Bacterial skin infections
Dr. Hadaf Aljunaiyehobjectives
After completing this lecture, the student should be able to:Describe the morphology of common cutaneous bacterial infections.
Discuss the bacterial etiologies of cellulitis and erysipelas.
Become familiar with superinfection of resident normal flora
Recommend initial steps for the evaluation and treatment of common cutaneous bacterial infections.
Natural defense of skin
1- Temperature more than 37cº2- Dryness
3- Keratin & normal desquamation
4- Sebum with its low PH & high lipid content
5- Sweat with its low PH & high salt content
6- Skin associated Lymphoid tissue
7- Resident Microflora (mainly gram positive)
Resident microflora
Millions of micro organisms, reside harmlessly on skin
The total microbial cell count in and on our bodies is 10 times greater than the number of human cellsAfter the gut, there are more microorganisms on the skin than anywhere else in the body
Bacterial species are the most numerous among the flora
Fungi, viruses and mites are also found on the normal skin
Resident microflora
Resident flora are found in the upper parts of the epidermisand congregated in and around the hair follicles. They include:
Bacteria: Staphylococci, Micrococci, Diphtheroids: Corynebacterium, & Brevibacterium
Fungi: Candida albicans, Malasezzia & many other species
Staph.epidermidis+aerobic diphtheroids predominate on the surface, Anaerobic diphtheroids are deep in the hair follicles
Transient bacteria
