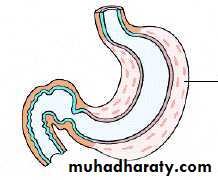
Stomach Pathology
GastritisAcute
Causes: infectious, chemical
Histologically: Edema, hyperemia, mucosal erosions and hemorrhage.
Chronic
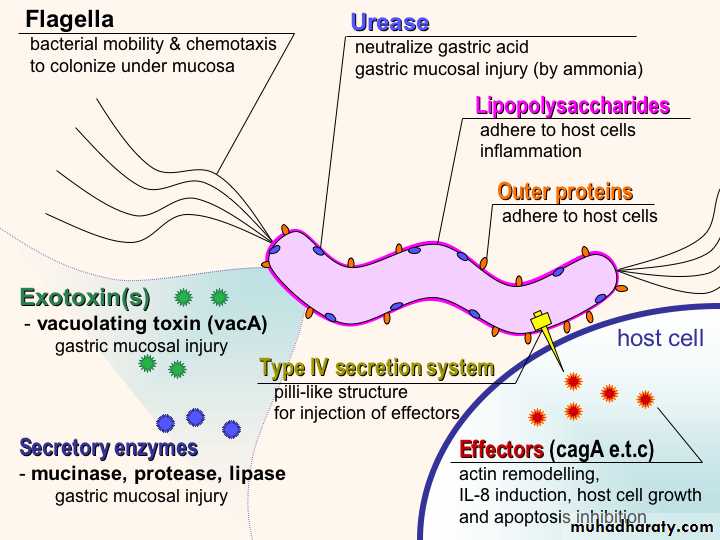
Helicobacter pylori infection (type B, antral, chronic active with lymphoid follicles)
Autoimmune (type A, body, atrophy, pernicious anemia)
Chemical (induced by drugs, bile reflux, alcohol(
Nonspecific symptoms, abdominal pain
The pathogenesis of acute ulceration
• NSAID-induced ulcers are caused by direct chemical irritation as well as cyclooxygenase inhibition, which prevents prostaglandin synthesis.• This eliminates the protective effects of prostaglandins, which include enhanced bicarbonate secretion and increased vascular perfusion.
• Lesions associated with intracranial injury are thought to be caused by direct stimulation of vagal nuclei, which causes gastric acid hypersecretion.
Systemic acidosis, a frequent finding in critically ill patients, also may contribute to mucosal injury by lowering the intracellular pH of mucosal cells.
Hypoxia and reduced blood flow caused by stress-induced splanchnic vasoconstriction also contribute to acute ulcer pathogenesis.
Acute gastric ulcers
Macroscopic finding
It range in depth from shallow erosions caused by superficial epithelial damage to deeper lesions that penetrate the mucosa.
Acute ulcers are rounded and typically are less than 1 cm in diameter.
The ulcer base frequently is stained brown to black by acid digested extravasated red cells, in some cases associated with transmural inflammation and local serositis. While these lesions may occur singly, more often multiple ulcers are present within the stomach and duodenum.Acute stress ulcers are sharply demarcated, with essentially normal adjacent mucosa, although there may be suffusion of blood into the mucosa and submucosa and some inflammatory reaction.
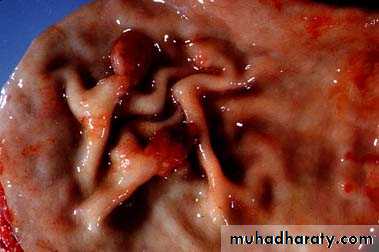
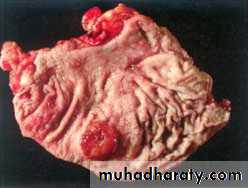
Acute gastritis
A, Gross view showing punctate erosions in an otherwise unremarkable mucosa; adherent blood is dark due to exposure to gastric acid.B, Low-power microscopic view of focal mucosal disruption with hemorrhage; the adjacent mucosa is normal.
