
1
Pulmonary Hydatid Disease
By: NAZAR B. ELHASSANI
Introduction
The word hydatid is Hellenic in origin and means "a cyst full of water". Hydatid
disease exists all over the world and is a major health problem in the Middle East.
Epidemiology
Hydatid disease is a serious public health hazard and a major problem for the
community. It exists in most parts of the world and is hyperendemic in sheep raising
areas. There are focci in New Zealand, Australia, the Indian continent, the
Mediterranean basin, East Africa, Eastern Europe, Iceland and Latin America, but it is
most prevalent in the middle east. In Iraq, the disease is still endemic and is
considered to be one of the most serious helminthic disease in the country. Domestic
hygiene, the standard of living and human behavior play an important role in the
epidemiology of transmission to man.
Life cycle of the parasite
Hydatid disease is caused by the adult and larval stages of the Echinococcus
Granulosus. The adult is a cestode of 5-7 mm. in length with a scolex bearing four
suckers and with a body containing tow to six proglottids. The larval stage or meta-
cestode is a cyst with acellular laminated outer layer and an inner nucleated germinal
layer which gives rise to brood capsules and then scolices. The adult worm lives in
dog which is the primary host. The cystic part of the cycle occurs in sheep, horse, pig,
ox, camel or map, which act as intermediate hosts.
The adult worm lives in dog’s intestine for months. The terminal segment
proglottids detach from the worm and release thousands of ova with the stools. These
are ovoid in shape and can remain infective for long periods. Ingestion of the ova by
sheep in contaminated water, grass or vegetables causes infection , and hydatid cysts
subsequently develop in the viscera. The parasite gets back into the dog when the
sheep is slaughtered and it’s viscera containing hydatid cysts are eaten by another
dog. In each of these cysts thousands of scolices are found which will grow into new
tapeworms in the dog’s intestine and so the cycle repeats itself indefinitely.
If an ovum gets into a man instead of a sheep, the life cycle of the parasite will
broken because the entrails of men are not eaten by dogs. Contamination of food is a
common source of infection in man, more frequently he contaminates his fingers by
fondling a dog and then takes his food without washing his hands. The ova hatch in
the stomach and the hexacanth embryos or oncospheres are released in the stomach
and duodenum and pass through the wall and travel via the portal vein to the liver,
where the majority settle and develop into hydatid cysts. Only those embryos which
successfully pass through the capillaries in the liver to reach the lungs develop into
hydatid cysts, and the few which get through the lungs are then carried to the viscera
and tissues supplied by the systemic circulation. Sometimes the hatched embryo
passes through the wall of the stomach or duodenum into a lymphatic channel to be

2
carried into the lungs via the thoracic duct, thus by-passing the liver; this explains the
few cases of pulmonary hydatids without hepatic involvement.
Once implanted in the interstitial tissue of the lung, the embryo grows into a
vesicle and then into a hydatid cyst.
Pathology
The hydatid cyst in the lung is surrounded by a capsule formed of atelectatic
alveoli and fibrous tissue. This adventitia (pericyst) is part of the host and becomes
thicker and tougher with age, thus separating the cyst from the lung parenchyma; this
is of importance in the surgical excision pf the cysts.
The hydatid cyst itself is composed of a nucleated thin germinal layer (endocyst)
which secretes the hydatid fluid into its cavity and forms externally an acellular white
laminated membrane (ectocyst). The germinal layer is the only living part of the cyst.
The laminated membrane is completely separated from the adventitia. And this
explains the feasibility of surgical removal of intact hydatid cyst by enucleation.
The main bulk of the cyst is made up of its contained fluid which is highly
antigenic.
Brood capsules develop from the germinal layer by the process of asexual budding
and vacuolation and are attached by pedicles to the innermost wall of the germinal
layer. Within each brood capsule, tow to three scolices (head of future worms)
develop. The attachment of the brood capsule to the germinal layer becomes loose and
the capsule bursts, releasing the scolices into the fluid of the cyst. These fall to the
bottom by gravity and are sometimes referred to as "hydatid sands".
There is a tendency for the growing cyst to enlarge peripherally towards the
pleural space ( an important factor in considering the surgical approach to the cyst).
In this paper the term "simple" cyst indicates that the cyst is intact , and the term
"complicated" indicates that it has been injured, ruptured, or infected.
Rupture into the bronchial tree is common whilst rupture into the pleura is very
rare.
In partial rupture, the adventitia bursts, small bronchial fistulae appear and air may
enter the space between the adventitia and the laminated membrane which is still
intact. This appears as a crescent-shaped "perivesicular pneumocyst".