S. aureus does not normally reside on the skin, but may be present transiently, inoculated from colonized sites such as the nares(30%), axillae & vaginaThis colonization is usually transient except in 10-20% of cases where it becomes persistent, these are called staph carriers & are a hazard to the society
primary bacterial infections
Impetigo & ecthymaFolliculitis
Furuncles & Carbuncles
Erysipelas
Cellulitis
Secondary bacterial infection
Infection of previously damaged or diseased skin, such as
Dermatitis
Herpes simplex
Burn
Scabies & pediculosis
*Any child presenting with recurrent impetigo of the scalp we should look for underlying pediculosis capitis*
impetigo
Acute, contagious bacterial infection of the skin, of 2 types:Bullous: caused by S. aureus
Non-bullous: mainly by group A ℬ heamolytic streptococci
Peak incidence in ages 2-5 years, but can affect older children & adults, with equal incidence in males & females
Can be primary or secondary
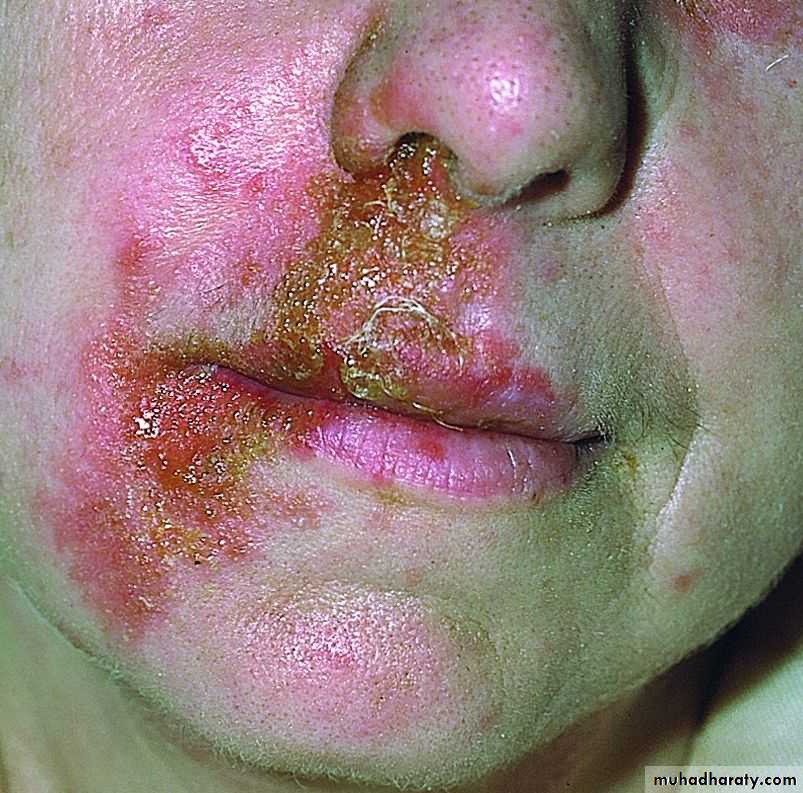
Non- bullous impetigo
Caused by strept., staph., or usually a mixture of bothStarts as a thin walled vesicle on an erythematous base, which soon ruptures & a crust forms (yellowish brown= honey colored)
It heals without scarring
May cause regional adenitis & fever in severe cases
It can affect any part, except palms & soles
Mostly exposed parts, especially central face around
the nose; the site of staph carriage
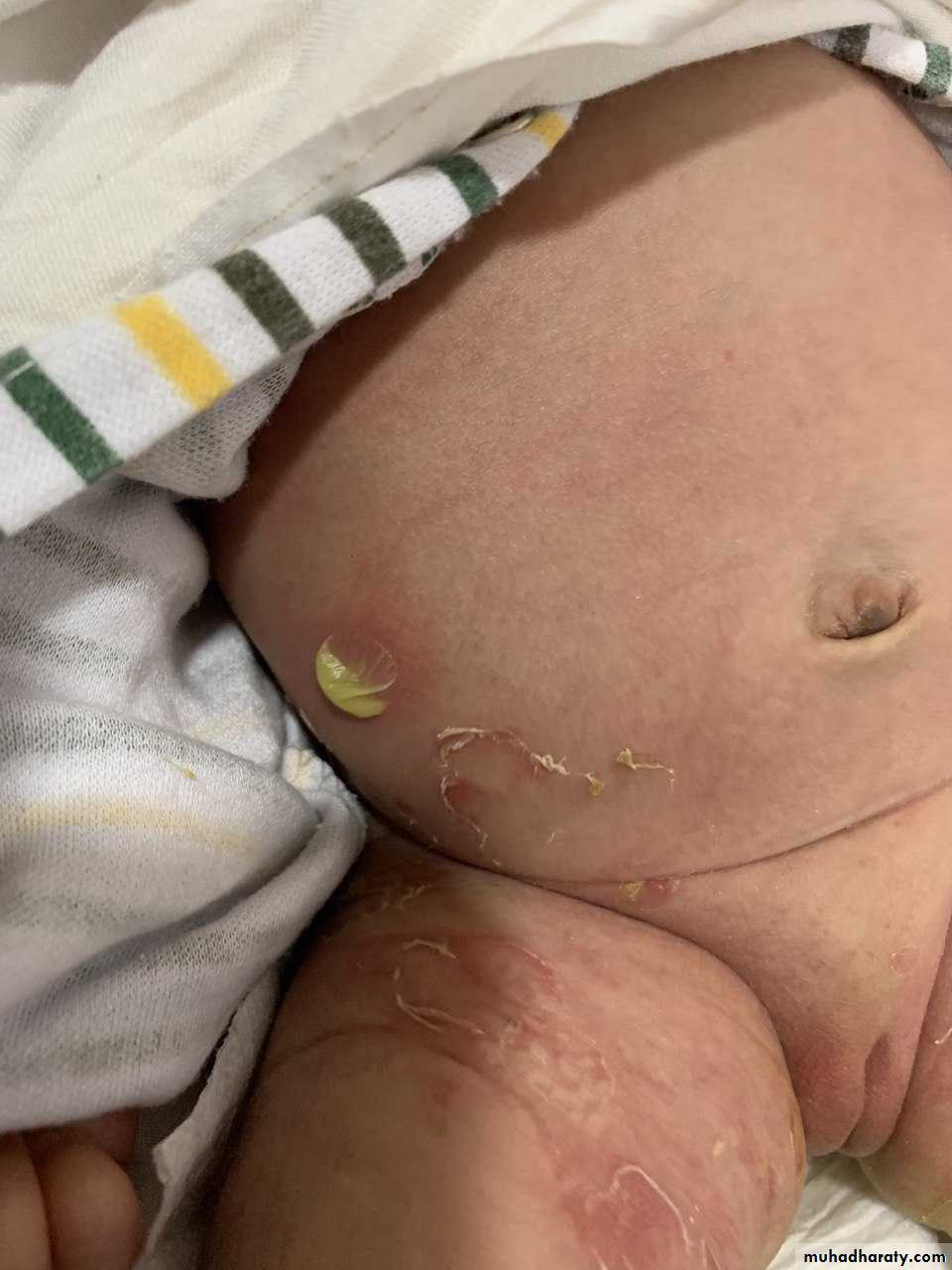
Bullous impetigo
Mostly caused by s. aureusThe newborn is the main victim, but can affect older
children
Target area is the face, but can occur anywhere even palm & soles
