Lecture-1(4th year)
Assist. Prof. Dr. Hussein NajiHaemopoesis (Blood cells formation)
Blood : Suspension of differentiated mature non-dividing cells, (RBC,WBC and platelets), synthesis in the bone marrow and released to the peripheral blood.Objectives: To Know:
1. Sites of haemopoesis throughout life
2. Structure of the bone marrow
3. Significance of haemopoietic stem cell
4. Control of haemopoesis
5. Assessment of haemopoesis
Introduction and definition
Haemopoesis: Process of blood cells formation in the bone marrow by differentiation, proliferation, maturation and release of mature cells, in its three different types; erythropoiesis, leukopoiesis, and thrombopoiesis .Sites of haemopoiesis:
Hemopoiesis development divided in to two periods; intrauterine and extra-uterine period .
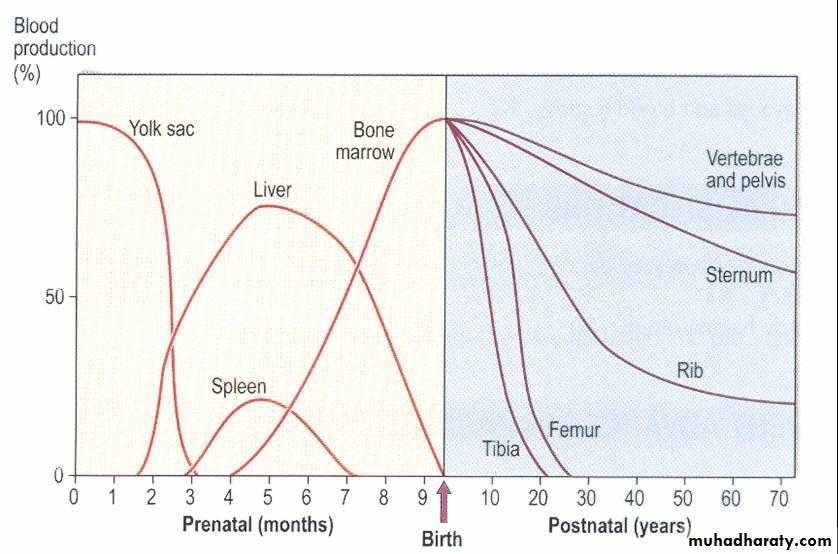
1. Fetal hemopoiesis divided into three periods :
Prenatal; Fetus:(intrauterine) : 0—2month (Yolk sac)
2—7months (liver & spleen)
5—9 months (bone marrow)
Postnatal; Extra uterine:
a. Fetus : Bone marrow in Whole bony skeleton (axial and peripheral long bones)
b. Adult and elderly: Vertebrae, ribs, sternum, skull, pelvic bones and proximal ends of long bones
Note: Normal bone marrow can expand 6—8 time its normal capacity to compensate blood cells loss( acute anaemia) with normal nutrients and environment until deficiency appear. Extra medullary hemopoiesis : hemopoiesis confined to sites out of normal red bone marrow mostly in the embryonic primitive sites of hemopoiesis( liver and spleen). Occur chronic hemolytic anaemia with failure of the normal red marrow to compensate the blood loss. It cause increase size of these organs (hepato—splenomegaly).
Anatomy (structure) of bone marrow
The bone marrow consist two parts , red marrow (parenchyma tissue) and stoma tissue with extracellular matrix.1. red bone marrow: ; consist of four main (parenchymal)cells types:
A. Stem cells.B. cells of Erythropoiesis series (Stem cells—CFUE—Proeythroblase—Erythroblast ( early, intermediate and late erythroblast) – reticulocytes).
C. Cells of myeloid series ( stem cell –CFUM—Blast—promyelocytes—myelocytes— metamyelocytes—band cells and mature granulocytes.
