
By:
Assist Prof. Saba Hazim Hasan
.أ
م صبا حازم حسن
UNIVERSITY OF MOSUL
COLLEGE OF DENTISTRY
2020-2021
Department of
Pedodontics,
Orthodontics
and Preventive
Dentistry
Department of:
HERE
Pedodontics
5th academic year

U N I V E R S I T Y O F M O S U L
C O L L E G E O F D E N T I S T R Y
Department of:
HERE
A pulpectomy involves complete pulp tissue removal from the crown and root and
is indicated when no vital tissue remains. It is also indicated when root maturation
is complete and the permanent restoration requires a post buildup. In the absence of
inflammatory root resorption, treatment is to obturate the canal with gutta-percha.
One of the greatest challenges facing the clinician is the treatment of a nonvital
immature permanent tooth with an open apex. Physiologic root maturation cannot
occur without the presence of vital pulp tissue, apical papilla stem cells,
odontoblasts, and Hertwig epithelial root sheath. Traditional treatment for these
cases was an apexification procedure wherein CaOH was carried to the root apex
to contact vital tissues directly. The CaOH stimulated the formation of a cementoid
barrier against which gutta-percha could subsequently be condensed. Multiple visits
over a period of 9 to 18 months were required, however, and the outcome was a
shortened root with thin walls. Additionally, long-term CaOH therapy has been
shown to weaken the tooth root and increase the likelihood of root fractures.
U N I V E R S I T Y O F M O S U L
C O L L E G E O F D E N T I S T R Y
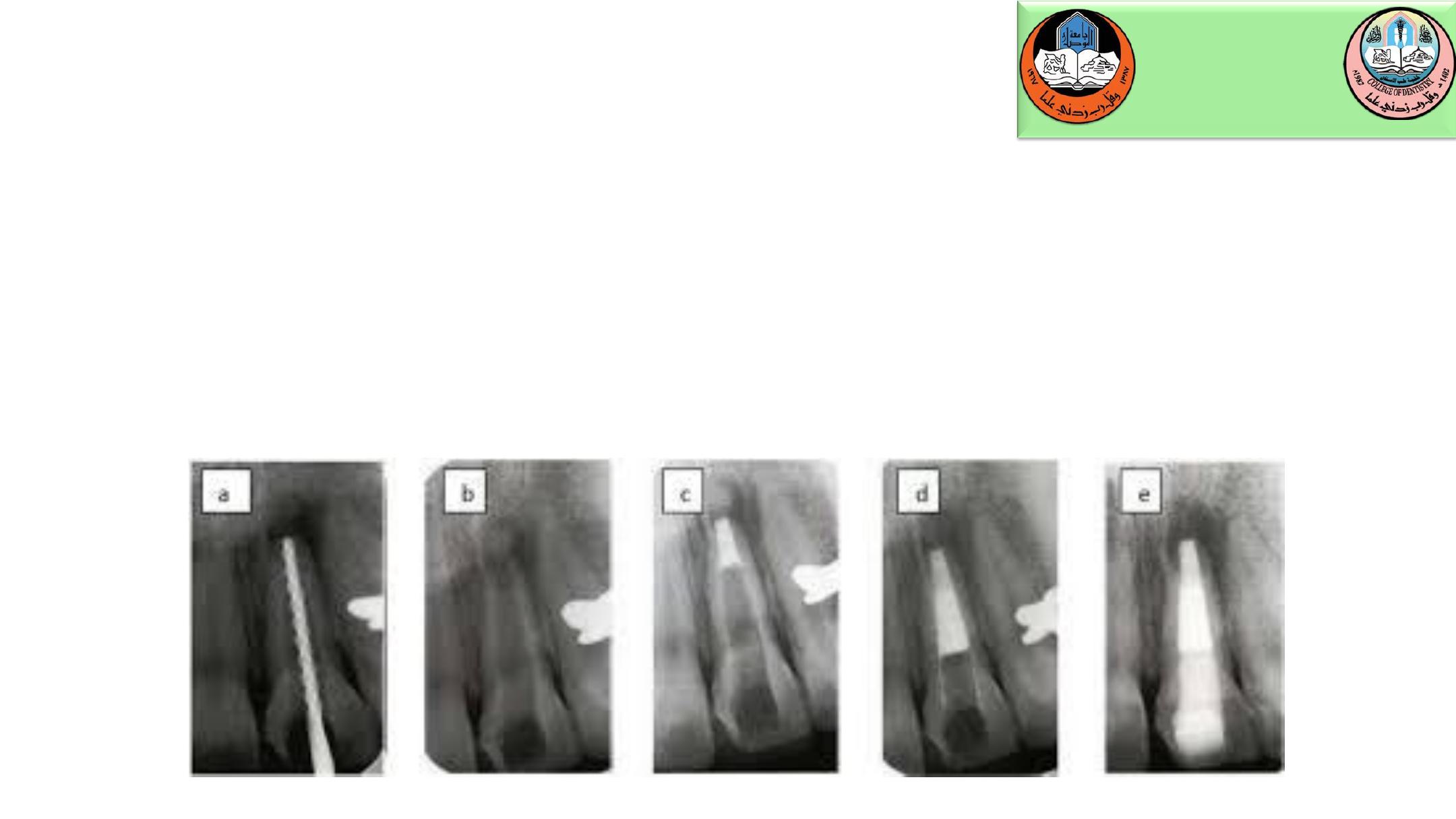
An alternative to the CaOH apexification technique for managing devitalized
immature incisors is the apical barrier technique using MTA. The material is
condensed into the apical area, and allowed to set. Gutta-percha is then condensed
against the MTA barrier at a subsequent appointment. Though overall treatment
time is greatly reduced, the shortened root and thin walls continue to place the
tooth at risk for subsequent cervical root fracture.

U N I V E R S I T Y O F M O S U L
C O L L E G E O F D E N T I S T R Y
Department of:
HERE
Regenerative Endodontics
An alternative to apexification of necrotic immature teeth termed
revascularization or “regenerative” endodontics. These procedures seek to
replace damaged dentin, root structures, and pulp cells with live tissues that
restore normal physiologic function. The concept is to thoroughly disinfect the
root canal system and then stimulate bleeding from the apical papilla to fill the
root chamber with a blood clot. A host of growth factors in the area then act on
dental stem cells, primarily from the apical papilla, to use the clot as a scaffold
and differentiate into healthy cells of the pulp-dentin complex that can complete
physiologic root maturation.