Bullae are larger, persist longer(2-3 days),
contents are first clear then become turbid,
then rupture forming thin varnish-like
brownish crusts
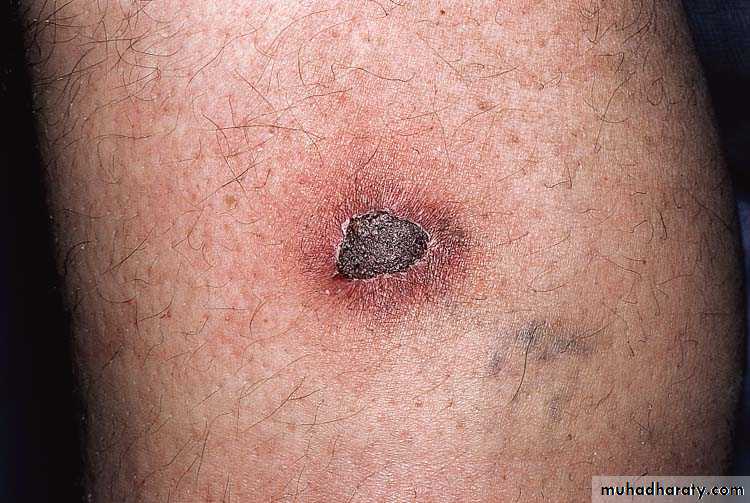
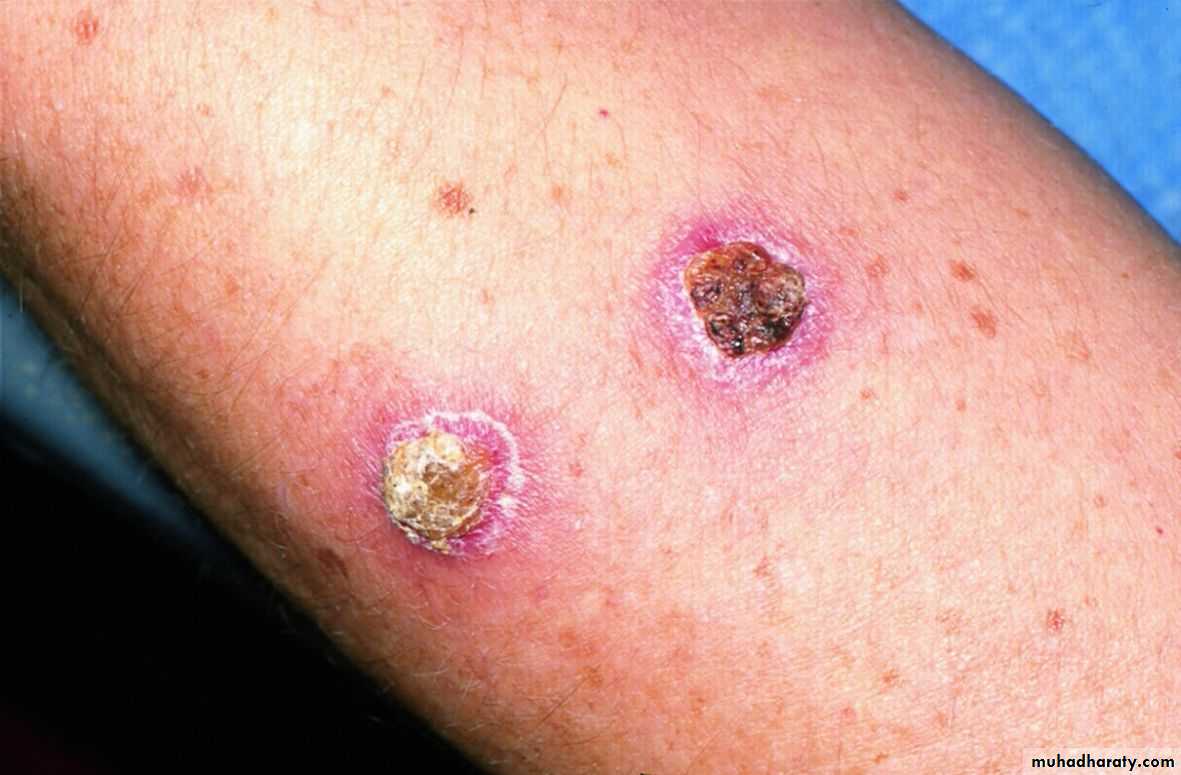
Ecthyma
A lesion of neglect, develops at site of old traumaMostly elderly, diabetic, debilitated, or alcoholic
patients (= vagabond’s disease)
Caused by strpt. pyogenes, & staph. aureus
Mostly on lower limbs
Present as adherent crusts, beneath which is a purulent irregular ulcer, & delayed healing with scarring.
Complications of impetigo
lymphangitis, lymphadenitis.Staphylococcal scalded skin syndrome (SSSS).
Post streptococcal acute glomerulonephritis, especially in cases due to streptococcus pyogenes M type 49
Treatment
Wet compresses with an antiseptic solution as potassium permanganate solution to remove crusts plus a topical antibiotics is usually enough in mild cases.If severe or a nephritogenic strain of streptococci is suspected; then a systemic antibiotic is added as flucloxacillin, erythromycin or cephalexin.
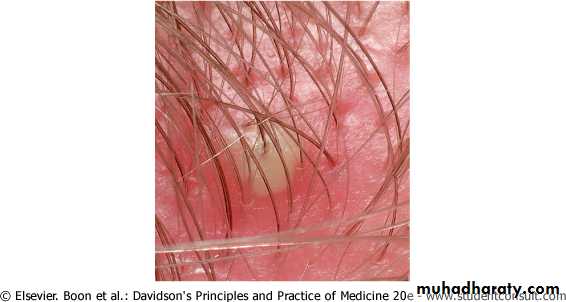
Staphylococcal infections: 1- superficial folliculitis:
An inflammatory disease of the hair follicles, which may be infectious or non infectiousThe infection is superficial involving the ostium of the hair follicle
Usually caused by staph aureus
Common on scalp of children, beard, axillae, extremities, buttocks
Usually heal spontaneously in 1 week, or become chronic
In adults can progress to boils
Folliculitis
Can be:1- Infective: bacteria & yeast (pityrosporum)
