LEC3
د. علي الشالجيINTRACRANIAL SPACE OCCUPYING LESIONS
( I.C.S.O.L )CLASSIFICATION
Haematoma :1. EDH ( extradural haem. )
2. SDH ( subdural haem. )
3. ICH ( intracerebral haem. )
4. IVH ( intraventricular haem. )
● Infection :
1. Bact. : which could be Acute ( brain abscess ) or chronic ( Granuloma )2. Parasitic : hydatid cyst
3. Fungal
● Tumour : Primary or Secondary .
General signs and symptoms of increased intracranial pressure
A- HeadacheThe most common complaint of ICSOL . It’s usually chronic, not very severe (mild), throbbing in nature & it's an early morning headache awakening the patient from sleep. The localization of the headache is not significant in the localization of the lesion, for example; having frontal headache does not mean the lesion is in the frontal lobe.
The headache occurs at early morning due to :
i. Respiration during sleeping is usually slower than normal increased C02 vasodilatation - -congestion stretching of meninges ~> headache .
ii. CSF gets collected intracranially due to the supine sleeping position, and with the presence of ICSOL; the gradual pooling of CSF intracranialiy increases the ICP which leads to headache.
B- Vomiting
Usually projectile also occurs at early morning. It can give temporary relief of the headache and thus can be self-induced (the patient himself induces vomiting so as to get relief).** Vomiting is an important feature in Pediatrics Brain tumour .
he’s having a bad day ..
C- Papilloedema
( swelling of the optic disc).# The optic nerve is part of the brain with full meningeal coverings.
In early papilloedema ; there will be 1 absence of venous pulsation leading to2 congestion of the disc, after that there will be 3 nipping of the blood vessels & later there will be 4 haziness of the temporal margin of the disc .
# At the very late stages there will be 5 complete absence of the disc with areas of haemorrhage.
# Vision will not be much affected by papilloedema even in late stages.
# There may be different types of scotomas.# Prolonged papilloedema can lead to secondary optic atrophy (white or pale disc with small blood vessels).In secondary optic atrophy the vision will be severely impaired.
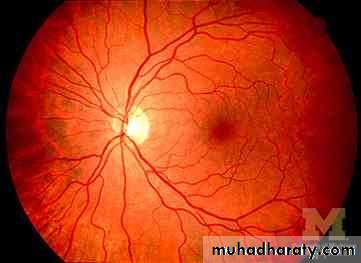
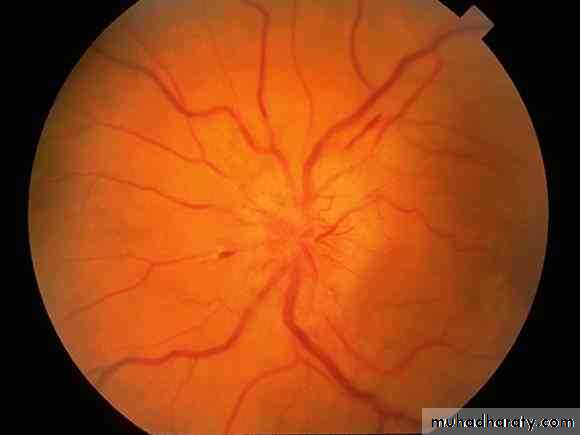
NORMAL OPTIC FUNDUS & Papilloedema ( loss of venous pulsation
NORMAL OPTIC DISC and congestion )
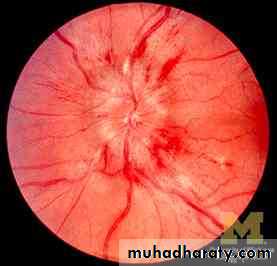
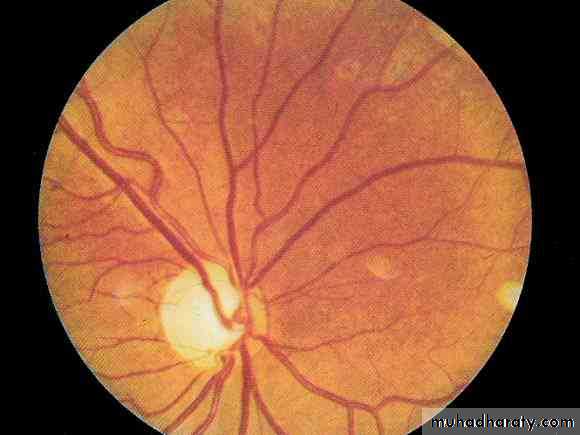
Papilloedema ( nipping of blood vessels ,
complete absence of the disc with areaof haemorrhage ) OPTIC NERVE ATROPHY
Notes:
• Venous pulsation is absent in about 20% of normal people.• Seeing the pulsation excludes the presence of papilloedema, but not seeing it means either there is papiiloedema or the person examined is normal.