U N I V E R S I T Y O F M O S U L
C O L L E G E O F D E N T I S T R Y
Department of:
HERE
Regenerative Endodontics
The technique is to first cleanse the canal by copious irrigation with sodium
hypochlorite or Ethylenediaminetetraacetic acid (EDTA). Owing to the immature
status of the root and thin radicular walls, instrumentation is kept to a minimum
and used mainly to agitate the irrigant. The irrigant is also activated by placing
an ultrasonic tip about 3 mm short of the working length in the canal to facilitate
better debridement of the pulp tissue remnants and to minimize the substrate for
microbial proliferation. The canal space is then dried using sterile paper points.
A triple antibiotic mix of 250 mg ciprofloxacin, 250 mg metronidazole, and 150
mg clindamycin is prepared to a creamy paste with propylene glycol as a
vehicle. The antibiotic paste is carefully placed into the root canal system using a
Lentulo spiral up to the cementoenamel junction (CEJ). The access cavity is
sealed with a sterile cotton pellet and glass ionomer cement.
U N I V E R S I T Y O F M O S U L
C O L L E G E O F D E N T I S T R Y
Department of:
HERE
Regenerative Endodontics
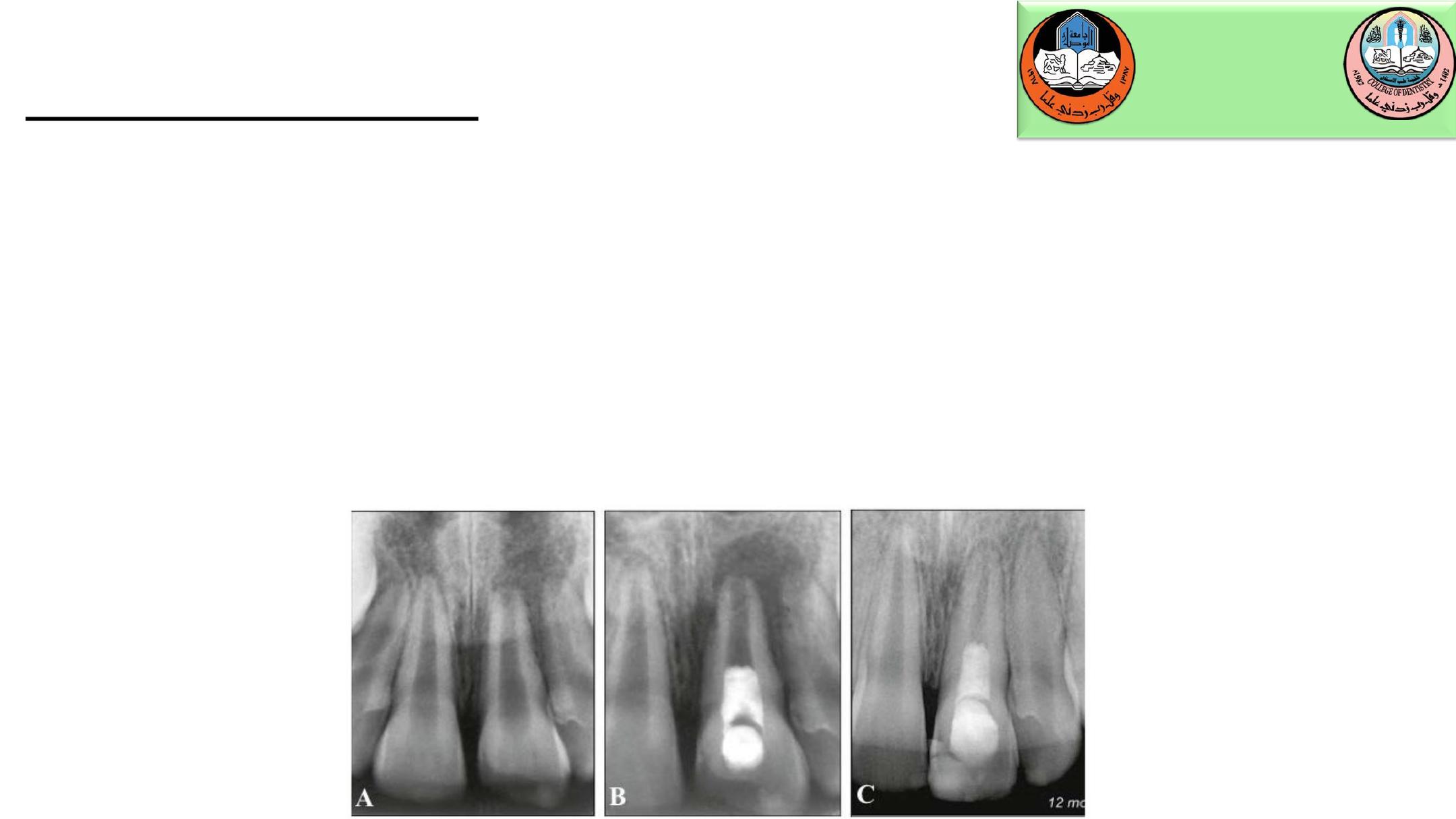
The patient is scheduled for follow-up appointments after 3 to 4 weeks. At the
follow-up appointment, the area is anesthetized with local anesthetic containing
no epinephrine. The antibiotic paste is rinsed out, and a sterile endodontic file is
placed beyond the apex to initiate bleeding. A clot is allowed to form as close to