In complete rupture, the cyst itself ruptures and a small amount of fluid escapes
between the laminated membrane and the adventitia. If at the same time a little air
gets in through small bronchial fistulae, a fluid level will appear on either side of the
shrunken but dome-shaped hydatid. This is known as "double arc sign".
Complete rupture of the cyst may permit expulsion of its contents through large
bronchial fistulae and allow air to enter the cyst; the laminated membrane then
collapses and floats upon what remains of the fluid, producing irregular projections
above the level of the fluid. The appearance is likened to a "water- lily" floating on a
pond. One of tow complications may develop in this cavity with the retained
disintegrated membranes inside it
:
either some parts of the germinal layer survive
inspite of complete rupture and form "daughter cysts" in the space occupied by the
original cyst, or the parasite dies after complete rupture, and the retained disintegrated
fragments of the laminated membrane acts as a sequestrum and with the associated
bronchial fistulae lead to infection and the formation of a "lung abscess".
Occasionally all the membranes are coughed out leaving a "pulmonary cavity" and a

3
cured patient. Rarely, "calcification" may occur in the adventitia of complicated cyst
but this does not necessarily signify death of the parasite.
A "primary hydatid cyst" indicates that the cyst has developed from an ovum,
whilst a"secondary hydatid cyst" means that a primary cyst lodged in the lung or in
the liver has ruptured and caused new daughter cysts to develop. These daughter cysts
develop either from fragmentation of the germinal layer left behind after spontaneous
evacuation or inadequate surgical removal of the parasite, or from scolices in the
liquid which has been split during surgery or spontaneous rupture. This latter
possibility is questionable , since the elements inside a hydatid cyst should go on to
grow into tapeworms, however; Deve in 1945 proved that live hydatid elements could
revert to new hydatid cysts by the process of retrograde metamorphosis.
Clinical features
1. There is a high incidence of the disease in children who fondle dogs and in young
men who work with dogs on farms.
2. There is no significant difference in sex distribution.
3. The lesions may be asymptomatic unless, or until, some complications develop.
4. Many patient present to the thoracic surgeon with a circumscribed opacity found
incidentally on a routine CXR.
5. Patients with intact or mildly infected cysts may experience transient symptoms of
pain, cough, and hemoptysis.
6. The acute onset of rigor, fever, cough with purulent expectoration and pleuritic pain
is experienced by all patients with lung abscess.
7. Fragments of membranes or daughter cysts, described by patients as" grape skin",
may be coughed up when cysts have ruptured into the bronchial tree.
8. Severe dyspnea may occur in the rare event of rupture into the pleural cavity
causing hydro. or pyopneumothorax.
