Babylon University Stage Fourth
College of Medicine Lecture 1Dr. Athraa Falah
THE HEPATIC PATHOLOGY
Jaundice and cholestasisAlterations of bile formation become clinically evident as yellow discoloration of the skin and sclera (jaundice and icterus, respectively) due to retention of bilirubin, and as cholestasis, characterized by systemic retention of not only bilirubin but also other solutes eliminated in bile.
Pathophysiology of Jaundice
There are two important pathophysiologic differences between the two forms of bilirubin. Unconjugated bilirubin is virtually insoluble in water at physiologic pH and exists in tight complexes with serum albumin. This form cannot be excreted in the urine even when blood levels are high.
Normally, a very small amount of unconjugated bilirubin is present as an albumin-free anion in plasma. This fraction of unbound bilirubin may diffuse into tissues, particularly the brain in infants, and produce toxic injury which may cause severe neurologic damage, referred to as kernicterus.
In contrast, conjugated bilirubin is water-soluble, nontoxic, and only loosely bound to albumin, and can be excreted in urine.
Serum bilirubin levels in the normal adult vary between 0.3 and 1.2 mg/dL, Jaundice becomes evident when the serum bilirubin levels rise above 2.5 mg/dL;
Jaundice occurs when the equilibrium between bilirubin production and clearance is disturbed by one or more of the following mechanisms :
(1) excessive extrahepatic production of bilirubin ex: Hemolytic anemias, thalassemia
(2) reduced hepatocyte uptake;ex: Some cases of Gilbert syndrome and some drugs
(3) impaired bilirubin conjugation; ex; Physiologic jaundice of the newborn, Breast milk jaundice , Gilbert syndrome, Diffuse hepatocellular disease (e.g., viral or drug-induced hepatitis, cirrhosis)
(4) decreased hepatocellular excretion; ex: Deficiency of canalicular membrane transporters (Dubin-Johnson syndrome, Rotor syndrome)
(5) impaired bile flow.
The first three mechanisms produce unconjugated hyperbilirubinemia, and the latter two produce predominantly conjugated hyperbilirubinemia.
Neonatal Jaundice.
Because the hepatic machinery for conjugating and excreting bilirubin does not fully mature until about 2 weeks of age, almost every newborn develops transient and mild unconjugated hyperbilirubinemia, termed neonatal jaundice or physiologic jaundice of the newborn. This may be exacerbated by breastfeeding, as a result of the presence of bilirubin-deconjugating enzymes in breast milk
Hereditary Hyperbilirubinemias.
Multiple genetic mutations can cause hereditary hyperbilirubinemia(Tablebelow).
TABLE 18-3 -- Hereditary Hyperbilirubinemias
Disorder
Inheritance
Defects in Bilirubin Metabolism
Liver Pathology
Clinical Course
UNCONJUGATED HYPERBILIRUBINEMIA
Crigler-Najjar syndrome type I
Autosomal recessive
Absent UGT1A1 activity
None
Fatal in neonatal period
Crigler-Najjar syndrome type II
Autosomal dominant with variable penetrance
Decreased UGT1A1 activity
None
Generally mild, occasional kernicterus
Gilbert syndrome
Autosomal recessive
Decreased UGT1A1 activity
None
Innocuous
CONJUGATED HYPERBILIRUBINEMIA
Dubin-Johnson syndrome
Autosomal recessive
Impaired biliary excretion of bilirubin glucuronides due to mutation in canalicular multidrug resistance protein 2 (MRP2)
Pigmented cytopasmic globules; ?epinephrine metabolites
Innocuous
Rotor syndrome
Autosomal recessive
Decreased hepatic uptake and storage?
Decreased biliary excretion?
NoneInnocuous
Gilbert syndrome is a relatively common, benign, inherited condition presenting with mild, fluctuating hyperbilirubinemia, in the absence of hemolysis or liver disease. It affects 3% to 10% of the U.S. population. The mild hyperbilirubinemia may go undiscovered for years. When detected in adolescence or adult life it is typically in association with stress, such as an intercurrent illness, strenuous exercise, or fasting. Individuals who have Gilbert syndrome may be more susceptible to adverse effects of drugs that are metabolized by UGT1A1.