the CEJ as possible to facilitate root thickening at the tooth cervix. MTA is then
placed against the clot, and the tooth is temporarily sealed with glass ionomer
cement. The final restoration is placed at a subsequent appointment. Root
maturation should be apparent radiographically within several months
U N I V E R S I T Y O F M O S U L
C O L L E G E O F D E N T I S T R Y
Department of:
HERE
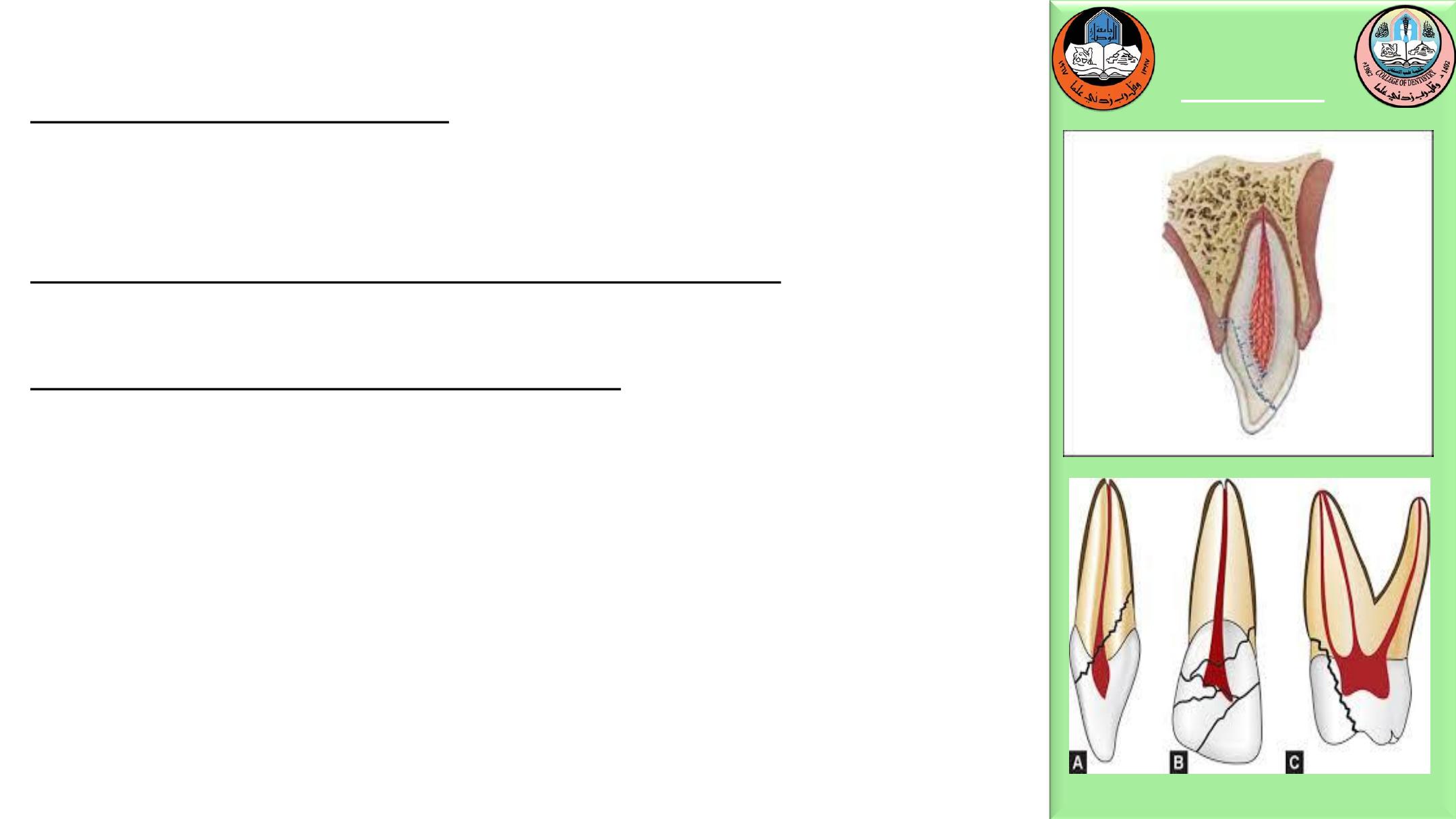
Crown/Root Fracture
Without pulp exposure:
fragment removal with or without gingivectomy and
restore.
With pulpal exposure and immature roots:
Perform a partial pulpotomy to preserve pulp vitality.
Pulp exposure with mature roots:
Perform endodontic treatment then restore with a
postretained crown.
Orthodontic or surgical extrusion of apical fragment
may be indicated to expose the margins prior to
permanent restoration.
Extraction is inevitable in crown root fractures with a
severe apical extension, the extreme being a vertical
fracture

020-2021
U N I V E R S I T Y O F M O S U L
C O L L E G E O F D E N T I S T R Y
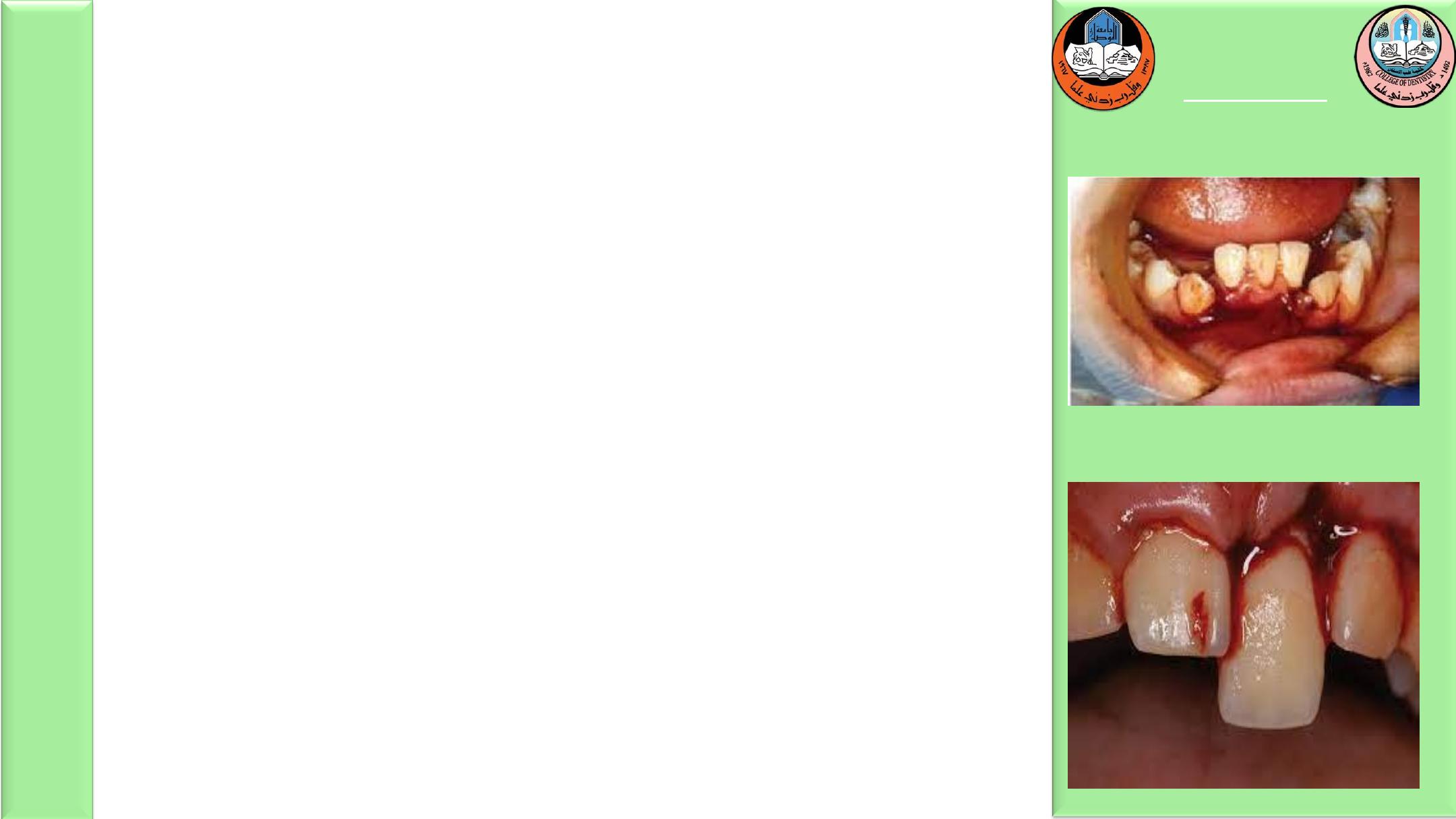
Root fracture
If the coronal fragment is stable and immobile (high
apical root fracture), no treatment is indicated. If the
coronal fragment is mobile, reposition and stabilize the
fragment with rigid splinting of composite resin and wire
or orthodontic appliances for 3 to 4 weeks ;. If the root
fracture is near the cervical area of the tooth, stabilization
is beneficial for a longer period of time (3-4 months).