2- Chemical: by mineral oils
3- Physical: as after hair epilation
2- deep folliculitis (=furuncles=boils)
Staphylococcal infection of the hair follicles, similar to but deeper than folliculitisStart as firm, red, tender papule that becomes painful & fluctuant nodule, finally ruptures & discharges pus, leaving a scar
Sites of friction & sweating; mostly on the neck, buttocks & ano-genital area due to staph. carriage at these areas
Constitutional symptoms may be present
Some patients may have recurrent attacks (=chronic furunculosis)
Chronic furunculosis
They may recur at intervals for no apparent cause, these patients are staph carriers (carry s. aureus in their nostrils, axillae & groins)
May be treated by topical antibiotics applied to carrier sites
Long courses of oral flucloxacillin
Care about hygiene & predisposing factors
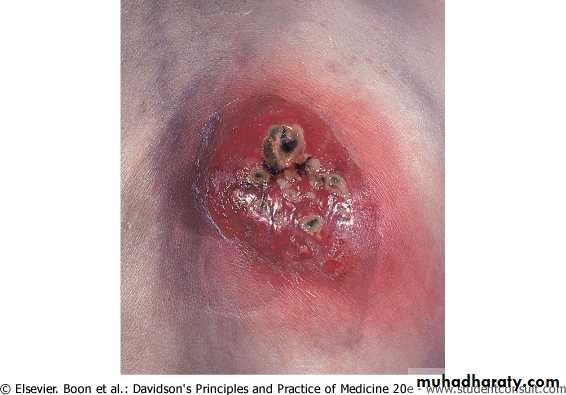
Carbuncle
A collection of boilsSwollen suppurating painful areas discharging pus from several points (sieve-like)
Usually occur in areas of thick inelastic skin, the infection spreads to subcutaneous fat such as nape of neck, back & thighs
More painful & severe with constitutional symptoms
More in diabetics
Blood stream invasion may occur
Management of folliculitis
Correction of underlying causes: diabetes, anemia, poor hygieneSwabs for culture from lesions & carrier sites
Topical & systemic antibiotics
Incision of boils & carbuncle to speed healing
Recurrent boils need treatment of carrier sites by BID topical antibiotics for 6 weeks+ improve patient’s hygiene.