• We depend on temporal margins to detect haziness because nasal margins can be normally hazy.
• Nipping means a snake - like appearance of the blood vessels which happens because the vessels don't enter the disc in a straight line due to its swelling .
• In optic disc atrophy there will be a white or pale area, detecting blood vessels would not be possible then.
• There are two causes for late presentation: 1 headache being mild and 2 normal vision until late stages of papilloedema.
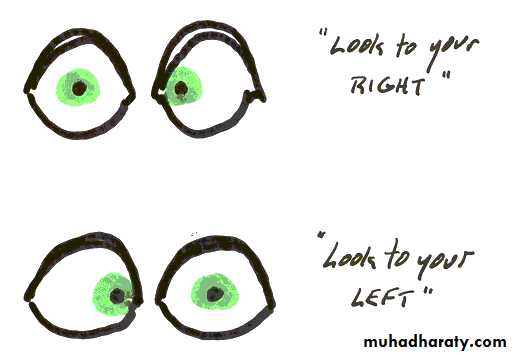
D. Others, such as epilepsy (in adults with negative family history) & 6th cranial nerve palsy.
* The 6tn cranial nerve has a long intracranial course and can be considered as an intracranial structure & that's why its palsy is considered as a general sign ; it is also considered as a false localization sign because it doesn't give an accurate idea about the lesion's site.
RIGHT 6TH NERVE PALSY
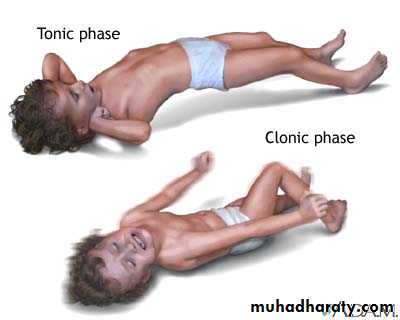
hold him tight people he’s having a seizure
GRAND MAL SEIZURE
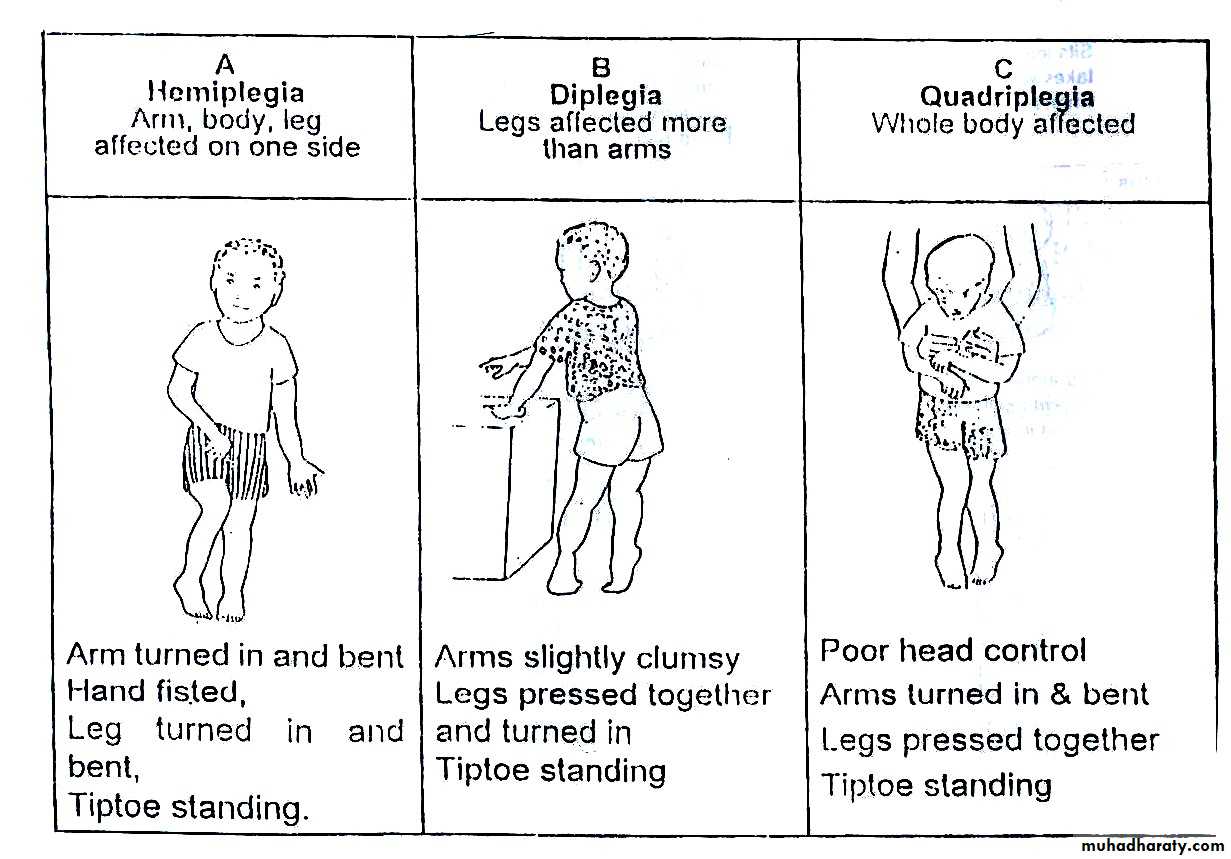
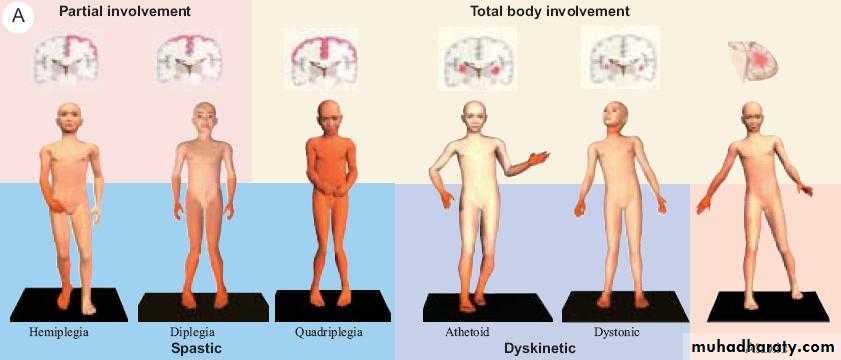
Focal signs :
Such as hermiplegia, hemianaesthesia , aphasia or focal epilepsy. They depend on the site of the ICSOL.TYPES OF PLEGIA
