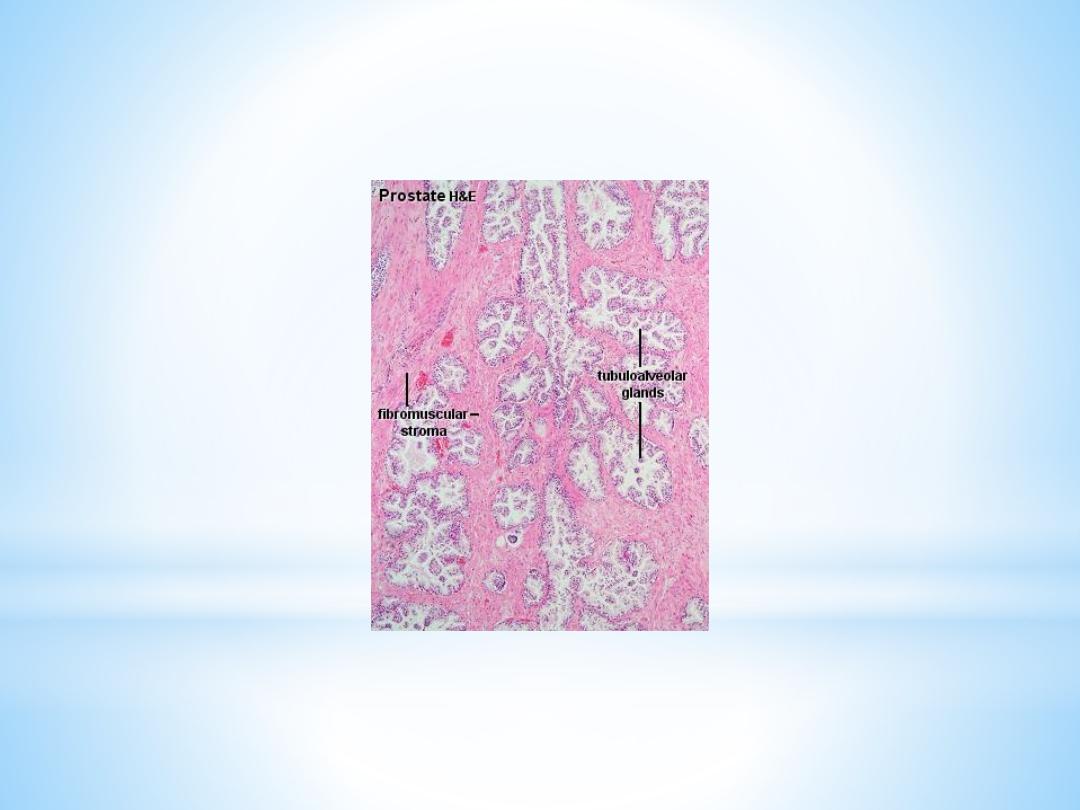
The prostate is the largest accessory sex gland in men (about 2 × 3 × 4 cm). It
contains 30 - 50 tubuloalveolar glands, which empty into 15 - 25 independent
excretory ducts. These ducts open into the urethra. The glands are embedded
into a fibromuscular stroma, which mainly consists of smooth muscle
separated by strands of connective tissue rich in collagenous and elastic
fibres. The muscle forms a dense mass around the urethra and beneath the
fairly thin capsule of the prostrate.

The secretory alveoli of the prostate are very irregularly shaped
because of papillary projections of the mucosa into the lumen of
the gland. The epithelium is cuboidal or columnar. Basal cells are
again present, and the epithelium may look pseudostratified
where they are found. The secretory cells are slightly acidophilic
and secretory granules may be visible in the cytoplasm. Small
extensions of the apical cytoplasm into the lumen of the alveoli
may represent cells which release their secretory products
(secretion is apocrine/merocine). The secretion of the prostate
contains citric acid, the enzyme fibrinolysin (liquefies the semen),
acid phosphatase, a number of other enzymes and lipids. The
secretion of the prostate is the first fraction of the ejaculate.