Chronic gastritis
Epithelial damage: increase of nuclei, distorsion of foveolae and glands)Mucosal infiltrates of lymphocytes and plasma cells
Active process: neutrophil granulocytes (acute damage of epithelial cell)
Atrophy: chief and parietal cell loss and replacement by intestinal type epithelial cells
Intestinal metaplasia: acid mucin containing goblet cells, microvilli, Panneth cells
Regenerative changes: foveolar hyperplasia, increase of myofibroblasts and capillaries
Chronic gastritis
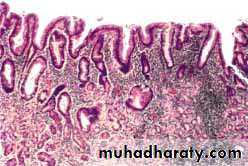
partial replacement of the gastric mucosal epithelium by intestinal metaplasia (upper left) and inflammation of the lamina propria (right) containing lymphocytes and plasma cells.Helicobacter associated chronic gastritis
Gross: red mucosa, coarser texture than normal, may have thickened rugal folds or thin/flat mucosa; with long term disease, mucosa may be thin/flat; usually affects antrum (particularly in children), and cardia .Micro:
Bacteria is curved, spirochete-like, in superficial mucus layer and along microvilli of epithelial cells; are (not invasive); are usually not seen in areas of intestinal metaplasia; associated with chronic inflammatory infiltrate with germinal centers (follicular gastritis) and plasma cells in lamina propria; active inflammation if neutrophils in glandular or surface epithelial layerHelicobacter pylori.
Steiner silver stain demonstrates the numerous darkly stained Helicobacter organisms along the luminal surface of the gastric epithelial cells.Note that there is no tissue invasion by bacteria.
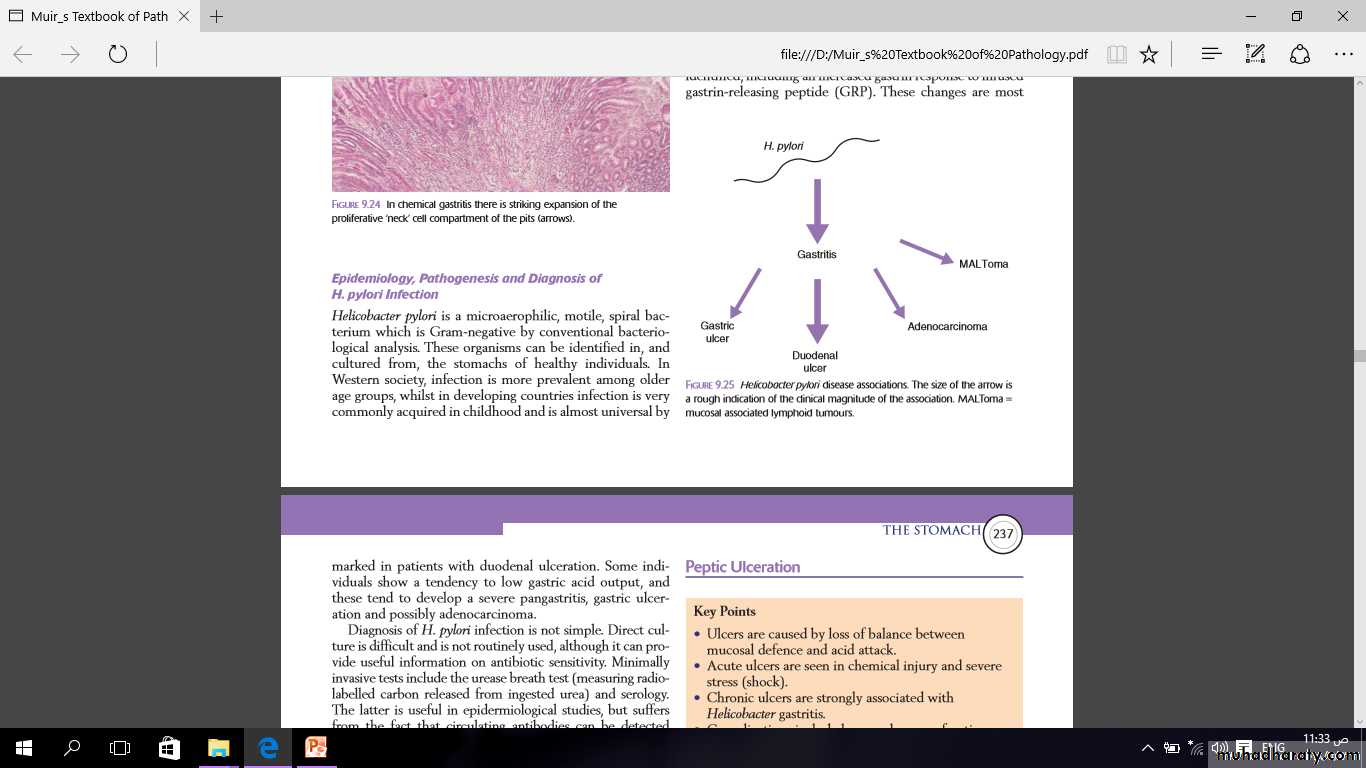
Helicobacterpylori disease associations. The size of the arrow is a rough indication of the clinical magnitude of the association. MALToma = mucosal associated lymphoid tumours
PEPTIC ULCER DISEASE
Ulcer: focal destruction of mucosa or deeper (necrosis)Erosion: less than full thickness focal loss of mucosa, can progress to ulcer or heal without scarring.