Streptococcal infections: Erysipelas & cellulitis
Cellulitis: infection of the subcutaneous tissue
Erysipelas: infection of the dermis & upper part of subcutaneous tissue by group A ℬ heamolytic streptococci
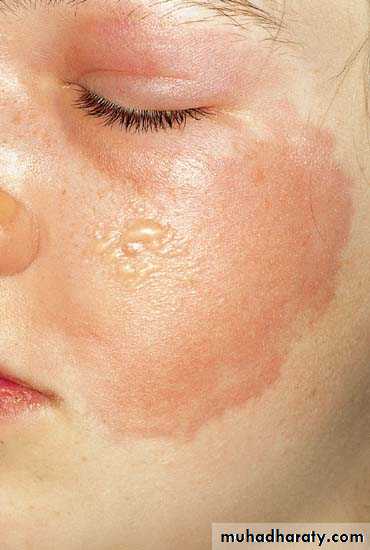
Erysipelas
Minor cracks or wounds in the skin are the port of entryStarts with severe constitutional symptoms
Followed by appearance of rapidly spreading painful erythematous plaque with well defined margins
May show hemorrhage or blistering
80% occur on the face
Can be fatal if untreated
Cellulitis
Similar to erysipelas, with some differences1- Deeper level of skin involvement (subcutaneous tissue)
2- can be caused by other organisms in addition to streptococci like s. aureus, E. coli
3- More raised & swollen but less well-defined border
4- More on the lower limbs than the face
Cellulitis
Complications
1- Recurrences may lead to lymphedema2- Subcutaneous abscess
3-Septicemia
4- Nephritis
Treatment
Rest, analgesiaSystemic antibiotics especially penincillin e.g: benzyl penicillin 600-1200 mg IV/6 hourly or cephalosporin
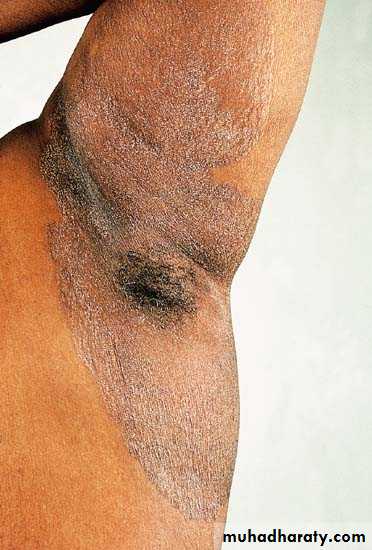
Erythrasma
Caused by corynebacterium minutissimum a member of resident floraAsymptomatic, well demarcated, scaly, reddish brown
Body folds: axilla, groins, toe webs
Coral red fluorescence with Wood’s lamp
Treated by topical antifungal, antibiotics, or sometimes systemic erythromycin
Bacterial
STAPH.STREPT.
MIXED
SUPERFICIAL
FOLLICULITIS
ERYSIPELAS
IMPETIGO
DEEP
FURUNCLES & CARBUNCLES
CELLULITES