
Fifth Stage
Dermatology
Dr. Hadaf – Lecture 5
1
Psoriasis
–
A common inflammatory disease of skin
–
Chronic relapsing condition
–
Unpredictable course
–
Has a great impact on patient’s life
Emotional impact
Depression
Unattractiveness
Fear about future & prognosis
Wrongly assumed to be contagious
Embarrassment in public places & hair dressers
Epidemiology
–
Prevalence 0.3-25%
–
Equal male & female ratio
–
Estimated incidence 60 per 100000 per year

2
Age of onset
Mean age of onset 23-37
2 peaks with possible genetic associations
1- early onset 16-22 with more severe & aggressive presentation & possible first
degree relative affection
2
_
late onset 57-60 which is milder & absent first degree relative involvement
Pathogenesis
2 key pathophysiological aspects:
1)Increased rate of keratincytes proliferation+ parakeratosis.
2) large inflammatory cell infiltrate as polymorphs, T cells, & others.
Familial component, many relatives affected, increased in successive generations,
multifactorial inheritance.
Psoriasis is a T cell mediated auto-immune disease
Current hypothesis:
–
Unknown skin antigen stimulate immune response
–
Antigen-specific memory T cells are primary mediators
–
Leading to impaired differentiation & hyper proliferation of keratinocytes
Triggering factors in susceptible patients
1-Infection:
β hemolytic strept.
Throat infection precede guttate psoriasis.
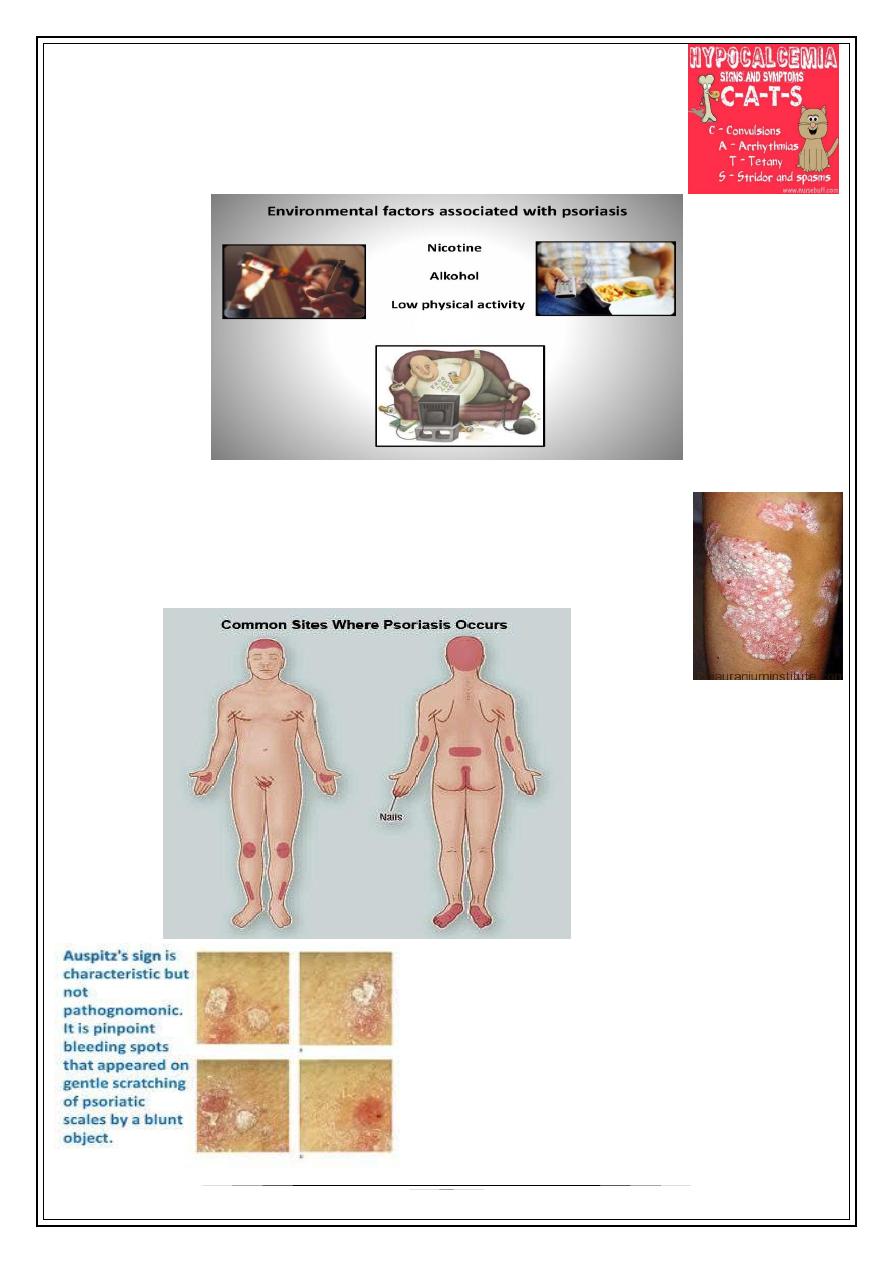
2-Trauma: positive Kobner’s phenomenon
3-Emotion: in 50% stress worsen psoriasis especially in children
4- Drugs: antimalarials, lithium, β blockers worsen psoriasis, stopping steroids
causes rebound of the rash.
