بسم الله الرحمن الرحيم
10/01/2021
كلية الطب جامعة ذي قار
ذي قار الناصريه
Pneumonia
Dr. Majeed Mohan Alhamami
Dep. Of medicine
Objectives
To know the the followingEpedimology
Etiology
Pathogenesis
Clinical presentation
Complication
Investigation
Treatment
Prognosis
Community-acquired pneumonia (CAP)
The sixth leading cause of death in the United States.
Responsible for 4 to 10 million respiratory infections each year..
5-12% of all lower respiratory tract infections.
The incidence varies with age, being much higher in the very young and very old, in whom the mortality rates are also much higher.
• Pneumonia
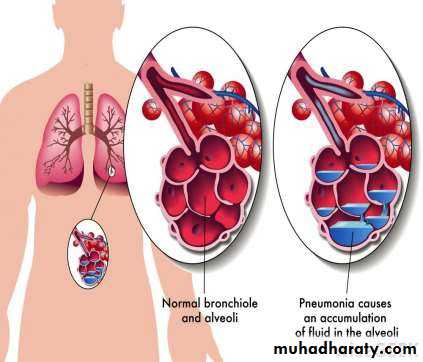
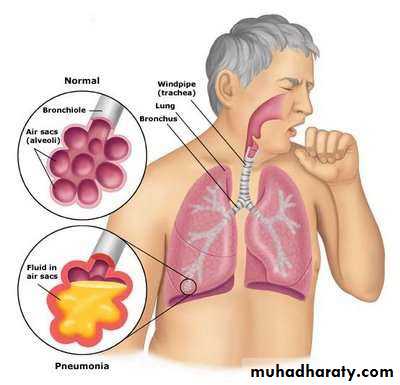
• Pneumonia is an infection• in one or both lungs.
• Pneumonia causes
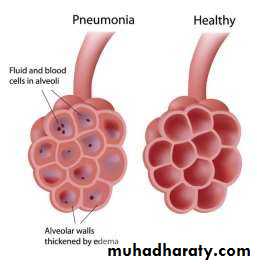
• inflammation in the alveoli.
• The alveoli are filled with fluid or pus, making it difficult to breathe.
•
• DEFINITION
It is as an acute respiratory illness associated with recently develope Pneumonia is as an acute respiratory illness associatedwith recently developed radiological pulmonary shadowing, which may be segmental, lobar or multilobar. pulmonary shadowing, which may be segmental, lobar or multil
• COSOLIDATION = ‘Inflammatory induration of a normally aerate
Pneumonias classification
Clinicalcommunity-acquired
hospital-acquired, HCAP VAP
immunocompromised hosts. ‘
Morphological
Lobar pneumonia’ .Bronchopneumonia’.
Interstitial pneumonia.
Etiological a causative organism:
bacerial
viral .
fungal.
Parasitice
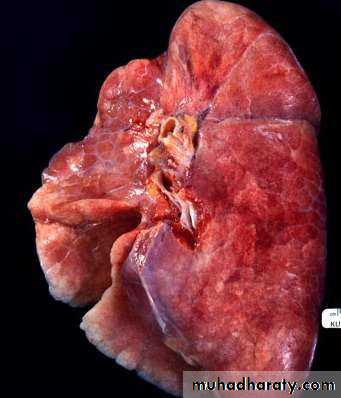
Lobar and bronchopneumonia
Lobar pneumonia’ is a radiological and pathological term referring to homogeneous consolidation of one or more lung lobes, often with associated pleural inflammation.
Bronchopneumonia’ refers to more patchy alveolar consolidation associated with bronchial and bronchiolar inflammation, often affecting both lower lobes.
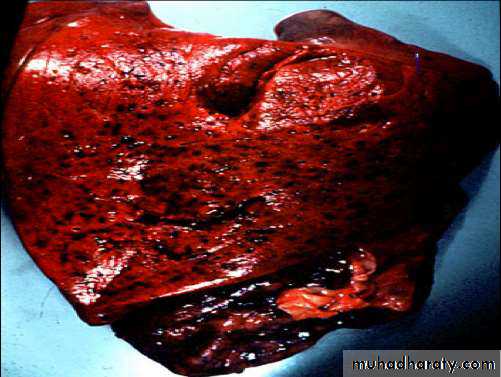
The inflammatory response in lobar pneumonia
Evolves through stages ofCongestion.
