
1
Poisoning
General approach to the poisoned patient
Taking a history in poisoning
• What toxin(s) have been taken and how much?
• What time were they taken and by what route?
• Has alcohol or any other substance (or substances, including drugs of
misuse) been taken as well?
• Obtain details from witnesses (e.g. family, friends, ambulance
personnel) of the circumstances of the overdose
• Assess immediate suicide risk in those with apparent self-harm (full
psychiatric evaluation when patient has recovered physically)
• Assess capacity to make decisions about accepting or refusing
treatment
• Establish past medical history, drug history and allergies, social and
family history
• Record all information carefully
Triage and resuscitation
• immediately assessing vital signs
• identifying the poison(s) involved and obtaining adequate information
about them

2
• identifying patients at risk of further attempts at self-harm and
removing any remaining hazards
Clinical assessment and investigations
Glasgow Coma Scale (GCS) and AVPU (alert/verbal/painful/
unresponsive) scale are used to assess conscious level
Vital signs
Systemic examination (neurological, cardiac, respiratory)
ECG and cardiac monitoring instituted in all patients with
cardiovascular features or where exposure to potentially
cardiotoxic substances is suspected.
Patients who may need antidotes should be weighed if possible
RBS, urea, electrolytes and creatinine
Arterial blood gases and calculation of anion and osmolar gaps
measurement of the amount of toxin in the blood
Psychiatric assessment
General management
Resuscitation (ABC measures)
Remove patient from poising area
Patients presenting with eye/skin contamination should undergo
local decontamination measures.
Supportive care
Treatment of complications
antidots

3
Gastrointestinal decontamination
Patients who have ingested potentially life-threatening quantities of
toxins may be considered for gastrointestinal decontamination if
poisoning has been recent
1. Activated charcoal
Given orally as a slurry, activated charcoal absorbs toxins in the
bowel as a result of its large surface area. It can prevent
absorption of an important proportion of the ingested dose of
toxin, but efficacy decreases with time and current guidelines do
not encourage use more than 1 hour after overdose, unless a
sustained-release preparation has been taken or when gastric
emptying may be delayed. Use is ineffective for some toxins like
iron, lithium, acids, alkalis, ethanol, Ethylene glycol, Mercury,
Methanol, Petroleum distillates . In patients with impaired
swallowing or a reduced level of consciousness, activated
charcoal, even via a nasogastric tube, carries a risk of aspiration
pneumonitis, which can be reduced (but not eliminated) by
protecting the airway with a cuffed endotracheal tube. A laxative
is generally given with the charcoal to reduce the risk of
constipation or intestinal obstruction .
2. Gastric aspiration and lavage
Gastric aspiration and/or lavage is very infrequently indicated in
acute poisoning, as it is no more effective than activated charcoal

4
for most substances and complications are common, especially
pulmonary aspiration. It is contraindicated if strong acids, alkalis
or petroleum distillates have been ingested. Use may be justified
for life-threatening overdoses of those substances that are not
absorbed by activated charcoal
3. Whole bowel irrigation
This involves the administration of large quantities of osmotically
balanced polyethylene glycol and electrolyte solution (1–2 L/ hr for an
adult), usually by a nasogastric tube, until the rectal effluent is clear. It
is occasionally indicated to enhance the elimination of ingested packets
of illicit drugs or slow-release tablets such as iron and lithium that are
not absorbed by activated charcoal. Contraindications include
inadequate airway protection, haemodynamic instability,
gastrointestinal haemorrhage, obstruction or ileus. Whole bowel
irrigation may precipitate nausea and vomiting, abdominal pain and
electrolyte disturbances.
Urinary alkalinisation
If the urine is alkalinised (pH > 7.5) by the administration of sodium
bicarbonate (e.g. 1.5 L of 1.26% sodium bicarbonate over 2 hrs)
resulting in enhanced urinary excretion of salicylates and methotrexate.
Urinary alkalinisation is currently recommended for patients with
clinically significant salicylate poisoning when the criteria for
haemodialysis are not met . It is also sometimes used for poisoning with
methotrexate. Complications include alkalaemia, hypokalaemia,
occasionally alkalotic tetany and hypocalcaemia may occur but is rare.