020-2021
U N I V E R S I T Y O F M O S U L
C O L L E G E O F D E N T I S T R Y
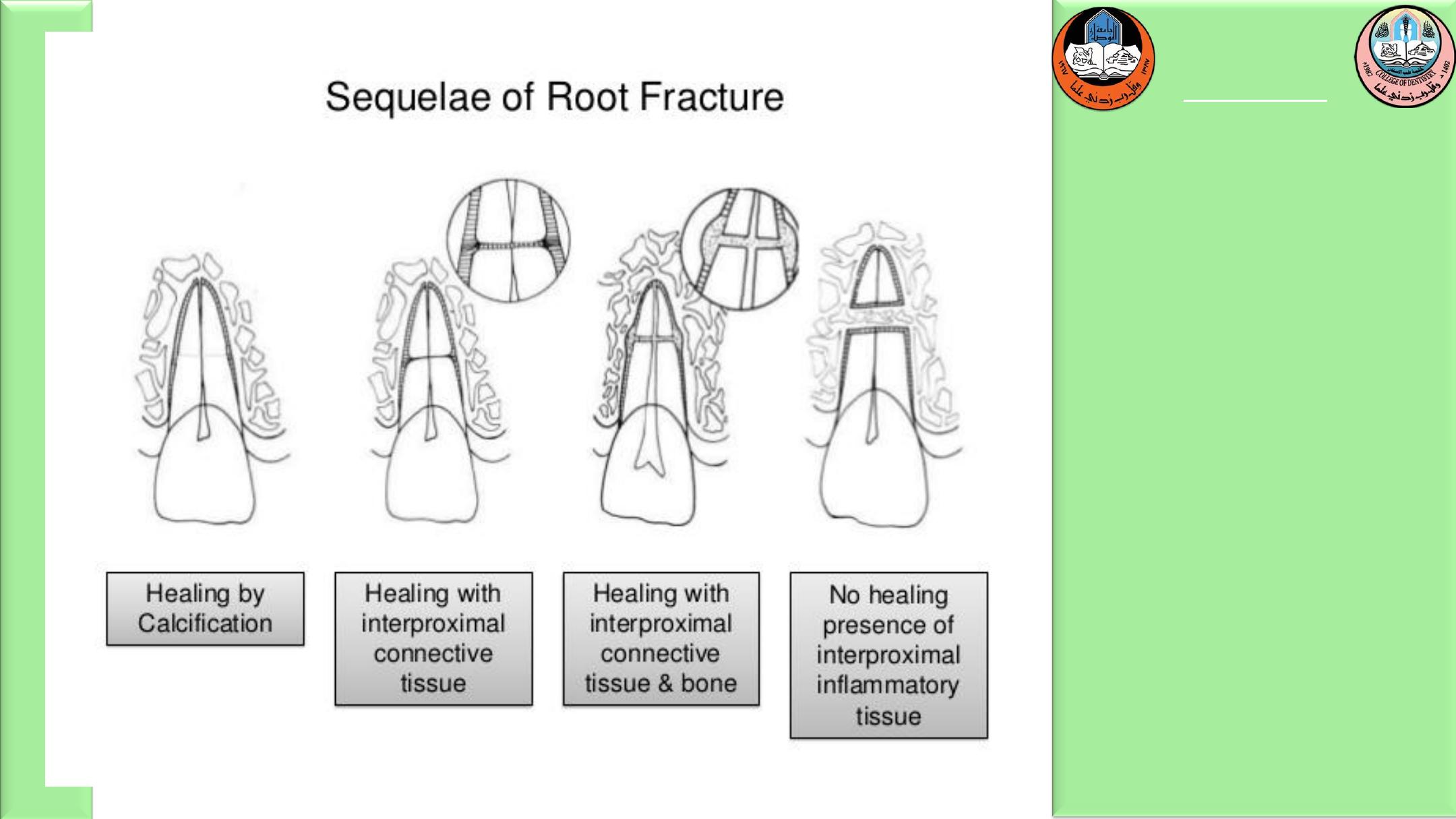
Root canal therapy should not be initiated until clinical
and radiographic signs of necrosis or resorption are
apparent. Even in those cases, treatment can often be
limited to the coronal fragment, because in most
instances the apical fragments maintain their vitality.
U N I V E R S I T Y O F M O S U L
C O L L E G E O F D E N T I S T R Y
Department of:
HERE
U N I V E R S I T Y O F M O S U L
C O L L E G E O F D E N T I S T R Y
Department of:
HERE
Alveolar fracture
Reposition any displaced segment and then splint
the involved teeth with a flexible splint for 4
weeks. Suture gingival laceration if present.