9. Rupture of a cyst may cause signs of anaphylaxis . this rare presentation is due to
the high antigenicity of the hydatid fluid.
Diagnosis
Ι. Radiographic findings
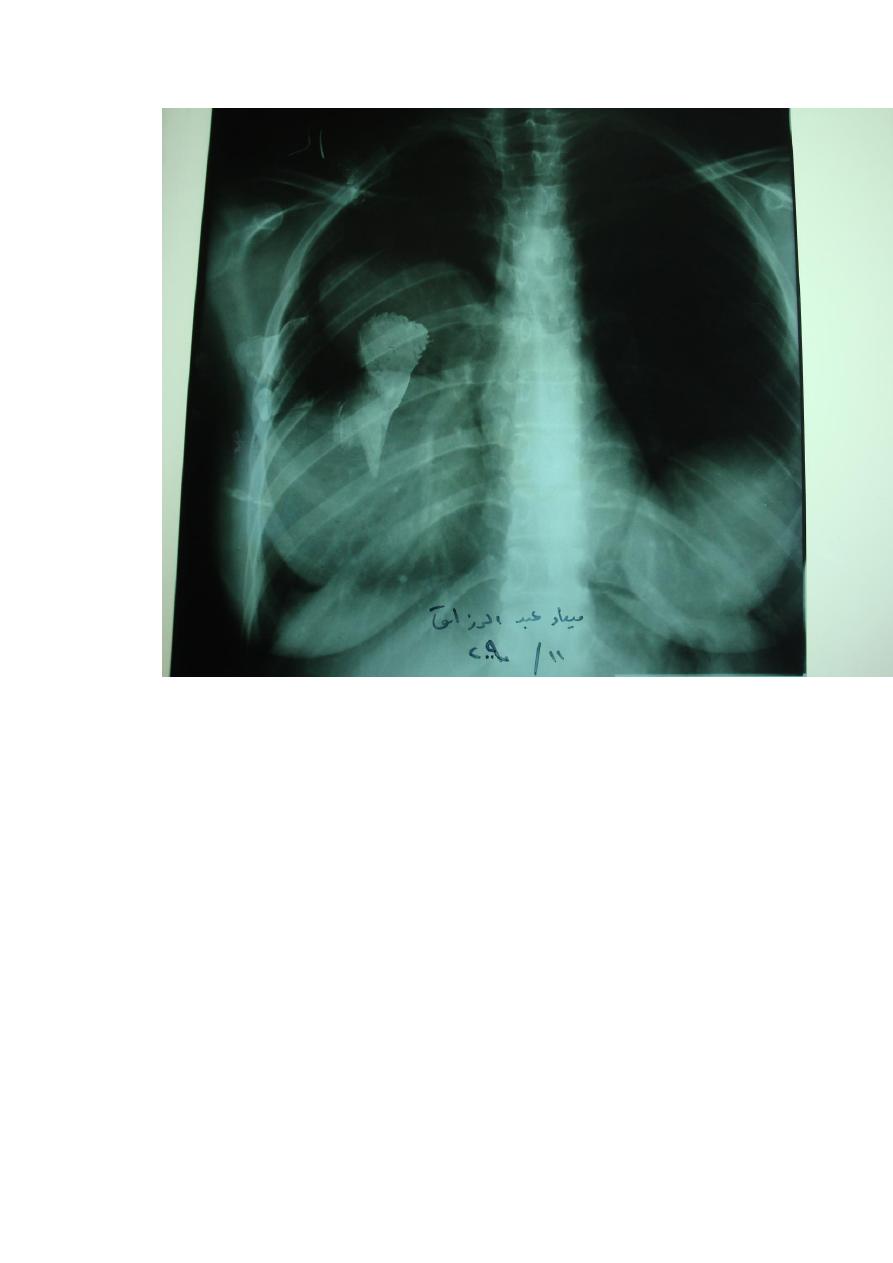
1. a well defined circular or oblonged shaped opacity of homogenous density is
diagnostic of a simple intact hydatid cyst.
2. a pathognomonic radiographic finding is a "perivesicular pneumocyst" due to
the presence of air between the adventitia and the laminated membrane . this
appears as a slender crescent "signet-ring" in cases of adventitial rupture.
3. the "double arc sign" appears as a cyst with a fluid level on either side of the
shrunken but dome-shaped hydatid.
4. the "water-lily" or "camalote sign" appears as a cyst with the collapsed
membrane floating in the fluid and is seen in cases of rupture of the cyst itself.
5. daughter cysts may produce radiographic appearances identical with the
primary cysts. A large daughter cyst with a partially or completely drained
pericyst produces the "rising sun sign".
6. if suppuration occurs, a huge abscess with conspicuous fluid level marking is
seen.
7. often, an empty cavity with remnants of collapsed membranes are seen.

4
8. rarely, all the membranes are coughed up and a "pulmonary cavity"
surrounded by a thin margin is seen.
9. in rare instances, the adventitia may calcify, and this gives the appearance on
X-ray of a thin shell of an egg.
10. hydropneumothorax may be seen, and this indicates rupture into the pleural
cavity.
11. bilateral multiple cysts is a common radiographic finding.
ΙΙ. Non invasive procedures
*Isotope liver scan
*Ultrasonic scanning
*CT scan
These procedures are of great value in demonstrating the exact site, size, and
the number of cysts, specially the liver.
ΙΙΙ. immunological tests
1. Casoni intradermal test: Absolute reliance can not be placed on a positive
Casoni reaction because it may be positive in an apparently unaffected individual
living in an endemic area , and it may remain positive long after the cyst have
been removed . this test have been abandoned in most centers because of its non-
specificity and difficulty in obtaining test fluid.
2. Weinberg complement fixation test
This is the best method of detecting infestation and is accurate.
3. Latex slide agglutination test
This is simple, reliable, and non specific.
4. Indirect haemagglutination test
This is relatively non specific
5. Immunoelectrophoresis
This demonstrates the specific band 5 of echinococcus granulosus.
ΙV. Blood test
Eosinophilia is common finding, but this is of little value since multiple parasitic
infestation are common in the middle east.
V. parasitological test
These are based on the finding of scolices, brood capsules, and daughter cyst in
the sputum or pleural aspirate.
Differential diagnosis
Radiological diagnosis of pulmonary hydatid disease is a problem when the
cyst is simple, small and single, or when multiple and bilateral. When distinction
must be made from other causes of solitary round peripheral lesions or from
metastases.