D. Cells Megakaryocytes : precursor of platelets
2. Stromal supportive tissue (They form the environment for haemopoesis):
a. bone trabecular forming the architecture of bone marrow,
b. network of microcirculation,
c. supportive cells: macrophages, fatty cells, dendritic cells, and fibroblast
Haemopoietic stem cells:
The specific property of stem cells : Has Two types of mitotic division:A. Symmetrical division to restore stem cell quantity, (Ability to give rise to new stem cells (Self Renewal)
B. Asymmetrical division: Ability to differentiate (Committed) into any blood cells lines precursor
Control (regulation ) of hemopoiesis
1. Normal physiological requirements.
2. Stimulated by different Cytokines and interleukins .
3. Nutrients support : minerals (IRON) , vitamins (B12, folic acid, ), Amino acids.
4. Hormones : Erythropoietin, thrombopoitein, Androgen, thyroid hormones.
5. Growth factors: Colony growth factors: Stem cell-GF, GM-GF, Monocytes GF.
6. Normal bone marrow environment and supportive tissue .
1. Erythropoietin : Hormone produced by the kidney :
a. Control erythroid proliferation and differentiationb. Absence results in Anemia of renal failure
c. Its secretion controlled by tissue hypoxia which is secondary to anaemia
2. Hemoglobin lever increase with increase thyroid hormone level and Androgen.
3. Macrophages Has different functions:
a. storage Iron in the bone marrowb. Denaturation of the aged red cells
c. Release of cytokines and control hemopoiesis
d. Defense mechanism.
Assessment of Hemopoiesis:
1. Htc and Hb (PCV, hemoglobin),2, CBC: erythrocytes count, leukocytes count, platelets count
3. Blood film ( for cells morphology)
4. Reticulocytes count
5. Bone marrow aspirate
Erythrocytes: Immature red cells, still have small amounts of RNA on their cytoplasm, so appear retic like on methylene blue stain . Named polychromatophilic cells on blood film stain, Slightly larger than mature RBC , loss the RNA with 24—48 h0urs and become mature red cell
Erythropoiesis
Mature red blood cells develop from erythroblast in the bone marrow. The development involves four mitotic divisions so that each precursor cell give rise to 16 mature red cells.The young red cell called reticulocyte, non-nucleated red cells with residual amount of RNA in cytoplasm. They take 24—48 hours in the bone marrow and 24—48 hours in the peripheral circulation to mature and count ( <2% ) from total red blood cells.
Classification of anaemia
1. Functional classification:a. infective hematopoiesis.
b. bone marrow failure
c. blood loss
d. Nutritional deficiency anaemia
e. Abnormal peripheral distribution.
2. The most Important scientific classification in use based on :
a. Blood cell indices (MCV, MCH, MCHC)
b. Staining appearance of red cells (Chromia) and ( red cells morphology).
Red cells indices
1. MCV (mean corpuscular volume):The average volume of RBC ( 80—10 fl) which classify anemia on cell size into microcytic<80, normocytic 80—100, and macrocytic >100fl
MCV= Htc (PCV)/ Red cells count = NV: (80—100 fl)
2. MCH (mean corpuscular hemoglobin):
The average content of Hb in RBC.
MCH= Hb/ total Red cell count : NR: 27-32 pg
3. MCHC (mean corpuscular hemoglobin concentration):
Express the average concentration of hemoglobin per unit volume of RBC.
MCHC= Hb/Htc (PCV) = NR: 32-36%
It defined as the ratio of the weight of hemoglobin to volume of RBC .
Classification of anaemia:
1. Hypochromic microcytic2. Normochromic macrocytic
3. normochromic macrocytic
Normochromic (1/3 central pallor)
Macrocytic (MCV>100fl)
Normochromic 1/3 central pallor) Normocytic (MCV 80—10fl)
Hypochromic (≥2/3 central pallor) microcytic (MCV <80fl)
1. Megaloblastic anaemia secondary to B12/or folate deficiency
2. Non-Megaloblastic macrocytic anaemia (many causes)
1. Anaemia of blood loss
2. Acquired hemolytic anaemia
3. Anaemia of chronic disorders in early stage
1. Iron deficiency anaemia
2. Thalassemia
3. Anaemia of chronic disorders in late stage
4. Lead poisoning
5. Some sideroblastic anaemia
Good luck