3
5-Hypocalcemia
6-Hormonal
7-Role of obesity
–
doubles the risk of psoriasis
–
BMI correlate with psoriasis severity
Clinical features
Well-demarcated, sharply defined erythematous (salmon pink)
plaques covered by silvery white scales. Usually symmetrical
4
Koebner’s phenomenon:
The complaints are (Sorted by the commonest downward):
1. Scales
2. Itching
3. Redness of skin
4. Tightness of skin
5. Bleeding
6. Burning
7. Fatigue
Types of psoriasis
–
Chronic plaque psoriasis
–
The commonest type 85%
–
Can be extensive
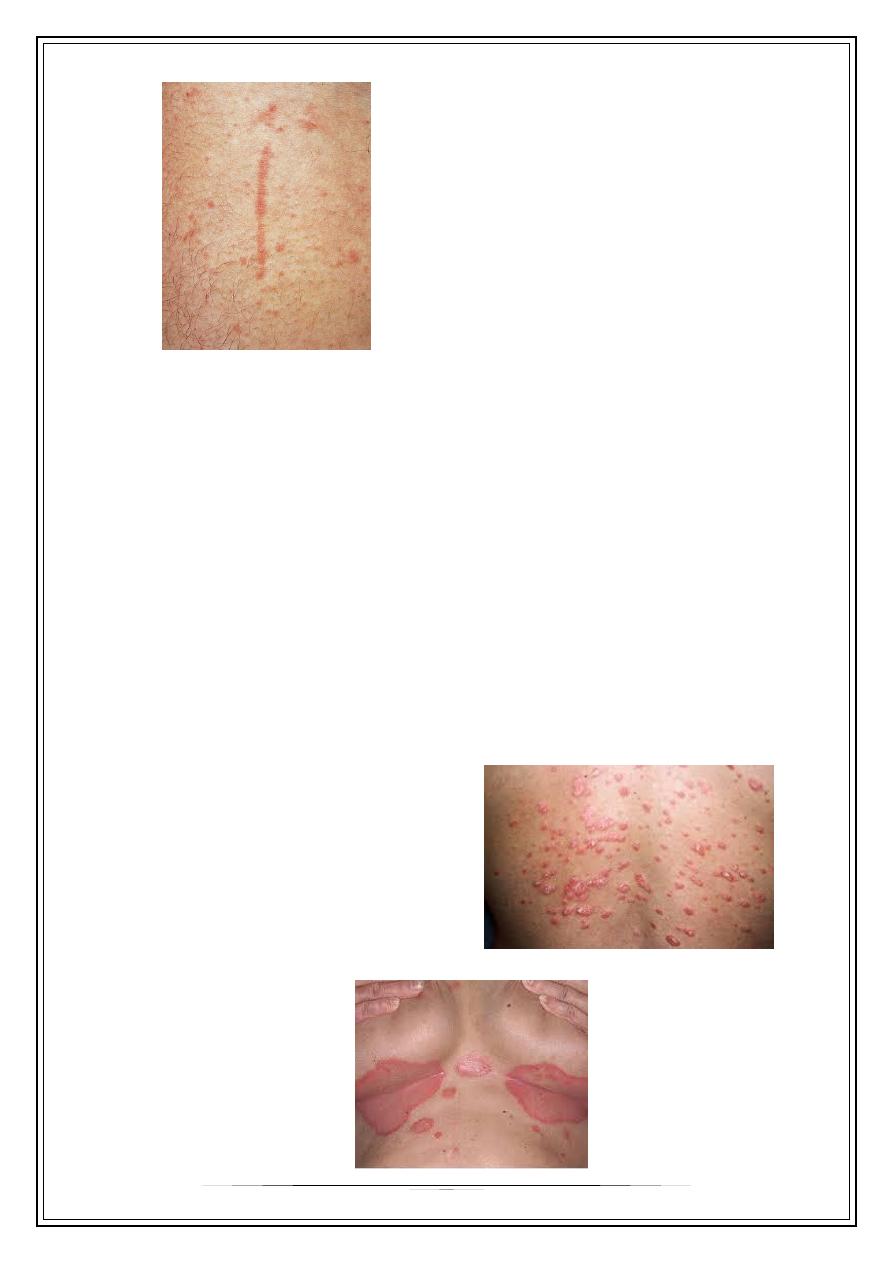
Guttate psoriasis
–
Numerous small lesions about 1cm
–
Usually less scaly
–
Trunk & proximal limbs
–
Usually patients less than 30
–
Often preceded by strept URTI.