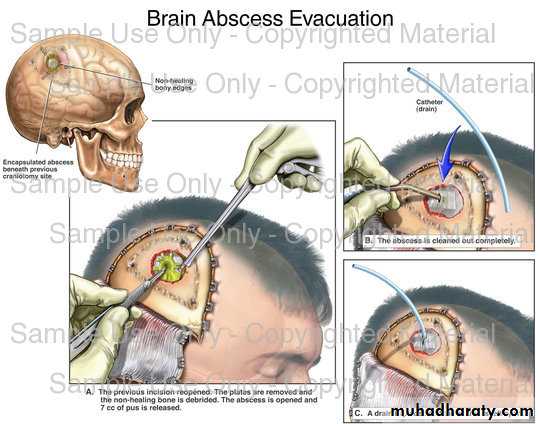
BRAIN ABSCESS
It's the collection of pus inside the brain's parenchyma surrounded by true capsule.It’s usually secondary to a focus outside the cranial cavity which reaches the brain either directly or indirectly (blood borne) .
1- Direct route :
a- Chronic otitis media, which reaches the brain by 2 mechanisms ;i- Perforation of the tympanic membrane leading to temperal lobe abscess.
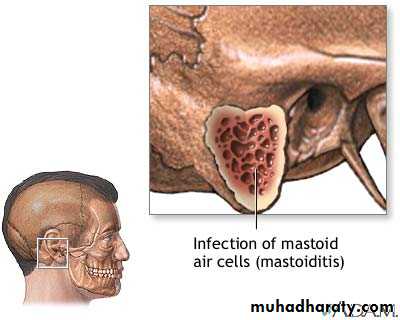
ii- Posterior perforation of the mastoid process leading to cerebellar abscess (less
common),
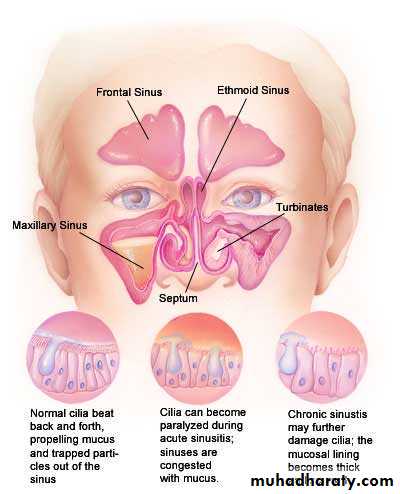
b- Paranasal sinuses (mainly ethmoidal or frontal sinus ).
c- Penetrating wounds especially with foreign bodies as missiles & bullets.
d- Infections around the face (the dangerous triangle).
e- Osteomyelitis of skull bones (uncommon as we here have a heavy blood supply).
2- Indirect (blood borne):
By emboli from lung abscesses, bronchiectasis, valvular heart disease (esp. cyanotic) or osteomyelitis of peripheral bones. Congenital valvular heart diseases are the most important cause in children.
Clinical features:
9Picture of the underlying cause, such as osteomyelitis, lung abscess or valvular heart disease.
2- Signs & symptoms of ICSOL (general & focal).