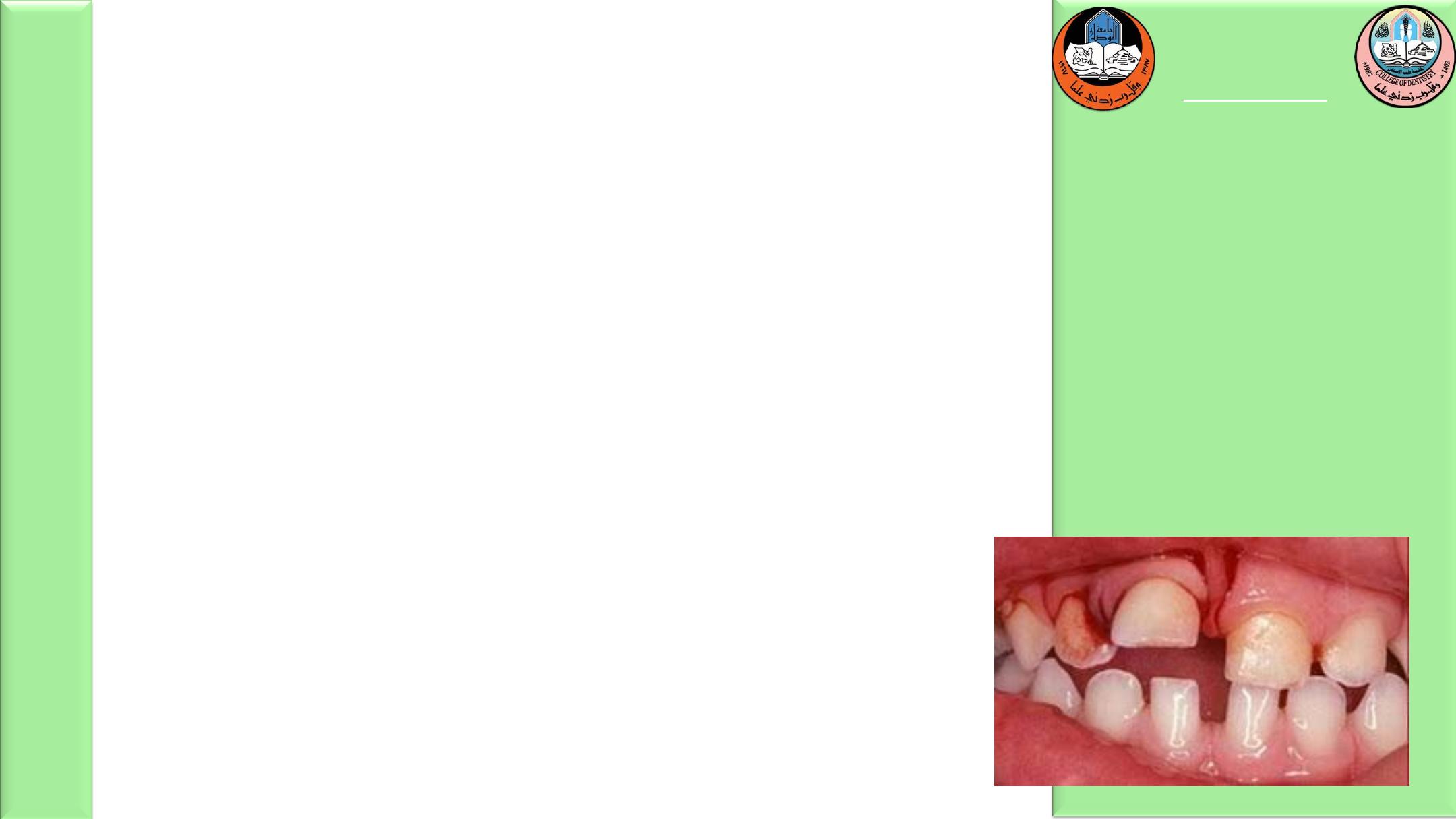
Extrusive luxation
Extruded permanent teeth should be repositioned as
soon as possible and splinted for 2 to 3 weeks. It
normally takes the PDL fibers this period of time to
reanastomose. Extruded permanent teeth with closed
apices will undergo pulpal necrosis; therefore root canal
therapy should be initiated after the teeth are splinted.
Extruded teeth with open apices have a chance to
revascularize and maintain their vitality, so the decision
to initiate therapy should be delayed until clinical or
radiographic signs indicate necrosis.
U N I V E R S I T Y O F M O S U L
C O L L E G E O F D E N T I S T R Y
Department of:
HERE
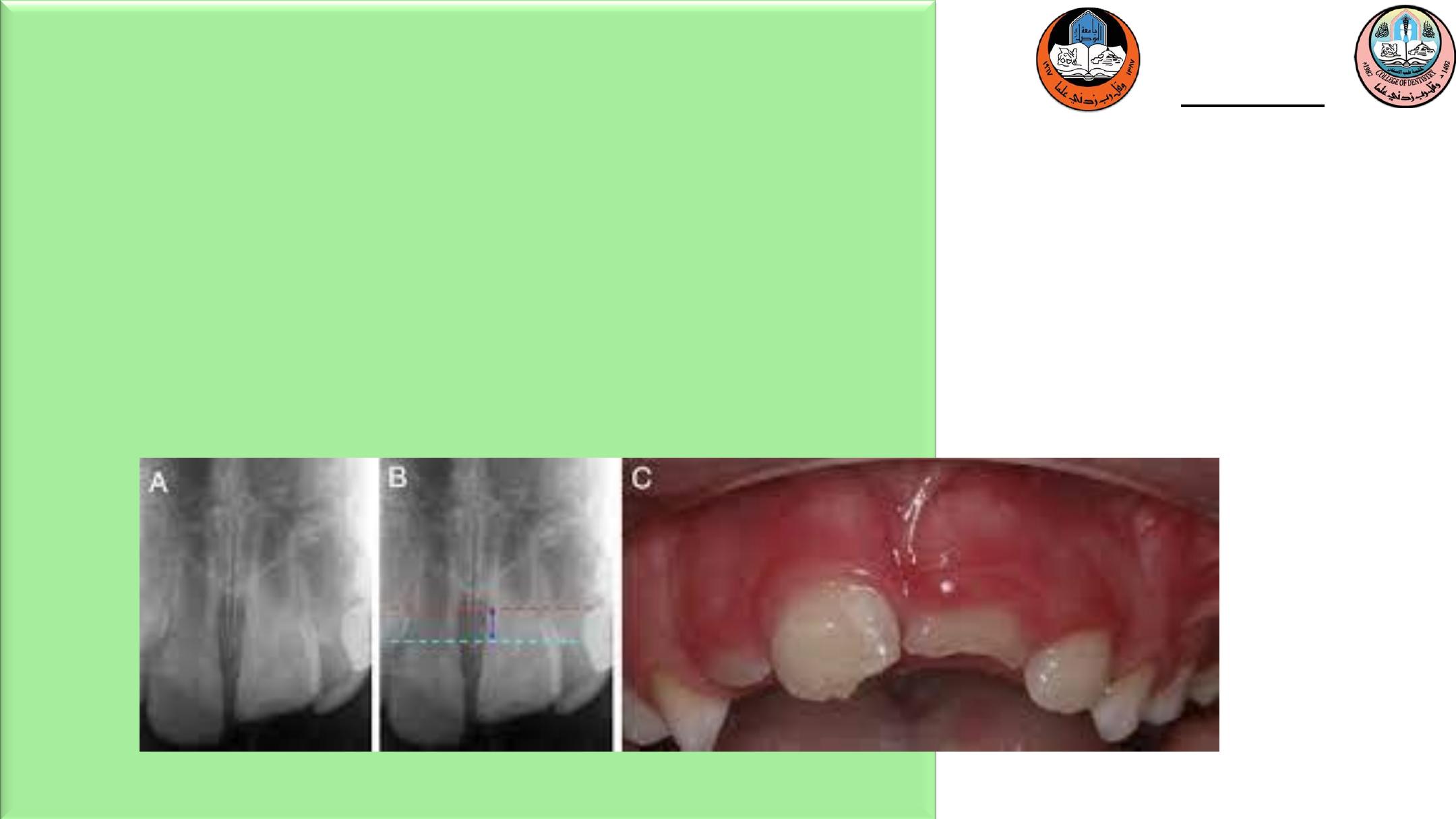
Lateral luxation
Alveolar bone fractures frequently occur in lateral
luxation
injuries
and
can
complicate
their
management. In the most severe cases, PDL and
marginal bone loss occur. Treatment is to reposition
the teeth and alveolar fragments as soon as possible. A