Flexural psoriasis
–
In body folds
–
Less scaly
–
Often miss DX if no
other signs of psoriasis
5
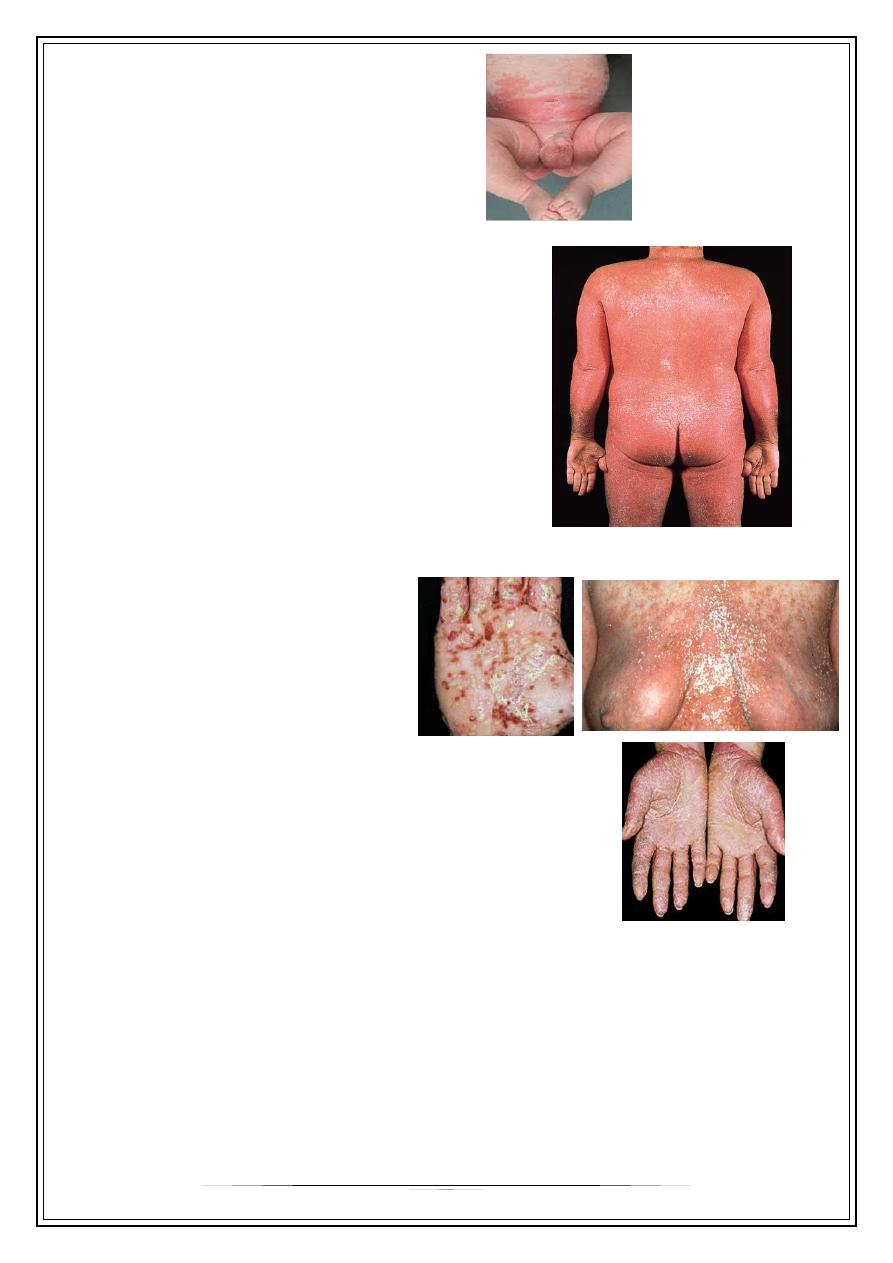
Napkin psoriasis
–
2-8 months old babies
–
disappear by topical treatment
–
Might reappear in adult life.
