• Lec : 10
Suturing and Periodontal Dressing• UNIVERSITY OF MOSUL
• COLLEGE OF DENTISTRY
• By:
• Dr.Ghayath Aljawady
• B.D.S, M.Sc., Ph.D in periodontics
• 2020-2021
• Department of:
• Oral and Maxillofacial surgery / Periodontics unit
• Department of:
After all of the necessary procedures are completed, the area is reexamined and cleansed, and the flap is placed in the desired position.
The flap should remain in this position without tension. It is convenient to keep the flap in place with light pressure by use a piece of gauze to allow the blood clot to form.
The purpose of suturing is to maintain the flap in the desired position until healing has progressed to the point at which sutures are no longer needed.
Many types of sutures, suture needles, and materials are available. Suture materials may be either non resorbable or resorbable, and they may be further categorized as braided or monofilament.
The resorbable sutures have gained popularity because they enhance patients' comfort and eliminate suture removal appointments.
The monofilament type of suture alleviates the “wicking effect” of braided sutures that may allow bacteria from the oral cavity to be drawn through the suture to the deeper areas of the wound.
The braided silk suture was the most common non resorbable suture used in the past because of its ease of use and low cost.
The expanded polytetrafluoroethylene, synthetic, monofilament suture is an excellent non resorbable suture that is widely used today.
The needle is held with the needle holder, and it should enter the tissues at right angles and be no less than 2 to 3 mm from the incision. The needle is then carried through the tissue, where it follows the needle's curvature. The knot should not be placed over the incision.
Suturing Techniques
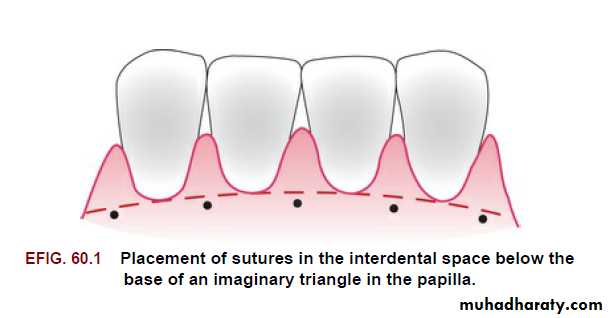
Sutures of any type that are placed in the interdental papillae should enter and exit the tissue at a point located below the imaginary line that forms the base of the triangle of the interdental papilla.
Two types of interdental ligation can be used: the direct loop suture and the figure-eight suture.
With the figure eight suture, thread is placed between the two flaps.
This suture is used when the flaps are not in close apposition as a result of apical flap position or non scalloped incisions.
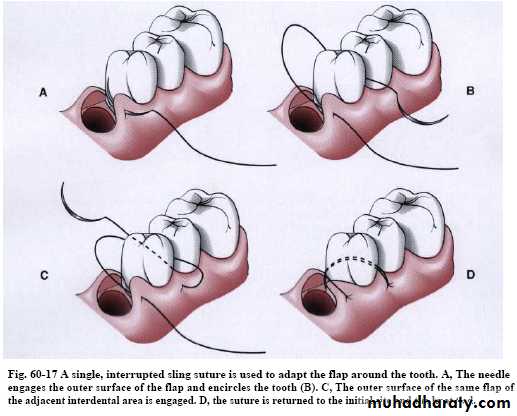
Interrupted interdental suture
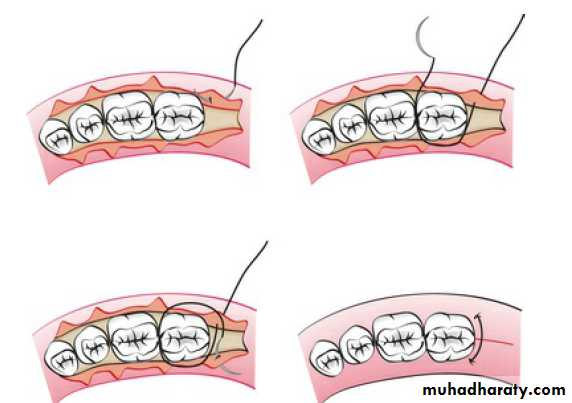
The sling ligation can be used for a flap on one surface of a tooth that involves two interdental spaces.
