By Dr Dhafer A. Alghezi Ph. D. Cancer research
Cancer andImmune System
Introduction
Neoplasia (Neo= new; plasia= growth) means new growth.A neoplasm is a type of abnormal and excessive growth of tissue. The growth of a neoplasm is uncoordinated with that of the normal surrounding tissue, and persists in growing abnormally, even if the original trigger is removed.
Oncology (oncos=tumor, logos=study) is the branch of science dealing with the study of neoplasms or tumors.
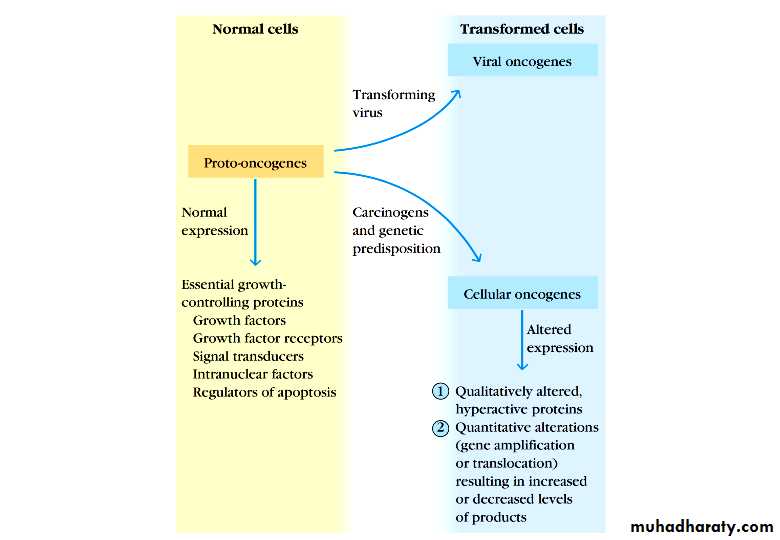
Proto-oncogenes: normal cellular genes whose products promote cell proliferation.
Oncoprotein: a protein encoded by an oncogene that drives increased cell proliferation through one of several mechanisms.Oncogenes: mutated or overexpressed versions of proto-oncogenes that function autonomously, having lost dependence on normal growth promoting signals
Nomenclature
All tumors, benign as well as malignant, have two basic componentsNeoplastic cells constitute the tumor parenchyma
Supportive stroma is composed of fibrous connective tissue and blood vessels; it provides the framework on which the parenchymal tumor cells grow.
Classifications of neoplasms
based on their parenchymal components.Benign when they are slow-growing and localised without causing much difficulty to the host.
Malignant when they proliferate rapidly, spread throughout the body and may eventually cause death of the host. The common term used for all malignant tumors is cancer.
The suffix ‘-oma’ is added to denote benign tumors. Malignant tumors of epithelial origin are called carcinomas, while malignant mesenchymal tumors are named sarcomas (sarcos = fleshy).
Benign
MalignantTumor
Classification of neoplasms
Epithelial tumorsBenign forms – adenoma , papilloma
Malignant forms – carcinoma, e. g adenocarcinoma , squamous cell carcinoma
Mesenchymal tumors
Benign forms – fibroma, leiomyoma.
Malignant forms – sarcoma, e. g fibrosarcoma, leiomyosarcoma
Except
Melanoma: Carcinoma of the melanocytes
Hepatoma: Carcinoma of the hepatocytes
Lymphoma: Malignant tumor of the lymphoid tissue
Seminoma: Malignant tumor of the testis.
Leukaemia: Cancer of blood forming cells.
Differentiation
Rate of growthMetastasis
Local invasion
Benign
Vs
Malignant
Differentiation
BenignMalignant
Well differentiated
Poorly differentiated
like tissue of origin
Does not like tissue of origin
Rate of grow
Benign
Malignant
Slow growing
Fast growing
Local invasion
BenignMalignant
NOT invade
Invade the surrounding tissue
Surrounding by fibrous capsule
Not capsulated
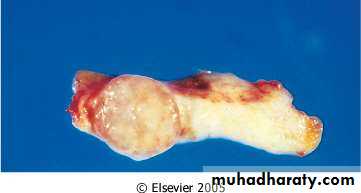
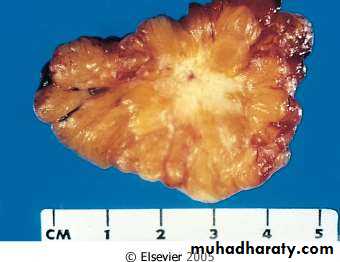
• Gross (macroscopic features of two breast neoplasms)
• Benign – circumscribed, often encapsulated, pushes normal tissue aside
• Malignant – infiltrative growth, no capsule, destructive of normal tissues
•
Metastasis
BenignMalignant
NOT metastasized
Metastasized
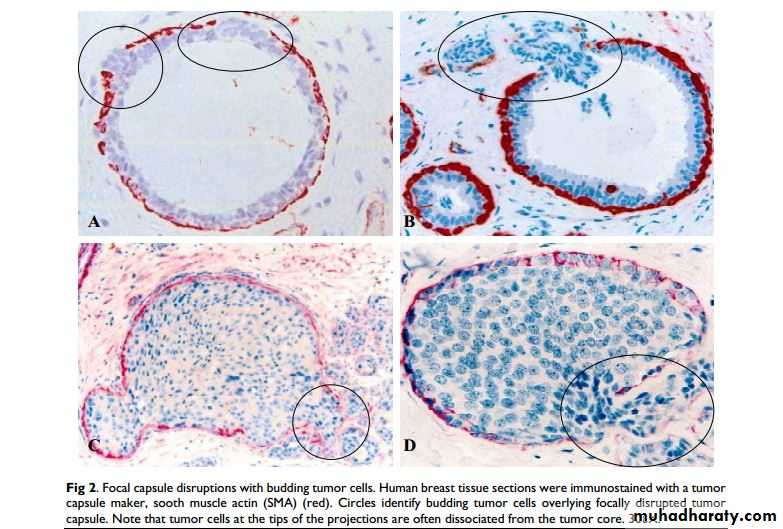