Peptic : primary autodigestive lesion caused by the action of gastric juice.
Sites: Esophagus, stomach, duodenum and ectopic mucosa
Hyperacidity.
Decreased mucosal protection.
Diagram of causes of, and defense mechanisms against, peptic ulceration.
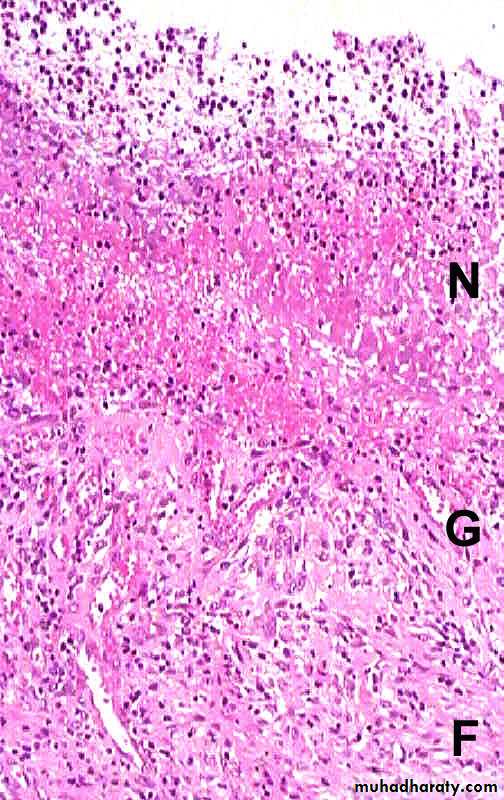
Diagram of the base of a non perforated peptic ulcer, demonstrating the layers of necrosis (N), inflammation (I), granulation tissue (G), and scar (S), moving from the luminal surface at the top to the muscle wall at the bottom.Complications of ulcer
BleedingPerforation
Obstruction
Penetration
Pain
• Complications of gastric ulcer:
• Bleeding
• Occurs in 15% to 20 % of patients.
• Most frequent complication.
• May be life-threatening.
• Accounts for 25% of ulcer deaths.
• May be the first indication of an ulcer.
• Perforation
• Occurs in up to 5% of patients.
• Accounts for two thirds of ulcer deaths.
• It is rarely the first indication of an ulcer.
• Obstruction
• Mostly in chronic ulcers.
• Secondary to edema or scarring.
• Occurs in about 2% of patients.
• Most often associated with pyloric channel ulcers.
• May occur with duodenal ulcers.
• Causes incapacitating crampy abdominal pain.
• Can rarely cause total obstruction and intractable vomiting.
Predisposing factors for peptic ulcer of stomach and duodenum
Helicobacter pyIoridirect mucosal injury
increased acid secretion
inflammatory reaction
Trauma: surgery, fractures, burns (Curling ulcer)
Stress.
Cerebral Lesions.
Vagus nerve stimulation (hypothalamus)
Smoking.
Zollinger-Ellison syndrome.
gastrin overproduction, tumor (gastrinoma)
Genetic Factors.
Steroid hormons and Nonsteroidal anti-inflammatory drugs.
blocks prostaglandin synthesis.