Suspensory (sling) suture
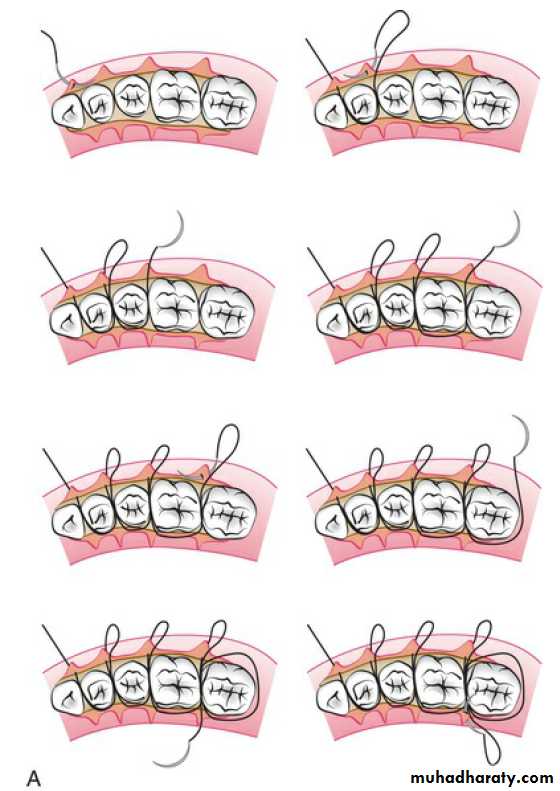
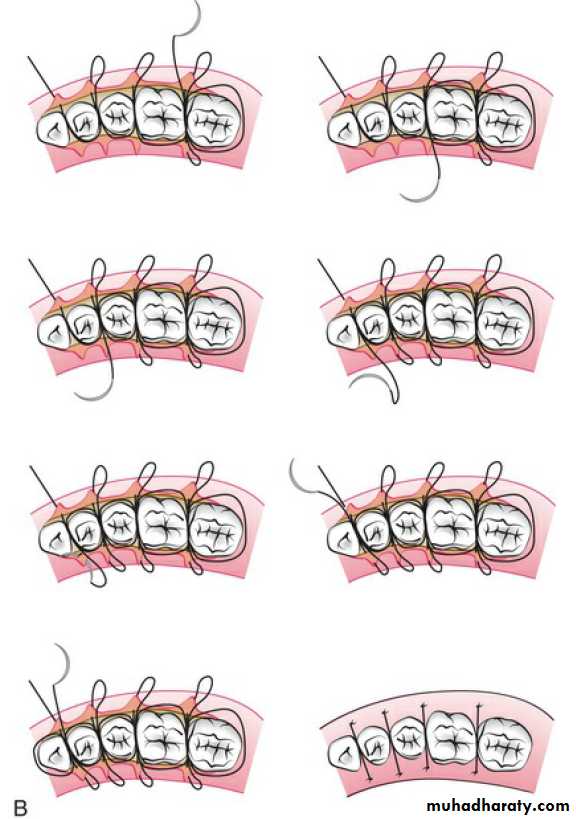
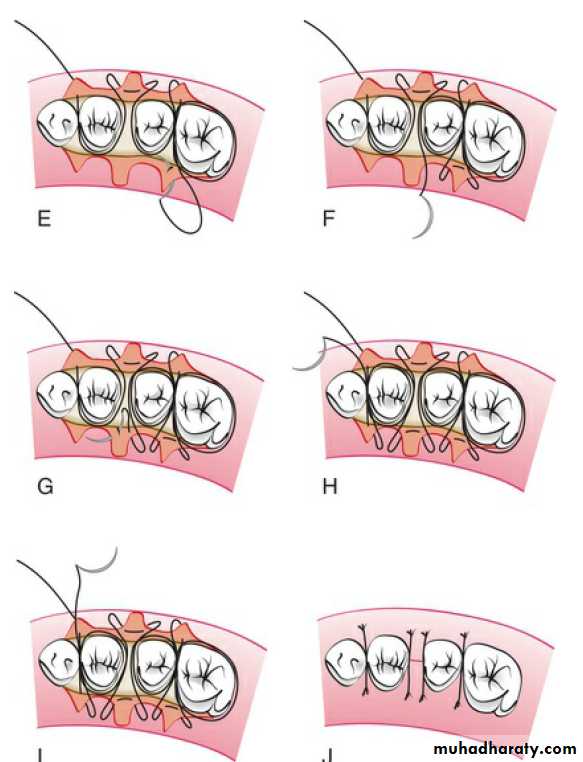
A sling suture is used when both a facial flap and a lingual flap are used and when they involve many teeth.