Cholestasis
It is a pathologic condition of impaired bile formation and bile flow, leading to accumulation of bile pigment in the hepatic parenchyma. It can be caused by:
-extrahepatic or intrahepatic obstruction of bile channels, or by
-defects in hepatocyte bile secretion.
Patients may have jaundice, pruritus, skin xanthomas (focal accumulation of cholesterol), or symptoms related to intestinal malabsorption, including nutritional deficiencies of the fat-soluble vitamins A, D, or K.
-A characteristic laboratory finding is elevated serum alkaline phosphatase and γ-glutamyl transpeptidase (GGT) enzymes.
Extrahepatic biliary obstruction is frequently amenable to surgical alleviation. In contrast, intrahepatic cholestasis is not benefited by surgery (short of transplantation), and the patient's condition may be worsened by an operative procedure.
Infectious Disorders of liver
VIRAL HEPATITIS
Unless otherwise specified, the term viral hepatitis is applied for hepatic infections caused by a group of viruses known as hepatotropic virus (hepatitis viruses A, B, C, D, and E) that have a particular affinity for the liver.TABLE -- The Hepatitis Viruses
Virus
Hepatitis A
Hepatitis B
Hepatitis C
Hepatitis D
Hepatitis E
Type of virus
SsRNA
partially dsDNA
ssRNA
Circular defective ssRNA
SsRNA
Viral family
Hepatovirus; related to picornavirus
Hepadnavirus
Flaviridae
Subviral particle in Deltaviridae family
Calicivirus
Route of transmission
Fecal-oral (contaminated food or water)
Parenteral, sexual contract, perinatal
Parenteral; intranasal cocaine use is a risk factor
Parenteral
Fecal-oral
Mean incubation period
2–4 weeks
1–4 months
7–8 weeks
Same as HBV
4–5 weeks
Frequency of chronic liver disease
Never
10%
∼80%
5% (coinfection); ≤70% for superinfection
Never
Diagnosis
Detection of serum IgM antibodies
Detection of HBsAg or antibody to HBcAg
PCR for HCV RNA; 3rd-generation ELISA for antibody detection
Detection of IgM and IgG antibodies; HDV RNA serum; HDAg in liver
PCR for HEV RNA; detection of serum IgM and IgG antibodies
Hepatitis A Virus
Hepatitis A virus (HAV) is a benign, self-limited disease with an incubation period of 2 to 4 weeks. HAV does not cause chronic hepatitis or a carrier state and only rarely causes fulminant hepatitis, so the fatality rate associated with HAV is about 0.1%.
HAV is endemic in countries with substandard hygiene and sanitation, where populations may have detectable antibodies to HAV by the age of 10 years. Clinical disease tends to be mild or asymptomatic, and is rare after childhood. Affected individuals have nonspecific symptoms such as fatigue and loss of appetite, and often develop jaundice.