3- Signs & symptoms of intracranial infection, including fever, lassitude and, if meningitis present , neck stiffness , kernig’s sign & brudzinski’s sign .Diagnosis:
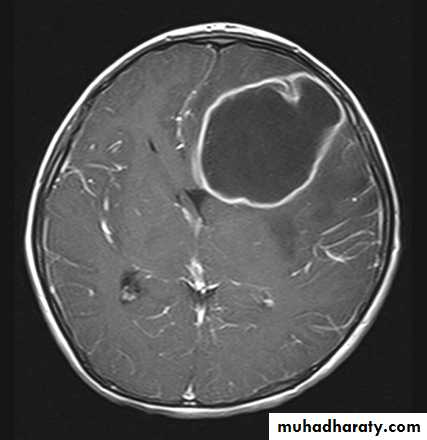
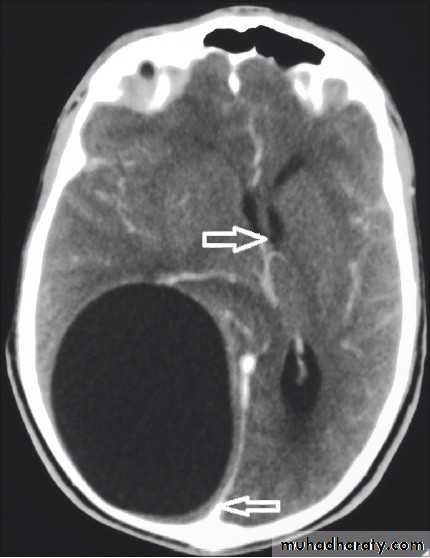
Is by C.T. scan with contrast which will show hypodense lesion surrounded by a ring of enhancement (the capsule) & oedema, MRI is not used as it takes a long time to achieve good result, a time which we don't usually have in patients with ICSOL as they are irritable and (unstable).Mastoiditis
Sinusitis
CT scan of a brain abscess
Treatment :
1. Drainage ; usually by bur hole drainage, sometimes there's recurrence & may need to do several drainages, It's done by using a catheter but its downside is that the capsule will not be evacuated which means high recurrence rates. Some surgeons prefer to do craniotomy & excision of the abscess with the capsule, usually done in a single surgery but it carries high morbidity &mortality rates.
2. Heavy systemic antibiotics, usually combination. Steroids are given when there's focal oedema only,
3. Proper treatment of the underlying cause.
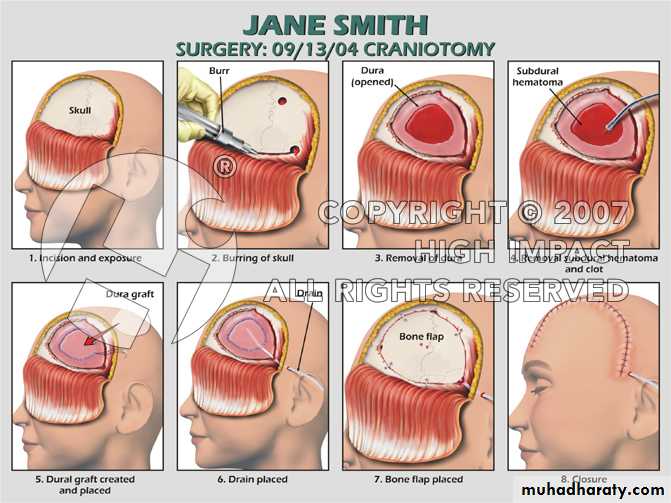
CRANIOTOMY
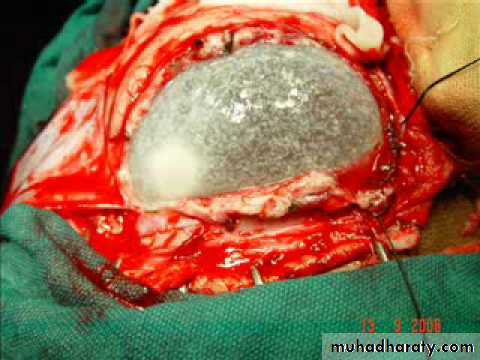
HYDATID CYST
Primary or secondary (the latter can be multiple and if multiple priority is given to the brain EXCEPT when the lung is involved).
Diagnosis;
C.T. scan: very well circumscribed orange-like hypodense area with ventricular shift.* Do CXR to exclude lung involvement .
Treatment
Craniotomy & excision (always try to evacuate the cyst intact).*If there was rupture then wash the brain with hypertonic saline then give albendazole for 3 months
* Some researches suggest that rupturing the cyst then a 3 month treatment with albendazole is sufficient.
* In treatment we must begin with hydatid cyst in lung, brain and then to the other organs
PrognosisIf it's primary & removed intact the prognosis is excellent, otherwise it's bad.