The continuous, independent sling suture is initiated on the facial papilla closest to the midline because this is the easiest place to position the final knot.
A continuous sling suture is laced for each papilla on the facial surface.
Continuous, independent sling suturing is especially appropriate for the maxillary arch. This is true because the palatal gingiva is attached and fibrous, whereas the facial tissue is thinner and mobile.
Continuous suture
The horizontal mattress suture is often used for interproximal areas of diastemata or for wide interdental spaces to adapt the interproximal papilla properly against the bone. Two sutures are often necessary.
The horizontal mattress suture can be incorporated with the continuous, independent sling sutures
Horizontal Mattress Suture:
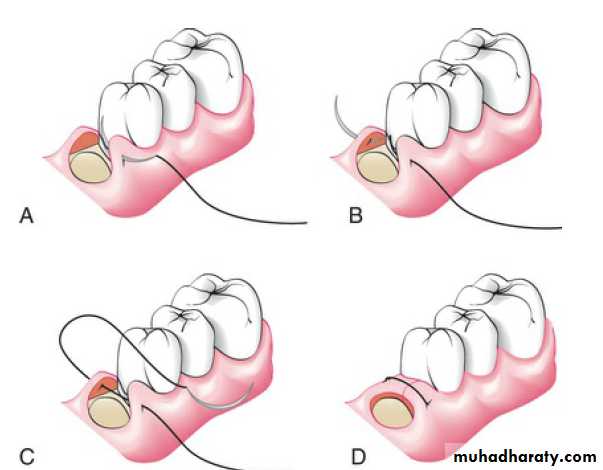
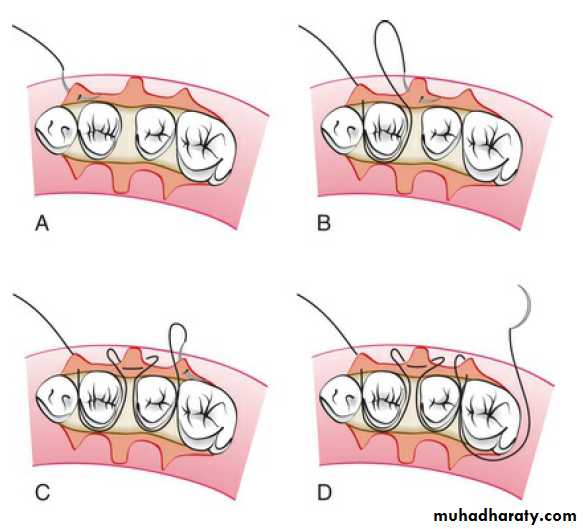
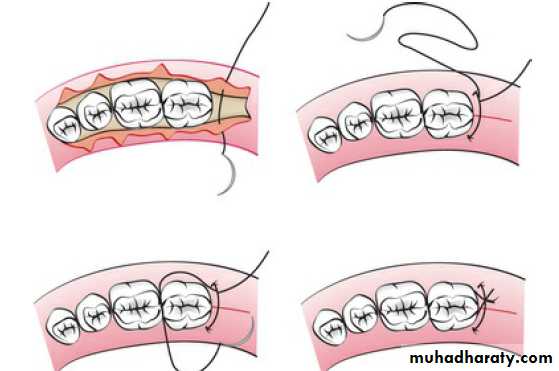
The closing of a flap mesial or distal to a tooth, as in the mesial or distal wedge procedures, is best accomplished by the anchor suture.
This suture closes the facial and lingual flaps and adapts them tightly against the tooth.
The needle is placed at the line–angle area of the facial or lingual flap adjacent to the tooth, anchored around the tooth, passed beneath the opposite flap, and tied.