5
Haemodialysis and haemoperfusion
These techniques can enhance the elimination of poisons that have a
small volume of distribution and a long half-life after overdose; use is
appropriate when poisoning is sufficiently severe. The toxin must be
small enough to cross the dialysis membrane (haemodialysis) or must
bind to activated charcoal (haemoperfusion) . Haemodialysis can also
correct acid–base and metabolic disturbances associated with
poisoning .
Lipid emulsion therapy
Lipid emulsion therapy is increasingly used for poisoning with lipid-
soluble agents, such as local anaesthetics, tricyclic antidepressants,
calcium channel blockers and lipid-soluble β-adrenoceptor antagonists
(β-blockers) such as propranolol. It involves intravenous infusion of 20%
lipid emulsion (e.g. Intralipid).
6
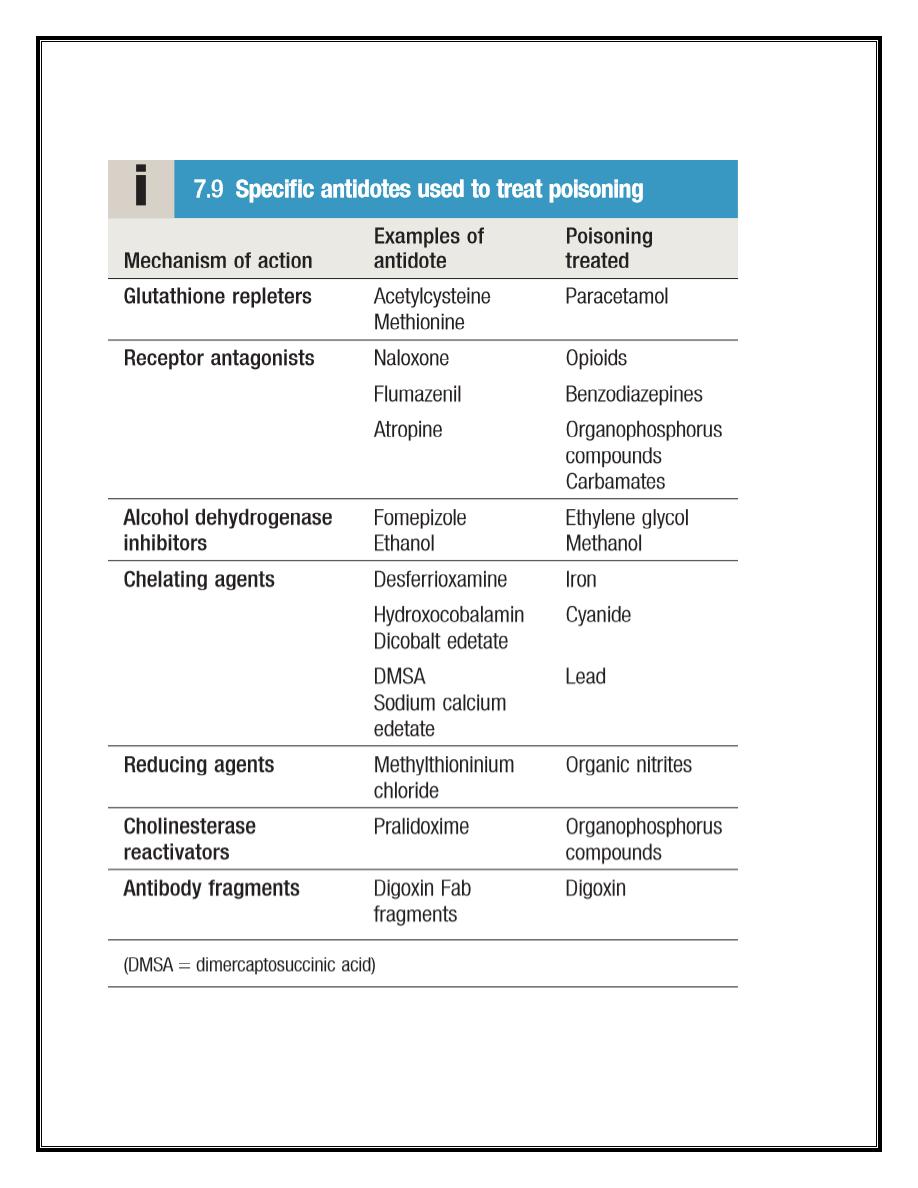
Antidotes