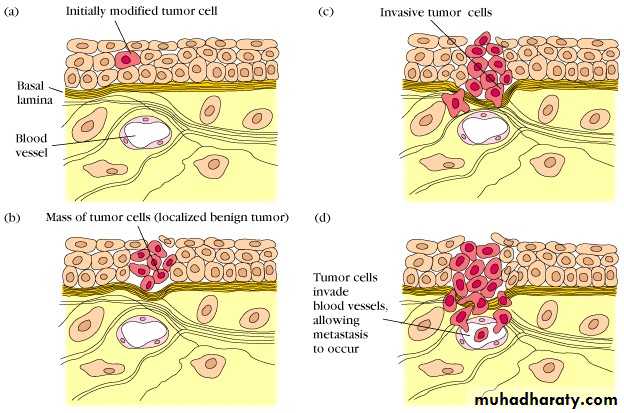
It is defined by the spread of a tumor to sites that are physically discontinuous with the primary tumor, and unequivocally marks a tumor as malignant.
The invasiveness of cancers permits them to penetrate into blood vessels, lymphatics, and body cavities, providing the opportunity for spread.
Etiology Of Tumor
• 1) Inherited :• Expression of inherited oncogene
• e.g. viral gene incorporated into host gene
• 2) Viral:
• - Human papilloma, herpes type 2, HBV, EBV (DNA)
• - Human T-cell leuckemia virus (RNA)
• 3) Chemical:
• - Poly cyclic hydrocarbons cause sarcomas
• - Aromatic amines cause mammary carcinoma
• - Alkyl nitroso amines cause hepatoma
• 4) Radiological: Ultraviolet & ionizing irradiation
• 5) Spontaneous: failure in the cellular growth control
Tumor Associated Antigens
!) Viral Antigen:
a- Viral proteins and glycoproteins
b- New antigens produced by virally infected host
cells under control of viral nucleic acid
2) Tumor specific antigens:
- Tumor cells develop new antigen specific totheir carcinogens
3) Tumor specific transplantation antigens:
- Tumor cells express new MHC antigens due toalteration of normally present MHC antigens
4) Oncofetal antigens:
a- Carcino-embryonic antigens (CEA)- Normally expressed during fetal life on fetal gut
- Reappearance in adult life:
GIT, pancreas, biliary system and cancer breast
b- Alpha fetoprotein:
- Normally expressed in fetal life- Reappearance in adult life; hepatoma
Immunosurveillance
The immune system continually surveyed the body for the presence of abnormal cells, which were destroyed when recognized.The immune system also played an important role in delaying the growth, or causing regression of established tumors.
This may be evident by:
• Many tumors contain lymphoid infiltrates.
• Spontaneous regression of tumors occurs (e.g melanomas, neuroblastomas )
• Tumors occur more frequently in the neonatal and in old age, when the immune system function less effectively.
• Tumors arise frequently in immunosuppressed individuals.
The term immune surveillance proposed that the immune response of normal individual regularly eliminates malignant cells, thereby preventing the establishment and growth of tumors.
The concept of immune surveillance state that the malignant disorders occur when there is a failure of the immune system to recognize and destroy tumors cells before they become established.
Tumor antigen
It is an antigenic substance produced in tumor cells, i.e., it triggers an immune response in the host.Tumorigenesis may lead to expression of new antigens or alteration in existing antigens that are found on normal cells.
These antigens may include membrane receptors, regulators of cell cycle and apoptosis, or molecules involved in signal transduction pathways.
Tumor antigens are useful tumor markers in identifying tumor cells with diagnostic tests and are potential candidates for use in cancer therapy.