splint should then be applied for 3 to 6 weeks,
depending on the degree of bone involvement. If the
apices are closed, the pulps will likely become
necrotic. Again, teeth with open apices should be
monitored until signs of necrosis are evident.
020-2021
U N I V E R S I T Y O F M O S U L
C O L L E G E O F D E N T I S T R Y
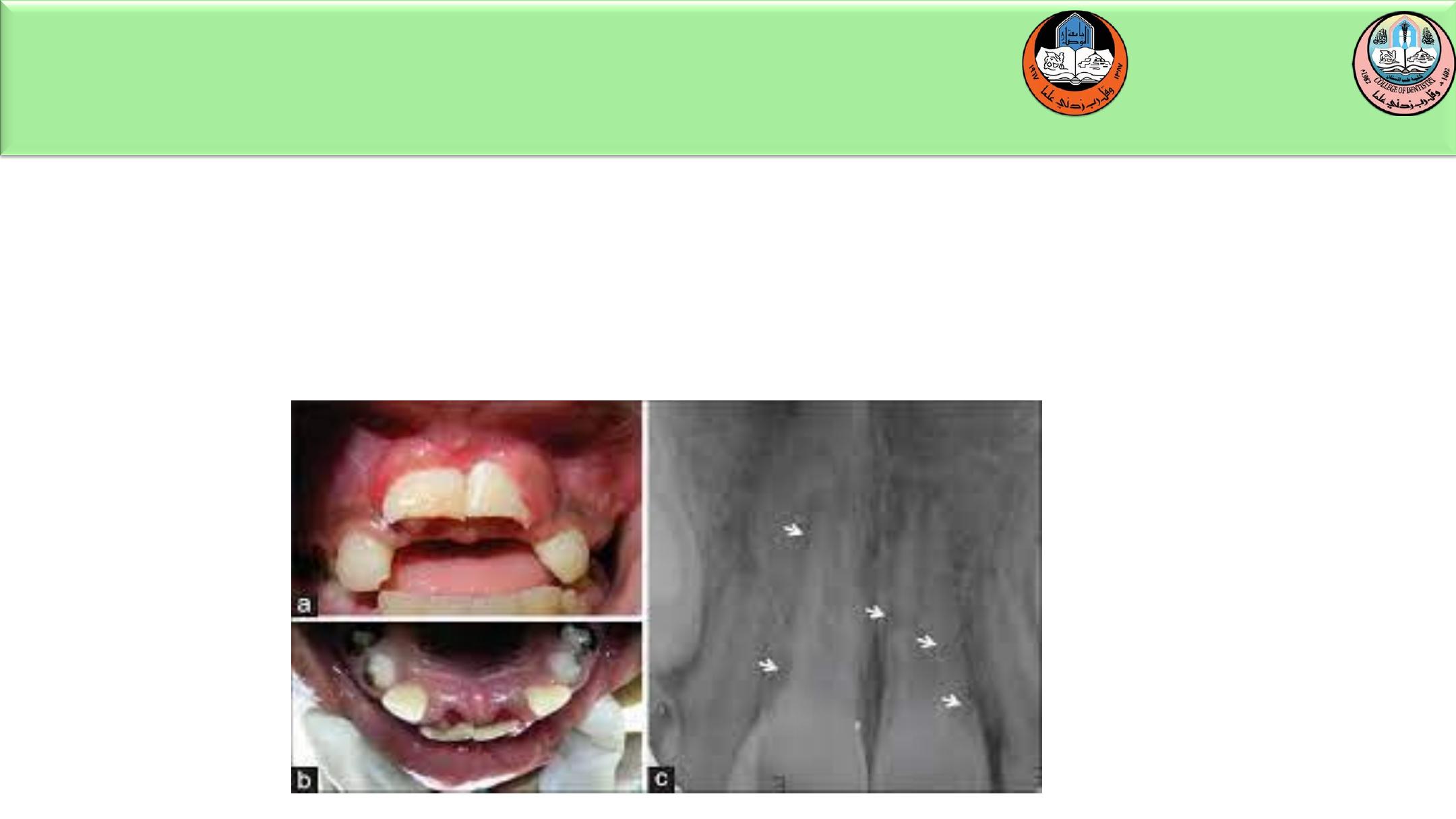
Intrusive luxation
Teeth with incomplete root formation:
If the crown remain visible and there is very wide
immature apex (>2mm ) the tooth may be allowed to
re-erupt spontaneously . If no movement is noted
within 3 weeks, orthodontic repositioning using light
forces should be employed.
U N I V E R S I T Y O F M O S U L
C O L L E G E O F D E N T I S T R Y
Department of:
HERE
Mature permanent teeth intruded less than 3 mm should be allowed to
reemerge without intervention. If no movement is noted within 3 weeks they
should be repositioned surgically or orthodontically before they ankylose.