The anchor suture can be repeated for each area that requires it
Anchor Suture
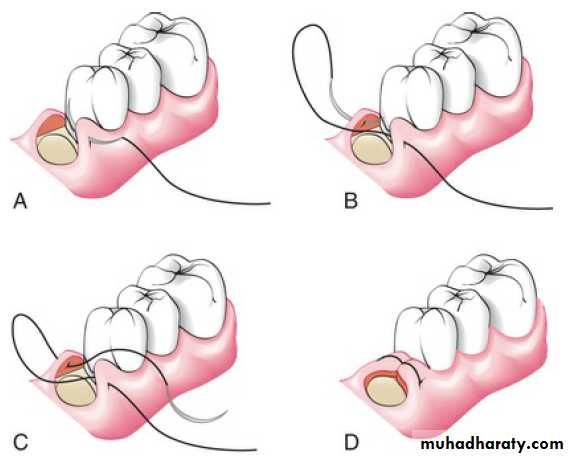
Another technique to close a flap that is located in an edentulous area mesial or distal to a tooth consists of tying a direct suture that closes the proximal flap, carrying one of the threads around the tooth to anchor the tissue against the tooth, and then tying the two threads.
Closed-Anchor Suture
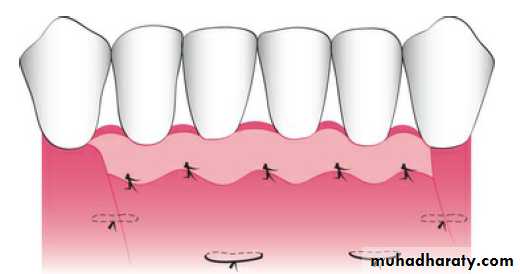
The periosteal suture is used to hold the apically displaced partial thickness flaps on the periosteum.
The two types of periosteal sutures are the holding suture and the closing suture.
The holding suture is a horizontal mattress suture that is placed at the base of the displaced flap to secure it into the new position.
Closing sutures are used to secure the flap edges to the periosteum.
Periosteal Suture
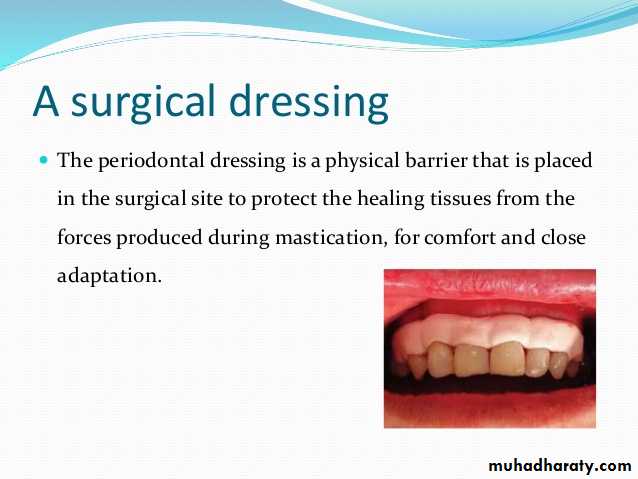
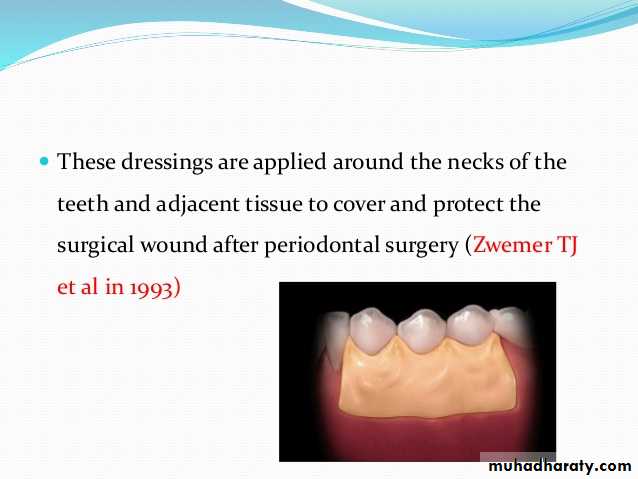
At completion of the periodontal surgical procedure, clinicians may elect to cover the area with a surgical dressing. In general, dressings have no curative properties but assist healing by protecting the tissue rather than providing “healing factors.
The dressing minimizes the likelihood of postoperative infection,
Facilitates healing by preventing surface trauma during mastication,
And protects the patient from pain induced by contact of the wound with food or with the tongue during mastication
Periodontal Dressings (Periodontal Packs)
Eugenol-based dressing –Gingivectomy due to-obtunding pain and sites less sensitive.