Erythrodermic psoriasis
–
Uncommon
–
More than 90% of skin surface
–
Can evolve from chronic or eruptive
–
Fever, hypo & hyperthermia, dehydration
–
Complications: Heart failure, infections,
malabsorption,& anaemia
Pustular psoriasis
–
Localized:
more common
On palms & soles
–
Generalized:
Associated with fever
Palmoplantar psoriasis
–
Can be hyperkeratotic or pustular
–
Difficult to distinguish from chronic eczema or tinea
May be aggravated by trauma
Nail changes in psoriasis
1) Distal onycholysis.
2) Random pitting from parakeratosis of proximal matrix.
3) Oil spots which are yellow areas of subungual parakeratosis
4) Salmon patches due to nail bed psoriasis.
5) Subungual hyperkeratosis resembling onychomycosis.

6
Psoriatic arthritis
–
in 5-10% of psoriatic
–
rare before age 20
–
rheumatoid factor negative arthritis
–
5 types either peripheral or central, often overlap
Treatment
–
Reassurance, explanation are vital
–
Psoriasis is not contagious
–
No cure, so the aim is to induce remission or making it more tolerable
–
Spontaneous remission in 50% of cases
–
Quit smoking
Calcipotriol
–
vitamin D agonist, only reduce thickness & scaling of the plaques
–
Irritant so combined with steroid to get a greater response, fewer S.E.,
+steroid sparing
Topical corticosteroids
–
Most commonly used
–
clean & effective
–
but frequent S.E.
1-as dermal atrophy
2-tachyphylaxis
3-early relapse
4- precipitation of pustular type
–
Indications of topical steroids:

7
1)On face, ears & flexures
2) Patients can’t tolerate tar, dithranol, etc, due to allergic or irritant
reaction
3)Unresponsive psoriasis of scalp, palm & sole
4) Patients with minor, localized type
5) In combination with other modalities
Light therapy
–
Most patients benefit from sunlight
–
UVR is the main treatment for moderate to severe psoriasis.
–
S.E. include sunburn & increased risk of skin CA
–
Artificial UVB by fluorescent bulbs, either narrow band(311nm.) or broad
band
–
Max. effect achieved at MED (min. dose to induce erythema in a test patch
after 24h)
PUVA
–
Psoralens are natural phtosensitizers
–
High intensity, long wave UVR( UVA), given 2 hours after ingestion of 8-
methoxy psoralen, twice weekly
–
20-25 sessions are needed, +maintenance doses
–
Clearance ‘ll occur in 75% of patients
–
Not for young patients
–
UVR resistant glasses worn for24 hours
Methotrexate
•
folic acid antagonist, inhibit DNA synthesis in S phase
•
Given orally or parentally , 7.5-15mg, once weekly
•
Minor S.E. nausea & malaise in 1
st
.24hr.
•
Serious S.E. are liver toxicity, marrow suppression, teratogenicity & male
oligospermia
•
Should monitor liver, renal & marrow function, before & during treatment
Neotigasone (=Acitretin)
–
Acitretin is vitamin A analougue
–
Especially effective in pustular psoriasis of palms& soles, also in plaque
psoriasis.
–
Frequent minor S.E. as dryness of skin & m.m., pruritis, hair fall, &
paronychia.

8
–
Serious S.E. are hyperlipidemia especially of triglycerides & teratogenicity
–
Can be combined with PUVA
Cyclosporine
–
Inhibits cell mediated immunity
–
Very effective in psoriasis
–
Serious S.E. as hypertension, renal damage, persistent viral warts & a risk of
skin cancer.
Biologics
–
Biologics: new, monoclonal antibodies to key pathological pathways in
psoriasis
–
Against T.N.F. α(alpha)
–
Against receptors involved in T-cell trafficking as interleukin 12/23(IL-12/IL-
23) blockade agents
–
Interleukin 17-A
–
Expensive, requires careful consideration of medical Hx, disease severity &
monitoring of infections
Thank You,,,