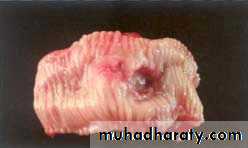
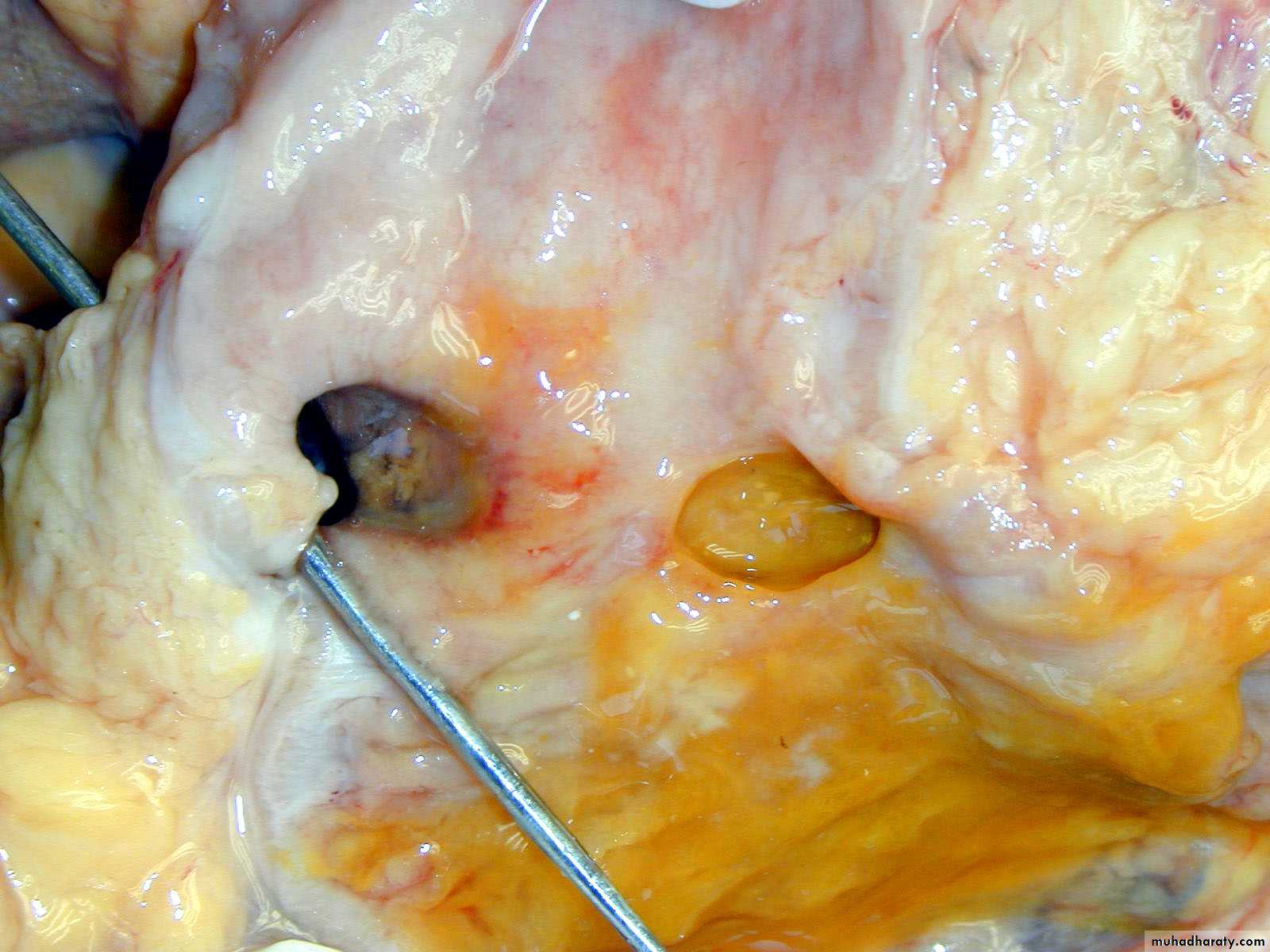
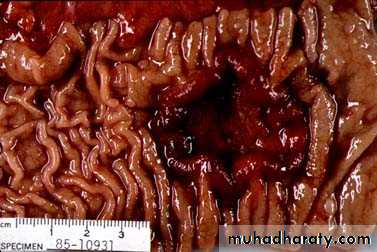
Peptic ulcer of the duodenum.
Note that the ulcer is small (2 cm) with a sharply punched-out appearance. Unlike cancerous ulcers, the margins are not elevated.
The ulcer base is clean.