Zinc oxide- eugenol dressings prevent or retard bacterial growth (antiseptic properties)Irritate oral mucosal tissue.
Allergic reactions-tissue necrosis(bone)-↓ healing.
Difficulties in manipulation.
Rough surface after setting.
Histologic evidence -↑ inflammatory cell infltration and connective tissue response.
Eugenol has proven to be cytotoxic effect on fibroblasts and osteoblasts- like cells.
Advantages and Disadvantages
Non- eugenol dressing are currently the most widely used periodontal dressing: commercially available non-eugenol include:
Coe- Pack.
Cross Pack.
Peripac.
Septopack.
Perio Care.
Perio Putty.
Periogenix.
Non-Eugenol Dressing
Minimal irritation of the mucous membrane.
Pleasant odor.Neutral taste.
Ease of manipulation.
Pliability- easy removal from under cut areas.
Elimination of the objectionable taste of eugenol.
They are less irritating.
Form a closely adapted adhesive barrier to saliva and oral bacteria.
Advantages of non eugenol Dressing
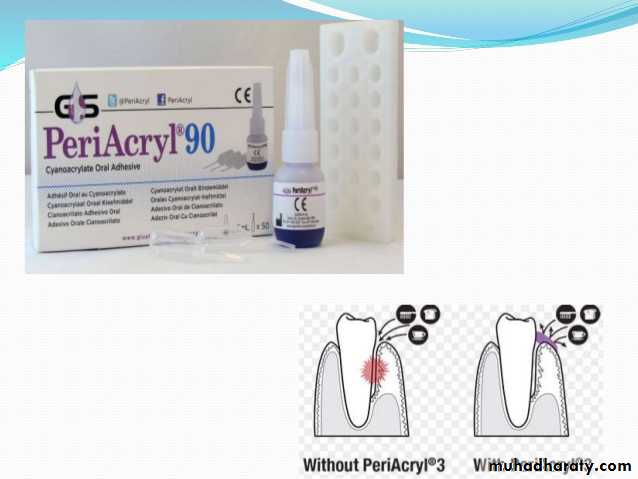
cyanoacrylates dressing.
light cure dressing.
Collagen dressing .
Mucoadhesive dressing.
Tissue conditioners (methacrylate gels).
Dressing containing neither Zinc oxide Nor eugenol
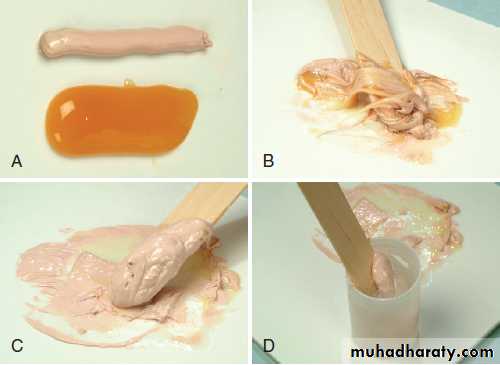
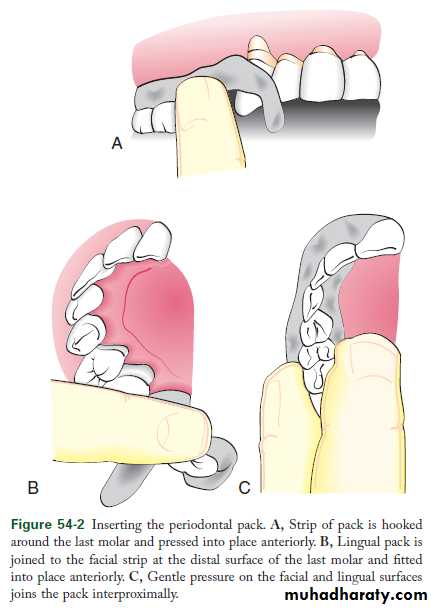
Inserting the periodontal pack. A, Strip of pack is hooked around the last molar and pressed into place anteriorly. B, Lingual pack is joined to the facial strip at the distal surface of the last molar and fitted into place anteriorly. C, Gentle pressure on the facial and lingual surfaces joins the pack interproximally.