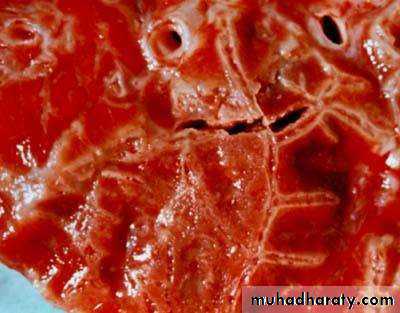
Red hepatisation.
Grey hepatisation .
Finally resolution.
.
• Congestion
• Presence of a proteinaceous exudate—and often of bacteria—in the alveoli• RED HEPATIZATION
• Presence of erythrocytes in the cellular intraalveolar exudate• Neutrophils are also present
• Bacteria are occasionally seen in
• cultures of alveolar specimens collected
• Normal Lung
• Red Hepatization• GRAY HEPATIZATION
• No new erythrocytes are extravasating, and those• already present have been lysed and degraded
• Neutrophil is the predominant cell
• Fibrin deposition is abundant• Bacteria have disappeared
• Corresponds with successful containment of the
• infection and improvement in gas exchange
• Factors that predispose to Pneumonia
Cigarette smoking
• Upper respiratory tract infections• Alcohol
• Corticosteroid therapy
• Old age
• Recent influenza infection
• Pre-existing lung disease
• HIV
• Indoor air pollution
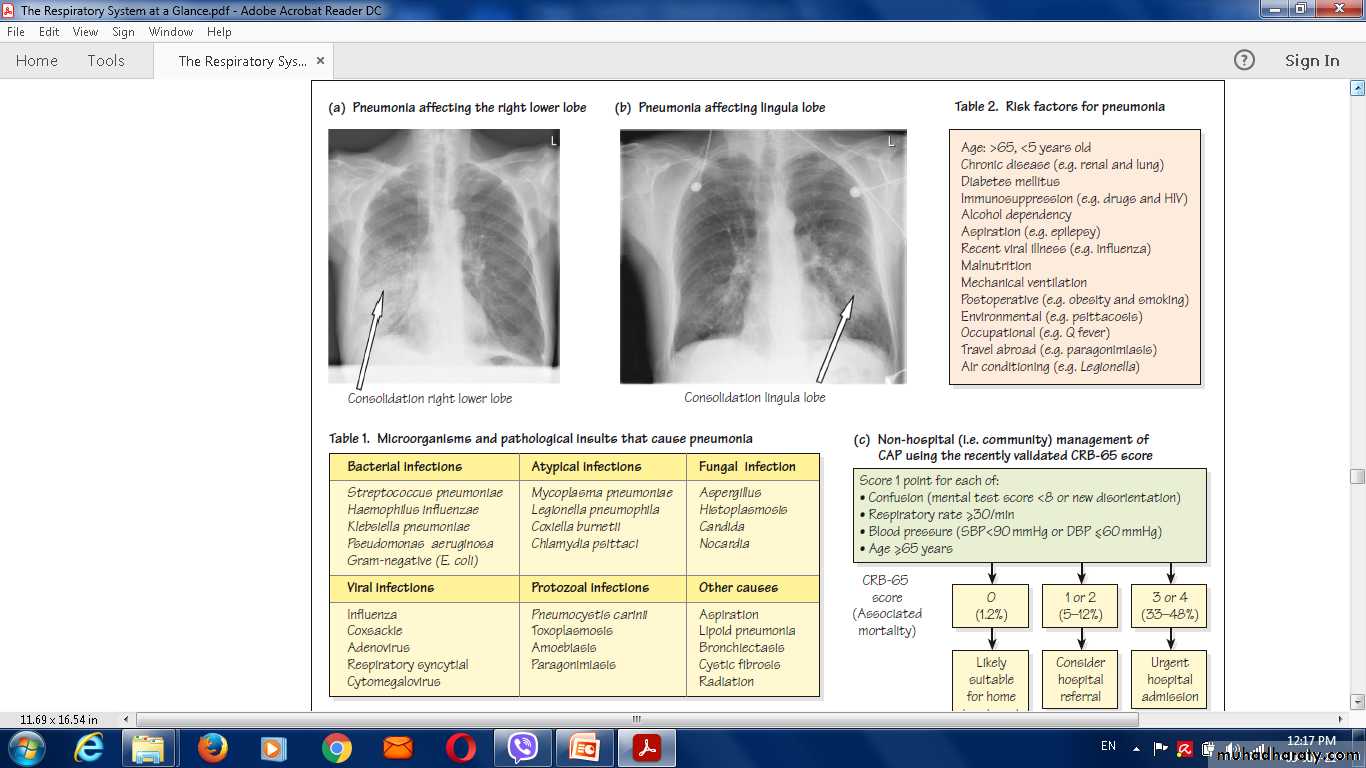
Organisms causing community-acquired pneumonia
Bacteria• Streptococcus pneumoniae
• Mycoplasma pneumoniae
• Legionella pneumophila
• Chlamydia pneumoniae
• Haemophilus influenzae
• Staphylococcus aureus
Chlamydia psittaci
• Coxiella burnetii (Q fever,
‘querry’ fever)
• Klebsiella pneumoniae
• Actinomyces israelii
Organisms causing community-acquired pneumonia
Viruses
SARS-CoV-2(COVID-19)
• Influenza, parainfluenza
• Measles
• Herpes simplex
• Varicella
• Adenoviruse
Cytomegalovirus (CMV)
(• Coronavirus ( SARS,MERS
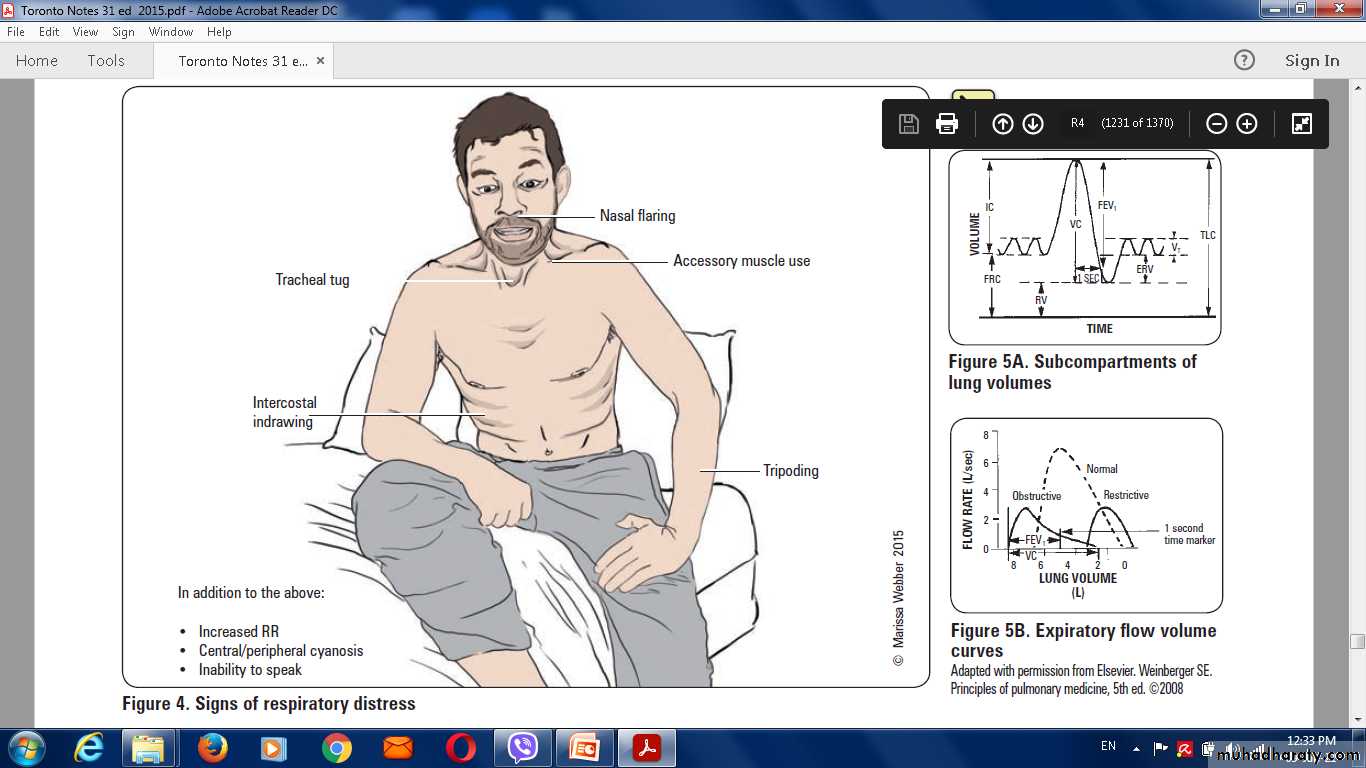
Clinical features
Pneumonia, particularly lobar pneumonia, usuallypresents as an acute illness.