TUMORS
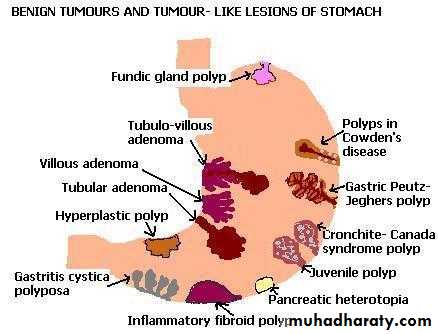
Benign Epithelial Tumors:Hyperplastic and inflammatory polyps
True adenomas rare and not the leading cause of carcinoma
Malignant Epithelial Tumors:
Adenocarcinoma
Malignant Non - Epithelial Tumors:
Lymphoma
Potentially Malignant Tumors:
Endocrine tumors (carcinoid)
GIST
Gastric tumors
PolypsUncommon 0.4% of adults at autopsy as compared to colon polyps in 25-50% of adults at autopsy.
Many types
Hyperplastic- response to damage.
Fundic gland polyp: small hamartoma.
Note:
(hyperplastic and fundic gland polyps have no malignant potential)
Adenomatous polyp have malignant potential!
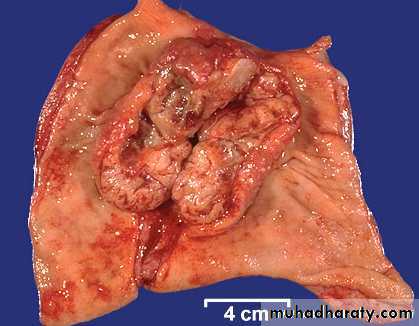
Pedunculated gastric adenoma
Gastric adenoma
Gross photograph showing a large polyp in the stomach.Etiologic factors of stomach carcinoma
• Related to socioeconomic level and diet.• High incidence in Japan, actually is decreasing in the Western world, continue to be high in Asia and Russia.
• Smoked, salted foods.
• Low fresh vegetable diet.
• Nitrosamines.
• Chronic gastritis with atrophy and metaplasia.
• H. pylori infection.
• Intestinal reflux.
• Blood group A.
• Relatives with stomach cancer.
Precancerous lesions
DysplasiaEnlarged, hyperchromatic, irregularly outlined, crowded nuclei.
Irregular glands, mitoses.
High grade dysplasia = in situ carcinoma = intraepithelial neoplasia.
Adenoma
Malignant neoplasms of the stomach:
Gastric Adenocarcinoma (~ 95%).
Squamous Cell Carcinoma.
Adenoacanthoma.
Carcinoid.
Gastrointestinal stromal tumors.
Lymphoma.
Carcinoma of the stomach
Sites: classically prepyloric, antral and lesser curvature.Macroscopic types (Borrmann I-IV):
polypoid, ulcerative, ulcerating and infiltrating, infiltrating.
Microscopic types (Laurens):
Intestinal:
Gland forming, distal, better differentiated, usually old.
Diffuse:
Proximal, intracellular mucus, signet ring cells, less differentiated, usually young patient.
Lauren classification System for gastric adenocarcinoma
Intestinal• Environmental.
• Gastric atrophy with intestinal metaplasia.
• Men > women.
• Increasing incidence with age.
• Gland formation.
• Hematogenous Spread.
• Microsatellite instability.
• APC gene mutations.
• p53, p16 inactivation.
• APC, adenomatous polyposis coli.
• Diffuse
• Blood group type A.
• Women > men.
• Younger age group.
• Poorly differentiated,signet ring cells.
• Transmural /lymphatic spread.
• Decreased E-cadhedrin.
• p53, p16 inactivation.
Clinical Presentation
AsymptomaticEarly:
Vague epigastric discomfort / indigestion
• Pain is constant, nonradiating, unrelieved by food digestion
More advanced disease:
Weight loss
Anorexia
Fatigue
Emesis
Symptoms dependent on location
Proximal
Distal
Diffuse gastric ca. presented with GI bleeding, obstruction
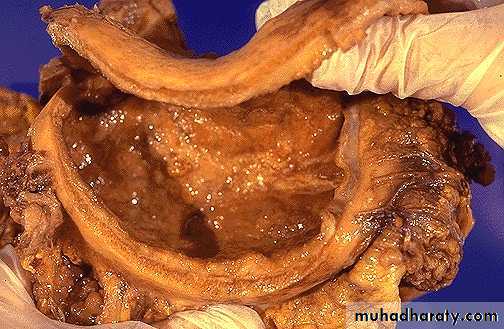
Morphologic types of carcinoma of the stomach
Fungating
UlceratingDiffuse
Fungating Carcinoma Stomach
Ulcerating Gastric Carcinoma