Those teeth intruded beyond 7 mm should be repositioned surgically
U N I V E R S I T Y O F M O S U L
C O L L E G E O F D E N T I S T R Y
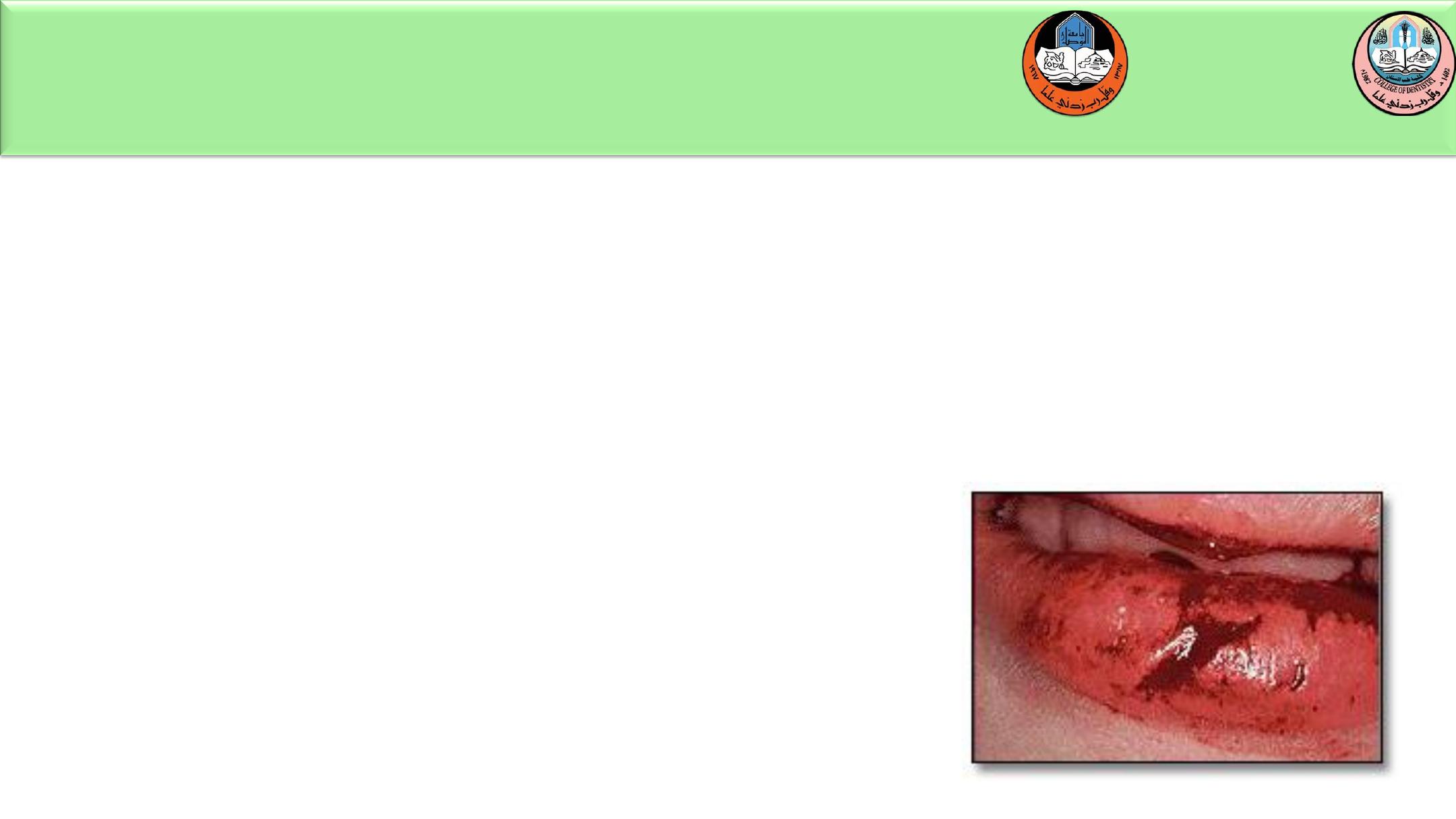
Soft Tissue Trauma
Lips often cushion the teeth during a fall, bearing the
brunt of the injury and resulting in bruises and
lacerations. If a laceration is present, it should be
carefully examined to determine whether a foreign
object such as a tooth fragment or gravel has been
introduced into the wound.
:
HERE
U N I V E R S I T Y O F M O S U L
C O L L E G E O F D E N T I S T R Y
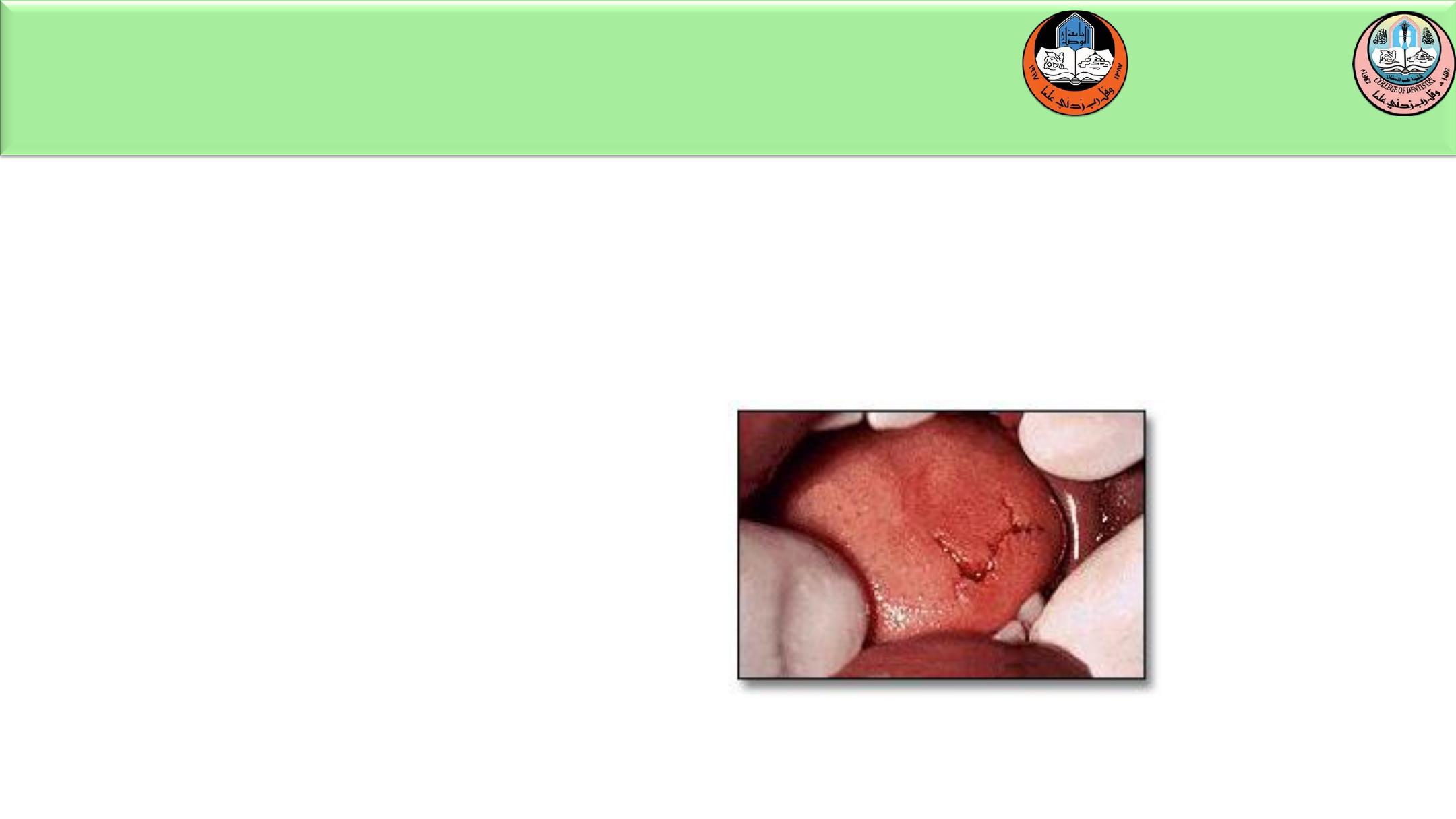
Trauma to the tongue can result in laceration or puncture.