Systemic features such as
fever,
rigors, shivering
malaise
delirium .
Decrease appetite .
headache.
Clinical features
Pulmonary symptoms
cough, which at first is short, painful and dry, but later accompanied by the expectoration of mucopurulent sputum.
Rust-coloured sputum may be seen in patients with Strep. pneumoniae,
haemoptysis.
Pleuritic chest pain.
Upper abdominal tenderness .
On examination
The respiratory and pulse rate may be raisedThe blood pressure low,
delirium.
Temperature may be normal
Oxygen saturation on air may be low, and the patient cyanosed and distressed.
Herpes labialis-----Streptococcal pneumonia
poor dental hygiene ----Klebsiella or Actinomyces israelii
Chest signs
Depending on the phase of the inflammatory response.When consolidated, the lung is
typically dull to percussion ,
bronchial breathing and whispering pectoriloquy; crackles..
Prevention
Stop smoking.Influenza and pneumococcal vaccination .
Legionella pneumophila notification.
• Malneutrion treatment.
• Correct indoor air pollution,
• encouragingimmunisation against measles, pertussis and Haemophilus ,influenzae type b are particularly important in children.
Differential diagnosis of pneumonia
Pulmonary infarction• Pulmonary/pleural TB
• Pulmonary oedema (can be unilateral)
• Pulmonary eosinophilia .
• Malignancy: bronchoalveolar cell carcinoma
• Rare disorders: cryptogenic organising pneumonia/
bronchiolitis obliterans organising pneumonia (COP/BOOP
Investigations in CAP
Blood
Full blood count
• Very high (> 20 × 109/L) or low (< 4 × 109/L) white cell
count: marker of severity
• Neutrophil leucocytosis > 15 × 109/L: suggests bacterial
aetiology
• Haemolytic anaemia: occasional complication of Mycoplasma
Urea and electrolytes
• Urea > 7 mmol/L (~20 mg/dL): marker of severity
• Hyponatraemia: marker of severity
Liver function tests
• Abnormal if basal pneumonia inflames liver
• Hypoalbuminaemia: marker of severity
Erythrocyte sedimentation rate/C-reactive protein
• Non-specifically elevated
Investigations in CAP
BloodBlood culture
• Bacteraemia: marker of severity
Serology
• Acute and convalescent titres for Mycoplasma, Chlamydia,
Legionella and viral infections
Cold agglutinins
• Positive in 50% of patients with Mycoplasma
