• Seizures in Childhood
Prof .razzaq alrubaee
thiqar collee of medicine 2020Seizures in Childhood
Seizure (convulsion): is a paroxysmal, time-limited change in motor activity and/or behavior that results from abnormal electrical activity in the brain.It is either focal or generalized.
Focal seizures may be characterized by motor or sensory symptoms such as paresthesia or pain localized to a specific area.
Epilepsy : is a recurrent seizures . It is either idiopathic or secondary to underlying disorders.
CLASSIFICATION OF SEIZURES
• Partial seizures:• Simple partial (consciousness retained)
Motor
Sensory
Autonomic
Psychic
• Complex partial (consciousness impaired)
Simple partial, followed by impaired consciousness
• Partial seizures with secondary generalization
• 2- Generalized seizures:
Absences• Typical(petit mal)
• Atypical
Generalized tonic-clonic
Tonic (increased tone or rigidity)
Clonic (rhythmic muscle contraction & relaxation)
Myoclonic (shock like contraction of groups of muscles)
Atonic (flaccidity or lack of movement during convulsion)
Infantile spasms
Unclassified seizures
Typical absence (petit mal) seizures
It is characterized by a sudden cessation of motor activity or speech with a blank facial expression and flickering of the eyelids.It is uncommon before age 5 yr & more prevalent in girls.
Never associated with an aura.
Persist for 30 sec.& can occurs several times per day.
Not associated with a postictal state & patient return to normal activity immediately after seizure.
This seizure precipitate by hyperventilation or any stress conditions.
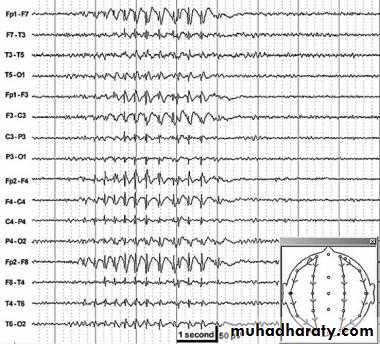
• The EEG shows a typical 3/sec spike and generalized wave discharge.
• The drug of choice is ethosuximide or valproic acid .Generalized Tonic-Clonic seizure:
It may be associated with an aura.Patients suddenly lose consciousness, their eyes roll back, tonic contractions of body musculature, with cyanosis & apnea.
This followed by rhythmic clonic contractions alternating with relaxation of all muscle groups . During the seizure, children may bite their tongue with loss of sphincter control. This attack persists for a few minutes.
Poetically child pass in a deep sleep for 30min-2hr.
The cause mostly Idiopathic
It means the cause of a generalized seizure cannot be identify.
Infantile spasms (West syndrome)
It is begin between the ages of 4 and 8 mon.Etiology
Infantile spasms are classified into two groups:1-cryptogenic(primary) :
The child has an uneventful pregnancy and birth history with normal developmental milestones before the onset of seizures.
Brain CT and MRI scans are normal. 10-20% of infantile spasms are cryptogenic.
2-Symptomatic (secondary):
Are related directly to several prenatal, perinatal, and postnatal factors
Prenatal and perinatal factors include:
- hypoxic-ischemic encephalopathy
-congenital infections
-inborn errors of metabolism
-neurocutaneous syndromes such as tuberous sclerosis
-congenital malformation of the brain
-prematurity.
Postnatal conditions include:
- CNS infections- head trauma (especially subdural hematoma)
- intraventricular hemorrhage
Clinical manifestations:
It is characterized by brief symmetric contractions of the neck, trunk, and extremities.There are three types of infantile spasms:
1-Flexor: occur in clusters and consist of sudden flexion of the neck, arms, and legs onto the trunk.
2-Extensor : extension of the trunk and extremities and are the least common form of infantile spasm.
3-Mixed : consisting of flexion in some clusters and extension in others, is the most common type of infantile spasm.
These clusters persist for minutes & can occurs during sleep or immediately on awakening from the sleep .
Investigations:
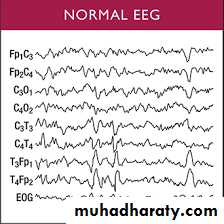
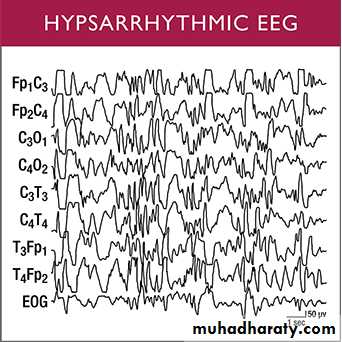
EEG showing the characteristic finding called hypsarrhythmia, which consists of a high-voltage,bilaterally asynchronous, slow-wave spikes.Treatment :
The preferred drug is Adrenocorticotropic hormone (ACTH)(synacthin)®, initial dose 20 unit/day i.m injection for 2wk., if no response the dosage is increased to 40 unit /day for additional 4wk.Ulternative drugs: oral prednisone 2mg/kg/day, Vigabatrin & clonazepam .