Careful examination of the injury is important since the
necessity for suturing is dependent on the extent of injury.
U N I V E R S I T Y O F M O S U L
C O L L E G E O F D E N T I S T R Y
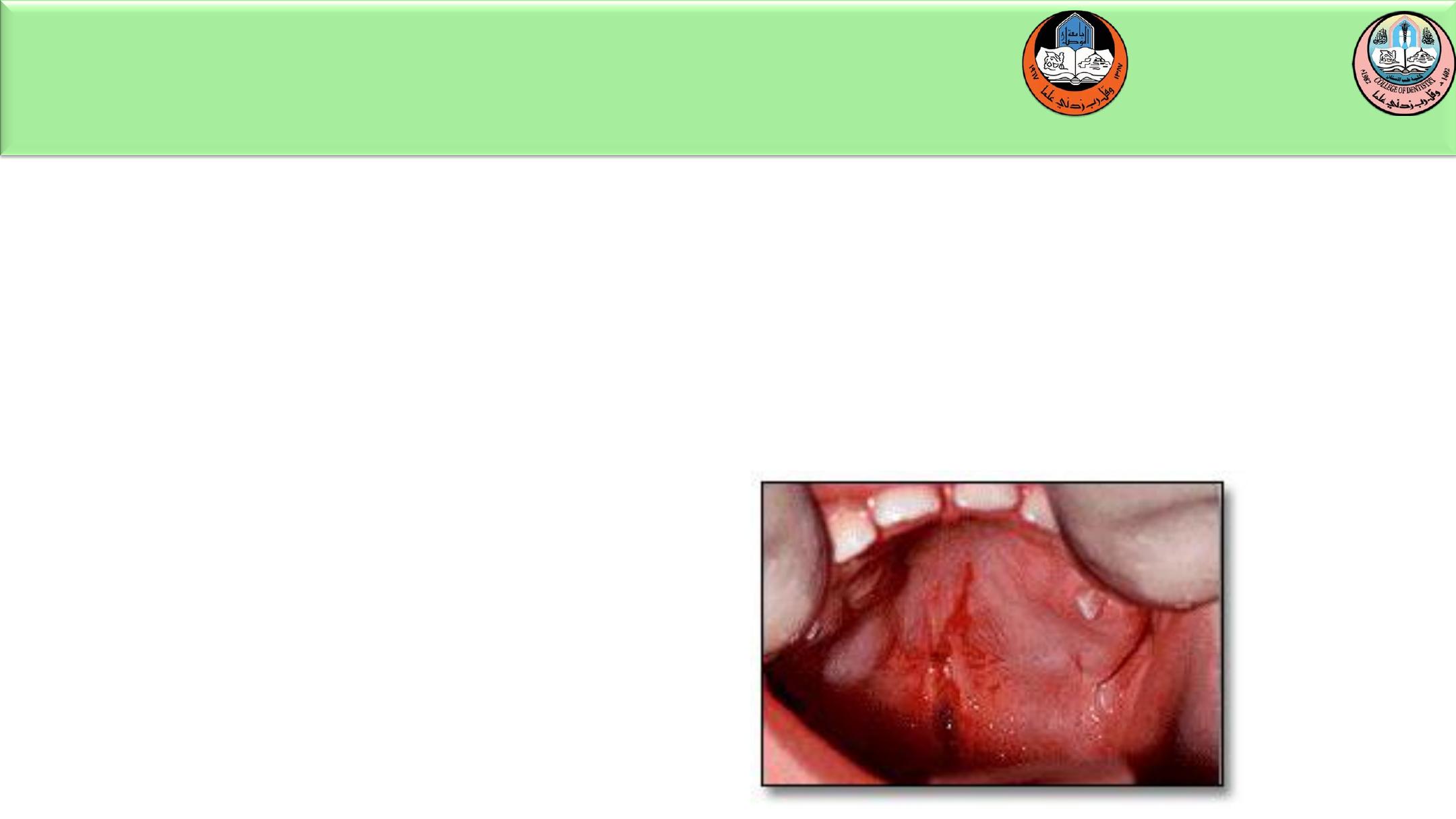
Impalement of the soft palate is commonly found in the child who falls while
holding an object in the mouth, i.e., a stick, pencil or pen, straw or
toothbrush. Most impalement injuries heal spontaneously and do not require
treatment, however the area should be thoroughly explored for foreign body
objects and a prophylactic antibiotic should be prescribed to avoid infection
complications.

THE END
U N I V E R S I T Y O F M O S U L
C O L L E G E O F D E N T I S T R Y
2020-2021