Laboratory findings
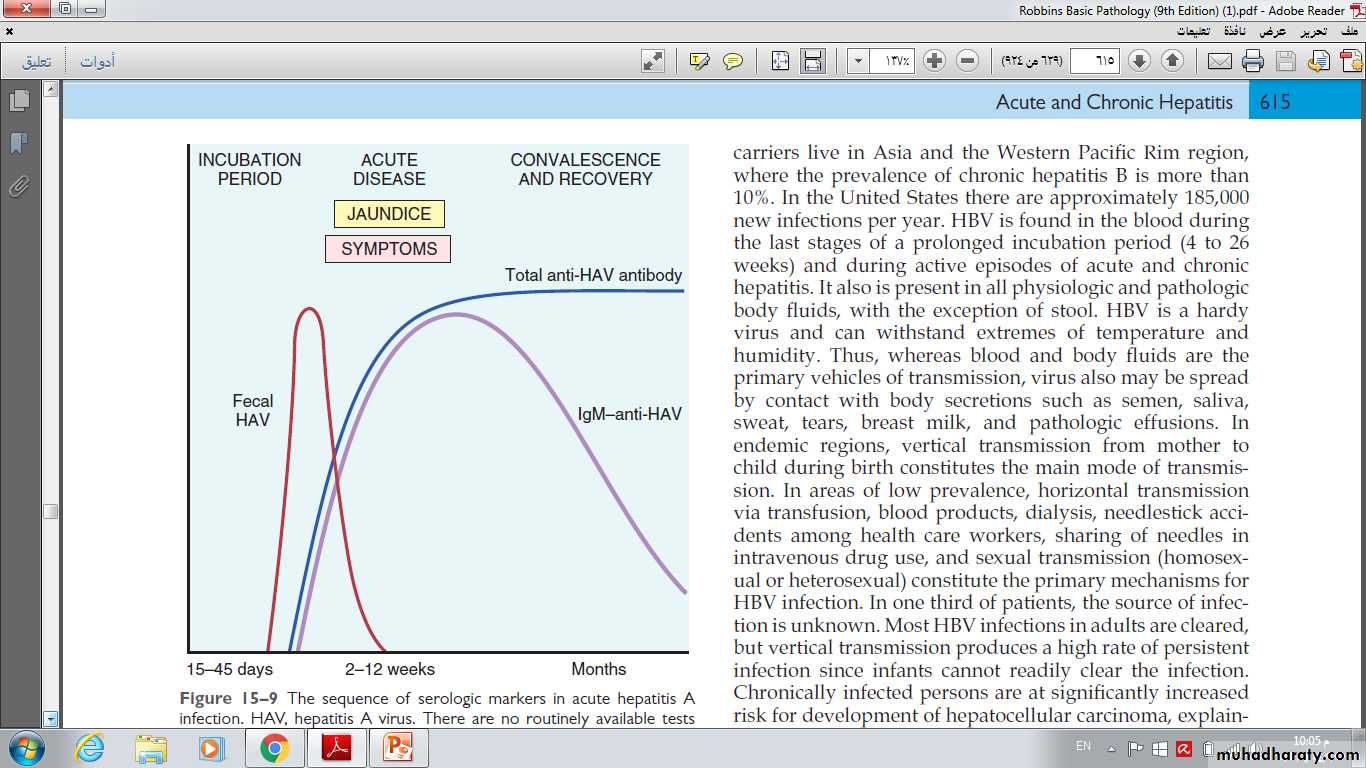
-Specific IgM antibody against HAV appears in blood at the onset of symptoms, constituting a reliable marker of acute infection ( Fig. below ).
-Fecal shedding of the virus ends as the IgM titer rises.
-The IgM response usually begins to decline in a few months and is followed by the appearance of IgG anti-HAV. The latter persists for years, perhaps conferring lifelong immunity against reinfection by all strains of HAV.
-However, there are no routinely available tests for IgG anti-HAV. The presence of this antibody is inferred from the difference between total and IgM anti-HAV.
The sequence of serologic markers in acute hepatitis A infection
Hepatitis B Virus (HBV)The clinical outcomes of HBV infection are:
(1) acute hepatitis with recovery and clearance of the virus,
(2) non-progressive chronic hepatitis,
(3) progressive chronic disease ending in cirrhosis,
(4) fulminant hepatitis with massive liver necrosis, and
(5) an asymptomatic carrier state.