Arterial blood gases
• Measure when SaO2 < 93% or when severe clinical features to assess ventilatory failure or acidosis
Investigations in CAP
Sputum
Sputum samples
• Gram stain culture and antimicrobial sensitivity testing
Oropharynx swab
• PCR for Mycoplasma pneumoniae and other atypical
pathogens
Urine
• Pneumococcal and/or Legionella antigen
Investigations in CAP
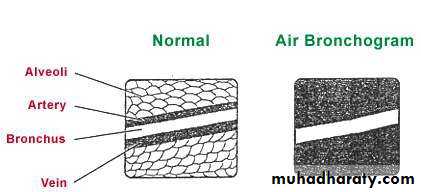
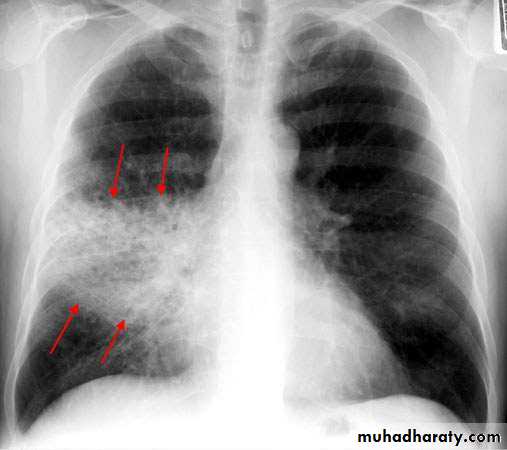
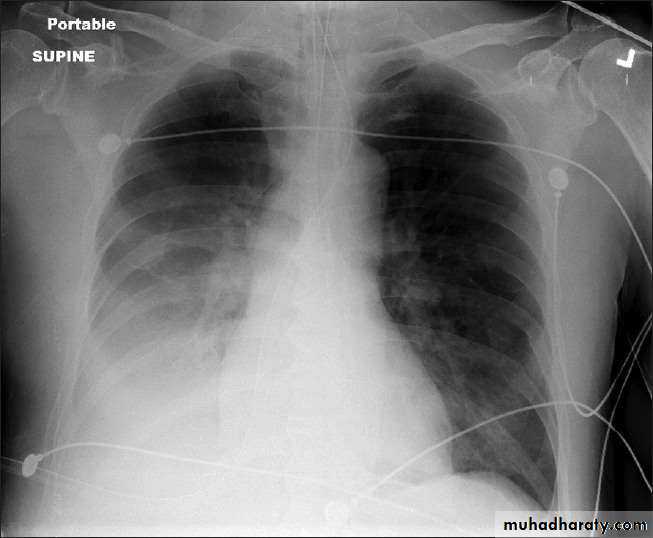
Chest X-ray and UltrasoundLobar pneumonia
• Patchy opacification ,consolidation.
• Air bronchogram (air-filled bronchi appear lucent against
consolidated lung tissue)
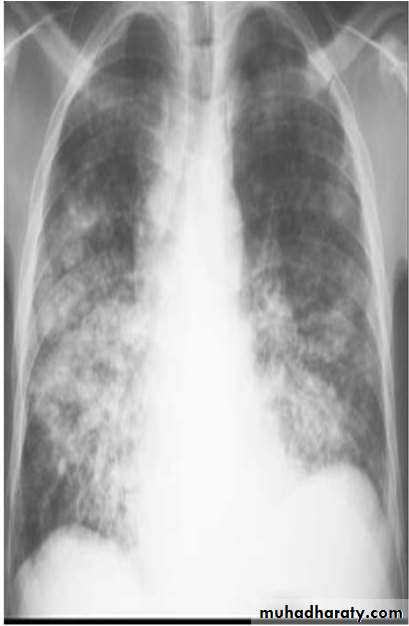
Bronchopneumonia
• Typically patchy and segmental shadowing
Complications
Staph. aureus
• multilobar shadowing, cavitation, pneumatocoeles and abscesses.
Pleural fluid
• Always aspirate and culture.
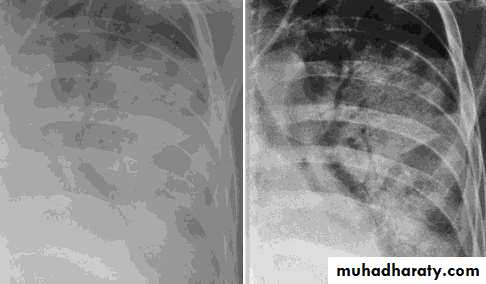
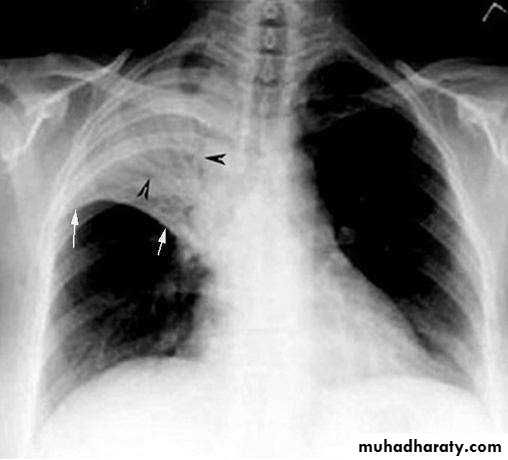
• X Ray
• Homogenous opacity with air bronchogram
• LOBAR PNEUMONIA
• Peripheral airspace consolidation pneumonia• Without prominent involvement of the bronchial tree