Prognosis :
infants with cryptogenic type have a good prognosis, where as those with symptomatic type have 80-90% risk of mental retardation.Guide line in the Treatment of seizures as a general
1-Treatment of the underlying causes if present.2-Investigation : CBC, serum electrolytes ,CSF,EEG,CT,MRI.
3-Drug therapy :
In a previously healthy child with the 1st afebrile convulsion, negative family history, normal physical examination and EEG, NO need for long term anticonvulsant therapy.
While those with recurrent seizures or neurologic dysfunction, anticonvulsant therapy should be maintained.
Important points on anticonvulsant drugs :
A-Selection of drug depend on the type of seizure & the age of the child (Valproic acid not used under 3mo.).B-Should not use polytherapy only in rare cases with intractable seizure unresponsive to single drug, because risk of toxicity & drug interaction.
C-for how long use drug?
For 2yr, then if no fit, stop drug with gradual withdrawal because abrupt withdrawal may cause recurrent seizure or status epilepticus , then can use other drug .• Anticonvulsant drugs :
Side effects
phenytoin include Hirsutism, gum hypertrophy, ataxia, skin rash, Stevens-Johnson sydrome
Phenobarbital are Hyperactivity, irritability, Stevens-Johnson syndrome
phenytoin
phenobarbital(luminal)• Use for Generalized tonic-clonic
Carbamazepine(Tegretol)
Use for partial seizures
Side effects : Nausea, vomiting, , weight gain, alopecia, hepatotoxicity.
Valproic acid(Depakine)Used for generalized seizure, partial ,absence , myoclonic.
Clonazepam(Rivotril)
• Used for absence, myoclonic
• & Partial seizures.
• Used for absence petimal seizure
Ethosuximide
3-Ketogenic diet:
This treatment considered forthe management of intractable seizures.
This diet contain restricted amount of carbohydrate & protein, with large amount of fat.
4- Surgery: considered for children
with intractable seizures unresponsive
to multiple anticonvulsants.
This surgery done for epileptogenic area which localized by EEG &
neuroimages .
For most children with epilepsy, restriction of physical activity is unnecessary except bathing and swimming which need supervision.
STATUS EPILEPTICUS
STATUS EPILEPTICUS
Is defined as continuous seizure activity or recurrent seizure activity without regaining of consciousness lasting for > 5 min.Refractory S.E. that has failed to respond to therapy, usually with at least 2 medications.
Causes include:
new-onset epilepsy of any type,
drug withdrawal in patients on antiepileptics,
drug intoxication,
hypoglycemia, electrolyte imbalance (hypocalcemia, hyponatremia,hypomagnesemia), acute head trauma,
encephalitis, meningitis, postinfectious encephalitis
ischemic stroke,
intracranial hemorrhage,
inborn errors of metabolism,
brain tumors, or any other disorder that can cause
an ordinary epilepsy.
Investigations
Laboratory studies include: serum glucose, sodium, calcium, or other electrolytes, blood and spinal fluid cultures, toxic screens, and tests for inborn errors of metabolism. Antiepileptic drug levels need to be determined if the patient is already on an antiepileptic.
EEG is helpful in identifying the type of S.E
Neuroimaging needs to be considered after the child has been stabilized.
Treatment
A medical emergency that isbetter managed in the ICU
because it requires initial
attention to securing
Airway , Breathing and Circulation with continuous monitoring of vital signs (including ECG)
Antiepileptic drugs are usually given parenterally in following sequential steps:-
• BenzodiazepinesDiazepam IV 0.3 mg/kg .
If intravenous access is not available ; use intranasal lorazepam, rectal diazepam, or IM /intra nasal /buccal Midazolam.
• Phenytoin (or fosphenytoin)
IV loading dose 15-20 mg/kg . A level is usually taken 2 hr later to ensure achievement of therapeutic concentration & accordingly the maintenance dose 5 mg/24 hr can be started either soon or after 6 hr.4.Valproate IV loading 25 mg/kg , maintenance 30-60 mg/kg/24 hr.
5. inhalational anesthetics For Refractory
• IV bolus of midazolam, propofol, Occasionally, inhalational anesthetics (especially isoflorane) are useful.
3. Phenobarbital IV loading dose 15-20 mg/kg , the dose can be repeated if there is no adequate response, then 5 mg/24 hr as maintenance.
Q1.Characteristics of simple partial seizures include all of the following except:
• Loss of consciousness• Versive seizures
• Duration of 10-20 sec
• No postictal state
• Abnormal EEG findings
• Q2:how can manage pt. with S.E.?