In Iraq, the finding of a solitary opacity of homogenous density and clear-cut
borders on a CXR will be a hydatid cyst in 90% of cases.
Hydatid cyst is a major cause of lung abscess in Iraq, but it must be differentiated
from other causes of lung abscess.
Surgical treatment

5
The treatment for hydatid cyst is surgical removal. The various surgical
techniques currently in use are:
A) removal of the cyst
the principles of removal of a hydatid cyst are evacuation of the contents of
the cyst, avoidance of spillage during the procedure, closure of the bronchial
fistulae, and prompt re-expansion of the lung.
1. aspiration\evacuation technique
The technique of aspirating the fluid with a fine needle followed by the
extraction of the cyst through a small adventitial incision was described by Barrett
in 1947. this procedure can be used for simple and complicated cysts. Aspiration
may result in some leakage, but this will not be dangerous if adequate
precautionary packing of the operative field has been carried out. The author has
used this technique in most patients for the last 20 years with good results.
2. enucleation
Enucleation in the plane between the adventitia and the laminated membrane
was first described by Ugon in 1947, suggested by Barrett in 1949, and advocated
by Barrett and Thomas in 1952. Technically this is a beautiful procedure , though
applicable only to simple cysts . although a plane of cleavage can readily be found
between the adventitia and the laminated membrane, there is appreciable risk of
accidental rupture during the dissection, if this does occur, the risk of
contamination is high, much greater than in aspiration\ evacuation technique
such a high risk is not acceptable to most thoracic surgeons.
3. excision
Excision of the cyst with its capsule was first described by Fontana in 1948,
suggested by Barrett and Thomas in 1952 and Xanthakis in 1972. This procedure
is applicable to all cases irrespective of whether the cyst is simple or complicated
and it offers the best chance of avoiding soiling. It appears sound, simple and
attractive, but the continuous oozing of blood and the persistent leakage of air
from the raw surface of the lung may render it unsuitable.
After removal of the cyst by whether method, the edges of the sac must be
trimmed and sutured, and a meticulous search must be made for all bronchial
openings which should be sutured individually. The residual sac is left open, and
there is no need to obliterate it.
Zafirokopoulas in 1969 reported the results of microscopic examination of
cysts from more than 300 patients , in 4%, live scolices and daughter cysts were
found in the layers of adventitia and the surrounding lung parenchyma, pulmonary
resection was suggested for these cases. A similar results was obtained by
Galloway and Rob in 1976. A follow up of the authors patients and of others
shows that recurrence following removal of the cyst is minimal.
B) Resection
Pulmonary resection is reserved for:
1) giant simple cyst that causes permanent and irreversible changes in the affected
part of the lung.
2) complicated cyst where infection has caused a lung abscess or bronchiectasis.
3) multiple daughter cysts involving one lobe.
4) calcified cysts.
5) patients presenting a diagnostic problem.

6
6) patients with massive hemoptysis, or recurrent suppuration following the
removal of a cyst , resection of the involved part of the lung is advisable.
Methods of resection are:
1. segmentectomy
This is the usual procedure. The aim being to preserve as much lung tissue as
possible.
2. lobectomy
This is the procedure of choice when resection is indicated.
3. pneumonectomy
This is rarely needed.
Notes
When the disease is bilateral, the side with a large simple cyst or with a
complicated cyst is operated on first, and after a few weeks the other side is
tackled.
In patients with lung and liver involvement, the priority is for the pulmonary
lesion.
Recent rupture into the bronchial tree should be treated conservatively by
treating the anaphylactic shock, postural drainage, administration of antibiotic,
and regular observation for signs of recurrence.
Rupture into the pleural cavity with hydropneumothorax requires
thoracotomy. The main objective is removal of the cyst , which is usually found
floating in the pleural cavity, and re-expansion of the lung, even in patients with
pyopneumothorax and daughter cyst formation in the pleura, the same treatment is
indicated.
Medical treatment
The medical treatment of hydatidosis is far from being established, no drugs
have yet been found that can effectively reach and destroy the parasite even if
drugs are capable of destroying the live elements of the cyst do become available,
the retained membranes will ultimately become infected and produce lung
abscess.
Mebendazole (vermox) and flouromebendazole are being benzimedazole
derivatives and may have a limited role in the treatment. They are safe drugs with
few side effects and may be used in dissiminated cases when the cysts are
multiple and inaccessible and when surgery is contraindicated for reasons of
extreme ill health. Mebendazole is prescribed in high dose 50 mg\kg\day in
divided doses for three months.
7
8
9
10
11