• RUL Consolidation
• RML Consolidation
• RLL Consolidation
• BRONCHOPNEUMONIA
• Centrilobular and Peribronchiolar opacity pneumonia• Tends to be multifocal
• Patchy in distribution rather than localized to any
• one lung region
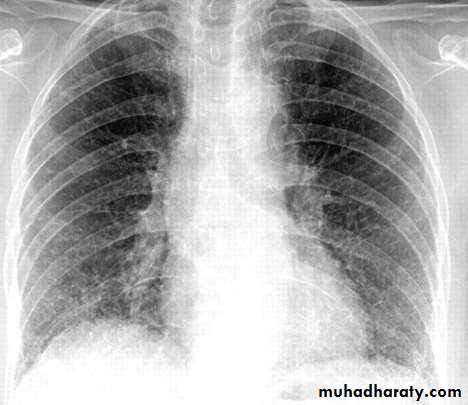
• INTERSTITIAL PNEUMONIA
• Peribronchovascular• Infiltrate
• Mycoplasma , viral
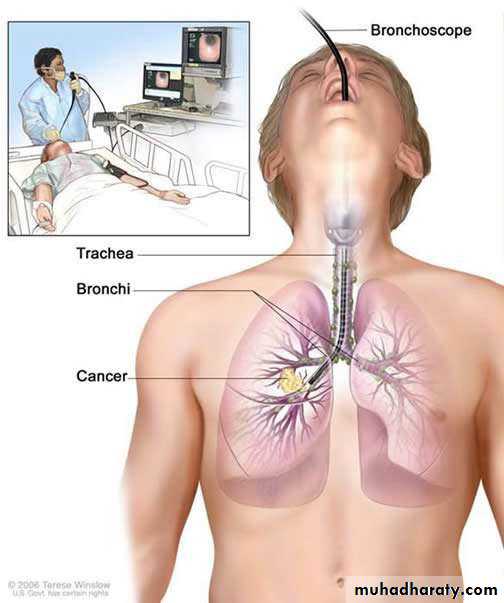
• INVASIVE Investigation
• Bronchoscopy• Thoracoscopy
• Percutaneous aspiration/biopsy
• Open lung biopsy
• Pleural aspiration
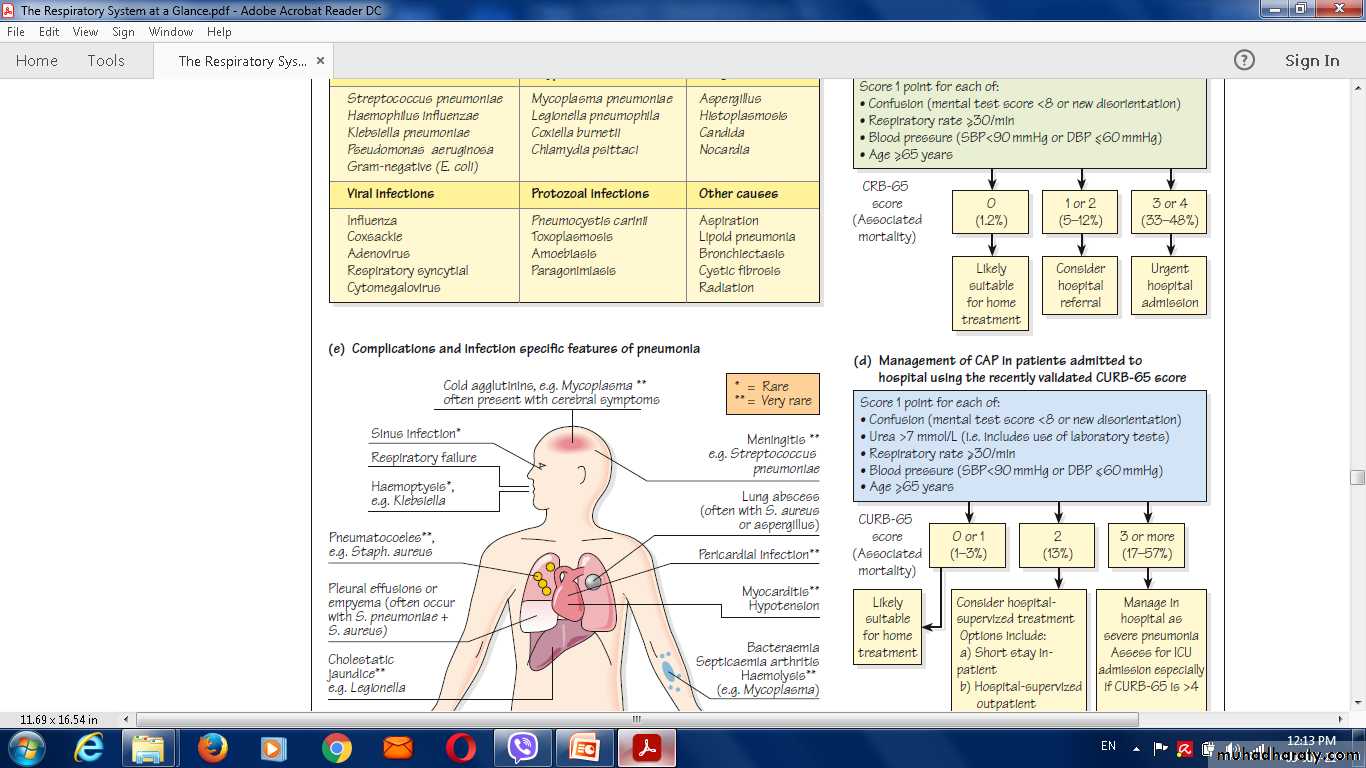
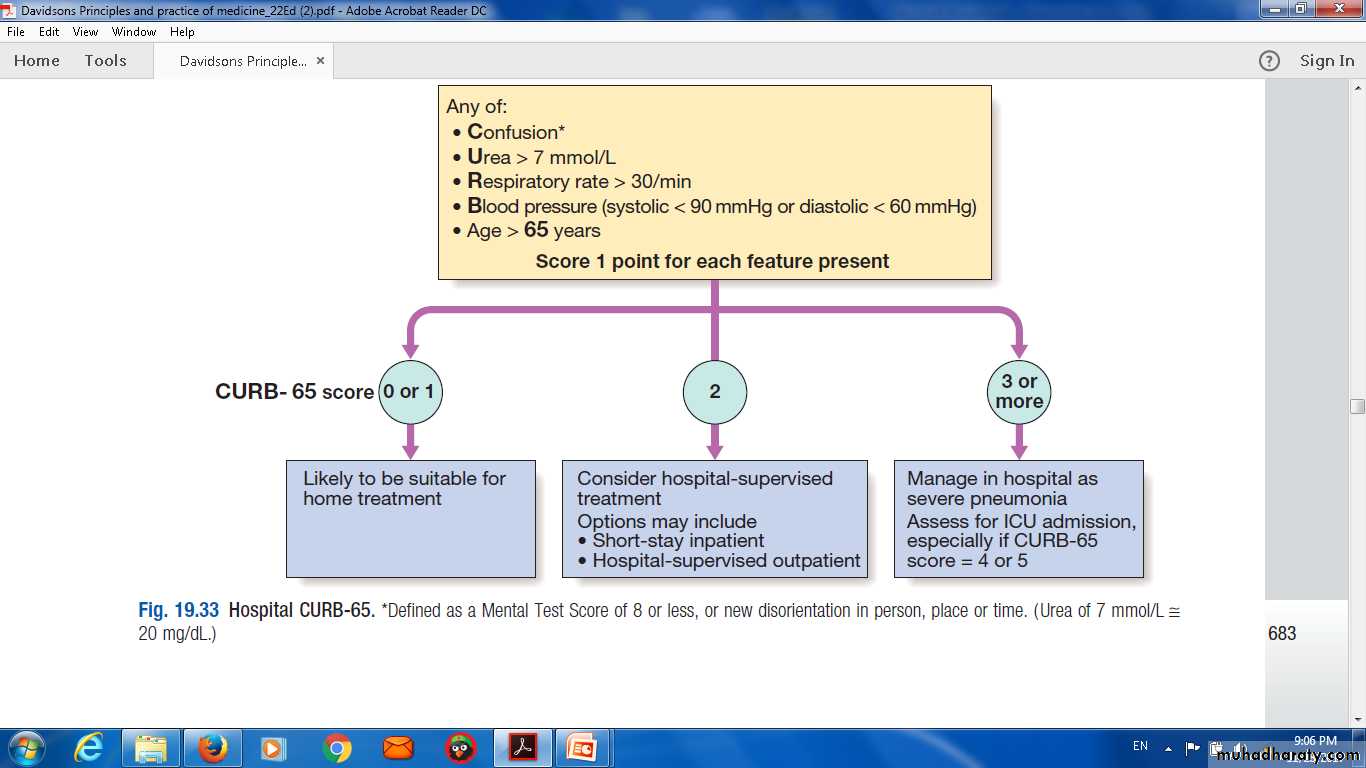
Hospital CURB-65. * Confusion Defined as a Mental Test Score of 8 or less, or new disorientation in person, place or time. ( Urea of 7 mmol/L ≅20 mg/dl)
Indications for referral to ITU
CURB score of 4–5, failing to respond rapidly to initialmanagement
• Persisting hypoxia (PaO2 < 8 kPa (60 mmHg)), despite high concentrations of oxygen
• Progressive hypercapnia
• Severe acidosis
• Circulatory shock
• Reduced conscious level
Complications of pneumonia
Para-pneumonic effusion – common• Empyema .