Immunogenicity tumors
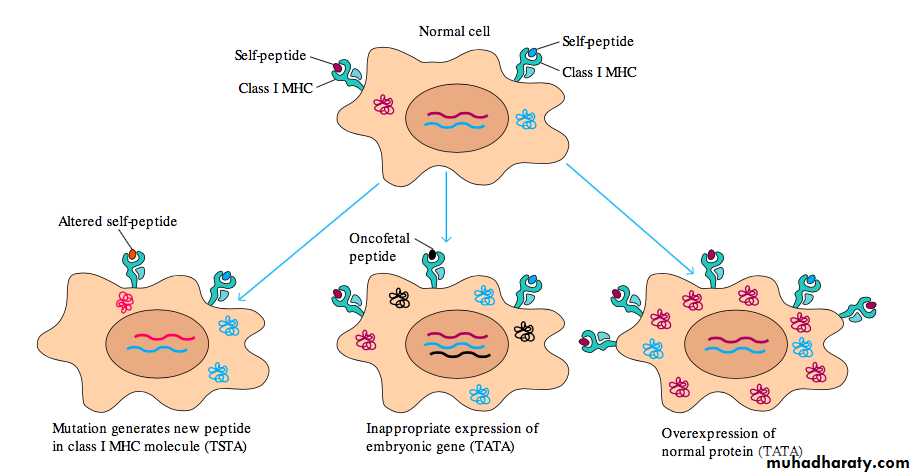
Two types of tumor antigensTumor specific antigens (TSTA)
Present only on tumor cells (usually viral induced) but not normal cells.
Tumor associated antigens (TAA)
Are more common and found on both tumor and normal cells during fetal life (oncofetal antigens) when the immune system is immature and unable to respond but that normally are not expressed in the adult ( or in low concentration).Examples: carcinoembryonic antigen (CEA), alpha-fetoprotein (AFP), and beta human chorionic gonadotropin, (β-HCG).
Carcino-embryonic antigen (CEA):
CEA is a glycoprotein normally synthesised in embryonic tissue of the gut, pancreas and liver.Their serum levels are high in cancers of the gastrointestinal tract, pancreas and breast.
CEA levels are also elevated in certain non-neoplastic conditions e.g. in ulcerative colitis, Crohn’s disease, hepatitis and chronic bronchitis.
Alpha-foetoprotein (AFP):
It is a glycoprotein synthesised normally by foetal liver cells.Their serum levels are elevated in hepatocellular carcinoma and non- seminomatous germ cell tumours of the testis.
Certain non- neoplastic conditions also have increased serum levels of AFP e.g. in hepatitis, cirrhosis, toxic liver injury and pregnancy.
Beta-human chorionic gonadotrophin
Beta-HCG is produced by the trophoblast epithelium of the placenta during pregnancy.
Detectable β-HCG in males or nonpregnant females indicates an underlying tumor.
Gonadal germ cell tumors, and adenocarcinomas of the ovary, pancreas, stomach, as well as hepatomas, produce this molecule.
Immune Surveillance System
This system include :1) Natural killer (NK) cells
They kill directly tumor cells,helped by interferon, IL-2
2) Cytotoxic T-cells
They also kill directly tumor cells3) Cell mediated T-cells (effector T-cells)
They produce and release a variety of lymphokines :a-Macrophage activation factor that activate macrophag
b-Gamma interferon and interleukin-2 that activate NK
c-Tumor necrosis factor (cachectine)
Immune Surveillance System
4) B-cells :
- Tumor associated antigens stimulate production of
specific antibodies by host B-cells
- These specific antibodies bind together on tumor cell surface
leading to destruction of tumor through:a- Antibody mediated-cytotoxicity :
killCytotoxic T-cells IgG-coated tumor cells
b- Activation of macrophages
releaseSensitized T-cells macrophage activating factor
IgG-coated tumor cells macrophages activate
c- Activation of classical pathway of complement leading to
Lysis of tumor cells
Tumor Escape
• Mechanisms by which tumor escape immune defenses:• 1) Reduced levels or absence of MHCI molecule on tumor so that they can not be recognized by CTLs
• 2) Some tumors stop expressing the antigens
• These tumors are called “antigen loss variants”
• 3) Production of immunosuppressive factors by tumor e.g. transforming growth factor (TGF-β)
• 4) Tumor antigens may induce specific immunologic tolerance
Tumor Escape
• 5) Tumor cells have an inherent defect in antigen processing and presentation
6) Ag shed from the tumor have been detected in human serum, these soluble Ags may saturate the receptors on T- or B- cells.
• 7) Antigens on the surface of tumors may be masked by sialic acid-containing mucopolysaccharides
8. Many tumors have the capacity to modulate their surface Ags, expressing different Ags if the original Ags have been recognized.
9. Lymphocytes that are sensitized to the tumor Ag may get trapped in the lymph nodes or lymph organ that drains the affected site. The shed Ags described earlier may be considered to be blocking factors.
Trapping the effector cells in the node, preventing them from entering the peripheral circulation.
10. Certain type of tumors tends to invade bone and cartilage has been shown to secrete collagenase, which causes lytic destruction of those components that would otherwise be impermeable to growth of a soft tissue.
11. Other tumor can secrete prostoglandins (PGs), which negatively regulate NK- and K-cells.
12. Tumors that produce substances that interfere with the production of IL1 by macrophages or IL2 by T-cell subsets would limit the overall responsiveness to tumors.