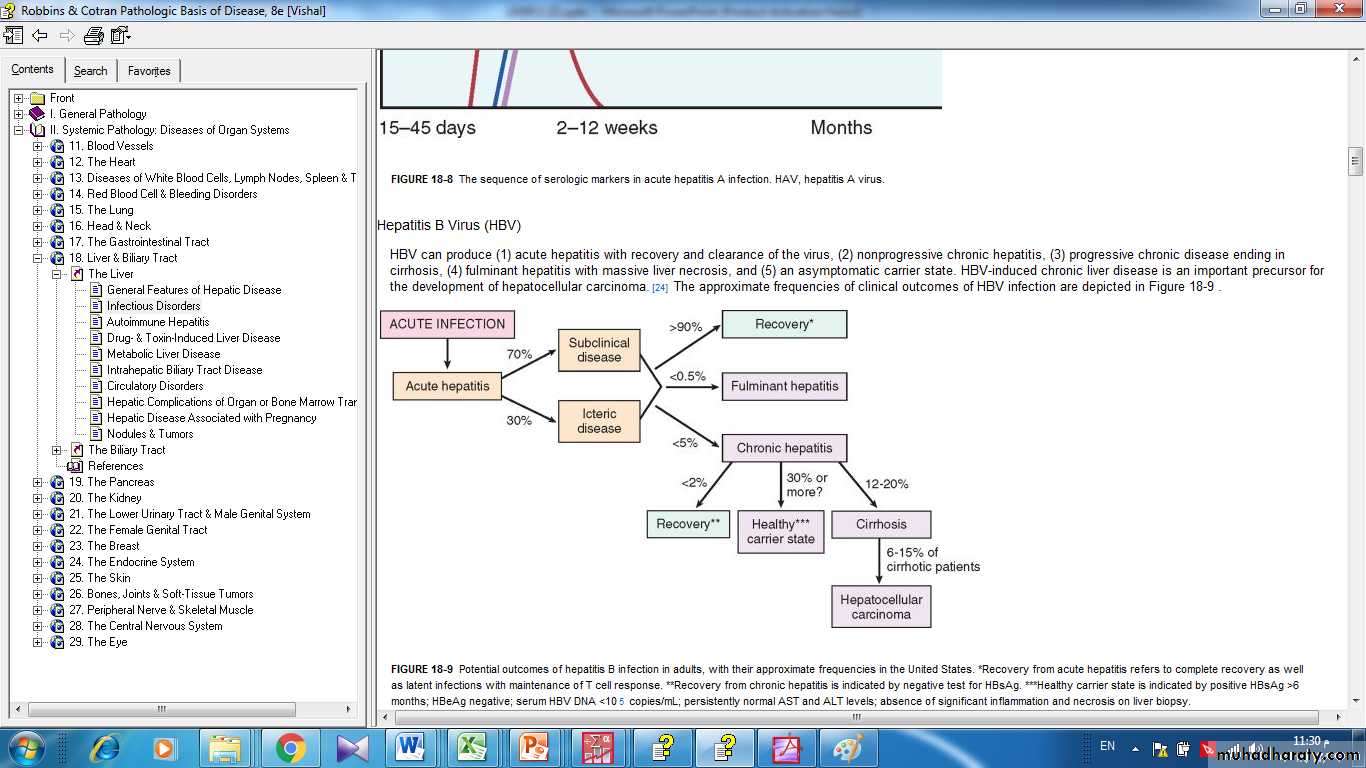
HBV-induced chronic liver disease is an important precursor for the development of hepatocellular carcinoma. The clinical outcomes of HBV infection are show in Figure below .
The potential outcomes with hepatitis B infection in adults
One third of the world population (2 billion people) have been infected with HBV, and 400 million people have chronic infection. The carrier rate is largely dictated by the age at infection, being the highest when infection occurs in children perinatally and the lowest when adults are infected.The mode of transmission of HBV occurs in different ways:
-perinatal transmission during childbirth .
-horizontal transmission (through minor cuts and breaks in the skin or mucous membranes among children with close bodily contact),
-unprotected heterosexual or homosexual intercourse and intravenous drug abuse (sharing of needles and syringes) .
The incidence of transfusion-related spread has decreased greatly in recent years due to screening of donated blood.
Approximately 70% have mild or no symptoms and do not develop jaundice. The remaining 30% have nonspecific constitutional symptoms such as anorexia, fever, jaundice, and upper right quadrant pain. In almost all cases the infection is self-limited and resolves without treatment. Chronic disease rarely occurs in adults in non-endemic areas. Fulminant hepatitis is also rare.