the secretory ducts of the prostate are lined by a simple
columnar epithelium, which changes to a transitional
epithelium near the openings of the ducts into the urethra.
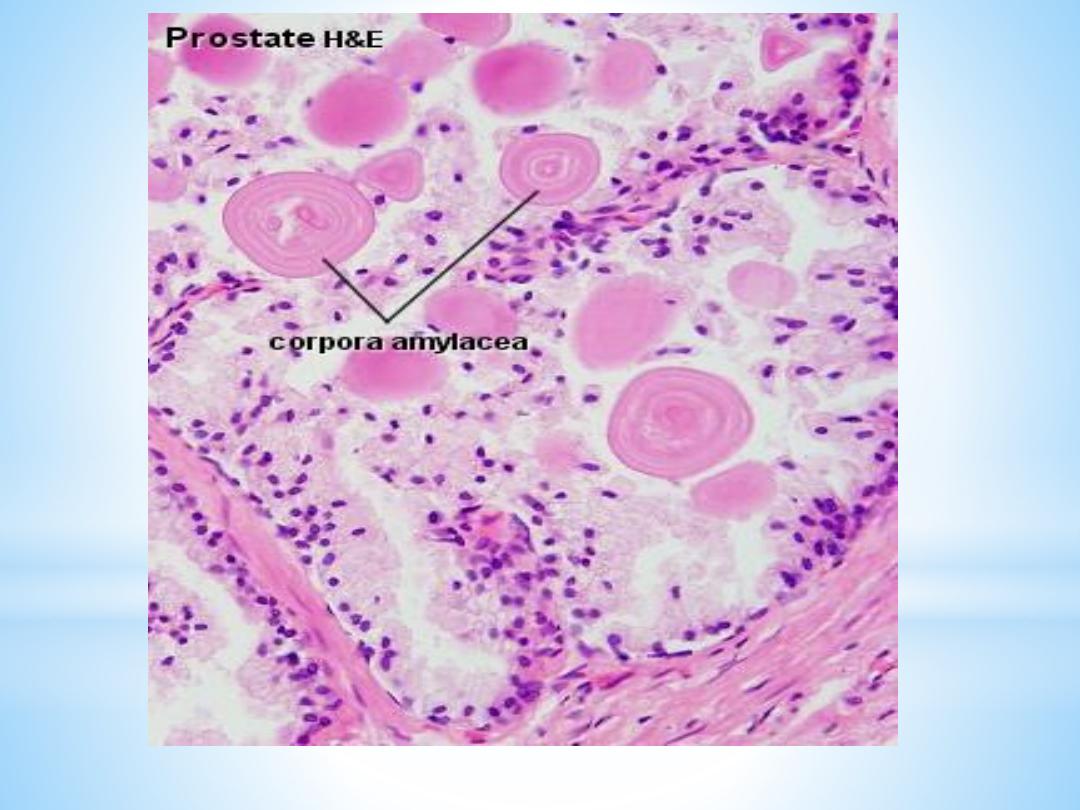
A characteristic feature of the prostate is the appearance
of
corpora amylacea
in the secretory alveoli. They are
rounded eosinophilic bodies. Their average diameter is
about 0.25 mm (up to 2 mm).. They may undergo
calcification. Corpora amylacea may appear in semen.

Macroscopically
the prostrate can be divided into lobes, but they are
inconspicuous in histological sections. In good histological
sections it is possible to distinguish three concentric zones, which
surround the prostatic part of the urethra.
1-The peripheral zone contains large, so-called main glands,
whose ducts run posteriorly to open into the urethra.
2-The internal zone consists of the so-called submucosal glands,
whereas
3-the innermost zone contains mucosal glands.

This subdivision of the prostate is of clinical importance.
With age the prostate becomes enlarged due to benign
nodular hyperplasia. The onset age of these hyperplastic
changes is 45. About 3/4 of the males above 60 are affected
of which half will be symptomatic. This condition affects the
mucosal glands.
Cancer of the prostate, which is the second most common
malignant tumor in western males, involves the peripheral
zone.