• lobar collapse
• Deep vein thrombosis and pulmonary embolism
• Pneumothorax, particularly with Staph. aureus
• Suppurative pneumonia/lung abscess
• ARDS, renal failure, multi-organ failure .
• Ectopic abscess formation (Staph. aureus)
• Hepatitis, pericarditis, myocarditis, meningoencephalitis
• Pyrexia due to drug hypersensitivity
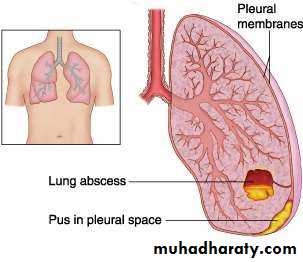
• COMPLICATIONS
• Lung abscess
• Para-pneumonic effusions
• Empyema
• Sepsis
• Metastatic infections (meningitis,endocarditis,arthritis)
• ARDS , Respiratory failure
• Circulatory failure
• Renal failure
• Multi-organ failure
Management
The most important aspects of management areOxygenation,
Fluid balanceAntibiotic therapy.
Nutritional support in severe or prolonged illness,
Oxygen
tachypnoea,
hypoxaemia,
hypotension
acidosis,
The aim of maintaining the PaO2 at or above 8 kPa
(60 mmHg) or the SaO2 at or above 92%.
High concentrations (35% or more), preferably humidifiedContinuous positive airway pressure (CPAP) for hypoxic despite this .
Intravenous fluids
severeillness,older patients
vomiting.
an adequate oral intake of fluid encouraged.
Antibiotic treatment for CAP
Antibiotics improves the outcome.The initial choice of antibiotic is guided by
1-clinical context,
• 2-severity assessment.
• 3- local knowledge of antibiotic resistance patterns .
• 4- available epidemiological information.
Antibiotic treatment for CAP
Uncomplicated CAP
• Amoxicillin 500 mg 3 times daily orally
If patient is allergic to penicillin
• Clarithromycin 500 mg twice daily orally or Erythromycin
500 mg 4 times daily orally
If Staphylococcus is cultured or suspected
• Flucloxacillin 1–2 g 4 times daily IV plus
• Clarithromycin 500 mg twice daily IV
If Mycoplasma or Legionella is suspected
• Clarithromycin 500 mg twice daily orally or IV or
Erythromycin 500 mg 4 times daily orally IV plus
• Rifampicin 600 mg twice daily IV in severe cases
Antibiotic treatment for CAP
Severe CAP• Clarithromycin 500 mg twice daily IV or Erythromycin 500 mg 4 times daily IV plus
• Co-amoxiclav 1.2 g 3 times daily IV or Ceftriaxone 1–2 g
daily IV or Cefuroxime 1.5 g 3 times daily IV or
• Amoxicillin 1 g 4 times daily IV plus flucloxacillin 2 g 4 times daily IV
Discharge and follow-up
The decision to discharge patients depends on their home circumstances and the likelihood of complications.
Clinical review should be arranged around 6 weeks later and a chest X-ray obtained if there are persistent symptoms,physical signs or reasons to suspect underlying malignancy.
Thank you
QQUIZE