Laboratory findings
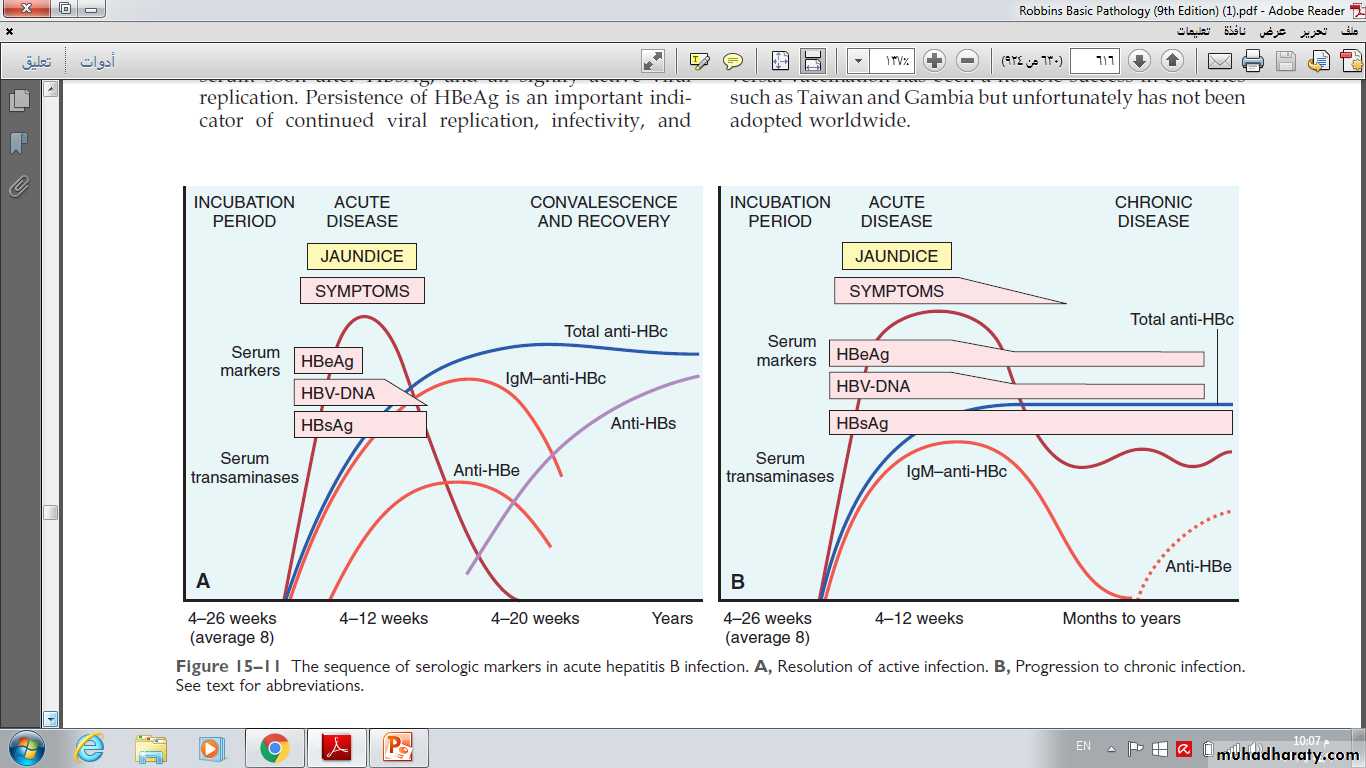
The natural course of the disease can be followed by serum markers ( figure below).
Sequence of serologic markers for hepatitis B viral hepatitis demonstrating (A) acute infection with resolution and (B) progression to chronic infection.
•
HBsAg appears before the onset of symptoms, peaks during overt disease, and then declines to undetectable levels in 3 to 6 months.(for diagnosis of acute infection)•
Anti-HBs antibody does not rise until the acute disease is over.
•
HBeAg, HBV-DNA, and DNA polymerase appear in serum soon after HBsAg, and all signify active viral replication. Persistence of HBeAg is an important indicator of continued viral replication, infectivity, and probable progression to chronic hepatitis. The appearance of anti-HBe antibodies implies that an acute infection has peaked and is on the wane.
•
IgM anti-HBc becomes detectable in serum shortly before the onset of symptoms.(for diagnosis of acute infection) Over a period of months the IgM anti-HBc antibody is replaced by IgG anti-HBc.
Hepatitis B can prevented by vaccination and by the screening of donor blood, organs, and tissues.