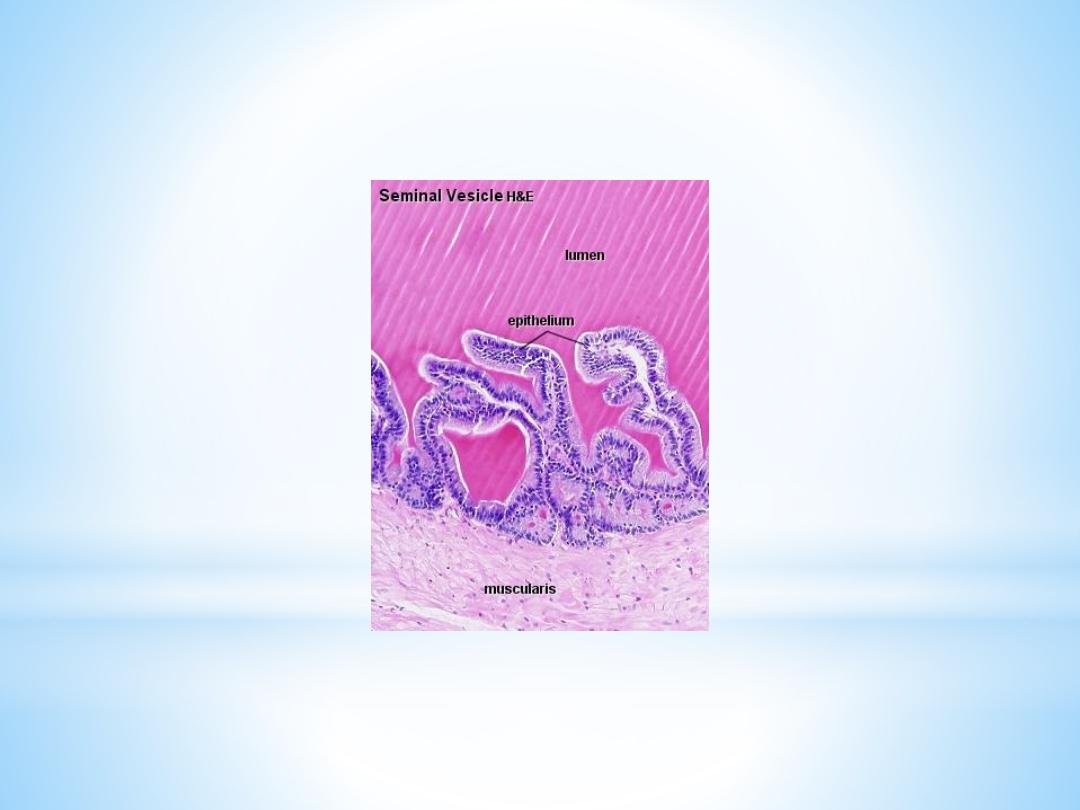
Seminal Vesicles
The seminal vesicles develop from the vas deferens. Their
histological organisation resembles to some extent that of the
vas deferens. They are elongated sacs (about 4 cm long and 2
cm wide), which taper where they unite with the vas
deferens. Each seminal vesicle consists of one coiling tube
(about 15cm long). All the lumina visible in sections of the
seminal vesicle are in continuity in the intact organ.
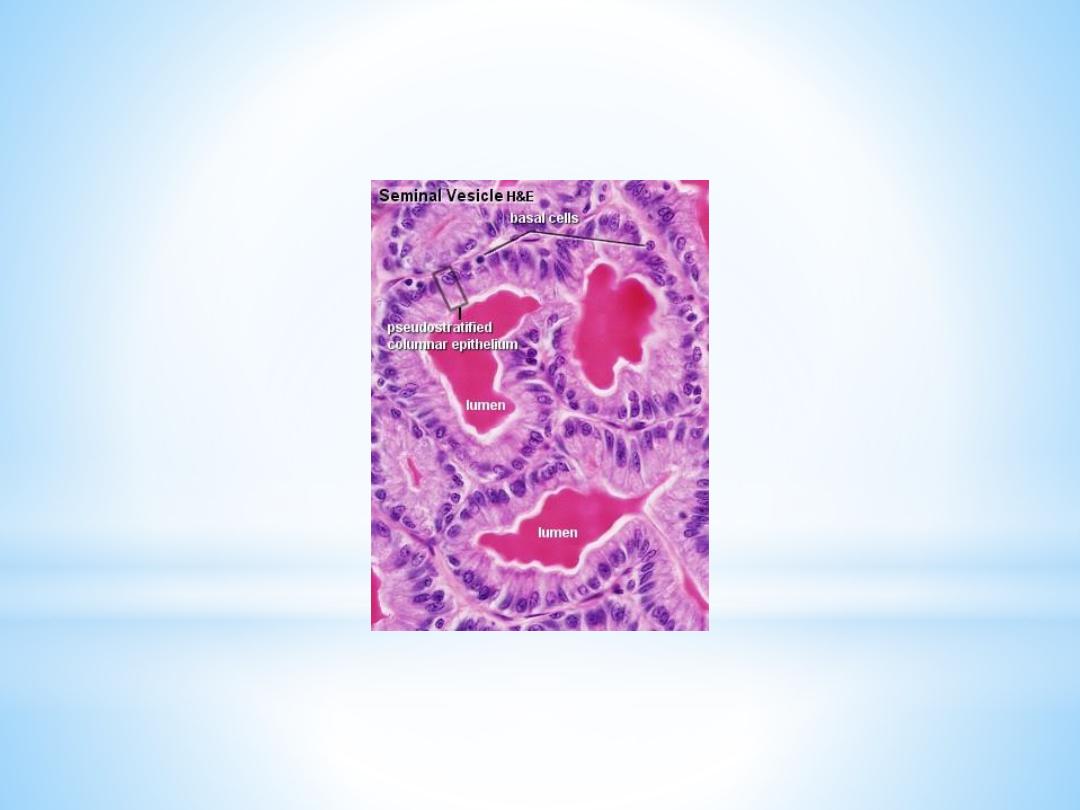
The mucosa shows thin, branched, anastomosing folds. The
structure of the epithelium is variable appearing columnar or
pseudostratified columnar (columnar cells and basal cells).
The lamina propria of the mucosa is fairly thin and loose. The
muscularis consists of inner circular and outer longitudinal
layers of smooth muscle.

Seminal vesicles were thought to store semen - hence there name. This
turned out to be wrong. They are glands, whose secretion constitutes 60-
70 % of the ejaculate. The secretory product of the columnar cell, which
may be seen in the lumen of the seminal vesicles, is strongly acidophilic. It
contains large amounts of fructose which the spermatozoa utilise as a
source of energy. Furthermore, the secretion contains prostaglandins,
flavins (yellow fluorescing pigment - of use in forensic medicine to detect
semen stains) and several other proteins and enzymes.
The cocktail of compounds which is released by the seminal vesicles in
addition to fructose has three main functions:
1-the formation of the sperm coagulum,
2-the regulation of sperm motility and
3-the suppression of immune function in the female genital tract
.
The secretion of the seminal vesicles is the third fraction of the ejaculate
(the spermatozoa are released with the second fraction - the contents of
the vas deferens).